![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
26 Cards in this Set
- Front
- Back
|
what are the two main functions of the male reproductive system |
production/development, maturation and transport of spermatozoa synthesis of hormones (testosterone) |
|
|
what are the 4 major components of the male reproductive system |
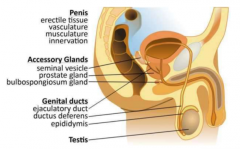
testis genital ducts accessory glands penis |
|
|
what are all the coverings of the testis and what are their abdominal correlates |
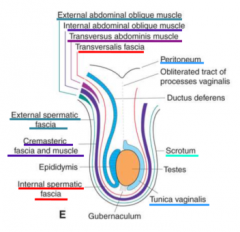
tunica vaginalis (parietal and visceral) from peritoneum internal spermatic fascia from transversalis fascia cremaster muscle from internal oblique external spermatic fascia from external oblique (Buck's fascia in penis) Dartos Fascia (colles) from scarpas fascia (superficial penile fascia in penis) dartos muscle (smooth muscle) from campers fascia from gubernaculum pulling layers down during development |
|
|
define cryptorchidism |
absence of one or both testes from scrotum 80% descend in first year 1% true incidence |
|
|
describe the tunica albuginea |
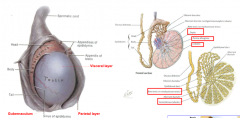
most intimate layer covering testes sends septa into testes, separating seminiferous tubules into lobules |
|
|
describe the lobules of the testicle |
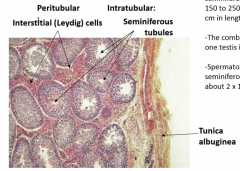
two compartments peritubular: interstitial (leydig) cells intratubular: seminiferous tubules |
|
|
describe leydig cells |
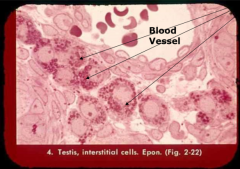
site of testosterone production (steroid synthesis) lipid droplets, smooth ER, mitochondria testosterone profuses to sertoli cells estradiol feedback (block) growth factor feedback (promote) leutinizing hormone receptor-- produce enzymes-- more testosterone |
|
|
describe the seminiferous tubules |
spermatozoids produced here ~2000 per second |
|
|
describe briefly spermatogenesis |
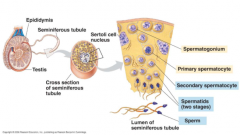
1. spermatocytogenesis: spermatogonium on periphery to secondary spermatocyte medially (cell division-- mitosis and meiosis I) 2. spermiogenesis: differentiation/maturation of sperm cell from spermatid (meiosis II) golgi apparatus collects and makes acrosomal vesicle centrioles collect opposite and make flagellum compact nucleus |
|
|
describe sertoli cells |
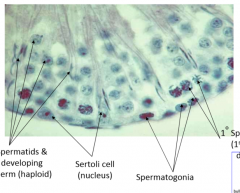
engulf developing spermatids and provide environment for development nutrients clear excess cytoplasm makes androgen binding protein (ABP) which binds and concentrates testosterone form tight junctions to separate basal and adluminal compartments-- blood testes barrier (autoimmune defense) follicle stimulating hormone receptor-- growth factor or aromatase (estradiol) |
|
|
what are the mechanisms of thermoregulation of the testis |
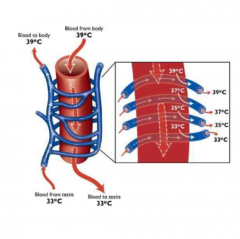
1. testis located outside body 2. superficial testicular artery 3. contraction of dartos (cremaster) if cold 4. counter-current exchange of blood flow by pampiniform plexus |
|
|
describe the rete testis |
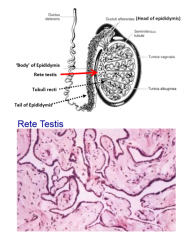
next step after seminiferous tubules simple cuboidal epithelium with microvilli and cilia to move nonmotile spermatozoa carries sperm to head of epididymis |
|
|
describe the epididymis |
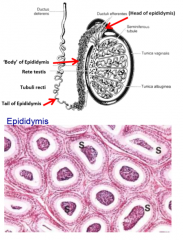
sperm storage depot pseudostratified columnar with smooth muscle layer convoluted tubule sperm become compacted, fluid removed and replaced |
|
|
describe the ductus deferens |
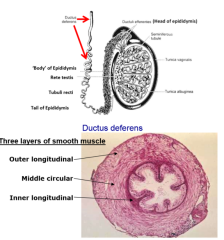
vas deferens larger, more organised version of epididymis folds for expansion (hold more) strong, perstialtic contractions (sympathetic nervous system) 3 muscle layers: outer longitudinal, middle circular, inner longitudinal |
|
|
describe a vasectomy |
cut ductus deferens to sterilize must cauterize ends |
|
|
describe the ejaculatory duct and accessory glands |
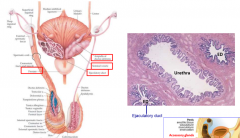
2 ejaculatory ducts on either side of urethra vas deferens meets with seminal vesicle and prostate gland to form ED |
|
|
describe the seminal vesicle |
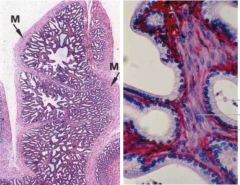
produces most of ejaculate pseudostratified epithelium smooth muscle lining (sympathetic) produces lots of fluid-- fructose, citrate etc. |
|
|
describe the prostate gland |
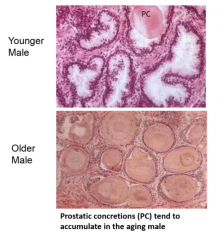
pseudostratified columnar/cuboidal epithelium secretes various substances can form concretions, accumulate with aging peripheral zone-- most glandular tissue, common cancer site transition zone-- location of urethra central zone-- location of ejaculatory ducts |
|
|
what are the last 2 accessory glands |
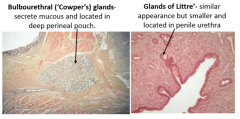
bulbourethral glands: located in deep perineal pouch, secrete mucous glands of littre: similar in appearance but smaller and in penile urethra pre-ejaculate-- lubrication |
|
|
describe testosterone |
stored in sertoli cells differentiation and maintenance of glands, ducts, smooth muscle facial hair, sperm production, muscle mass, male voice, hypothalamus/pituitary |
|
|
what happens if you have excess testosterone in blood stream |
~100x less testosterone than in seminiferous tubules high testosterone, hypothalamus and pituitary inhibits LH and FSH, decrease testosterone |
|
|
what are the erectile bodies in the penis |
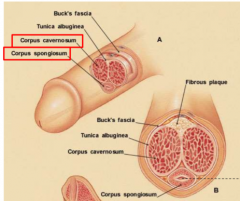
surrounded by tunica albuginea paired corpus cavernosa (dorsal)-- thinner trabeculae to fill with blood corpus spongiosum (ventral, contains urethra) |
|
|
how is an erection achieved |
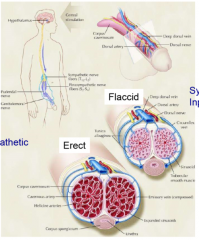
parasympathetic-- secrete nitric oxide relax smooth muscles in helican artery, release blood into cavernosa compresses dorsal vein, blood doesn't flow out somatic input-- muscle contraction push blood distally |
|
|
what are the 4 stages of the male sexual response |
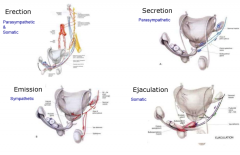
erection: para on vascular smooth muscle, somatic on striated secretion: para on secretory epithelium (seminal vesicles, prostate, bulbourethral, penis) emission: sym on smooth muscle (epididymis, seminal vesicles, prostate) ejaculation: somatic on striated muscle of penis |
|
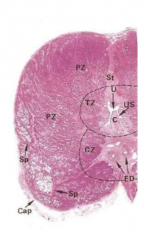
describe this image |
prostate tissue demonstrating zones |
|
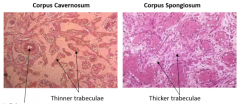
describe this image |
corpus cavernosum and corpus spongiousum histology of erectile tissue |

