![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
101 Cards in this Set
- Front
- Back
|
circulation
|
- pressure driven bulk flow of blood through a system of tubular vessels or passages
- rapid transport of oxygen, carbon dioxide, nitrogenous wastes, hormones, immunoglobulins, heat, nutrients, ions |
|
|
pumps
|
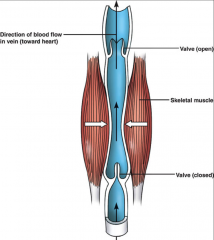
- peristaltic pump
- wave of contraction pushes blood |
|
|
muscular heart
|
- single chambered
- may have accessory or auxiliary hearts - multichambered |
|
|
open circulation for single chambered
|
- blood baths tissue directly
- no clear distinction between blood and extracelluar tissue - fluid = hemolymph - blood exits discrete blood vessels - enters lacunae = small spaces around tissues - enter sinuses = large spaces used as channels for blood flow |
|
|
blood flow through lacunae and sinuses
|
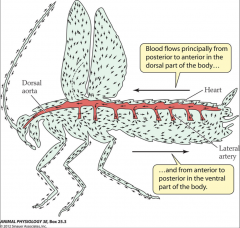
- aorta and lateral artery branches end abruptly
- slow rate of blood flow - circulatory system can remain simple because tracheal system - blood flows principally form posterior to anterior in dorsal part of body - anterior to posterior in ventral part of body |
|
|
circulation through body or crayfish or lobster
|
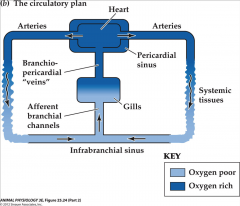
|
|
|
closed circulation for single chambered
|
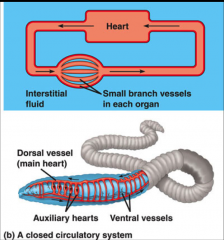
|
|
|
vertebrate circulation
|
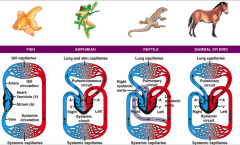
- single loop
- double loop |
|
|
circulatory plan in gill-breathing fish
|
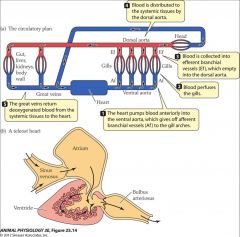
- heart pumps blood anteriorly into ventral aorta
- gives afferent branchial vessels to gill arches - blood perfuses gills - blood is collected into efferent branchial vessels which empty into dorsal aorta - blood distributed to systemic tissues by dorsal aorta - great veins return deoxygenated blood from systemic tissues to heart |
|
|
circulatory plan through human
|
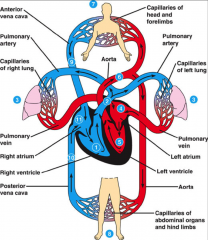
|
|
|
teleost heart
|
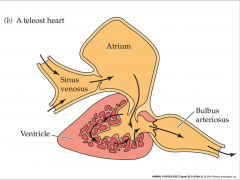
- myocardium usually spongy and oxygenated by blood in ventricle
- sinus venosus are great veins that empty into it - ventricle is main propulsive force - bulbus arteriosus acts as an elastic chamber and pressure reservoir |
|
|
amphibians
|
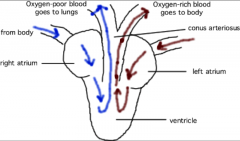
- 2 separate atrial chambers
- ventricular trabeculas and spongy myocardium help shunt right atrial blood into pulmonary arteries - conus arteriosus is contractile and has spiral folds which contribute to shunting - double loop circulation |
|
|
truncus arteriosus
|
- formed from conus arteriosus
- systemic arch goes to body - pulmocutaneous arch goes to lungs and skin - carotid arch goes to head region |
|
|
crocodiles
|
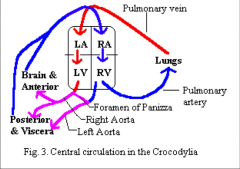
- ventricle incompletely divided by muscular ridges and spongy septa
- 2 systemic aortas: one from right and left ventricle - formen of panizza prevents left systemic arch from carrying deoxygenated blood |
|
|
blood flow in ventricles and atrium of crocodiles
|
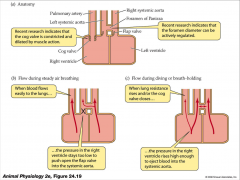
- cog valve is constricted and dilated by muscle action
- foreman diameter can be actively regulated - when blood flows to lungs - pressure in right ventricle stays too low to push open the flap valve into systemic aorta - lung resistance rises and/or cog valves closes - pressure in right ventricle rises high enough to eject blood into systemic aorta |
|
|
vertebrate heart
|
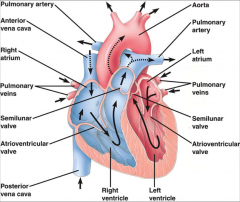
- anterior vena cava = superior vena cava
- posterior vena cava = inferior vena cava |
|
|
chordae tendinae
|
- thread-like bands of fibrous tissue
- attach one end to tricuspid and mitral valves and the other end to papillary muscle - serve to anchor the valves |
|
|
papillary muscle
|
- originate in ventricule wall
- small muscle within heart - anchor heart valves - attach to tricuspid valve by chordae tendinae |
|
|
heart valves
|
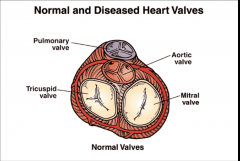
- pulmonary valve
- tricuspid valve - aortic valve - mitral valve |
|
|
heart contraction and relaxation
|
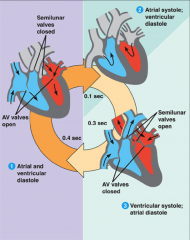
- systole is period of contraction
- diastole is period of rest/relaxation - atrial and ventricular diastole - atrial systole and ventricular diastole - ventricular systole and atrial diastole |
|
|
human heart
|
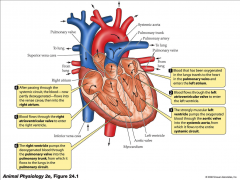
- oxygenated blood travels to heat in pulmonary veins and enters left atrium
- blood flows through left atrioventricular valve to enter left ventricle - strongly muscular left ventricle pumps oxygenated blood through aortic valve into systemic aorta - slows to entire systemic circuit - after passing through systemic circuit, blood is partly deoxygenated - flows into venae cavae, then into right atrium - blood flows through right atrioventricular valve to enter right ventricle - right ventricle pumps deoxygenated blood through pulmonary valve into pulmonary trunk - flows to lungs in pulmonary circuit |
|
|
heart rate
|
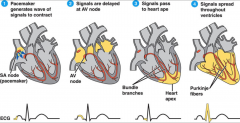
- pacemaker generates wave of signals to contract
- signals are delayed at AV node - signals pass to heart apex - signals spread throughout ventricles |
|
|
pacemaker action potential
|
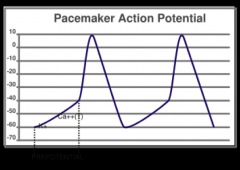
- pacemaker cells are special myocardial cells that discharge rhythmically
- have special type of action potential - first part of prepotential is caused by relatively smaller efflux of K+ in phase 4 of action potential - transient type of calcium channel (T) opens - form second part of prepotential - as potential declines, the long lasting calcium channel opens - leads to depolarization - mostly due to Ca2+ with only little influence from Na+ influx - absence of sharp depolarizing spike |
|
|
cardiac action potential
|
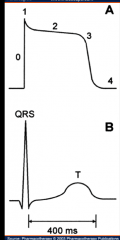
- sodium enters the cell through fast Na channels
- fast Na channels close - Ca and additional Na enter cell through slow channels - K exits cell and resting membrane potential is reestablished - equilibration of Na and K occurs |
|
|
conducting system
|
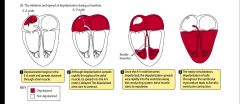
- depolarization begins in SA node and spreads outward through atrial muscle
- spreads into AV node is delayed - depolarized atria starts to contract - once AV becomes depolarized, depolarization spreads rapidly into ventricles along conducting system - atrial muscle starts to repolarize - nearly simultaneous depolarization of cells throughout ventricular myocardium leads to forceful ventricular contraction |
|
|
human electrocardiogram
|
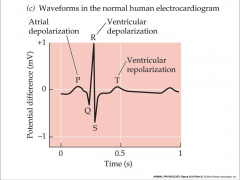
|
|
|
heart as a pump
|
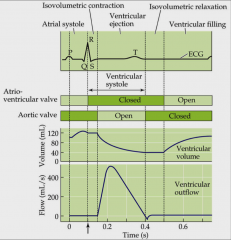
- cardiac output is volume of blood per unit time
- vertebrate cardiac output is volume of blood in left ventricle to systemic circulation - product of heart rates in beats per minute - stroke volume is volume of blood pumped per cardiac cycle |
|
|
anatomy of blood vessels
|
- arteries carry blood away from heart
- veins carry blood back to heart - capillaries connect smallest arteries to veins |
|
|
layers of muscular artery
|
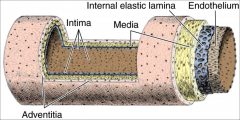
- tunica intima
- tunica media - tunica externa/adventitia |
|
|
tunica intima
|
- simple squamous endothelium
- overly basement membrane - layer of fibrous tissue |
|
|
tunica media
|
- usually thickest
- smooth muscle - collagen - some elastic |
|
|
tunica externa/adventitia
|
- loose connective tissue with vasa vasorum
|
|
|
large artery
|
- conducting or elastic arteries
- internal elastic lamina - expand during systole and recoil during diastole - collagenous tissue - aorta, common carotid, subclavian, pulmonary trunk, common illeac |
|
|
medium artery
|
- muscular or distributing arteries
- brachial, femoral, renal - internal and external elastic lamina |
|
|
arteriole
|
- resistance arteries
- smallest of these are arterioles - smooth muscles in walls are responsible for vasomotor control of blood distribution - vasoconstriction and vasodilation |
|
|
arteries
|
- become smaller in diameter
- walls become thinner - very little drop in pressure in arterial system - circumferential tension (stretch) developed within walls is directly proportional to tube radius - small artery exposed to same blood pressure as larger one - tension developed in walls is lower in large one because radius is smaller - smaller artery can be less fortified than a larger one and not over-expand |
|
|
microcirculatory bed
|
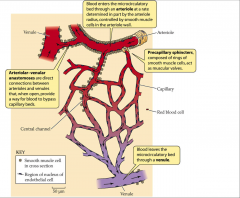
- arteriolar-venular anastomoses are direct connection between arterioles and venules
- when open provide way for blood to bypass capillary bed - precapillary sphincters composed of rings of smooth muscle cells that act as muscular valves - blood enters through arteriole at rate determined by arteriole radius - controlled by smooth muscle cells in arteriole wall - blood leaves through venule |
|
|
sphincters
|
- smooth muscles and precapillary sphincters permit highly sensitive temporal and spatial control of blood distribution
- change blood pressure and blood flow |
|
|
fenestrated capillary
|
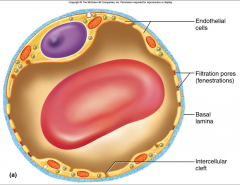
- only endothelium
- filtration holes - contain channels - discontinuous and continuous cells - important in kidneys, endocrine glands, smal intestines, choroid plexus of brain |
|
|
continuous capillary
|
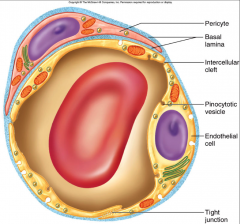
- endothelial cells held together by tight junctions
- may have pericytes that contract to regulate blood flow |
|
|
sinusoidal capillary
|
- discontinuous capillaries
- irregular blood filled spaces - liver, bone marrow, spleen - blood forming organs - huge sinus - diffusion through cell - thicker epithelium |
|
|
circulatory routes
|
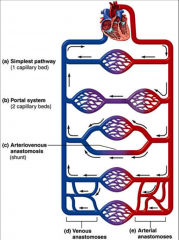
- simplest pathway = one capillary bed
- portal system - arteriovenous anastomosis |
|
|
portal system
|
- 1 capillary system to next capillary system
- hypothalamus and anterior pituitary - small intestine and liver - kidney |
|
|
arteriovenous anastomosis
|
- can pass through capillary bed, around capillary bed, or combination of both
- embryonic - shunt |
|
|
capillary exchange
|
- only occurs across capillary walls between blood and surrounding tissues
- 3 routes across endothelial cells - intracellular clefts - fenestrations - cytoplasm or transcytosis |
|
|
diffusion
|
- most important mechanism of capillary exchange
- movement of material through OM - high concentration to low concentration - lipid soluble substances = steroid hormones - O2 and CO2 diffuse easily - insoluble substances - glucose and electrolytes must pass through channels, fenestrations, or intracellular clefts - large particles such as proteins are held back |
|
|
transcytosis
|
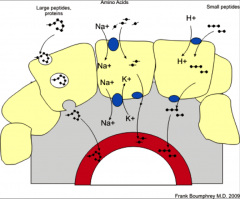
- endothelial cells pick up material on one side of PM by pinocytosis or receptor mediated endocytosis
- transport it through cell to other side where it exits by exocytosis - mediated by endocytosis and exocytosis - enters one cellular face and leaves through another - tissues to blood or blood to tissue - large proteins and small peptides |
|
|
filtration
|
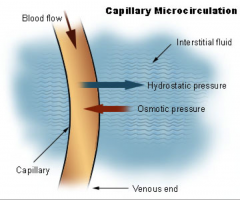
- hydrostatic pressure forces fluid through a selectively permeable membrane
- driven by pressure differences - capillaries give off fluid at arteriole end due to higher BP/hydrostatic pressure - hydrostatic and osmotic pressure decrease along length of capillary - create collodial pressure that's greater than outside pressure - collodial osmotic pressure higher at venule end forces fluid back in (reabsorption) - net filtration pressure is difference between outward and inward pressure |
|
|
blood plasma volume
|
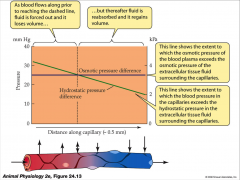
- loses volume in initial segment of blood capillaries
- regain fluid in final segments - lose at arteriole and gain at venous - hydrostatic pressure of blood pushes stuff out - hydrostatic pressure of tissue and collodial osmotic pressure bring stuff in |
|
|
net filtration pressure
|
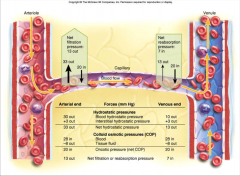
- hydrostatic pressure of blood in capillaries
-minus hydrostatic pressure of tissue fluid outside capillaries - plus collodial osmotic pressure of blood |
|
|
veins
|
- lower blood pressure with fluctuation
- thinner walls - less muscular and elastic tissue - expand easily - high capacitance - valves aid skeletal muscles in upward blood flow |
|
|
venous sinuses
|
- veins with thin walls
- large lumens - no smooth muscle |
|
|
large vein
|
- venae cavae, pulmonary veins, internal jugular, renal veins
|
|
|
medium vein
|
- many have valves
- infoldings of tunica interna - skeletal muscle pump pushes blood through valve toward heart - prevents backflow |
|
|
venule
|
- post capillary
- surrounded by pericytes - porous - exchange fluid with surrounding tissue |
|
|
mechanism of venous return
|
- pressure gradient
- gravity drains blood from head and neck - skeletal muscle pump in the limbs = pushes blood back - thoracic has negative pressure = draws blood up - cardiac suction of expanding atrial space = sucks blood up |
|
|
venous return
|
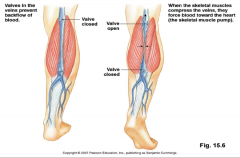
- valves in veins prevent backflow of blood
- skeletal muscles compress veins - force blood towards heart |
|
|
blood distribution
|
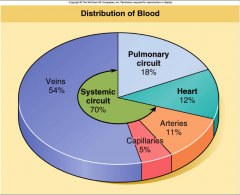
- majority in veins
|
|
|
cross sectional area and capillaries
|
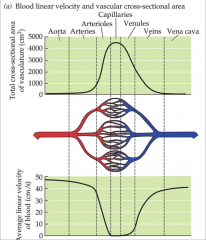
- as blood flows from aorta to capillaries
- total cross sectional area increases - average linear velocity decreases - greatest cross sectional area in capillaries - cross sectional area increases, velocity decreases - velocity slowed down due to decreased pressure - pressure decreases from arteries to veins - never return to original velocity - greatest velocity in arteries |
|
|
hematocrit
|
- 43% erythrocytes (RBC)
- thin layer of leukocytes called buffy coat between erythrocytes and plasma |
|
|
red blood cells
|
- erythrocytes
- 7-7.4 um - biconcave - increased surface area |
|
|
reticulocyte
|
- immature RBC
- everyone has certain number - carry almost as much oxygen as normal RBC |
|
|
sickle cell anemia
|
- abnormal RBC
- get stuck in capillaries - heterozygous have some sickling - homozygous have a lot of sickling |
|
|
rouleaux
|
- RBC done't settle very much
- some disease conditions increase production of fibrinogen and immunoglobulins causing RBC to clump - ERS used to follow progress of certain disease conditions |
|
|
2 classes of leuckocytes
|
- granulocytes
- a granulocytes |
|
|
granulocytes
|
- have granules
- neutrophils - eosinophils - basophils |
|
|
a granulocytes
|
- azurophilic granules
- some granules but very little - lymphocytes - monocytes |
|
|
neutrophils
|
- larger than RBC
- one nucleus and variable number of lobes - squeeze out of blood into tissue - diaponeses is process of squeezing into tissue |
|
|
basophils
|
- numerous granules cover nucleus
- release histamines - deal with inflammatory response - larger than RBC |
|
|
eosinophils
|
- found in high numbers
- allergic reaction and parasitic infection - larger than RBC |
|
|
monocyte
|
- large kidney shaped nucleus
- cytoplasm slightly basophilic - located in blood - called macrophage in located outside blood - phagocytic - antigen presenting cell |
|
|
lymphocyte
|
- killer cells, B and T cells
- antibody production = B cells - mediated cell response = T cells - specific protein receptors on cell surface |
|
|
platelets
|
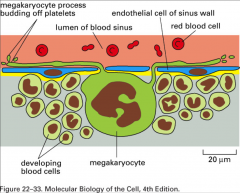
- derived from megakarocytes in bone marrow
- multi nucleated cells - live in bone marrow - fragments of cell - contain growth factors and clotting factors |
|
|
blood cell production
|
- controlled by cytokines
- almost all glycoprotins that act of stem cells |
|
|
3 factors of cytokines affect blood cell production
|
- colony stimulating factors (CSF)
- erythropoietin - interleukins |
|
|
colony stimulating factors (CSF)
|
- made by endothelial cells and white blood cells
|
|
|
erythropoietin
|
- lack of oxygen or shortage of erythrocytes
- stimulates cells in kidney to synthesize and secrete hormone |
|
|
interleukins
|
- made by lymphocytes
- serve as growth factor for B cells - non-lymphocytes blood cells |
|
|
total fluid energy
|
- true driving force for blood flow
- potential energy of pressure produced by heart - plus kinetic energy - plus kinetic energy of position in earth's gravitational field |
|
|
pressure change
|
- important driving force
- around 100 - affects rate of blood flow - above heart = arterial pressure decreases - below heart = arterial pressure increases |
|
|
flow rate
|
- dependent on differences in blood pressure and vascular resistance
- poiseuille equation - proportional to pressure difference - proportional to fourth power of radius - inversely proportional to resistance - inversely proportional to viscosity - inversely proportional to length |
|
|
principles of blood flow
|
- blood flow is amount of blood flowing through a tissue in given time
- perfusion is rate of blood flow per given mass of tissue - blood flow and perfusion important for delivery nutrients and oxygen, and removal of waste - hemodynamics are physical principles of blood flow based on pressure and resistance |
|
|
change in radius
|
- muscles in walls of blood vessels change radius of vessel by contracting or relaxing
- exert profound control over flow rate |
|
|
heat
|
- pressure and flow turn to heat during circulation
|
|
|
velocity profile of laminar flow
|
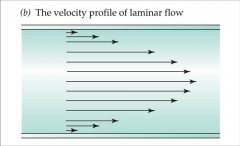
- velocity immediately next to tube wall are zero
- steady and non-turbulent flow, liquid moves in series of concentric layers that differ in linear velocity - layers closer to center move faster |
|
|
frictional force
|
- concentric layers encounter as they flow over each other
- total magnitude of internal friction depends in part on diameter and length - viscosity also contributes to internal frictional force - lack of intrinsic slipperiness between liquid layers moving at different velocities |
|
|
radius affects velocity
|
- large radius = high average velocity
- small radius = slower average velocity - slowed down by friction against vessel wall |
|
|
energy to heat
|
- results in degradation of kinetic energy into heat
- pressure provided at entry end of heart is potential energy - converted to kinetic energy - kinetic energy converted to heat energy - pressure converted to heat |
|
|
blood pressure
|
- dependent on elasticity of arteries
- expansion and recoil maintain steady flow of blood throughout cardiac cycle - smoothes out pressure fluctuations and decrease stress on small arteries - rises with age because arteries less distensible (elastic) - produce fewer elastic fibers as you age |
|
|
blood pressure determinants
|
- cardiac output = volume of blood pumped by heart
- blood volume - peripheral resistance = mean arterial pressure minus venous pressure divided by cardiac output |
|
|
mean arterial pressure
|
- diastole last longer than systole
- equals diastolic plus (systolic - diastolic) |
|
|
cardiac output
|
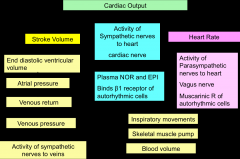
|
|
|
starling's law
|
- energy of contraction is proportional to initial length of cardiac fiber
- length of cardiac fiber is increased with increased filling - when cardiac muscle is stretched it contracts more forcefully - optimum overlap creates greatest contraction |
|
|
skeletal vs heart muscle
|
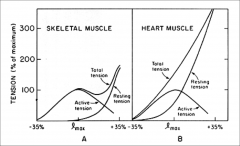
- both have developed forces rise to peak at optimal length then then fall off at very long lengths
- declining portion in both is due to diminishing overlap between actin and myosin - at lengths less than optimal, force declines because myosin collision with z line and Ca release from SR declines with short lengths - resting force higher in cardiac and significant at lengths less than optimal - intact heart can respond to increase of filling by improving contraction |
|
|
total peripheral resistance
|
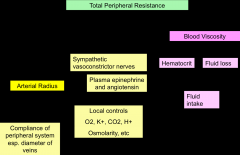
|
|
|
regulation of BP and flow
|
- local control
- neural control - hormonal control |
|
|
local control
|
- ability of tissue to regulate its own blood supply
- when tissue inadequately perfused = becomes hypoxic and metabolites accumulate - metabolites are CO2, H+, K+, lactic acid, adenosine - factors stimulate vasodilation - short term stimulate by vasoactive chemicals like histamine and nitric acid - derived from platelets, endothelial cells, perivascular tissue - long term achieved by growth of new vessels |
|
|
neural control
|
- control in vasomotor control center of medulla
- integrate baroreflexes, chemoreflexes, and medullary ischemic reflex - change in blood pressure - chemoreflexes monitor pH, O2, and CO2 levels - issue signals to blood vessels through sympathetic nerve fibers - medullary ischemic reflex responds to drop in perfusion by increasing heart rate and contraction force |
|
|
hormonal control
|
- regulated by various hormones like
- angiotensin 2 = vasoconstrictor - aldosterone = promotes Na+, water retention by kidney that increases BP - atrial natiuretic peptide = increases Na+ excretion by kidney that lowers BP - ADH = promotes water retention - epinephrine and norepinephrine = bind to smooth muscle of blood vessels causing vasoconstriction |
|
|
vasomotion
|
- generalized raising or lowering of BP
- selectively modifying perfusion of particular organ - rate of oxygen delivery = cardiac output x ([arterial O2] - [venous O2]) |
|
|
exercise
|
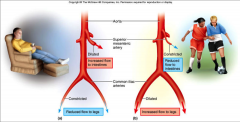
- cardiac output increased by both heart rate and stroke volume
- cardiac rate result of vagus nerve inhibition and sympathetic nerve stimulation - coordinated by cardiac centers in medulla - arterial blood pressure doesn't rise because vascular resistance reduced by vasodilation - arterioles shift blood flow with changing priorities - increase perfusion of lungs, myocardium, and skeletal muscles - decreases perfusion of kidneys and digestive tract |

