![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
26 Cards in this Set
- Front
- Back
|
What is the optimal blood pH of the human body
|
7.4 a slight change in pH can lead to death
|
|
|
what will happen if pH is low and CO2 is high
|
some causes can be possible lung disease acidosis as well as lactic acid build up and ketone body diabetes
|
|
|
what are the main functions of blood
|
transport oxygen and nutrients removes CO2 and other by products of cell activity help maintain homeostasis growth and tissue repair and defense against infection and participates in hemostasis and participlates in body heat distribution and regulation
|
|
|
what is the composition of blood
|
the formed element red blood cells and white blood cell and platelets
plasma water electrolytes, proteins carbohygrates and lipid and plasma proteins |
|
|
hematocrit and how to perform it
|
it is the percentage of RBC out of the total blood volume to do this you fill the tube centrifuge for five minutes measure total volume and then divide the total volume of RBC by that volume and multiply by 100
|
|
|
why are blood cells shaped the way the are
|
it is a concave in shape to increase surface area to bind hemoglobin to function as a more efficent gas exchanger and has no nucleus
|
|
|
What are the types of white blood cells are leukocytes
|
two main types
Granulocytes -->neutrophils oxidize bacteria --> eosinophils, attack parasites -->basophils hypersensitivity reaction |
|
|
which of the WBC are the most commpn
|
neutrophils
|
|
|
in the blood lab what method did you use to perform an blood analysis
|
wright stain method apply stain for 1 min add water for two minutes rinse off with water and blot it with bibulous paper
|
|
|
name the main composition of blood
|
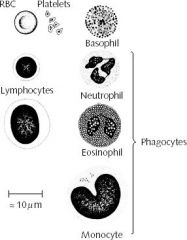
|
|
|
hopw to you measure frequency of a wave
|
1/# of periods
|
|
|
how to find beats per minute measuring a recording of someones heart rate
|
find # of interals/time multiplied by 60 secs
|
|
|
what is a force transducer
|
it is a device used to measure the electrical signal produced by the heart
|
|
|
name the main composition of blood
|
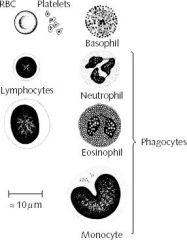
|
|
|
How is the anatomy of cardiac muscle cells different from skeletal and smooth muscle cells
|
1) consist of interlacing bundles like skeletal muscle it is straited but cardiac muscle is narrower and shorter and more rectangular than smooth muscle
2. single nucleus 3. irregularly spaced between dark bands intercalated disc that glue cells together to allow electrical signals to pass through gap junctions makiing the cardiac muscle a functional syncytium |
|
|
Excitation-contraction coupling (ECC)
|
is the process whereby an action potential triggers a myocyte to contract. When a myocyte is depolarized by an action potential, calcium ions enter the cell during phase 2 of the action potential through L-type calcium channels located on the sarcolemma. This calcium triggers a subsequent release of calcium that is stored in the sarcoplasmic reticulum (SR) through calcium-release channels
|
|
|
how is heart stimulated and inhibited
|
norepinephrine increase rate as well as accelerator nerves connected to SA and AV nodes
the heart in inhibited by Ach and vagus nerve connected to SA and AV nodes |
|
|
atropine
|
atropine blocks the action of the neurotransmitter acetylcholine at all the nerve endings where the membrane receptors are of the so-called muscarinic type. This includes those of the parasympathetic nervous system in the heart, glandular tissue, and smooth muscle. Thus atropine causes a rise in heart rate and inhibits secretions
|
|
|
Stretching of the heart effects on cardiac output
|
this is consider the autoregulation by the ventricle filling you get more blood in you can get more blood out this is the ventricular end diastolic pressure the degree of stretch of the ventricular muscle cells just before they contract
|
|
|
define contractility
|
the intrinsic strength of cardiac muscle
|
|
|
effects of ach on cardiac output
|
Heart is inhibited by the parasympathetic cardio- inhibitory center releases Ach decreases heart rate and prolongs delay at AV node has little effects on contractility
|
|
|
explain the dual effect of Norepinephrine on cardiac output
|
basically you will increase cardiac output by increasing the heart rate, but at the same time decreasing it because the ventricles have less time to fill causing a decrease in stroke volume
|
|
|
what is agonist
|
produces the action antagonist opposes the action
|
|
|
adrenergic receptors
|
Sympathetic adrenergic nerves innervate the SA and AV nodes, conduction pathways, and myocytes in the heart. These adrenergic nerves release the neurotransmitter norepinephrine (NE), which binds to specific receptors in the target tissue to produce their physiological responses. Neurotransmitter binding to receptors activates signal transduction pathways that cause the observed changes in cardiac function.
|
|
|
cholinergic receptors
|
the heart is innervated by parasympathetic cholinergic nerves derived from the vagus nerves. Acetylcholine (ACh) released by these fibers binds to muscarinic receptors in the cardiac muscle, especially at the SA and AV nodes that have a large amount of vagal innervation. ACh released by vagus nerve binds to M2 muscarinic receptors, a subclass of cholinergic receptors. This produces negative chronotropy and dromotropy in the heart, as well as negative inotropy and lusitropy in the atria (the negative inotropic and lusitropic effects of vagal stimulation are relatively weak in the ventricles).
|
|
|
what are the three determinant factors the effect blood flow
|
length of blood vessel diameter and viscosity the most quantitatively important is the radius very small changes in the diameter leads to large changes in resistance
|

