![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
430 Cards in this Set
- Front
- Back
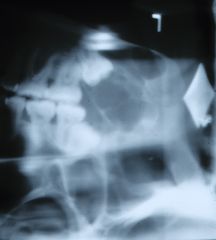
What is the most common clinically significant odontogenic neoplasm? |
Infiltrating Ameloblastoma
|
|
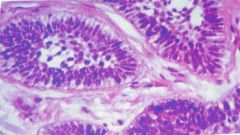
-Posterior mandible |
Conventional ameloblastoma
Benign aggressive neoplasm |
|
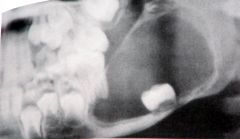
< 30 yrs
Differential diagnosis? |
Unicystic Ameloblastoma
Dentigerous Cyst |
|
|
Extraosseous form of ameloblastoma found in middle age adults?
|
Peripheral ameloblastoma
|
|
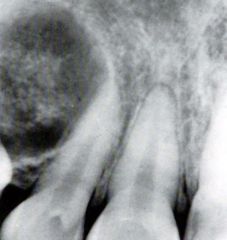
-Late mixed dentition
-75% associated w/ unerupted tooth -Never found in posterior jaws |
Adenomatoid Odontogenic Tumor
|
|
|
Cleft lip is the defective fusion of the _______ w/ the ______
|
CLEFT LIP is the defective fusion of the MEDIAL NASAL PROCESS w/ the MAXILLARY PROCESS
|
|
|
Cleft palate is the failure of _____ to fuse?
|
CLEFT PALATE is failure of PALATAL SHELVES to fuse
|
|
|
Which is most common?
-Isolated cleft lip? -Isolated cleft palate? -Cleft lip & palate? |
Cleft lip & palate is most common
-CL more common in males -CP more common in females -70% of unilateral CL occurs on left |
|
|
What is the minimal manifestation of cleft palate?
|
Bifid uvula
|
|
|
What are the 3 characteristic features of Pierre-Robin syndrome?
|
1. Cleft palate
2. Migrognathia 3. Glossoptosis |
|
|
Possible failure of normal fusion of embryonal maxillary & mandibular process?
|
Commisural lip pits
|
|
|
Possible persistence of lateral sulci on embryonic mandibular arch?
|
Paramedian lip pits
|
|
|
3 mm diameter & 2.5 mm depth depressions located bilaterally to midline of lower lip?
|
Paramedian lip pits
|
|
|
Double lip occurs in associated w/ which syndrome?
|
Ascher's syndrome
1. Double lip 2. Blepharochalasis 3. Non-toxic thyroid enlargement |
|
|
Mucosal tissue that projects from maxillary labial frenum?
|
Frenal tag
|
|
|
Multifocal yellow spots which are ectopic sebaceous glands?
|
Fordyce granules
|
|
|
Etiology of Fibromatosis GIngivae?
|
-Hereditary (auto dom)
-Associated w/ syndromes (hypertrichosis, craniofacial deformities, epilepsy & mental retardation) -Idiopathic |
|
|
-Dense, diffuse, smooth/nodular overgrowth of gingival tissue
-Normal color, not painful, no bleeding -Commonly in maxilla -Before age 20 |
Fibromatosis Gingivae
|
|
|
History of fibromatosis gingivae reveals that the tissue is :
Inflammed? Not inflamed? |
NO inflammation-- only fibrous hyperplasia
|
|
|
Migrognathia can be seen with which 2 congenital abnormalities?
|
-Congenital heart disease
-Pierre-Robin syndrome |
|
|
Macrognathia is associated w/ which 3 diseases?
|
1. Paget disease of bone
2. Acromegaly 3. Fibrous dysplasia |
|
|
Rare condition characterized by unilateral enlargement of body or parts of body?
|
Hemihyperplastia
|
|
|
Possible etiologies of hemihyperplastia? (4)
|
1. Vascular/lymph
2. Neurogenic 3. Hormonal (endocrine) 4. Chromosomal 5. Neoplasms (Wilm's tumor) |
|
|
Uncommon degenerative condition characterized by atrophic changes affected one side of face?
|
Progressive Hemifacial Atrophy
-Etiology: 1. Malfunction of nervous system 2. Trauma 3. Infection 4. Hereditary 5. Scleroderma |
|
|
Syndrome that presents w/ hemifacial atrophy, facial parasthesia, contralateral epilepsy & trigeminal neuralgia?
|
Romberg syndrome
|
|
|
Painless, unilateral enlargement of maxillary bone in bicuspid area during childhood?
-May be missing bicuspids -May have defects in primary teeth -Thickened bone trabecula |
Segmental Odontomaxillary dysplasia
|
|
|
Macroglossia can be caused by? (4)
|
1. vascular malformation (hemangioma, lymphangioma)
2. Hemihypertrophy 3. Down syndrome 4. Neurofibromatosis |
|
|
Fusion between tongue & floor of mouth causing a short lingual frenum?
|
Ankyloglossia
|
|
|
Which condition often develops simulatenously w/ benign migratory glossitis?
|
FIssured tongue
|
|
|
Multiple areas of tongue devoid of filiform papillae, outlined by yellow-white line which may be sensitive?
|
Benign Migratory glossitis
|
|
|
Benign migratory glossitis histologically resembles which disease?
|
Psoriasis
|
|
|
-Acummulation of keratin on filiform papillae
-Asymptomatic -Brown/black pigmentation |
Hairy tongue
|
|
|
Enlarged/tortuous vein on lingual surface of tongue
-2/3 of pt over 60 yr |
Lingual varices
|
|
|
Failure of normal development migration of thyroid gland?
|
Lingual thyroid nodule
|
|
|
Smooth, nodular "meaty mass" near foramen caecum?
|
Lingual thyroid nodule
|
|
|
Which type of biopsy should be performed on lingual thyroid nodule?
|
Incisional
|
|
|
Made up of Lymphoid tissue that includes:
-Palatine tonsils -Pharyngeal tonsils -LIngual tonsils -Foliate papilla |
Oral tonsil (Waldeyer ring)
|
|
|
Lateral lingual tonsil (foliate papilla) may be a site of?
|
malignant lymphoma
|
|
|
4mm raised pink area of mucosal gingival tissue lingual to mandibular cuspids usually bilateral?
|
Retrocuspid papilla
|
|
|
Only minor salivary gland in the mouth that is serous?
|
Circumvallate papillae
|
|
|
Enamel hypoplasia of a single tooth caused by local infection or trauma?
|
Turner's tooth
|
|
|
Incomplete or defective formation of organic enamel matrix of teeth that results in pits, grooves or larger areas of missing enamel?
|
Enamel hypoplasia
|
|
|
Defective mineralization of formed enamel matrix?
-Abnormal color (increased white opacities) -Soft enamel, abrades easily -Not especially caries susceptible |
Enamel hypocalcification
-Low mineral content, high organic content |
|
|
At what age is exposure to excess fluoride most critical to the teeth?
|
2-3 yrs
|
|
|
Physiologic wearing away of tooth structure as a result of tooth to tooth contact?
|
Attrition
|
|
|
Pathologic wearing away of tooth structure by abnormal mechanical processes?
|
Abrasion
-V shaped |
|
|
Wedge-shaped defect at cervical area of tooth?
|
Abfraction
|
|
|
Loss of tooth structure by non-bacterial chemical action?
|
Erosion
|
|
|
Pink tooth of Mummery is a sign of?
|
Internal resorption
|
|
|
Small, localized masses of calicified tissue having structures resembling dentinal tubules
|
True Denticles
-Free-- not attached to dentinal wall -Attached-- attached to dentinal wall (most common) |
|
|
Localized masses of calcified tissue w/ no dentinal tubules?
|
False denticles (dystrophic calcification)
|
|
|
Brown-black stain found on lingual, cervical 1/3 of teeth
-May penetrate into exposed dentin/cementum |
Tobacco stain
|
|
|
-Dark/brown stain along gingival 1/3 facial & lingual (rarely max ant)
-Usually clean teeth w/ low caries -Females, children, recurs |
Black stain
|
|
|
Etiology of Yellow dull discoloration
-All ages |
Food pigments
|
|
|
-Thick "furry" deposit cervical 1/3 of facial maxillary incisors in young
-Boys -Poor oral hygeine Ichromogenic bacteria, blood enzymes) |
Green stain
|
|
|
Intrinsic stain that turns teeth grey/brown due to breakdown of blood pigments?
|
Non-vital tooth (trauma)
|
|
|
Hemolytic anemia that causes blood pigments to be deposited in developing teeth
-Green, brown, blue staining -May have enamel hypoplasia --> ring-like defect near edges of incisors or middle of primary canines & first molars |
Erythroblastosis Fetalis
|
|
|
Intrinsic staining caused by destruction of bile ducts in neonatal period that give primary teeth green color?
|
Biliary Atresia
|
|
|
Overproduction of uroporphyrin causing:
-red urine -photosensitivity -red-brown discoloration of teeth -skin vesicles/bulla |
Congenital porphyria
|
|
|
Instrinsic stain that causes teeth become yellow-brown in band like fashion?
|
Tetracycline stain
-Contraindicated for chidlren less than 7 or pregnant women -Drug deposited during dentinogenesis |
|
|
Which teeth most commonly are affected by hypodontia?
|
1. Third molars
2. 2nd bicuspids 3. Maxillary lateral |
|
|
What is the most common supernumerary tooth?
|
Mesiodens- between centrals
|
|
|
2nd most common supernumerary tooth?
|
Maxillary 4th molar
|
|
|
Microdontia is seen in which diseases?
|
1. Pituitary dwarfism
2. Down syndrome |
|
|
Most commonly affected teeth by microdontia?
|
Peg lateral & 3rd molar
|
|
|
-Attempted division of single tooth germ
-Single enlarged tooth or joined tooth w/ NORMAL tooth count -One tooth w/ 2 crowns & 1 root |
Gemination
|
|
|
Fusion by union of 2 separate tooth germs
-Single enlarged tooth or joined tooth w/ MISSING tooth count |
Fusion
|
|
|
Teeth united by cementum
|
Concrescence
|
|
|
Anomalous structure projecting lingually from cingulum of maxillary incisor
-Usually contains pulp horn |
Talon cusp
|
|
|
Cusp-like elevation of enamel located in central groove on lingual ridge of buccal cusp of permanent bicuspids & molars?
|
Dens Evaginatus
|
|
|
Invagination in surface of tooth crown before calcification
-Max lat most common |
Dens in Dente
(Dens Invaginatus) |
|
|
Body of tooth enlarged at expense of roots (seen in x-ray only)
-"bull-like tooth" |
Taurodontism
|
|
|
Excess secondary cementum on root surfaces?
|
Hypercementosis
|
|
|
Angulation, bend or curvature in root/crown?
-Max incisors most common |
Dilaceration
|
|
|
3 classiciations of amelogenesis imperfecta
|
1. Hypoplastic
2. Hypocalcified 3. Hypomaturation |
|
|
Type of amelogenesis imperfecta in which enamel has not formed to full thickness?
|
Hypoplastic type
|
|
|
Type of amelogenesis imperfecta in which enamel is soft & can be easily removed but is normal thickness?
-Poorly mineralized & chips easily |
Hypocalcified type
|
|
|
Type of amelogenesis imperfecta in which enamel is normal thickenss but can be pierced by an explorer?
|
Hypomaturation type
|
|
|
Which type of dentinogenesis imperfecta occurs w/ osteogenesis imperfecta?
|
Type I
|
|
|
Which type of dentinogenesis imperfecta Never occurs w/ osteogenesis imperfecta?
|
Type II
|
|
|
Which type of dentinogenesis imperfecta is called the "Bradywine type" or shell teeth?
|
Type III
|
|
|
Which abnormality of teeth presents w/:
-Bell shaped teeth -Short roots -No pulp chambers -Amber color, enamel chips & roots fracture easily |
Dentinogenesis Imperfecta
|
|
|
Which abnormality of teeth presents w/:
-Normal enamel but thin dentin & large pulp chambers -Extremely short roots -Normal clinical appearnce |
Shell teeth (Type III dentinogenesis imperfecta)
|
|
|
Hereditary defect in dentin formation- coronal dentin & tooth color normal but root dentin abnormal (short & tapered roots)?
|
Dentinal Dysplasia (Type I)
|
|
|
Bulbous crowns, obliteration of pulp (thistle tube shaped pulps) w/ hereditary defect in dentin formation?
|
Dentinal dysplasia (Type II)
|
|
|
Localized, developmental distrubrance of several adjacent teeth in which enamel & dentin are thin, irregular & fail to adequately mineralize?
|
Regional Odontodysplasia
|
|
|
Abnormality of teeth that presents w/:
"Ghost like teeth" -Large pulp chambers -enamel layer not often evident -Delayed/total failure of eruption |
Regional Odontodysplasia
|
|
|
-Sensitive to cold/sweets
-Pain lasts 5-10 sec -Stimulus needed -Usually sensitivity to percussion absent |
Reversible pulpitis
|
|
|
-Very sensitive to cold/maybe hot
-Lingering pain (> 10 sec) -Spontaneous pain -May not be sensitive to percussion -May not be able to localized tooth |
Acute Irreversible pulpitis
|
|
|
-Mild, intermittent dull aching pain usually relieved by aspirin
-Reduced reaction to thermal change -May have fistulous tract -Pain may be intiate by lying down |
Chronic Irreversible pulpitis
|
|
|
-No true symptoms (painless or vague pain)
-Discoloration of crown -No reaction to pulp test |
Necrotic pulp
|
|
|
-Children, young adults
-Vital pulp -Painless except biting -Decidious molar, permanent 1st molar -Large caries -Tissue growing out of pulp Histo: granulation tissue |
Chronic hyperplastic pulpitis
|
|
|
-Localized, spontaneous excruiatiing pain
-Tooth in supraocclusion -No over swelling -Xray: no change/slight thickening of PDL |
Acute apical periodontitis
|
|
|
-Painful, rapid onset
-Pain to percussion -Adjacent teeth painful -Swelling -May have sinus tract -Nonvital tooth -Xray: wide PDL or large radiolucency |
Periapical abscess
|
|
|
Potential sequella of untreated abscess?
|
1. Cellulitis
2. Osteomyelitis 3. Parulis 4. Ludwig's angina 5. Cavernous sinus thombrosis |
|
|
-Painless
-Slow growing -Can develop into periapical cyst or abscess -Histo: Epithelial rests of Malassez, |
Chronic apical periodontitis (Dental granuloma)
|
|
|
Most common cyst of the jaws?
|
Periapical cyst (Radicular cyst)
|
|
|
How can a dental granuloma and radicular cyst be distinguished histologically?
|
Radicular cyst has squamous epithelium lining (usually w/o keratin)
|
|
|
-Radiopacity at apex of tooth w/ pulpitis
-Entire root outline visible -Usually mand 1st molar -No clinical symptoms -Children & young adults |
Condensing osteitis
|
|
|
Bilateral filmy milky opalescence on buccal mucosa that disappears when stretched?
|
Leukoedema
|
|
|
Most common papillary lesion of oral mucosa?
|
Squamous papilloma
|
|
|
-Cauliflower like soft lesion, usually solitary
-Palate & uvula (33% of lesions) -White or pink -HPV -Rare malignant transformation -Adults |
Squamous papilloma
|
|
|
-Finger-like projection, often multiple
-Contagious to other parts of the body -Keratin horn -HPV -Children & young adults -Vermillion border, labial mucosa, ant tongue |
Veruccous vulgaris
|
|
|
-STD & autoinoculation
-HPV -Up to 2 cm -Multiple papillary masses, white or pink -HPV 16 & 18- increase maligancy |
Condyloma Acuminatum
|
|
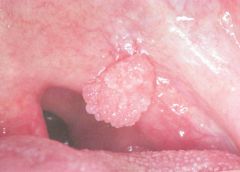
-Adult
-Solitary lesion on palate -Rare malignant transformation -Most common papillary lesion of oral mucosa |
Squamous papilloma
|
|
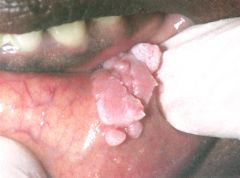
-Adult
-HPV -STD |
Condyloma acuminatum
|
|
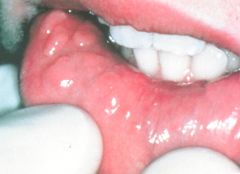
|
Focal epithelial hyperplasia
|
|
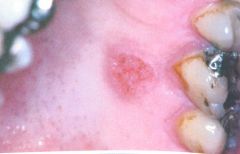
|
Verruciform Xanthoma
|
|
|
-Over 45 yrs
-Sun exposed skin (lower lip) -Elevated crater form lesion w/ keratin plug -Grows rapidly & regresses 6-12 months -Malignant transformation rare |
Keratoacanthoma
|
|
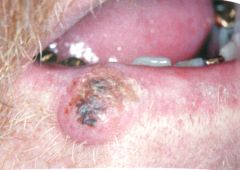
Differential?
|
Keratoacanthoma
SCC |
|
|
Thickened & corrugated white buccal mucosa
-Often bilateral -Childhood onset -Rare |
White sponge nevus
|
|
|
White patch that will not wipe off & is no other specific disease
|
Leukoplakia (clinical term)
|
|
|
Which clinical type of leukoplakia is not premalignant?
|
Frictional keratosis
|
|
|
Order of increasing malignancy of clinical types of leukoplakia?
|
1. Thin leukoplakia
2. Thick leukoplakia 3. Granular/nodular leukoplakia 4. Verrucous leukoplakia 5. Proliferative verrucous leukoplakia 6. Erythroleukoplakia 7. Speckled leukoplakia |
|
|
What % of oral leukoplakias become SCC?
|
5-16%
|
|
|
-White lesion on mucobuccal fold of mandible
-Smokeless tobacco user -Disappears when tobacco use is stopped -Low risk for malignant transformation |
Smokeless tobacco lesion
|
|
|
Chronic, progressive scarring premalignant condition of oral mucosa due to chornic placement of betel quid?
|
Oral submucous fibrosis
|
|
|
ASD murmur
|
fixed S2 splitting
|
|
|
-Premalignant lesion on sun-exposed sites
-Pt over 40, whites -Smooth White diffuse, scaly plaques |
Actinic Keratosis or Actinic Chelitis
|
|
|
Dysplasia is found in what % of leukoplakia lesions?
|
5-25%
|
|
|
What % of floor of the mouth leukoplakia are dysplasia, carcinoma in situ or SCC?
|
42%
|
|
|
What % of tongue & lip leukoplakias are dysplasia, carcinoma in situ or SCC?
|
24%
|
|
|
-Diffuse white papillary/warty lesions of buccal mucosa
-4:1 Female: male - Non-smokers -Persisent, multifocal, recurrent -High rate of transition to verrucous or squamous cell carcinoma |
Proliferative Verrucous Leukoplakia
|
|
|
Leukoplakia or erythroplakia more common?
|
Leukoplakia
|
|
|
What % of erythroplakias show dysplasia, carcinoma in situ or SCC?
|
60-90%
|
|
|
How many cases of oral cancer are estimated to occur each year?
|
22,000
|
|
|
How may people die of oral cancer every year?
|
5,300
|
|
|
Most common site for intraoral malignancy?
|
Tongue
|
|
|
Site w/ best survival rate for SCC?
|
Lips- 90% 5 yr survival
|
|
|
2nd most common site for intraoral malignancy?
|
Floor of mouth
|
|
|
5 yr survival for SCC of the tongue?
|
20-30%
|
|
|
5 yr survival for SCC of floor of the mouth?
|
40-50%
|
|
|
What is the overall 5 yr survival rate of SCC?
|
45-50%
|
|
|
-Slow growing, exophytic lesion
-Invades but doesn't metastasize -Low grade variant of SCC -Buccal mucosal vestibule or gingiva -Association w/ smokeless tobacco |
Verrucous carcinoma
|
|
|
Prognosis of verrucous carcinoma?
|
Excellent- 90% 5 yr survival
|
|
|
-Small scaly ulcer w/ rolled borders
-Slow growing -Over 40 -Middle third of face -Invades but doesn't metastasize |
Basal cell carcinoma
|
|
|
Darker pigmentation on attached gingiva
History of long duration May increase during pregnancy Increased melanin by melanocytes in basal cell layer |
Physiologic Pigmentation
|
|
|
-More common in females (esp. bc)
-Brown patches -Mand ant gingiva, buccal mucosa, palate -May disappear after quit smoking -Not premalignant |
Smoker's melanosis
|
|
|
-Any age
-Flat brown-black lesion -Lower lip (sun related) -less than 5 mm |
Ephelis
|
|
|
-Focal brown-black spot
-Oral mucosa (verm border & gingiva) -Does not enlarge after diagnosis -Not dependent on sun exposure -Not premalignant |
Oral melanotic macule
|
|
|
-History of long duration
-Brown lesion (does not blanch on pressure) -Palate, buccal mucosa -Less than 6 mm -No premalignant potential |
Pigmented cellular nevus
|
|
|
Nevus cells are probably derived from?
|
Neural crest
|
|
|
Most common human "tumor" but uncommon in oral cavity?
|
Pigmented cellular nevus
|
|
|
Nevus cells located at junction of epithelium & CT?
|
Junctional nevus
|
|
|
Nevus cells found along junctional area & within underlying CT?
|
Compound nevus
|
|
|
Nevus cells found only w/ in CT?
|
Intradermal (intramucosal nevus)
|
|
|
Most common intraoral nevi?
|
Intramucosal nevus
|
|
|
2nd most common intraoral nevi?
|
Blue nevus
|
|
|
Histo of blue nevus?
|
Spindle-shape cells deep within tissue
|
|
|
3rd most common skin cancer?
|
Malignant melanoma
|
|
|
Oral melanoma or skin melanoma has worse prognosis?
|
Oral melanoma has worse prognosis
|
|
|
Melanoma growth phase in which cells spread laterally but stay confied to the surface epithelium?
|
Radial growth phase
|
|
|
Melanoma growth phase in which cells invade & populate the connective tissue?
|
Vertical growth phase
|
|
|
Most common form of malignant melanoma?
|
Superficial spreading melanoma
|
|
|
Type of Melanoma w/ best prognosis?
|
Superficial spreading melanoma
|
|
|
Which type of melanoma has vertical growth which rapidly invades
-30% develop in head & neck region? |
Nodular melanoma
|
|
|
Which type of melanoma has radial growth phase (in situ) occurs exclusively on sun-exposed skin in midface? Develops from precursor lentigo maligna
|
Lentigo Maligna Melanoma
|
|
|
Most common form of melanoma in the oral cavity?
|
Acral lentiginous melanoma
|
|
|
Majority of malignant melanomas occur where?
|
Maxillary ridge & palate
|
|
|
Histology of malignant melanoma presents as?
|
Atypical melanocytic proliferation
|
|
|
-Destruction of adrenal cortex --> Decreased cortisol --> INcreased ACTH & MSH is present in which disease?
|
Addison's disease
|
|
|
Bronzing of the gingiva present in which disease?
|
Addison's disease
|
|
|
Syndrome w/:
-Oral & perioral melanotic macules -Intestinal polyposis (intussussecption) |
Peutz-Jeghers SYndrome
|
|
|
Most common intraoral soft tissue pigmentation?
|
Amalgam tattoo
|
|
|
Oral manifestations of plumbism (lead)?
|
-Lead sulfine line in gingiva
-Excessive salivation -Metallic taste -Swollen salivary glands |
|
|
-Thickened rough shredded white areas on buccal mucosa at occlusal plane
-Extensive hyperkeratosis -2x more in females -3x more common after 35 |
Morsicatio Buccarum (Chronic Cheek Chewing)
|
|
|
Injury w/ inflammatory host response but mucosal surface remains intact?
|
Traumatic mucositis
|
|
|
Fresh injury w/ broken mucosal surface & no significant host response yet
|
Traumatic laceration
|
|
|
Injury w/ loss of surface epithelum & w/ inflammatory host response
|
Traumatic ulceration
|
|
|
Persistent ulceration from chronic penetrating trauma to mucosa
|
Traumatic granuloma
|
|
|
Most common cause of focal oral ulceration?
|
Trauma
|
|
|
-Variant of traumatic ulcer
-Chronic deep ulcer occuring in mucosa over muscle (tongue) -Eosinophils |
Traumatic granuloma (Eosinophilic ulceration)
|
|
|
Treatment of traumatic granuloma?
|
If does not heal w/ in 10 days -2 weeks w/ conservative treatment --> MUST biopsy
|
|
|
Sites of predilection for thermal burns?
|
1. Anterior palate
2. Posterior buccal mucosa 3. Tip of tongue |
|
|
-Onset during 2nd week of radiation
-White surface w/ superficial sloughing -Residual atrophic epithelium red, swollen easily ulcerated -Pain burning & discomfort -Resolves 2-3 weeks after radiation |
Radiation mucositis
|
|
|
-Radiation pt
-Early signs: erythema, edema, burning, itching, frank ulcerations -Late/perm signs: hyperpigmentation, hair loss, scarring, chronic dermatitis |
Radiation dermatitis
|
|
|
Effects of xerostomia due to radiation therapy?
|
Progressive, permanent & irreversible loss of saliva
-Inreased risk of infection (candidiasis) -Increased caries incidence (radiation caries-cervical caries) |
|
|
-Treatment for cancer (somewhere other than head/neck)
-Epithelial atrophy, ulceration -Red, swollen background -Pain, burning & discomfort |
Chemotherapy mucositis
|
|
|
Inflammation of one or multiple fungiform papillae?
|
Transient lingual papillitis
|
|
|
-Type I hypersensitivity to drug
-Oral lesions & may include skin lesions & anaphylaxis |
Stomatitis Medicamentosa
|
|
|
-Type IV hypersensitivity
-Burning pain = most frequent symptom -Erythema w/ or w/o edema of mucosa |
Allergic contact stomatitis
|
|
|
Most commonly recognizable pattern of chronic reaction to restorative materials?
|
Lichenoid contact stomatitis
|
|
|
-Diffuse edematous swelling of soft tissues (upper lip, chin, tongue, around eyes)
-Rapid onset -Usually lasts 24-72 hrs |
Angioedema
|
|
|
Etiology of angioedema?
|
-Type I hypersensitivity
-Activation of complement pathways |
|
|
Syndrome characterized by triad of:
1. Oral ulcers 100% 2. Genital ulcers 75% 3. Ocular inflammation 90% |
Behcet syndrome
|
|
|
Which syndrome has:
-Parotid involvement -Anterior uveitis of the eye -Facial paralysis -Fever |
Heerfordt syndrome
|
|
|
-Nontender, persistent labial swelling
-May have swelling other parts of the face |
Chelitis granulomatosis
|
|
|
Non-tender labial swelling w/ vesicles, facial paralysis & fissured tongue
|
Melkersson-Rosenthal
|
|
|
-Necrotizing granulomatous lesions of respiratory tract, glomerulonephritis & systemic vasculitis of small arteries & veins
-Red, granular, hemorrhagic & friable attached gingiva |
Wegener Granulomatosis
|
|
|
Most common oral manifestation seen in HIV population?
|
Oral candidiasis
|
|
|
Treatment for simple oral candidiasis?
|
Nystatin
|
|
|
Treatment of candidiasis in immunocompromised host?
|
Oral- Mycelex
Systemic-Diflucan (fluconazole) Nizoral (ketoconazole-liver damage) |
|
|
What causes oral hairy leukoplakia?
|
EBV
|
|
|
-Rough, shaggy dense leukoplakia seen almost always bilateral & symmetric on lateral borders of tongue
-Corrugated surface w/ vertical extensions & irregular borders |
Oral hairy leukoplakia
|
|
|
Kaposi sarcoma is related to an infection by?
|
HHV-8
|
|
|
-Well circumscribed, red-purple-blue lesion
-Palate & ant max gingiva -Early-flat, Late-elevated -No surface ulceration |
Kaposi sarcoma
|
|
|
Oral lesions common in pt w/ non-hodgkin lymphoma?
|
oral lesions common in pt w HIV associated lymphoma
|
|
|
-Markedly red gingiva, out of proportion to plaque levels
-No attachment loss present -HIV |
Linear Gingival Erythema
|
|
|
-Necrosis of one or more interdental papilla
-No bone loss -Pain, bleeding, foul odor |
Necrotizing Ulcerative Gingivitis
|
|
|
-Focal or generalized
-Pronounced & rapid attachment loss -Spontaneous exfoliation of teeth -Necrosis & sloughing of bone/soft tissue |
Necrotizing ulcerative periodontitis
|
|
|
Herpes Zoster infection in HIV+ people?
|
Can get multiple recurrences which is not normal
|
|
|
Most common deep fungal infection in HIV?
|
Histoplasmosis
|
|
|
-Teens-20s
-Non-smokers -Shallow ulcer w/ red halo -No vesicle -No more than 3-5 lesions -Mucobuccal fold most common site |
Aphthous minor
|
|
|
Duration of aphthous minor?
|
3-7 days & recurs every couple mon/couple times a year
|
|
|
Main etiology of aphthous?
|
Autoimmune
-Genetic predisposition (90% both parents, 60% one parent, 20% neither) |
|
|
First choice of treatment for aphthous minor?
|
Topical steroids- Kenalog in orabase
|
|
|
-100 tiny ulcers 1-3 mm w/ no vesicle
-Clinically resembling primary herpes -Young adult females -Heal 7-10 days or weeks |
Herpetiform aphthous
|
|
|
-Large (several cm), deep ulcerations
-Last 4-6 weeks -May leave scarring -May recur for years |
Aphthous major
|
|
|
Most common viral disease (other than viral respiratory infections)?
|
Herpes simplex
|
|
|
Primary mode of transmission of herpes simplex?
|
Asymptomatic viral shedding
|
|
|
What % of adult population display Ab to herpes?
|
50-90%
|
|
|
-1-5 yrs
-Non-specific systemic symptoms -2-4 mm vesicles & ulcers in any area of mouth -Bleeding, painful gingiva |
Acute herpetic gingivostomatitis
|
|
|
Herpes virus remains latent in?
|
Trigeminal ganglia
|
|
|
-Adults
-Usually muco-cutaneous juntion -Clusters of vesicles that ulcerate & get crusty -Few times a month/year -Last 4-10 days |
Recurrent Herpes Simplex
|
|
|
-Multiple small painful ulcers which may coalesce into large ulcer
-Develop on mucosa bound to periosteum (hard palate & gingiva) -Last 7-10 days -Precipitated by dental treatment |
Recurrent intraoral herpes simplex
|
|
|
-Children
-Erythema, vesicle, pustule, hardened crust -Trunk & face, then extremities -Oral: small vesicles on buccal mucosa, palate & gingiva -May scar |
Chickenpox (Varicella)
|
|
|
-Adults
-Extremely painful -Fever, pain along nerve, headache, -Trunk- often unilateral -Vesicular eruptions that become crusty |
Herpes zoster (Shingles)
|
|
|
-Adolescents
-Lymphadenopathy, pharyngitis, rhinitis -Fever, malaise, fever -Petechiae on hard & soft palate 0Resolves 4-6 weeks |
Infectious mononucleosis
|
|
|
Infectious mononucleosis is caused by which virus?
|
EBV
|
|
|
Which 2 infections are caused by Coxsackie A?
|
1. Herpangina
2. Hand Foot & Mouth Disease |
|
|
-Children (esp summer)
-Sore throat, fever, headache -Small ulcers on hard & soft palate, tongue -Ulcers preceded by vesicles -Short duration: 1 week |
Herpangina
|
|
|
-Young children
-Numerous small vesicles found all over mouth -Maculopapular exanthematous & vesciles on skin -Flu-like symptoms |
Hand, Foot & Mouth Disease
|
|
|
-Fever, mailaise, conjunctivitis, photophobia & eruptive lesions on skin
-Oral: Koplik's spots on buccal mucosa (blueish white specks) 2-3 days before skin rash |
Measles
|
|
|
-Fever, headache, anorexia, conjunctivitis, pharyngitis, cough, lymphanedopathy
-Exanthematous rash on face or neck, body -Forchheimer's sign = oral lesions |
Rubella
|
|
|
-white plaques "curdled milk"
-Wipes off & may leave bleeding surface -Associated w/ antibiotic use, steriods & immunosuppression, newborns |
Pseudomembranous candidiasis
|
|
|
-Red macules & burning sensation
-Seen in denture wearers -Loss of filiform papillae (red bald tongue) |
Erythematous Candidiasis
|
|
|
-Erythematous zone in post dorsal surface of tongue
-Asymptomatic -Loss of filiform papillae |
Median Rhomboid Glossitis
|
|
|
-Red fissured area seen at corners of mouth
-Often seen in pt w loss of VDO & immunosuppresed, older pt -Treat w/ antifungals |
Angular Chelitis (Perleche)
|
|
|
-White patch that cannot be remocved
-Candidida infection superimposed on leukoplakia |
Chronic hyperplastic candidiasis
|
|
|
-Skin lesions- red papules that become tiny miliary abscesses w/ pus
-Fever, weight loss, productive cough -Oral lesions resemble actinomycosis or SCC |
Blastomycosis
|
|
|
-Low grade fever, preductive cough
-Oral: nodular, ulcerative lesion |
Histoplasmosis
|
|
|
-Most people have subclinical form
-Inhalation of dust w/ spores -Cough, respiratory disease, skin lesions -Proliferative granulomatous & ulcerative lesions |
Coccidiomycosis
|
|
|
-Superficial skin infection caused by Strep & Staph
-Young children -Fragile vesicles rupture & leave honey colored crusty areas around mouth |
Impetigo
|
|
|
-Children
-Severe pharyngitis, headache, chills, fevere -Skin rash on day 2-3 -Edema, elongated uvula, diffuse petechia -Strawberry tongue- erythematous fungiform papilla |
Scarlet fever
|
|
|
-Mucous patches- multiple painless, gray-white plaques on ulcerated surface
|
Secondary syphillis
|
|
|
Painless granulomas may form & become necrotic- sharp punched out ulcers
-chronic inflammation of tongue |
Tertiary syphilis
|
|
|
-Screw driver centrals & mulberry molars
|
Congenital syphilis
|
|
|
Gonoccoccal stomatitis shows clinical similarity to oral lesions of which 3 things?
-Painful ulcers -Erythematous gingiva -Gonococcal phayngitis & tonsillitis |
1. Erythema multiforme
2. Erosive lichen planus 3. Herpetic stomatitis |
|
|
Rapidly progressive infection by normal oral flora which has become pathogenic in immunocompromised pt
-May begin as ANUG -Areas of necrosis that extend deep into tissues -Very destructive |
Noma
|
|
|
-Normal oral flora
-May enter through wound following tooth extraction -Abscesses liberate pus containing sulfur granules -Extended course of penicillin to treat |
Actinomycosis
|
|
|
-Children
Small papule or vesicle -Lymphadenitis -Self limiting |
Cat Scratch disease
|
|
|
Most common cyst of the jaws?
|
Periapical cyst
|
|
|
-Ovoid/round lucency
-After removal of tooth from fragments of apical cyst |
Residual cyst
|
|
|
2nd most common odontogenic cyst?
|
Dentigerous cyst
|
|
|
Dentigerous cyst derived from?
|
Reduced enamel epithelium
|
|
|
What 3 things can develop in the lining of a dentigerous cyst?
|
1. Ameloblastoma
2. SCC 3. Mucoepidermoid carcinoma |
|
|
Variant of dentigerous cyst that is clinically visible.
-INfants & children -May spontaneously rupture -Fluctuant swelling over erupting tooth that has erupted through bone but not soft tissue |
Eruption cyst (Eruption hematoma)
|
|
|
Etiology of primordial cyst?
|
Remnants & degeneration of enamel organ
|
|
|
Sources of OKC?
|
1. Primordial cyst
2. Lateral periodontal cyst 3. Denterigerous cyst 4. Periapical cyst |
|
|
Nevoid basal cell carcinoma syndrome has which 3 features?
|
-Basal carcinomas of skin
-Multiple OKC -Bifid rib |
|
|
Why high recurrence rate of OKC?
|
Thin epithelial lining 6-8 cells thick
|
|
|
-Small multiple white papules
-Common in newborns -Keratin filled cysts found on alveolar mucosa -Remnants of dental lamina |
Gingival cyst of the newborn
|
|
|
-Unicystic swelling of gingiva
-Mandibular bicuspid, cuspid, incisor area -mucosal color - blue color -Adult 40-60 yrs |
Ginigival cyst of the adult
|
|
|
-Unilocular lucency between roots of vital teeth
-Manibular premolar & cuspid area -Arises from dental lamina |
Lateral periodontal cyst
|
|
|
-Well defined unilocular lucency, may have opacities
-Mandibula = maxila (> ant) -Any age -Histo: ghost cells (no nuclei) |
Gorlin cyst
|
|
|
-Unilocular/multilocular lucency w/ well defined margins
-Mandible - Histo: Mucous cells |
Glandular odontogenic cyst
|
|
|
-Age: young adult
-Mandibular molars -Cyst on buccal aspect of roots paritally erupted molars w/ history of pericoronitis -Lucency w/ buccal super-imposition |
Paradental cyst
|
|
|
-Multiple, small white nodules near midline junction of hard & soft palate
|
Palatal cyst of the newborn
|
|
|
-Females 40 & 50s
-Swelling in area of mucolabial fold/floor of nose -Histo: Pseudostratified columnar epithelium -No bone involvement |
Nasolabial cyst
|
|
|
Most common non-odontogenic cyst?
|
Nasopalatine duct cyst
|
|
|
-Ovoid heart shape lucency between centrals
-Adults 40-60 yrs - >6 mm in diameter |
Nasopalatine cyst
|
|
|
Histology of nasopalatine cyst?
|
Nerve & blood vessels
Simple, cubodial or pseudostrat ciliated columnar epithelium |
|
|
-Unilocular luceny posterior to incisive papilla in midline of hard palate
-Rare |
Median palatine cyst
|
|
|
-Young adults
-Floor of mouth -Dough like consistency -Lined by epidermis like epithelium |
Dermoid/epidermoid cyst
|
|
|
Cyst w/ numerous sebaceous glands, hair follicles, bone, muscle, GI derivatives?
|
Dermoid cyst
|
|
|
-Found anywhere along embryologic tract between foramen caecum and thyroid
-Fluctuant midline mass -Slow growth |
Thyroglossal duct cyst
|
|
|
-Cyst in neck composed of epithelium trapped in lymph nodes
-Asymptomatic fluctuant mass in lateral neck |
Cervical lymphoepithelial cyst
|
|
|
Small yellow mass
Usually asymptomatic Floor of mouth Develops in oral lymphoid tissue (Waldeyer's ring) |
Oral Lymphoepithelial cyst
|
|
|
-Middle age or older
-Prior maxillary sinus surgery -Vague pain, tenderness, discomfort -Well defined lucency adjacent to max sinus |
Surgical ciliated cyst of maxilla
|
|
|
-Posterior mandible
-Scalloped border between roots of adjacent teeth -Intact lamina dura -Cortical expansion possible |
Simple Bone Cyst
|
|
|
-Well defined lingual mandibular surface depression filled w/ salivary gland tissue
-Ovoid lucency usually between IA canal and inferior border of mand |
Static Bone Cyst (Lingual Mandibular Salivary Gland Depression)
|
|
|
-Multilocular "soap bubble" lesion
-Histo: blood filled vascular spaces in fibrous stroma, multinucleated giant cells |
Aneurysmal bone cyst
|
|
|
-Ground glass bone in all 4 quadrants
-Middle age female |
Hyperparathyroidism
|
|
|
Dense homogenous increase in opacity that may obscure tooth roots
-Middle age |
Osteopetrosis
|
|
|
-Kids
-Bilateral swelling of the mandible -Soap bubble multilocular lucency -Histo: pink cuffing of blood vessels |
Cherubism
|
|
|
Etiology of osteomyelitis?
|
Odonogenic infection - mixed organisms
|
|
|
Which form of osteomyelitis is more symptomatic- acute or chronic?
|
Acute
|
|
|
-Pain, swelling, cellulitis, fever, lymphadenopathy
-Moth eaten trabecula -Bony swelling -Sequestra |
Osteomyelitis
|
|
|
-Under 25 yrs
-Inflamed/slow spreading infection (toothache/pericoronitis) -"onion skin" layer of new bone over cortex |
Osteomyelitis w/ proliferative periostitis
-No sequestra |
|
|
Infection in bone due to compromised blood supply in previously irradiated bone
-Ill defined moth-eaten patter -Foci of opacity = sequestra |
Osteoradionecrosis
|
|
|
Bisphosphonates are used to treat:
|
1. osteoporosis
2. Metastases 3. Paget disease of bone 4. Multiple myeloma |
|
|
-Opaque lesion at root apex
-Fuses w/ lamina dura (can see tooth roots) -No lucent rim -Any age -Pulpal inflammation or necrosis of tooth |
Condensing osteitis
|
|
|
-Opaque lesion at apex of tooth that is contiguous w/ lamina dura
-No radiolucent rim -Vital teeth -Under 20 yrs -Mand bicuspids & 1st molar |
Idiopathic osteosclerosis
|
|
|
3 stages of cemento-osseous dysplasia?
|
1. Osteolytic stage
2. Blastic stage 3. Mature stage |
|
|
Most common fibro-oseeous lesion of jaws?
|
Cemento-osseous dysplasia
|
|
|
-Apices of mand inicisors
-Multiple lesions- vital teeth -African-american women 40-50s |
Periapical cemento-osseous dysplasia
|
|
|
-1 or 2 lesions
-30-60 yr female (caucasian) -Vital teeth -Lucent, opaque or mixed |
Focal cemento-osseous dysplasia
|
|
|
-Middle age african american female
-Lesions in all 4 quadrants -Vital teeth -May have periapical cemento-osseous dysplasia |
Florid cemento-osseous dysplasia
|
|
|
-Young people
-Ground glass/unilateral multilocular lucency -Bony expansion -Delayed eruption -Roots resorbed/teeth displaced Histo: No osteoblastic rimming |
Fibrous dysplasia
|
|
|
-Cotton wool
-Hypercementosis, root resorption, No PDL visible -Bony swelling -Histo: reversal lines |
Paget disease of bone
|
|
|
-Benign neoplasm of debatable origin (fibroblasts, cementoblasts, osteoblasts?)
-20-40 yrs -Mandible -Expansile, displacement of teeth -Lucent, mixed or opaque w/ smooth borders -Can cross midline -Histo: osteoblastic rimming |
Central Ossifying Fibroma
|
|
|
Gardner's syndrome consists of:
|
-Multiple osteomas in head & neck
-Multiple adenomatous polyps -Multiple impacted/supernumerary teeth |
|
|
-Young people
-Pain & swelling -Well defined mixed lesion -Histo: Increased vascularity, Looks like cementoblastoma, Atypical osteoblasts-- can be misdiagnosed as osteosarcoma |
-Osteoid osteoma < 2cm
-Osteoblastoma > 2cm |
|
|
-Extremely rare
-30-40s -Painless slow growing mass -Ant max & condyles -Lucent lesion w/ central opacity |
Chondroma
|
|
|
-Dense cortical bone w/ cartilage cap
-Rare in head & neck -Condyle |
Osteochondroma
|
|
|
-Younger than 30
-Asymptomatic, bony swelling -Mandible- can cross midline -Pure lucency w/ no cortication -Unilocular/multilocular -Histo: indistinguishable from brown tumors of hyperparthyroidism |
Central Giant Cell Tumor (Granuloma)
|
|
|
Why is important to aspirate before surgically entering any mulilocular radiolucency?
|
May be a hemiangioma or vascular malformation
|
|
|
Most common primary malignancy of bone?
|
Osteosarcoma
|
|
|
Contributing factors of osteosarcoma?
|
-Paget disease of bone
-Prior irradiation -Osteogenesis imperfecta |
|
|
-Over 30 yrs
-Mixed opaque/vague lesion -Pain & swelling- most common -Loose teeth, toothache -Parasthesia -Widened PDL = earliest sign |
Osteosarcoma
|
|
|
-Slow growing expansile mass w/ ill-defined speckled opacities
-Painless -Loose or shifting teeth |
Chondrosarcoma
|
|
|
-Under 25 yrs
-Males -Pain, swelling -Loose teeth, paresthesia -Irregular destructive diffuse radiolucency w/ ill-defined margins |
Ewing sarcoma
|
|
|
Most common malignancy of bone?
|
Metastatic tumors
|
|
|
3 most common tumors that metastasize to jaws?
|
1. Breast
2. Lung 3. Kidney |
|
|
2nd most common bone malignancy?
|
Multiple myeloma
|
|
|
Most common sign of salivary gland disease?
|
Swelling
|
|
|
4 basic causes of xerostomia?
|
1. Problem at salivary center
2. Problem w/ autonomic outflow path 3. Reduced gland function due to organic disease 4. Alterations in fluid/electrolyte balance |
|
|
Causes of excessive salivation (Sialorrhea)
|
-Higher CNS pathways or salivary center
-Local refle secretion stimulation -Inflammation- herpes or aphthous -Psychiatric or neuro disease -Cystic fibrosis -Mercury poisoning |
|
|
Clinical term referring to a swollen area filled w/ mucus?
|
Mucocele
|
|
|
Most common pattern of mucocele on biopsy?
|
Mucous escape reaction
|
|
|
What causes mucous escape reaction?
|
-Mucus escapes into CT due to rupture of a duct which causes inflammatory reaction
|
|
|
Where are mucoceles not expected to be found?
|
Hard palate or upper lip-VERY rare
|
|
|
Histology:
-Cavity filled w/ mucus -NO epithelial lining -Granulation tissue & foamy histiocytes |
Mucous escape reaction
|
|
|
Clinical term for mucocele that occurs in floor of the mouth
|
Ranula
|
|
|
How is mucus retention cyst different from mucous escape reaction?
|
-More likely to occur in adults
-Areas that are not easily subjected to trauma (vestibules) -Major or minor glands -FIrmer -Cyst- lined by epithelium |
|
|
-Pain
-Sudden enlargement of gland especially at mealtime -Opaque mass w/ in gland |
Sialolithiasis
|
|
|
Most common location for sialolithaiasis?
|
Whartons duct
|
|
|
Causes of sialadenitis?
|
1. Virus- mumps
2. Bacterial 3. Recent surgery 4. Sjogren syndrome, sarcoidosis, radiation, allergens |
|
|
Pain & swelling of gland
-Low grade fever, malaise, headache -Reduced salivary flow -Cloudy, thick saliva or pus from duct -Trismus -Erythema/edma of overlying skin |
Sialadenitis
|
|
|
-Middle age or older men
-Lower lip swollen & everted (develops slowly) -Minor salivary gland duct openings appear as tiny red dots |
Chelitis glandularis
|
|
|
Effects of xerostomia?
|
-Increased caries
-Increased periodontal disease -Difficulty eating & speaking -Increased opportunistic infection -Atrophic glossitis -Mucosal atrophy -Sore mucosa |
|
|
Unilateral or bilateral swelling of the parotid glands due to benign infiltration of lymphoid cells
|
Benign Lymphoepithelial Lesion
|
|
|
-Middle age female
-Progressive asymptomatic parotid gland enlargement -Reduced saliva |
Benign Lymphoepithelial Lesion
|
|
|
Which benign salivary gland disease is at risk for malignant transformation?
|
Benign Lymphoepithelial Lesion
|
|
|
-Dry eyes
-Dry mouth -Evidence of systemic autoimmunity |
Primary Sjogren syndrome
|
|
|
-Dry eyes
-Dry mouth -Clinical features of rheumatoid arthritis, SLE, polymyositis, scleroderma or biliary cirrhosis |
Secondary Sjogren syndrome
|
|
|
-Middle age woman
-Dry mucous membranes -Keratoconjuctivitis sicca -Lacrimal gland enlargement (rare) -Signs of autoimmune CT disease |
Sjogren syndrome
|
|
|
-30-40 yrs
-Tender swelling which progresses to ulceration in 2-4 weeks -Usually seen on palate -May be misdiagnosed as mucoepidermoid carcinoma -Infarction of minor salivary glands |
Necrotizing Sialometaplasia
|
|
|
Most common salivary gland tumor?
|
Benign Mixed Tumor
|
|
|
-30-50 yrs (females)
-Most often parotid gland -Slowly growing painless swelling usually behind angle of mandible in front of ear -Well defined & moveable -No skin ulceration |
Benign Mixed Tumor
|
|
|
Histo of benign mixed tumor?
|
-Lacks a capsule or defective capsule
-duct like structures -Mucoid, myxoid or chondroid tissue |
|
|
Is benign mixed tumor at risk for malignant transformation?
|
With multiple recurrences there is greater risk of transformation
|
|
|
-Usually parotid gland (rare in other locations)
-50-65 yrs (males) -Slow growing & localized -Fluctuant usually not paoinful -Can be bilateral |
Warthin tumor
|
|
|
-Strong predilection for minor salivary glands of upper lip
-Over 60 yrs female -Slow growing well circumscrible mobile mass- firm-fluctant, pink-blue |
Canalicular Adenoma
|
|
|
Benign tumor of salivary gland w/ epithelial cystic structures surrounded by lymphoid stroma?
|
Warthin tumor
|
|
|
Histo:
-Strands of epithelial cells arranged in double rows to form "party wall" pattern |
Canalicular Adenoma
|
|
|
Most common malignant salivary gland tumor?
|
Mucoepidermoid carcinoma
|
|
|
-20-40 yrs
-Painless slow growing firm or hard mass (more commonly minor salivary glands) -Moveable or fixed -Most appear clinically as mixed tumors |
Mucoepidermoid carcinoma
|
|
|
Most common malignant salivary gland tumor in kids?
|
Mucoepidermoid carcinoma
|
|
|
-Brachycephaly
-Trigonocephaly -Ocular proptosis -Hypertelorism -Hypoplastic maxilla w/ short upper lip -Malocclusion & ant open bite |
Crouzon disease
|
|
|
-Acrobrachycephaly (tower skull)
-Ocular proptosis -Hypertelorism -Down slanting -Syndactyly -Hypoplastic maxilla, mandibular prognathism -Gingival thickening (delayed eruption) -Shove shape incisors |
Apert Syndrome
|
|
|
-"Bird like"
-Zygomatic atrophy -Mandibular micrognathia -Ear defects -Pre-auricular hair -Down slanting of lower eyelid -Coloboma (notched lower eyelid) |
Treacher Collins Syndrome
|
|
|
-Bone deformity & fragilitiy
-Possible blue sclera -Dentinogenesis imperfecta -Malocclusion -Possible hearing loss |
Osteogenesis Imperfecta
|
|
|
-Absent or hypoplastic clavicles
-Brachycephaly -Hyperteleroism -Frontal & occipital bossing -Short stature -Teeth lack secondary cementum -Over-retained primary teeth, delayed eruption, supernumerary teeth |
Cleidocranial dysplasia
|
|
|
-Cleft palate
-Mandibular micrognathia -Glossoptosis |
Pierre-Robin Syndrome
|
|
|
-Small maxilla
-Frontal & sphenoid sinuses absent w/ hypoplastic max sinus -Smaller teeth w/ short roots -Macroglossia -Fissured tongue -Malocclusion, peg laterals -Flat face, hypertelorism & epicanthal folds |
Down syndrome
|
|
|
-Progressive bone destruction replaced by vascular tissue & then filled w/ fibrous tissue
-Mobile teeth, bone fracture |
Massive osteolysis
|
|
|
-Oral: looks like white sponge nevus or leukoplakia
-Eye: foamy gelatinous plaques -Triracial- white, black, american indians |
Witkop's Disease
|
|
|
-Excess keratin in nail beds
-Hyperkeratosis of hands & feet -Oral lesions: white plaques -Hyperhydrosis |
Pachyonychia Congenita
|
|
|
-Wide age range
-Occur anywhere but post mand common -Can have bony or soft tissue swelling -Unilocular or multilocular w/ big loculations w/ corticated border -May be associated w/ unerupted tooth |
OKC
|
|
|
Why does OKC have high recurrence rate?
|
Thin epithelial lining only 6-8 cells thick
|
|
|
Most common clinically significant odontogenic neoplasm?
|
Ameloblastoma
|
|
|
Nests of odontogenic epithelium w/ central core resembling stellate reticulum & rim of columnar ameloblasts?
|
Infilitrating ameloblastoma
|
|
|
Which odontogenic neoplasm is classified as benign aggresive?
|
Infiltrating ameloblastoma
|
|
|
-Late mixed dentition
-Anterior maxilla -Associated w/ unerupted tooth -Well defined lucency surrounding crown but extends past CEJ |
Adenomatoid odontogenic tumor
|
|
|
Which odontogenic tumor has columnar cells arranged in duct-like fashion?
|
Adenomatoid odontogenic tumor
|
|
|
-Pt over 40
-Any part of manidble -Lucent or mixed -Often associated w/ impacted tooth |
Calcifying epithelial odontogenic tumor (Pindborg tumor)
|
|
|
Presence of amyloid protein on biopsy is diagnostic for?
|
Pindborg tumor
|
|
|
-Triangular lucency lateral to tooth roots that mimics a vertical periodontal bone defect
|
Squamous odontogenic tumor
|
|
|
-Mixed dentition
-Posterior mandible -Well defined unilocular or multilocular -Often associated w/ unerupted tooth |
Ameloblastic FIbroma
|
|
|
-Small islands & narrow cords of odontogenic epithelium resembling dental lamina or developing tooth germ
-Primitive & cellular CT that resembles primitive dental papilla |
Ameloblastic Fibroma
|
|
|
Most common odontogenic tumor?
|
Odontomas
|
|
|
-Kids & adolescents
-Ant max between roots of teeth -Multiple small structures w/ recognizable tooth morphology -May block path of eruption |
Compound odontoma
|
|
|
-Kids & adolescents
-Post mand often w/ impacted tooth -calcified mass w/ radiodensity of tooth structure -May block path of eruption |
Complex odontoma
|
|
|
-Under 20
-Max or mand -Failure of eruption -Well defined unilocular w/ variable amounts of opacity -Looks like complex odontoma |
Ameloblastic Fibro-odontoma
|
|
|
-Facial gingiva of mand teeth
-Wide age range -Soft tissue density on xray not affecting bone -Rare odontogenic neoplasm |
Peripheral odontogenic fibroma
|
|
|
-Very rare odontogenic neoplasm
-Unilocular lesion in apical region w/ sclerotic border -often associated w/ unerupted tooth -Root resorption & divergence common -2 histo classifications |
Central odontogenic fibroma
|
|
|
Why is simple odontogenic fibroma considered to be odontogenic?
|
Occurs only in jaws
|
|
|
-Young adults
-Multilocular lucency w/ honeycomb appearance -Delicate wispy residual bone -Irregular margins -Poorly cellular histo w/ lots of ground substance |
Odontogenic Myxoma
|
|
|
-Under 25
-Mand 1st molar -Vital teeth -Pain/swelling -Mixed lesion w/ lucent rim (capsule) -Obscures root outline -Histo looks like osteoblastoma- May be misdiagnosed as osteosarcoma |
Cementoblastoma
|
|
|
Tumor that looks like benign ameloblastoma histologically & radiographically but metastasizes?
|
Malignant ameloblastoma
|
|
|
Most common site of metastasis for malignant ameloblastoma?
|
Lungs- may be due to aspiration during surgery
|
|
|
-Over 50 yrs
-Pain, bony swelling, unilocular or multilocular -Nests of epithelial cells w/ clear cytoplasm -Glycogen rich clear cells |
Clear cell odontogenic carcinoma
|
|
|
- late 20s
-Mandible -Lucency w/ poor-defined borders & destructive -Same histo as ameloblastic fibroma but more cellular mesenchymal component |
Ameloblastic fibrosarcoma
|
|
|
-Parotid gland most common
-All ages- mostly 40-60 -Slow growing mass w/ pain Histo: -Closely resemble normal serous acinar cells -Sometimes resemble thyroid tissue -Initial good survival rate but drops |
Acinic Cell Carcinoma
|
|
|
Malignant transformation in a previously benign mixed tumor w/ identifiable remnants of benign tumor?
|
Carcinoma-ex-mixed tumor
|
|
|
True malignant mixed salivary gland tumor where the tumor is composed of both malignant epithelial component & malignant mesenchymal component?
|
Carcinosarcoma
|
|
|
Most common malignant salivary gland tumor in submandibular glands?
|
Adenoid cystic carcinoma
|
|
|
-40-60 yr women
-Slow growing firm mass, pain/tenderness -Histo: Swiss cheese pattern-cystic spaces w/ mucoid material |
Adenoid cystic carcinoma
|
|
|
Malignancy that affects only minor salivary glands- palate, upper lip & buccal mucosa
-Like adenoid cystic carcinoma -"Indian filing" around nerves & blood vessels -Better prognosis than other salivary gland cancers |
Polymorphous Low-grade adenocarcinoma
|
|
|
-Sessile, non-vascular soft smooth mass
-Slow growing & asymptomatic -Usually pink, may be leukoplakic -Very common -Etiology: trauma, chronic irritation |
Irritation fibroma
|
|
|
-Long folds of dense CT in vestibule
-Asymptomatic -Caused by flange of loose denture -Malignant transformation rare |
Epulis fissuratum
|
|
|
-Asymptomatic mass
-Younger age than irritation fibroma -May have rough surface -Most common gingiva -Histo: large stellate fibroblasts |
Giant cell Fibroma
|
|
|
-Red edematous papillary projects
-Usually hard palate beneath denture -Cause-dentures worn 24 hrs w/ poor hygeine -Redness = candidiasis |
Papillary hyperplasia
|
|
|
-Found usually on gingiva
-Red, vascular & bleeds easily -Often ulcerated but painless -any age- more common in young people -Common during pregnancy -Histo: like granulation tissue |
Pyogenic granuloma
|
|
|
-Pedunculated/sessile mass on gingiva only
-Dark red or purple -May have surface ulceration -Painless -30, female -Histo: CT stroma w/ multinucleated giant cells |
Peripheral Giant cell granuloma
|
|
|
-Young people (female)
-Smooth firm mass, color of mucosa -Gingiva only -Xray: may show focal opacity |
Peripheral Ossifying Fibroma
|
|
|
-Red vascular tissue growing out of recent extraction site
-Made of granulation tissue -Painless, bleeds easily -Metastatic carcinomas tend to mimic this |
Epulis granulomatosa
|
|
|
-Slow growing mass usually on buccal mucosa
-Yellowish color w/ blood vessels on surface -Biopsy reveals adipose tissue -Rare in oral cavity |
Lipoma
|
|
|
-Slow growing painless mass
-Uncommon in oral cavity but 25-50% in head & neck -Tongue most common site in mouth -Histo: Antoni A & B & Verocay bodies |
Neurolemmoma (Schwannoma)
|
|
|
-Skin most common site
-Elevated nodular mass on buccal mucosa, palate & tongue -Can cause macroglossia -Arises from schwann cells, fibroblasts & perineural cell |
Neurofibroma
|
|
|
-Multiple neurofibromas
-Cafe-au-lait spots -15% have sarcomatous degeneration |
Von Recklinghausen's Disease of Skin
|
|
|
-Attempted repair of damaged never
-Small nodule w/ pain upon pressure -Mental nerve area most common -Middle age adults |
Traumatic Neuroma
|
|
|
-Congenital
-60% in head & neck -Flat or raised blue lesion -Honeycomb appearance in bone -Diascopy- blanches w/ pressure |
Hemangioma
|
|
|
-Hereditary
-Numberous telangiectasias on skin mucosa & GI tract -May suffer from anemia & epistaxis |
Hereditary hemorrhagic telangiectasia
|
|
|
-Portwine nevi- unilateral hemangioma on face following division of trigeminal nerve
|
Sturge-Weber Syndrome
|
|
|
-Most congenital
- Head & neck common area -Most commonly on tongue intraorally -May cause macroglossia -Histo: numerous spaces lined by endothelium containing lymph |
Lymphangioma
|
|
|
Rare variety of lymphangioma that occurs in neck & characterized by large cyst-like lymphatic vessels
|
Cystic hygroma
|
|
|
-Rare tumor of smooth muscle that is uncommon in oral cavity
-Slow growing mass on post tongue |
Leiomyoma
|
|
|
-Rare tumor of skeletal muscle that can occur on the tongue
|
Rhabdomyoma
|
|
|
-Can occur anywhere- esp tongue
-Any age -Asymptomatic sessile nodule -Thought to be derived from schwann cells -Histo: Large granular cells w/ eosinophilic cytoplasm & psuedoepitheliomatous hyperplasia |
Granular cell tumor
|
|
|
Which soft tissue lesion shows pseudoepitheliomatous hyperplasia on biopsy which may be confused w/ carcinoma?
|
Granular cell tumor
|
|
|
-Congenital
-Max ant gingiva -More common in females -Smooth pink-red nodular mass several cm in diameter -Similar to granular cell tumor but w/o pseudoepitheliomatous hyperplasia |
Congenital granular cell epulis
|
|
|
-Rare neoplasm in infants
-Ant max -Rapidly growing dark pigmented lesion -Radiographically looks malignant -High levels of vanilmadelic acid -Contains melanin |
Melanotic Neuroectodermal Tumor of Infancy
|
|
|
-Heat intolerance
-Fine, sparse hair -Periocular skin wrinkling & hyperpigmentation -Hypodontia -Conical shape teeth |
Ectodermal dysplasia
|
|
|
-Autoimmune
-Middle age women -Itchy skin papules on wrists & ankles -Most pt have oral lesions - most forms painless |
Lichen Planus
|
|
|
Most common location for lichen planus & 2nd most common?
|
1. Buccal mucosa
2. Tongue |
|
|
Form of lichen planus that has lacy pattern w/ striae of Wickham, bilateral & usually asymptomatic?
|
Reticular pattern
|
|
|
Most common form of lichen planus?
|
Reticular form
|
|
|
Type of lichen planus that resembles leukoplakia on dorsum of tongue?
|
Plaque form
|
|
|
Type of lichen planus that is ulcerative and painful, has radiating striae around ulcer, may have secondary candidiasis and can be confused w/ pemphoid or pemphigus?
|
Erosive lichen planus
|
|
|
Histology of lichen planus shows?
|
Infiltration of lymphocytes under basement membrane
|
|
|
Treatment of lichen planus?
|
Topical sterioids- Kenalog in orabase
|
|
|
Which type of lichen planus has a slight malignant potential?
|
Erosive lichen planus
|
|
|
-Autoimmune- Ab to desmosomes (intraepithelial/suprabasilar)
-Older adults -Vesciles rupture leave ulcers & are painful -Oral manifestations usually occur before skin lesions -positive Nikolsky sign Histo: Acantholysis & Tzank cells |
Pemphigus vulgaris
|
|
|
-Autoimmune- Ab to hemidesmosomes (subbasilar)
-Older adults -Oral mucosa, skin, genitals, ocular involvement -Oral- mainly gingiva -positive Nikolsky sign |
Benign Mucous Membrane Pemphigoid
|
|
|
-Older adults
-Rash on limbs -Oral manifestations only 10-45% -Similar to chronic desquamative gingivitivis -Subepithelial vesicles |
Bullous pemphigoid
|
|
|
-Hypersensitivity
-Young adults -Erythematous lesions on skin w/ concentric ring appearance "target" -Painful, ulcerative vesicles that bleed -Bloody, crusty lips |
Erythema multiforme
|
|
|
Severe form of erythema multiforme is known as?
|
Stevens-Johnson syndrome
|
|
|
-Young women
-Fever, weight loss, arthritis, malaise -Butterfly rash -Cardiac conditions -Lichenoid oral lesions |
Systemic lupus erythematousus
|
|
|
-Few or no systemic symptoms
-Affects sun-exposed areas -Scaly erythematous patches on skin -Oral lesions similar to lichen planus -May have butterfly rash |
Chronic cutaneous lupus erythematous
|
|
|
-Symmetrical scaly papules of skin
-Autzpitz sign- pull of silvery scales & leave bleeding pinpoints -Children & young adults -Histo: looks exactly like benign migratory glossitis |
Psoriasis
|
|
|
Which form of epidermolysis bullosa has the most oral manifestations?
|
Dystrophic
|
|
|
Oral manifestations of epidermolysis bullosa?
|
Gingival erythema
Anodontia Enamel hypoplasia Bulla & vesicle formation |
|
|
-Middle age adult
-Skin has diffuse hard texture & cannot wrinkle -Face has mask-like look -May have Raynaud's phenomenom -Neuralgia & parasthesia 0Waxy gray dusty skin -Oral involvment (tongue, soft palate, larynx, lips) -Universal widening of PDL |
Scleroderma
|
|
|
Localized variation of scleoderma that affects only solitary patch of skin
|
Morphea
|
|
|
-Abnormal response to microbial Ag
-Young adult men -1-4 weeks after dysentery or veneral disease -Triad of signs: Nongonoccal urethritis -Arthritis -Conjunctivitis |
Reiter's syndrome
|
|
|
-Numerous erythematous papules on skin
-Rough textured due to accumulation of keratin -Foul odor -Oral lesions- nodular papules on gingiva & palate -May become worse in sunlight |
Darier's Disease
|
|
|
Uncommon solitary lesion on skin or mucosa that histopathologically is identical to Darier's disease
|
Warty dyskeratoma
|
|
|
6 steps in management of oral lesions?
|
1. History
2. Exam 3. Clinical diagnosis 4. Diagnostic procedure 5. Definitive diagnosis 6. Treatment & follow up |

