![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
83 Cards in this Set
- Front
- Back
|
What is CHRONIC HYPERPLASTIC PULPITIS?
|
Unique pattern of pulpal inflammation where the pulp tissue reacts to injury by undergoing hyperplasia
|
|
|
What is the etiology of PULP POLYP?
|
- open chronic pulpitis
- ample blood supply - increased regenerative capacities of young pulpal tissue |
|
|
PULP POLYPS are generally found in which teeth?
|
Molars of children/ young adults
|
|
|
What is the treatment for PULP POLYP?
|
- endodontic therapy
- extraction |
|
|
Occurence of PULPAL CALCIFICATIONS increases with what two factors?
|
- aging
- trauma/caries |
|
|
What are PULP STONES?
|
Spherical calcifications formed within the coronal portions of the pulp.
|
|
|
Prominent PULPAL CALCIFICATIONS have been associated with what two conditions?
|
- Dentin Dysplasia Type II
- Ehlers Danlos Syndrome |
|
|
What is the treatment for PULPAL CALCIFICATIONS?
|
No treatment required
|
|
|
What is a PERIAPICAL ABCESS?
|
accumulation of acute inflammatory cells at the apex of a non-vital tooth
|
|
|
What is the etiology of a PERIAPICAL ABCESS?
|
- often associated with a non-vital tooth
- may be symptomatic or asymptomatic - spreads along path of least resitance |
|
|
What is a PARULIS?
|
- gum boil
- an intraoral opening of a sinus tract that often presents as an erythematous mass of subacutely inflamed granulation tissue |
|
|
What is the treatment for a PERIAPICAL ABCESS?
|
- drainage
- elimination of the focus of infection: reduction of occlusion, analgesic and Abx, endodontic therapy |
|
|
What is a PERIAPICAL GRANULOMA?
|
a mass of chronically inflamed granulation tissue at the apex of a nonvital tooth
|
|
|
PERIAPICAL GRANULOMA can arise from which two conditions?
|
- initial periapical pathosis
- progression of a periapical abcess |
|
|
What are the radiographic features of PERIAPICAL GRANULOMA?
|
- radiolucency with loss of apical lamina dura
- well circumscribed or ill defined - root resorption may occur |
|
|
What is a complication of PERIAPICAL GRANULOMA?
|
may transform into a periapical cyst
|
|
|
What is a PERIAPICAL CYST?
|
Inflammation stimulates epithelium at the apex of a nonvital tooth to form a true epithelium lined cyst
|
|
|
What are the two etiological sources of PERIAPICAL CYSTS?
|
- source of epithelium
- source of inflammation |
|
|
What are the epithelial sources of PERIAPICAL CYST?
|
- usually rest of Malassez
- crevicular epithelium - sinus lining - epithelial lining of fistula tract |
|
|
What are the inflammatory sources of PERIAPICAL CYST?
|
- peridontal disease
- pulpal necrosis with spread through lateral foramen |
|
|
What is a complication with PERIAPICAL CYST?
|
Rarely squamous cell carcinoma has been reported within them.
|
|
|
What is a FIBROUS PERIAPICAL SCAR?
|
Defect created by the periapical lesion is filled with dense fibrous tissue instead of bone (when facial and lingual cortical plates have been lost)
|
|
|
What is OSTEOMYELITIS?
|
Acute or Chronic inflammatory process in the medullary spaces or cortical surfaces of bone that extend away from the initial site of involvement.
|
|
|
What majority of OSTEOMYELITIS cases are caused by what?
|
Bacterial infection.
|
|
|
What is ACUTE SUPPURATIVE OSTEOMYELITIS?
|
Acute inflammation process spreads through the medullary spaces of the bone. There is insufficient time for the body to react to the presence of the inflammatory infiltrate.
|
|
|
What conditions pre-dispose people to OSTEOMYELITIS?
|
- chronic systemic diseases
- immunocompromised status - disorders associated with decreased vascularity of bone |
|
|
Most cases of ACUTE SUPP. OSTEOMYELITIS arise after what two events?
|
- odontogenic infections
- traumatic fracture of the jaws |
|
|
Which two bacteria are most frequently involved in cases of OSTEOMYELITIS?
|
Staphylococci
Streptococci |
|
|
What are the signs and symptoms of ACUTE SUPP. OSTEOMYELITIS?
|
- pain
- fever - lymphadenopathy - leukocytosis - significant sensitivity - soft tissue swelling - less than 1 MONTH duration |
|
|
Define SEQUESTRUM"
|
drainage or exfoliation of a fragment of necrotic bone
|
|
|
Define INVOLUCRUM:
|
When a fragment of necrotic bone becomes surrounded by vital bone
|
|
|
What are the radiographic features of ACUTE SUPP. OSTEOMYELITIS?
|
- significant resorption of trabecular bone
- diffusely blotchy area - motted with indistinct margins - islands of residual bone (sequestra) |
|
|
What is the treatment of ACUTE SUPP. OSTEOMYELITIS?
|
- surgical intervention to establish drainage and remove sequestra
- use of antibiotics - |
|
|
What is CHRONIC SUPP. OSTEOMYELITIS?
|
Defensive response leads to the production of granulation tissue which subsequently forms dense scar in attempt to wall off the infected area. Encircled dead space acts as a reservoir for bacteria, and antibiotics can't reach the site. Begins to evolve 1 month after spread of infection.
|
|
|
What are the two etiological patterns of CHRONIC SUPP. OSTEOMYELITIS?
|
- sequela of acute osteomyelitis
- low grade inflammatory reaction that never went through an acute phase |
|
|
Which area is affected more frequently in cases of OSTEOMYELITIS?
|
Mandible
|
|
|
What are the radiographic features of CHRONIC OSTEOMYELITIS?
|
patchy, ragged, ill-defined radiolucency often with central radiopaque sequestra
|
|
|
What is the treatment for CHRONIC SUPP. OSTEOMYELITIS?
|
- removal of all infected and necrotic tissue mandatory
- antibiotics but IV in high doses - hyperbaric oxygen in difficult cases to stimulate vascularization, collagen synth and osteogenesis - weakened jaw bones must be immobilized |
|
|
What is DIFFUSE SCLEROSING OSTEOMYELITIS?
|
obvious infection process directly is responsible for sclerosis of bone
- increased radiodensity develops around sites of chronic infection such as periodontisis, pericoronitis, and apical inflammatory disease. |
|
|
What is CONDENSING OSTEITIS?
|
A focal bony reaaction to low-grade inflammatory stimulus, seen at the apex of a tooth with long-standing pulpitis or pulpal necrosis
|
|
|
CONDENSING OSTEITIS occurs most frequently in...
|
- children and young adults
- at apices of Mn premolars and molars |
|
|
What are the radiographic features of CONDENSING OSTEITIS?
|
localized, uniform zone of increased radiodensity adjacent to the apex of a tooth that exhibits a thickened pariodontal ligament space or apical inflammatory lesion.
|
|
|
What is the treatment for CONDENSING OSTEITIS?
|
- resolution of odontogenic infection, endo or extraction
|
|
|
What is a BONE SCAR?
|
residual area of condensing osteitis which remains after resolution of inflammatory focus
|
|
|
What is OSTEOMYELITICS WITH PROLIFERATIVE PERIOSTITIS?
|
Periosteal reaction to presence of inflammation
|
|
|
What is the most common cause of GARRE's OSTEOMYELITIS?
|
dental caries associated with periapical inflammatory disease
|
|
|
An open apex in CHRONIC HYPERPLASTIC PULPITIS can help reduce what?
|
Pulpal necrosis
|
|
|
What things have been associated with increased frequency of OSTEOMYELITITS?
|
- tobacco use
- alcohol abuse - IV drug abuse - diabetes mellitus - malnutrition - AIDS - Radiation |
|
|
Define "BONE SCAR":
|
Residual area of condensing osteitis which remains after resolution of inflammatory focus
|
|
|
How long does bone remodelling normally take after OSTEOMYELITIS?
|
6-12 months
|
|
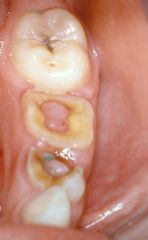
Identify the inflammatory lesions:
|
CHRONIC HYPERPLASTIC PULPITIS (pulp polyp)
|
|
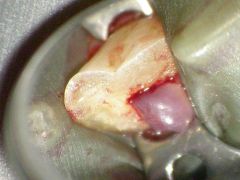
Identify the inflammatory lesions:
|
CHRONIC HYPERPLASTIC PULPITIS (pulp polyp)
|
|
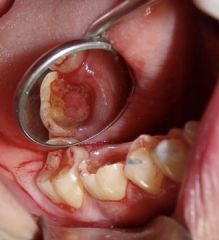
Identify the inflammatory lesions:
|
CHRONIC HYPERPLASTIC PULPITIS (pulp polyp)
|
|
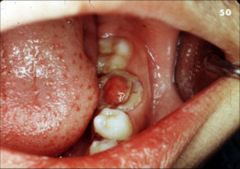
Identify the inflammatory lesions:
|
CHRONIC HYPERPLASTIC PULPITIS (pulp polyp)
|
|
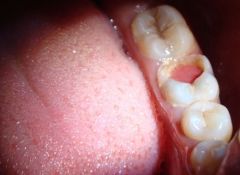
Identify the inflammatory lesions:
|
CHRONIC HYPERPLASTIC PULPITIS (pulp polyp)
|
|
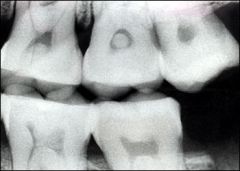
Identify the inflammatory lesions:
|
PULP STONES
|
|
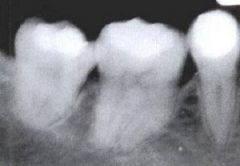
Identify the inflammatory lesions:
|
PULP STONES
|
|
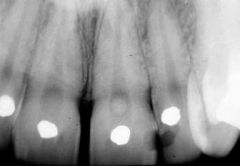
Identify the inflammatory lesions:
|
PULP STONES
|
|
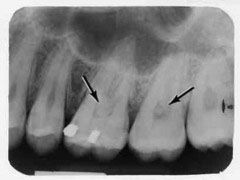
Identify the inflammatory lesions:
|
PULP STONES
|
|
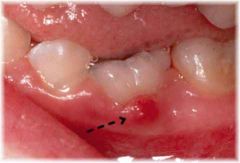
Identify the inflammatory lesions:
|
PARULIS
|
|
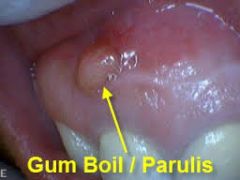
Identify the inflammatory lesions:
|
PARULIS
|
|
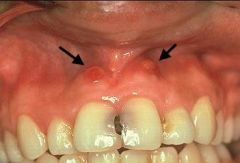
Identify the inflammatory lesions:
|
PARULIS
|
|
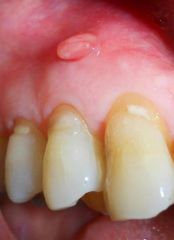
Identify the inflammatory lesions:
|
PARULIS
|
|
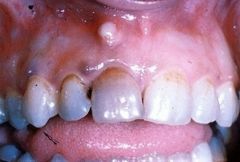
Identify the inflammatory lesions:
|
PARULIS
|
|
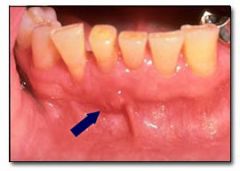
Identify the inflammatory lesions:
|
PARULIS
|
|
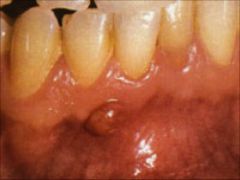
Identify the inflammatory lesions:
|
PARULIS
|
|
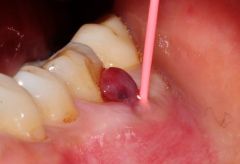
Identify the inflammatory lesions:
|
PARULIS
|
|
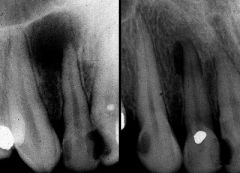
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
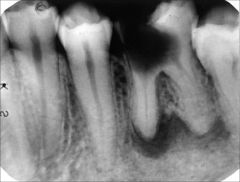
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
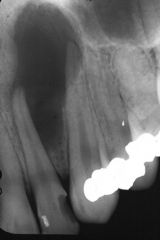
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
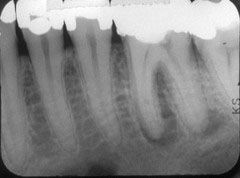
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
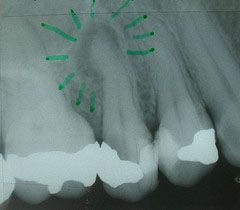
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
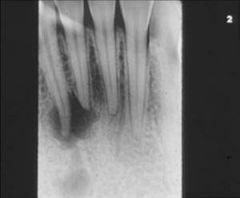
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
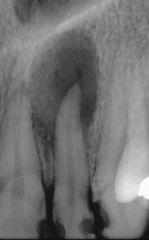
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
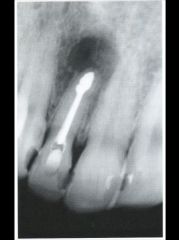
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
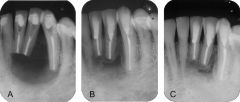
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
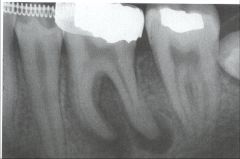
Identify the inflammatory lesions:
|
PERIAPICAL GRANULOMA
|
|
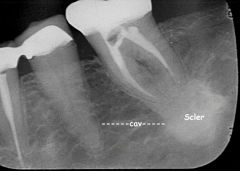
Identify the inflammatory lesions:
|
CONDENSING OSTEITIS
|
|
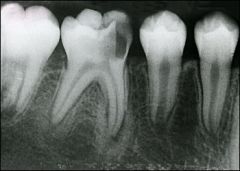
Identify the inflammatory lesions:
|
CONDENSING OSTEITIS
|
|
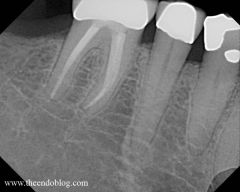
Identify the inflammatory lesions:
|
CONDENSING OSTEITIS
|
|
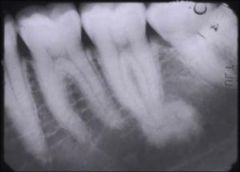
Identify the inflammatory lesions:
|
CONDENSING OSTEITIS
|
|
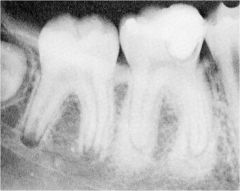
Identify the inflammatory lesions:
|
CONDENSING OSTEITIS
|
|
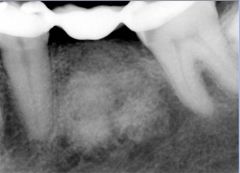
Identify the inflammatory lesions:
|
BONE SCAR
|

