![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
157 Cards in this Set
- Front
- Back
|
What is the largest glandular tissue in the body? Size?
|
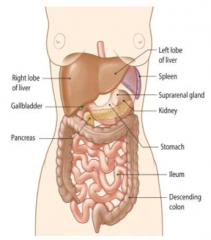
Liver
- 1200g to 1800g - 12-15 cm top to bottom - 15-18 cm across - Males: 1.8 kg (avg weight) - Females: 1.4 kg (avg weight) |
|
|
What are the lobes of the liver? Which are the biggest?
|
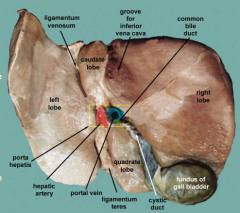
- Right
- Left - Quadrate - Caudate R and L lobes make up the bulk |
|
|
What blood does the liver receive? Origin?
|
Receives mainly venous blood, arriving directly from the spleen, pancreas, and intestine
|
|
|
What are the implications of the liver receiving venous blood from the spleen, pancreas, and intestine?
|
It is the first organ to encounter any ingested toxic substances as well as nutrients
|
|
|
What kind of tissue makes up the liver?
|
- Bulk is uniform parenchymal cells = hepatocytes
- Sparse connective tissue |
|
|
What are the functions of the liver?
|
- Detox metabolic waste products
- Synthesize plasma lipoproteins - Synthesize blood clotting factors - Synthesis, secretion, and storage of carbs and lipids - Destruction of spent RBCs and recovery of constituents - Synthesis and secretion of bile |
|
|
What are the two types of properties of the liver? How do they differ?
|
Endocrine
- From hepatocytes directly into the hepatic blood - Includes: albumin, fibronectin, transferrin, prothrombin, lipoproteins, α-1-antitrypsin, glucose (after glycogen breakdown), and thyroxin (highly active form) Exocrine - Production of bile |
|
|
What happens to endocrine secretions from the hepatocytes? Which ones?
|
- Directly enter the hepatic blood
- Albumin, fibronectin, transferrin, prothrombin, lipoproteins, α-1-antitrypsin, glucose (after glycogen breakdown), and thyroxin (highly active form of thyroid hormone) |
|
|
What compound is produced by hepatocytes to be released for exocrine function?
|
Bile
|
|
|
What are the four functional groups of liver components?
|
- Connective tissue
- Large vessels (including blood vessels, lymphatic vessels, nerves, and bile ducts) - Sinusoidal capillaries (sinusoids - which line the plates of hepatocytes and are responsible for blood flow through the liver) - Hepatocytes |
|
|
What surrounds the hepatocytes and sinusoids in the liver?
|
Reticular fibers composed of Collagen Type III
|
|
|
What is the only connective tissue in the lobules of the liver? Organization? Functions?
|
Reticular Fibers made of Collagen Type III
- Sparse - Extends outward from the central vein - Supports the hepatic parenchyma - Contributes toward keeping sinusoids open to allow normal blood flow |
|
|
What is the origin of the reticular fibers (collagen type III) that surround hepatocytes and sinusoids?
|
Stellate / Ito cells found in the Space of Disse
|
|
|
Where are Stellate / Ito cells found? Function?
|
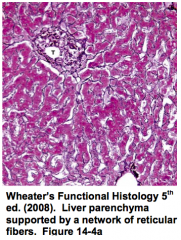
- Space of Disse
- Form the reticular fibers (collagen type III) that surrounds hepatocytes and sinusoids |
|
|
What can disrupt the reticular fiber network surrounding hepatocytes and sinusoids? How can you assess this?
|
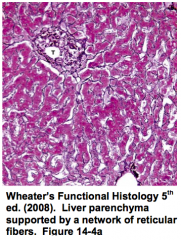
- Liver disease can cause disruption of this network
- Staining for Reticulin can aid diagnosis |
|
|
What are the fiver major vessel systems in the liver?
|
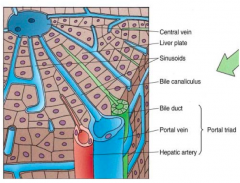
- Hepatic artery
- Hepatic portal vein - Central veins - Bile ducts - Lymphatic vessels |
|
|
What is the function of the hepatic artery? Origin?
|
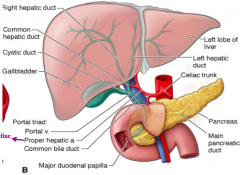
- Carries oxygenated arterial blood into the liver
- Arises from the celiac trunk |
|
|
What is the function of the hepatic portal vein?
|
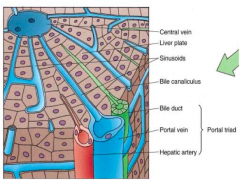
- Carries venous blood into the liver (high in nutrients)
- Brings blood from the intestines (contains many nutrients and toxic substances), pancreas (contains endocrine secretions like insulin and glucagon), and spleen (contains breakdown products of blood cells) |
|
|
What is the function of the central veins?
|
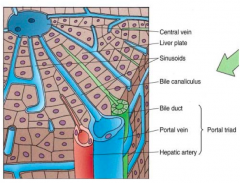
Carries blood away from the liver toward the hepatic veins and eventually into the IVC
|
|
|
What is the function of the bile ducts?
|
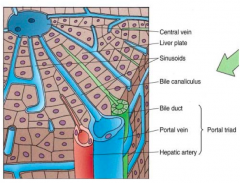
Transports bile from the liver
|
|
|
What is the function of the lymphatic vessels in the liver?
|
Carries lymph away from the liver
|
|
|
What are the contents of the hepatic portal vein blood from the intestine?
|
Nutrients and toxic substances
|
|
|
What are the contents of the hepatic portal vein blood from the pancreas?
|
Endocrine secretions like insulin and gluagon
|
|
|
What are the contents of the hepatic portal vein blood from the spleen?
|
Breakdown products of the blood cells
|
|
|
How does blood gain access to the hepatocytes?
|
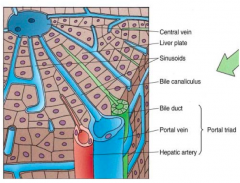
Arterial capillaries and inlet venules carry blood from the hepatic artery and portal veins into a network of sinusoidal capillaries (sinusoids)
|
|
|
What is the portal triad? How much blood is contributed by these components?
|
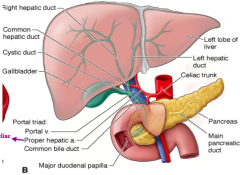
Combination of branches of:
- Hepatic artery (30%) - Hepatic portal vein (70%) - Common bile duct (also associated with lymphatic vessels) |
|
|
What is the flow of blood through the portal triad and the hepatocytes?
|
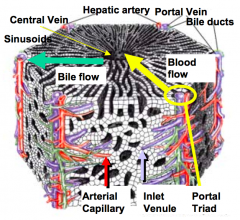
- Blood from hepatic arteries and portal veins flows through the sinusoids toward the central vein
- Efferent blood leaves through the central vein to join the vena cava - Flow past the hepatocytes allows for exchange of substances |
|
|
What kind of capillaries are in the hepatocytes? Function?
|
Sinusoidal (type III) - allows the exchange of substances between the blood and hepatocytes
|
|
|
What are the types of cells in the sinusoids of the liver?
|
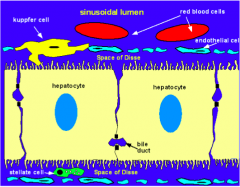
- Endothelial cells (sometimes called sinusoidal cells)
- Sinusoidal macrophages (Kupffer cells) |
|
|
What are Kupffer cells derivatives of? Function?
|
- Monocytes (they are aka sinusoidal MACROPHAGES)
- Possibly involved in breakdown of senile RBCs |
|
|
Which cells are possibly involved in the breakdown of senile RBCs?
|
Kupffer cells (aka sinusoidal macrophages)
|
|
|
What are the characteristics of the endothelium lining the sinusoids?
|
- Discontinuous to
- Allows unobstructed transfer of plasma and its substrates to the hepatocytes and endocrine secretions from the hepatocytes to the blood - Large spaces are evident between endothelial cells and there is no continuous basal lamina |
|
|
What is found within the sinusoidal lining?
|
Large numbers of fenestrae that are arranged as sieve plates
|
|
|
Where does exchange of substances between blood and hepatocytes take place?
|
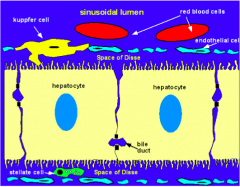
Peri-sinusoidal Space of Disse
|
|
|
Where is the peri-sinusoidal Space of Disse?
|
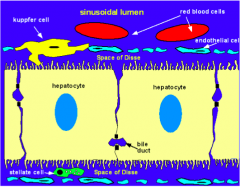
Lies between the basal surface of the hepatocyte and the sinusoid
|
|
|
What special feature is found on hepatocytes? Function?
|
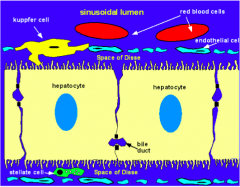
Microvilli on basal surface which increases the surface area available for substance exchange
|
|
|
Why do hepatocytes have microvilli?
|
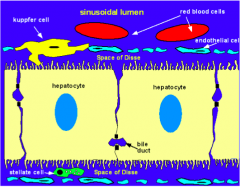
To increase the surface area available for substance exchange
|
|
|
What is commonly found in the peri-sinusoidal Space of Disse?
|
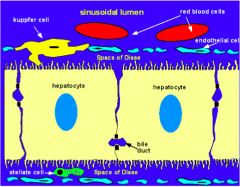
Stellate cells (Ito cells / adipose / lipocytes)
|
|
|
What is the structure and function of Stellate cells (Ito cells / adipose / lipocytes)?
|
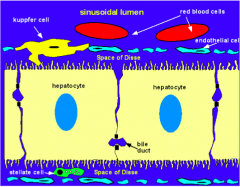
- Commonly found in peri-sinusoidal Space of Disse
- Often contain large lipid droplets - Major site of vitamin A storage |
|
|
What is the term for the "functional units" of the liver? What are the types?
|
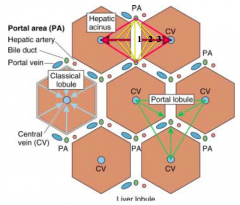
Lobules:
- Classic lobule - Portal lobule - Liver acinus |
|
|
What is the shape of the Classic Lobule? Organization?
|
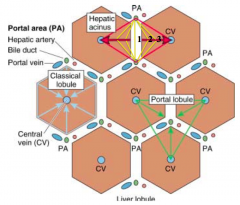
- Hexagonal block of tissue
- Single central vein at core - Portal triad at each of the 6 corners - Sinusoids and hepatic plates radiate toward the portal triads |
|
|
How do you identify the classic lobule in pig livers? Human livers?
|
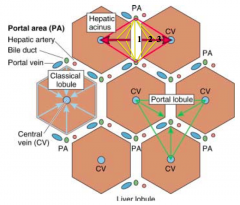
- Pigs: presence of CT surrounding each lobule
- Humans: very little interlobular CT, which makes it difficult to identify |
|
|
What is at the center of a classic lobule?
|
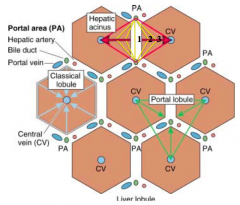
Single central vein
|
|
|
What is at the corners of the hexagonal classic lobule?
|
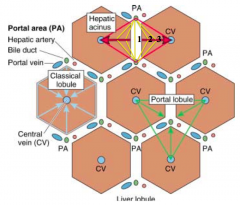
Portal triad: branches of the portal vein, hepatic artery, and bile duct
|
|
|
What radiates from the central vein to the portal triad at each corner of the hexagonal classic lobule?
|
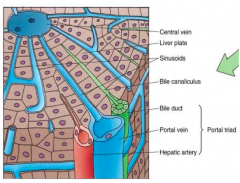
Sinusoids and hepatic plates
|
|
|
What is the shape of the liver acinus? Organization?
|
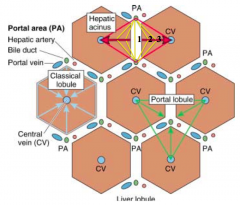
- Lozenge shaped
- Short axis formed between two adjacent portal triads - Long axis formed between adjacent central veins |
|
|
What does the liver acinus correlate with?
|
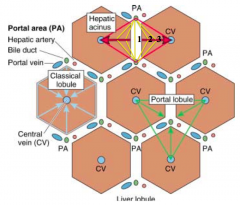
- Liver acinus closely correlates with blood perfusion, metabolic activity, and liver pathology
- It allows description of patterns of hepatocyte cell death and regeneration following toxicity |
|
|
What is the flow of oxygenated nutrient / toxin rich blood through the classic lobule?
|
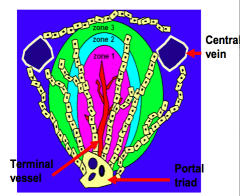
- Blood perfuses from the terminal vessel toward the central vein
- Produces a gradient of nutrients and substances encountered by hepatocytes |
|
|
What is the organization of the zones in the acinus?
|
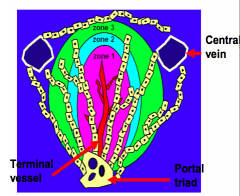
Three concentric zones surrounding a terminal vessel
- Zone 1: encounters afferent blood first - Zone 2: second - Zone 3: last (most susceptible to ischemia) |
|
|
How do the three zones of the acinus differ?
|
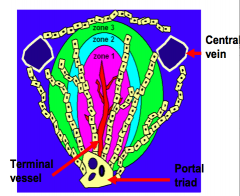
Differ with respect to metabolic activity, glycogen storage, and presence of organelles
|
|
|
Acetaminophen toxicity damages which part of the acinus?
|
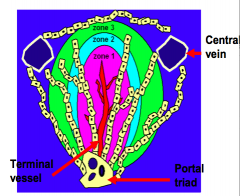
Zone 3
|
|
|
What is the principal functional cell of the liver?
|
Hepatocyte
|
|
|
How are hepatocytes organized?
|
- Makes up the liver parenchyma
- Arranged in anastomosing plates 1-2 cells thick separated by sinusoids - Plates of hepatocytes run from central vein out toward the portal triads |
|
|
What shape are hepatocytes? Size?
|
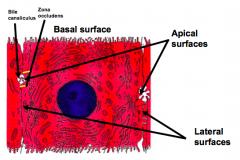
- Large polyhedral cells
- 30 µM wide - Six surfaces - two faces the perisinusoidal space and four face other hepatocytes and the bile canaliculi |
|
|
What do the peri-sinusoidal surfaces of hepatocytes face?
|
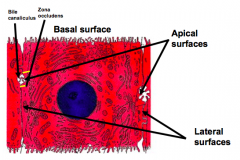
They represent the basal aspect of the cell
|
|
|
What sides of the hepatocytes face other hepatocytes?
|
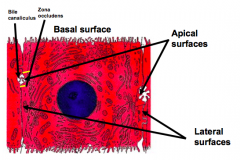
Lateral surfaces
|
|
|
What sides of the hepatocytes face bile canaliculi?
|
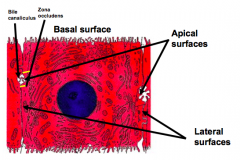
Apical surfaces
|
|
|
Where does transfer of substances between sinusoids and hepatocytes occur?
|
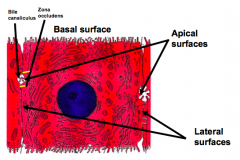
Across the basal surface (peri-sinusoidal surface)
|
|
|
What is the shape/organization of the nuclei in hepatocytes?
|
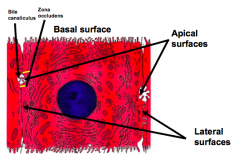
- Large spherical nucleus located in the center of the cell
- Majority are binucleate and are tetraploid (contain 4n DNA) |
|
|
What are the features of the organelles in hepatocytes?
|
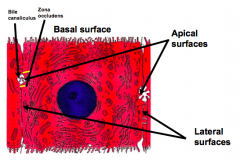
- Extremely rich in organelles
- Reflects their high metabolic activity - Particularly high in RER and mitochondria - Glycogen granules are deposited throughout the cytoplasm - Lipid droplets are also prevalent |
|
|
How can we prove that liver regeneration occurs?
|
Partial hepatectomy (in rodents):
- Intact lobes of the liver are removed, leaving a single intact lobe behind - Cells in the remaining lobe re-enter the cell cycle and begin to proliferate - Dissected lobes do not grow back, instead the residual lobe enlarges enough to make up for the mass of the removed lobes |
|
|
What cells regenerate after a partial hepatectomy?
|
All liver cell types:
- Hepatocytes - Biliary epithelial cells - Sinusoidal endothelial cells - Kuppfer cells - Stellate cells |
|
|
How long does the regeneration process from a partial hepatectomy take in rats?
|
5-7 days
|
|
|
How does liver regeneration occur in humans?
|
- During regeneration, normal liver function is maintained
- Liver mass is precisely regulated by both positive and negative signals - Several growth factors have been identified that play crucial roles in regulating regeneration |
|
|
What are the problems with hepatocyte transplantation?
|
- Recovering enough normal donor hepatocytes that are acceptable by the host
- Donor hepatocytes from another individual will be rejected by the host without prolonged immune suppression |
|
|
What would be the ideal way to transplant hepatocytes?
|
- Isolate hepatic stem cells from an afflicted individual
- Expand them in culture - Genetically modify to correct the defects - Corrected cells could be returned to the patient whereby they could replace diseased hepatic tissues |
|
|
Where are oval cells found? Characteristics?
|
- Rare population of cells present in the biliary epithelium
- Characteristics of a stem cell, an undifferentiated cell capable of self renewal, proliferation, and production of differentiated progeny - Bipotential - differentiate to form both biliary epithelial cells and hepatocytes |
|
|
What can oval cells become? Why?
|
They can differentiate to form both biliary epithelial cells and hepatocytes because they are bipotential
|
|
|
What happens during chronic liver damage when hepatocyte function and replication is severely compromised?
|
Oval cells proliferate and differentiate
|
|
|
How does bone marrow relate to oval cells?
|
- Transplanted BM has been shown to give rise to oval cells
- May provide a source of hepatic stem cells that are bipotential (can proliferate into biliary epithelial cells and hepatocytes) |
|
|
More recently, what have pluripotent stem cells been derived from? How can this be used for liver regeneration?
|
- Pluripotent stem cells have been derived from human fibroblasts
- They have been used to generate hepatocyte-like cells that could one day be used to treat human hepatic disease |
|
|
What is the main exocrine function of the liver?
|
Production of bile
|
|
|
What are the functions of bile salts?
|
- Emulsification - decreases surface tension and breaks fat globules into smaller size particles
- Forms micelles (soluble in chyme) and helps absorption of fat breakdown products (FA, monoglycerides, and cholesterol) |
|
|
Where is bile produced? How is it excreted?
|
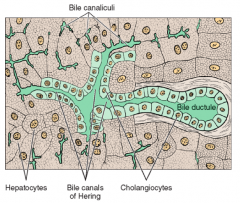
- Hepatocytes produce bile
- Bile is actively secreted by ATPases across their apical surface into the bile canaliculi |
|
|
What is found in the bile canaliculi (where bile is excreted after being produced by hepatocytes)?
|
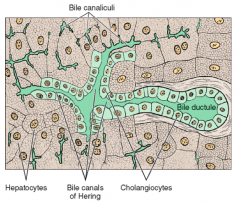
ATPases - which means that bile secretion is an active process
|
|
|
What is the organization of bile canaliculi?
|
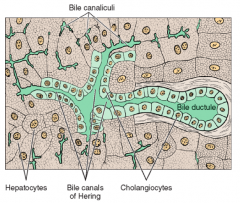
The canaliculi join together to form small terminal ductules called Canals of Herring
|
|
|
What are bile ducts made of?
|
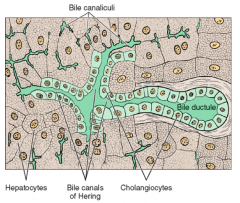
- Biliary epithelial cells
- Cuboidal epithelium which forms a ductule |
|
|
How does bile flow compare to blood flow?
|
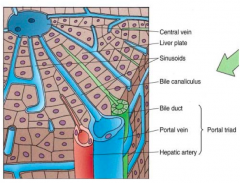
Bile flows in the opposite direction of the blood, i.e., away from the central vein toward the portal triad
|
|
|
Where do bile ducts lead?
|
Lead from the portal triad to join the hepatic duct that carries the bile to the gallbladder
|
|
|
How much bile is secreted by the liver per day?
|
1 L
|
|
|
What is the function of the gallbladder?
|
- Concentrates the dilute bile that comes from the liver 5-10x
- Stores up to 100 mL of bile / day |
|
|
What stimulates gallbladder contraction and release of bile into the duodenum?
|
- The presence of lipid in the duodenum induces secretion of the hormone CCK
- CCK: cholecystokinin-pancreozymin |
|
|
What is the function of CCK?
|
Cholecystokinin-pancreozymin stimulates gallbladder contraction and forces concentrated bile out
|
|
|
What is the shape/structure of the gallbladder?
|
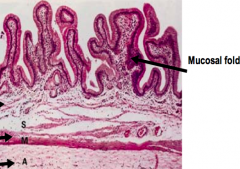
- Muscular sac
- Empty or distended GB has numerous deep mucosal folds |
|
|
What type of epithelium lines the gallbladder? Characteristics?
|
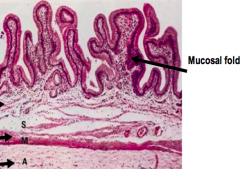
- Mucosa made of simple columnar epithelial cells
- Resembles the absorptive cells of the intestine - Cells have numerous short apical microvilli - Basally located nucleus |
|
|
How are the cells of the epithelium in the gallbladder connected?
|
Junctional complexes to produce a barrier between the luminal and intercellular compartments
|
|
|
What is the function of the epithelium of the gallbladder?
|
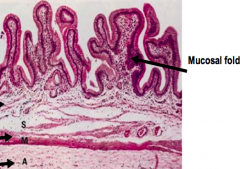
- Concentrate bile by actively absorbing water into a capillary rich network in the lamina
- Maintain a barrier between the luminal and intercellular components |
|
|
How big is the adult pancreas?
|
- 100-150 g
- 20-25 cm |
|
|
What are the parts of the pancreas? Location?
|
- Head: nestles within the concavity of the duodenum, which is C-shaped
- Body - Tail - Main pancreatic duct: traverses the length of the organ and joins the common bile duct before entering the duodenum |
|
|
What is the pancreas made of?
|
- Highly lobular
- Loose collagenous tissue separates the lobules as septa |
|
|
What is the path of the main pancreatic duct?
|
Transverses the length of the pancreas and joins the common bile duct before entering the duodenum
|
|
|
What are the functions of the pancreas?
|
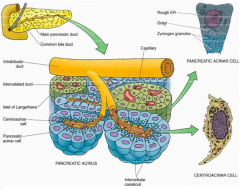
Exocrine (blue):
- Releases enzymes for digestion Endocrine (green): - Secretes hormones that control carbohydrate metabolism |
|
|
What is the organization of the exocrine pancreas?
|
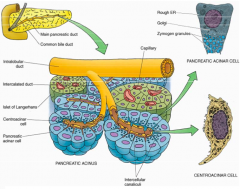
- Consists of densely packed Acini (blue)
- Secretes into a system of ducts: intercalated, intralobular, interlobular, and pancreatic - Ducts channel the pancreatic secretions into the pancreatic duct that leads to the dudoenum |
|
|
What is the organization of the endocrine pancreas?
|
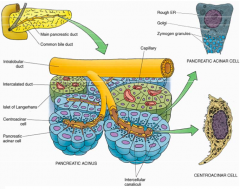
Consists of randomly distributed Islets of Langerhans (green) throughout the exocrine tissue (blue)
|
|
|
What does the exocrine pancreas release?
|
Enzymes involved in digestion in small intestine:
- Secretin - Cholecystokinin |
|
|
What hormones are released when the duodenum contains food? Function?
|
- Secretin
- Cholecystokinin - Induce secretion of pancreatic juice from the exocrine pancreas: contains alkaline fluid and enzymes and proenzymes (zymogens) required for digestion |
|
|
How are digestive enzymes stored in the exocrine pancreas?
|
Zymogen granules within the cytoplasm of acinar cells
- Granules allows them to be rapidly released into the gut after a meal - Zymogen form prevents their auto-digestion of pancreatic tissues - Stored with proteolytic inhibitors that block any errant activation of proenzymes in the pancreas |
|
|
How are the zymogen forms of digestive enzymes activated?
|
Proteolytic cleavage in the intestine
|
|
|
How does the pancreas ensure there is no auto-digestion of its tissues?
|
- Digestive enzymes exist in their proenzyme state (inactive) that only are activated in the intestine by proteolytic cleavage
- Proteolytic inhibitors are secreted by acinar cells to block any errant activation of the proenzymes |
|
|
What is the functional unit of the exocrine pancreas? Shape?
|
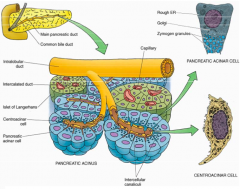
Acinus - roughly spherical containing 40-50 pancreatic acinar cells surrounding the lumen of a small ductule
|
|
|
What induces acinar cells to secrete pancreatic enzymes into the lumen?
|
Cholecystokinin, stimulated by fatty foods in the duodenum
ACh from vagus nerve is a weaker stimulus |
|
|
What is the organization and function of centroacinar cells?
|
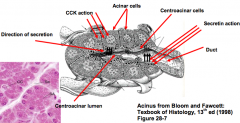
- Extend from the end of the duct into the acinus as a discontinuous epithelium
- Low squamous epithelial cells responsible for secretion of alkaline fluid component of pancreatic juice |
|
|
What induces centroacinar cells to secrete the alkaline fluid component of pancreatic juice?
|
Secretin
|
|
|
What is the function of Cholecystokinin?
|
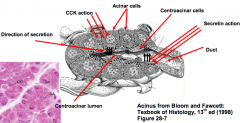
- Results in gallbladder contraction and emptying in under 1 hour
- Induces acinar cells to secrete pancreatic/digestive enzymes in the form of zymogen granules into the lumen - Relaxes Sphincter of Oddi |
|
|
What is the function of Secretin?
|
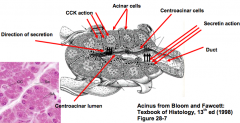
- Stimulates secretion of alkaline fluid, rich in sodium bicarbonate, from the centroacinar cells
- Helps neutralize acids and optimizes pancreatic function |
|
|
What is the importance of the alkaline fluid released from centroacinar cells?
|
- Solubilization of zymogen granules
- Helps neutralize acidic chyme as it enters the duodenum (prevents inactivation of enzymes and protects epithelium) |
|
|
What is the shape and organization of the acinar cells of the pancreas?
|
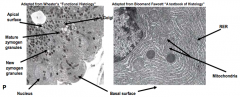
- Pyramidal shape
- Basally located nucleus - Cells are extremely active so the basal cytoplasm is packed with RER to synthesize exported proteins - Proenzymes are modified in the Golgi to form zymogen granules |
|
|
How are the zymogen granules released into the lumen?
|
Exocytosis at the apical surface of the acinar cell
|
|
|
How is pancreatic juice transported to the duodenum?
|
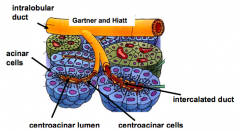
Network of pancreatic ducts:
- After entering the centroacinar lumen, juice moves through a series of Intralobular ducts - These ducts merge and transport the uice into the larger interlobular lobes - These then join the main pancreatic duct to transport the fluid to the duodenum |
|
|
What is the organization of the bile ducts in the liver and gallbladder?
|
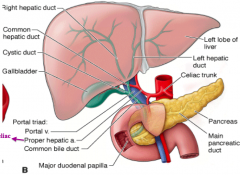
- R hepatic duct drains R lobe and L hepatic duct drains L lobe
- R and L hepatic ducts combine to form Common Hepatic Duct - Gallbladder drained by the Cystic Duct - Cystic Duct and Common Hepatic Duct combine to from the Common Bile Duct |
|
|
What does the round ligament separate? What is it a remnant of?
|
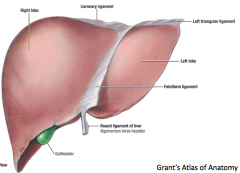
- Anatomically, the round ligament divides the left part of the liver into medial and lateral sections.
- The round ligament represents the remnant of the fetal umbilical vein. |
|
|
What does the coronary ligament of the liver do?
|
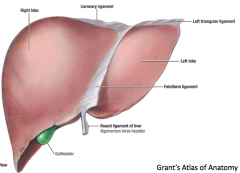
The coronary ligament of the liver refers to parts of the peritoneal reflections that hold the liver to the inferior surface of the diaphragm
|
|
|
What is the porta hepatis?
|
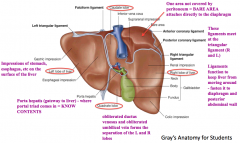
Gateway to the liver - where the portal triad enters the liver (portal vein, hepatic artery, and common bile duct)
|
|
|
What separates the right and left lobes of the liver?
|
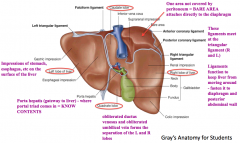
Obliterated ductus venosus and and obliterated umbilical vein
|
|
|
What area of the liver is not covered in peritoneum? What does this part attach to?
|
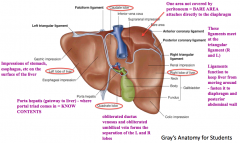
- The superior bare area on the right lobe
- Attaches directly to the diaphragm |
|
|
What are the functions of the ligaments on the liver?
|
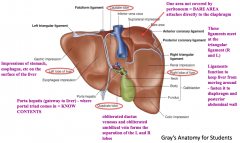
- Keeps the liver from moving around
- Fastens it to the diaphragm and posterior abdominal wall |
|
|
What is the function of the Left Triangular Ligament?
|
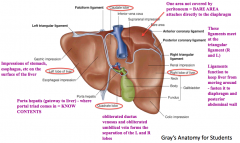
- Fold that connects the posterior part of the upper surface of the left lobe of the liver to the diaphragm
- Anterior layer is continuous with the left layer of the falciform ligament |
|
|
What is the location and function of the Right Triangular Ligament?
|
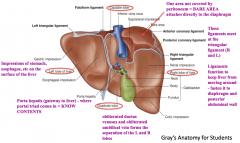
- Situated at the right extremity of the bare area
- Small fold which passes to the diaphragm - Formed by the apposition of the upper and lower layers of the coronary ligament |
|
|
If planning to resect part of the liver, how do you approach the task?
|
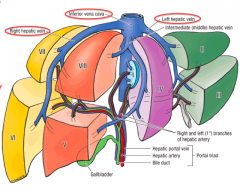
Hepatic Segments: based on arterial, venous, and biliary supply, in addition to the drainage of the liver
|
|
|
What drains the liver?
|
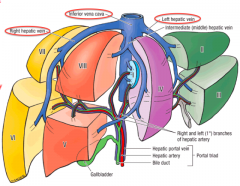
Hepatic veins (right, middle, and left) that empty into the IVC
|
|
|
What separates the L and R lobes clinically?
|
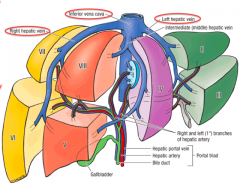
Middle hepatic vein
|
|
|
What do the segments of the liver represent?
|
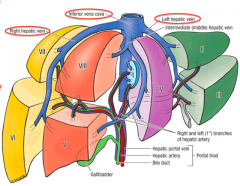
- Caudate lobe: segment 1
- L lobe: segments 2, 3, and 4 - R lobe: segments 5, 6, 7 and 8 |
|
|
What is special about segment 1 of the liver?
|
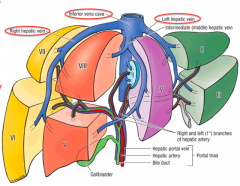
- Represents the caudate lobe
- Receives arterial and venous blood from both R and L sides - Directly empties into the IVC |
|
|
If you are transplanting a liver, which segments do you take?
|
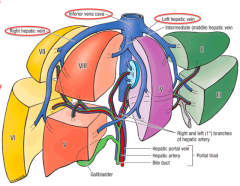
- Adult: R lobe (segments 5, 6, 7 and 8)
- Child: part of L lobe (segments 2 and 3) |
|
|
What is the route of bile from the gallbladder to the small intestine?
|
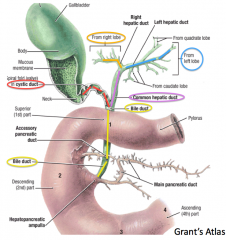
- Cystic duct drains gallbladder
- Flows into Bile duct - Empties into Duodenum at the hepatopancreatic ampulla |
|
|
What is the flow of blood leaving the midgut?
|
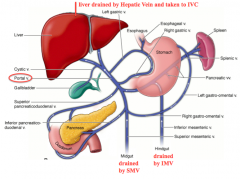
- Branches of Superior Mesenteric Vein
- Flows into the Portal Vein to the liver - Flows through Hepatic Sinuses - Enters IVC via Hepatic Veins |
|
|
What is the flow of blood leaving the hindgut?
|
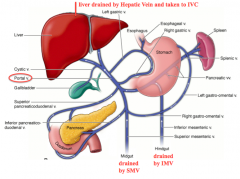
- Branches of Inferior Mesenteric Vein
- Flows into the Portal Vein to the liver - Flows through Hepatic Sinuses - Enters IVC via Hepatic Veins |
|
|
What can happen to the portal circulation if there is liver disease?
|
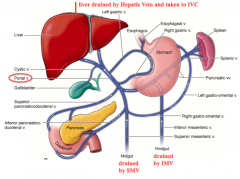
Liver disease can cause blood flow to back up and reverse direction to the spleen, causing the spleen to enlarge
|
|
|
How does fresh blood get to the liver? What percent of the blood comes via this route?
|
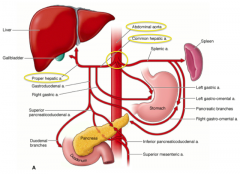
- Abdominal aorta supplies the Celiac Trunk
- The common hepatic artery is one of the branches - The proper hepatic artery and R and L hepatic arteries enter the liver and supply 30% of the total blood |
|
|
Once blood enters the liver via the hepatic artery or the portal vein, how does it flow through the liver?
|
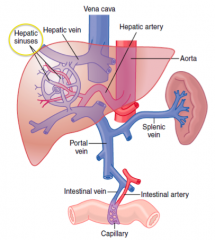
- The blood flows through the hepatic sinuses / sinusoids
- Blood leaves via the hepatic vein to get to the IVC |
|
|
What kinds of cells line the bile canaliculi?
|
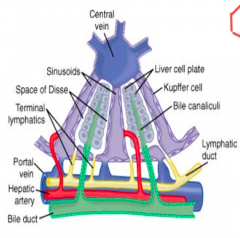
Liver cell plates
|
|
|
Where is the space of Disse?
|
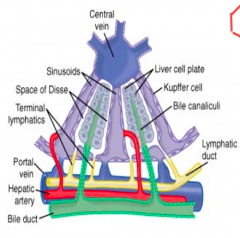
Located between the sinusoids and the liver cell plates that line the bile canaliculi
|
|
|
How does the concentration of bile in the liver compare to that in the gallbladder? How does this change occur?
|
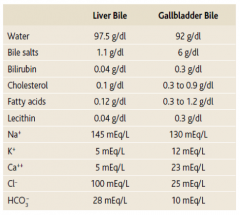
- Liver bile is more dilute than gallbladder bile
- Bile is concentrated once it gets to the gallbladder via absorption of water, Na+, and Cl- - Leaves concentrated salts, cholesterol, lecithin, and bilirubin - Volume goes from 500 mL to 50 mL |
|
|
What happens to the volume of bile that leaves the liver to that which is stored in the gallbladder?
|
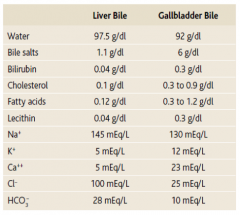
Volume goes from 500 mL to 50 mL via absorption of water, Na+, and Cl-
|
|
|
What happens to cholesterol and lecithin in the gallbladder?
|
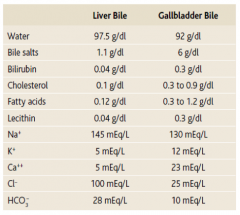
They are solubilized by bile salts
|
|
|
Where are bile acids reabsorbed?
|
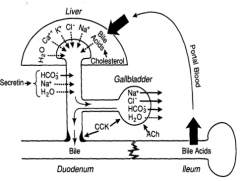
Ileum where they are taken via the portal blood back to the liver
|
|
|
What enzymes are released by the pancreas to digest proteins?
|
- Trypsinogen
- Chymotrypsinogen - Procarboxypeptidase All released in inactive form to prevent self-digestion |
|
|
How are the enzymes released from the pancreas to digest proteins activated?
|
- Trypsinogen is activated to Trypsin by Enterokinase
- Trypsin further activates Trypsinogen as well as converts Chymotrypsinogen to Chymotrypsin and Procarboxypeptidase to Carboxypeptidase |
|
|
What activates Trypsinogen to Trypsin?
|
- Enterokinase
- Other Trypsin molecules |
|
|
What activates Chymotrypsinogen to chymorypsin?
|
Trypsin
|
|
|
What activates Procarboxypeptidase to Carboxypeptidase?
|
Trypsin
|
|
|
What prevents activation of the pancreatic enzymes?
|
Trypsin inhibitor prevents activation until secretions reach the small intestine
|
|
|
What are the three forms of carbohydrates in our diet?
|
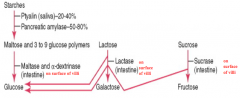
- Starches
- Lactose - Sucrose |
|
|
How do you digest starches?
|
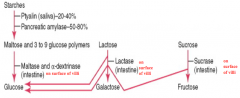
Starch → Maltose and 3-9 glucose polymers
- Ptyalin from the saliva (20-40%) - Pancreatic Amylase from the pancreas (50-80%) Maltose and 3-9 glucose polymers → Glucose - Maltase and α-dextrinase from the intestine |
|
|
How do you digest lactose?
|
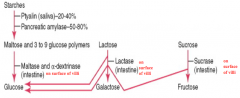
Lactase from the intestine breaks Lactose down into Galactose and Glucose
|
|
|
How do you digest Sucrose?
|
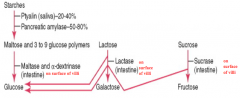
Sucrase from the intestine breaks down Sucrose into Fructose and Glucose
|
|
|
What is the form of the dietary fats?
|
- Majority are Triglycerides (TG): glycerol nucleus + 3 FA side chains
- Small amounts of Phospholipids, Cholesterol, and Cholesterol Esters |
|
|
What digests Triglycerides?
|

Pancreatic Lipase - can digest all TG it can reach within 1 minutes (requires emulsification by bile salts)
|
|
|
What is the function of Pancreatic Lipase?
|

Digests Triglycerides into Free Fatty Acids and 2-Monoglycerides
|
|
|
How do you digest Phospholipids?
|
Phospholipase
|
|
|
How do you digest Cholester esters?
|
Cholesterol Esterase
|
|
|
What happens to the digested fat remnants?
|
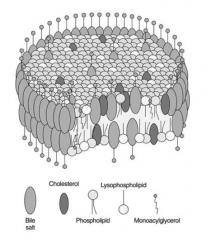
Bile salts form micelles and remove monoglycerides and fatty acids and transports them to the brush border for absorption
|
|
|
Where is bicarbonate secreted from?
|
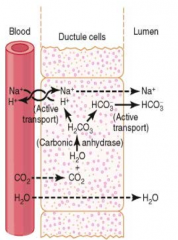
Bile ducts and pancreatic ducts
|
|
|
How does bicarbonate get formed?
|
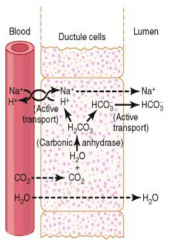
- CO2 diffuses in and combines with H2O to form H2CO3
- H2CO3 breaks down to form H+ and HCO3- - HCO3- goes into the lumen and associates with Na+, which causes a gradient into the lumen with water |
|
|
Which hormone has the greatest effect on Sphincter of Oddi relaxation?
|
Cholecystokinin
|
|
|
In a 40-yo male with Hepatitis C, which hepatic acinus zone would be exposed to the greatest number of viral particles?
|
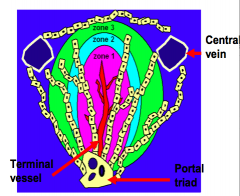
Zone 1 (this receives the greatest amount of blood flow)
|
|
|
Which zone of the hepatic acinus would be affected most by ischemia?
|
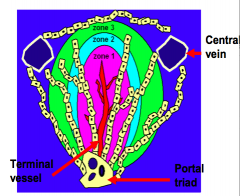
Zone 3
|

