![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
58 Cards in this Set
- Front
- Back
|
What are the functions of bones? |
1. Rigidity and shape 2. Protection and support 3. Locomotion 4. Ion Storage 5. Haemopoesis 6. Regulation of energy metabolism |
|
|
What are the two basic types of bone? (based on ECM type) |
1. Lamellar 2. Woven |
|
|
What are the physiological and functional properties of lammelar bone? |
1. Mature bone 2. Collagen arranged in lammellae (sheets) 3. Mechanically strong |
|
|
What are the physiological and functional properties of woven bone? |
1. Immature / healing - pathological bone 2. Haphazard meshwork of collagen 3. Replaced by lamellar bone. |
|
|
What are the types of lamellar bone? What bones fall under each type? |
1. Cortical - long bones 2. Trabecular - vertebrae |
|
|
How is trabecular bone distinct from cortical bone? |
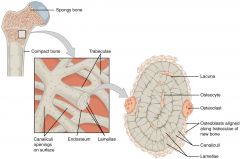
1. Thin cortical shell 2. 'Trabeculae' with connectivity increase compressive stress resitance Commonly known as 'Spongy Bone' |
|
|
What is the majority of the mass of the bone due to? |
Cortical bone - makes up the outer layer of the bone. |
|
|
What are the hallmark features of the periosteum? |
Fibrous membrane which is rich with nutrient capillaries. |
|
|
What are the hallmark features of trabecular bone? |
The internal region of the bone, made up of a honeycomb structure which resists compression. |
|
|
What are the hallmark features of the medullary cavity? |
1. Contains bone marrow 2. Rich in blood vessels 3. Site of blood cell formation (haematopoietic stem cells) |
|
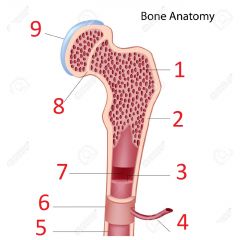
Label: |
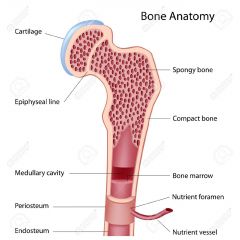
1. Spongy bone 2. Compact bone 3. Bone marrow 4. Nutrient vessel 5. Edosteum 6. Periosteum 7. Medullary cavity 8. Epiphyseal line 9. Cartilage |
|
|
What is an osteon / haversian system? |
These are the functional units of cortical bones. |
|
|
Describe, in words, an osteon. |
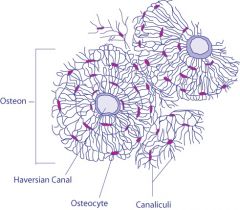
All blood vessels, lymphatic nerves, connective tissues are arranged in concentric rings (lamellae) surround a haversian canal. |
|
|
What are the mechanical properties of bone ultimately determined by? |
1. Rate of turnover 2. Collagen matrix 3. Size 4. Structure 5. Mineral density |
|
|
If you were to analyse the composition of a bone sourced from someone with osteoporosis what would be evident? |
Higher proportion of woven bone to cortical bone. 1:3 rather than 1:8 (50% increase) |
|
|
What are the process which are targeted when treating osteoporosis? |
1. Aimed at increasing bone formation 2. Decreasing bone loss |
|
|
What diseases could provide novel approaches to osteoporosis therapy? |
Excess bone diseases i) Scelerosteosis ii) Van Buchnen disease |
|
|
How often is the entire bone system remodelled? |
once every 7 years (a continuous process) |
|
|
What triggers increased bone remodelling? |
1. Mechanical forces 2. Dietary calcium 3. Vitamin D 4. Hormones 5. Signalling molecules - wnt signalling pathway is essential |
|
|
What hormones trigger increased bone remodelling? |
i) Parathyroid hormone (PTH) ii) Growth hormone iii) Oestrogen |
|
|
What hormones are intimately involved in calcium homeostasis? |
1. Parathyroid hormone (PTH) 2. Vitamin D 3. Calcitonin |
|
|
What is the role of calcitonin? |
Stimulates bone mineralisation. |
|
|
What is the progression of calcitonin's effects? |
1. Increase in blood calcium 2. Calcitonin release 3. Stimulates Ca2+ deposition in bones 4. Decreases calcium reuptake in the kidneys |
|
|
What are the effects of Vitamin D and PTH? |
Stimulate bone turnover (Calcium release) |
|
|
What is the progression of PTH and Vitamin D's effects? |
1. Decrease in blood calcium 2. Stimulation of Vitamin D and PTH release 3. Promotes Calcium uptake 4. Stimulates bone turnover - = calcium release |
|
|
What is the biochemical life cycle of vitamin D in the body? |
Begins life in an inactive form and becomes activated via hydroxylation in the liver and kidney |
|
|
What is the active form of Vitamin D called? |
Main active form is 1,25 hydroxy vitamin D (1,25(OH)2D) or Calcitriol |
|
|
What are the main three cell types involved in bone turnover? |
1. Osetocytes 2. Osteoclasts 3. Osteoblasts |
|
|
What are the overall stages of the bone remodelling cycle? |
1. Quiescence 2. Resorption 3. Reversal 4. Formation 5. Mineralisation 6. Quiescence |
|
|
What happens in the resorption phase of the remodelling cycle? |
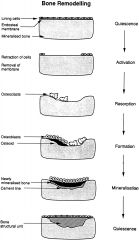
Migration of mononuclear proosteoclasts to the bone surface where they form multinucleated osteoclasts. |
|
|
What happens in the reversal phase of the bone remodeling cycle? |
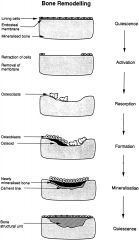
Mononuclear cells reappear on the bone surface following completion of resorption. These cells provide signals for osteoblast differentiation and migration. |
|
|
What happens in the formation phase of the bone remodeling cycle? |
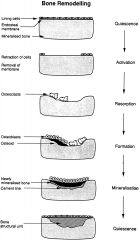
Osteoblasts lay down new bone until the resorbed bone is completely replaced by the new bone. The osteoblasts form a new osteoid. |
|
|
What happens in the mineralisation phase of the bone remodeling cycle? |
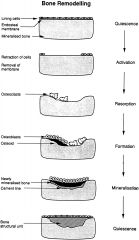
Osteoclast layer is subsequently calcified - which takes 3-4 months. |
|
|
What are osteoclasts? |
Osteoclasts are terminally differentiated cells which make up 90% of the total bone cells in an adult. They are derived from osteoblasts. |
|
|
Where can osteoclasts be found? What is their role? |
Osteoclasts can be found encased within the bond matrix. They are mechanosensory cells which are responsible for regulating bone structure and mass. |
|
|
What morphological properties of osteocytes allow them to fulfil their role? |
Osteocytes can communicate via dendritic processes which pass through cannaliculi |
|
|
What are osteoclasts? |
Osteoclasts are the bone resorbing cells of the bone. |
|
|
What are osteoclasts derived from? |
Derived from circulating monocytes / macrophages. |
|
|
How can an activted osteoclast be identified? |
Activated osteoclasts are multinucleated. |
|
|
What activation factors cause the activation of osteoclasts? |
1. RANK ligand ( Receptor activatior of nuclear factor KB Ligand) 2. M-CSF (monocyte - colony stimulation factor) |
|
|
What is the role of M-CSF in the bone remodeling cycle? |
Stimulates the proliferation of osteoclast progenitor cells. |
|
|
What is the role of RANK ligand in the bone remodeling cycle? |
RANK ligand controls differentiation by activating RANK |
|
|
Describe the process by which RANK ligand and M-CSF cause osteoclast mediated bone resorption. |
1. Monocytes recruited by action of M-CSF and RANK ligand 2. Monocytes adhere and differentiate into osteoclasts - Differentiation is activated by RANK ligand 3. Differentiated osteoclasts now being to divide 4. Osteoclast colony now begin to secrete H+ and lytic enzymes |
|
|
What are the lytic enzymes which cause the breakdown of bone? What secretes them? |
1. Tartate resistant acid phosphatase (TRAP) 2. Cathepsin K (CATK) |
|
|
What are osteoblasts? |
Osteoblasts are bone forming cells which are derived from stem cells. |
|
|
What is the role of an osteoblast? |
Lays down matrix which later becomes mineralised. Division and differentiation stimulated by hormones / cytokines. |
|
|
What factors stimulate mesenchymal stem cell differentiation from stem cells? |
1. Epidermal GF 2. Insulin like GF |
|
|
What factors stimulate preosteoblast differentiation from mesenchymal stem cells? |
1. IGF1 (Insulin like growth factor) 2. FGF-2 (fibroblast growth factor) 3. TGF - Beta 1/2 (transforming growth factor) 4. Parathyroid hormone 5. Prostaglandins 6. Vitamin D3 (1,25(OH)2 D3) |
|
|
What factors stimulate osteoblast differentiation from preosteoblasts? |
Transcription factors: 1. Runx2 2. Beta catenin 3. Osterix & same as before 1. IGF1 (Insulin like growth factor) 2. FGF-2 (fibroblast growth factor) 3. TGF - Beta 1/2 (transforming growth factor) 4. Parathyroid hormone 5. Prostaglandins 6. Vitamin D3 (1,25(OH)2 D3) |
|
|
What is the critical pathway involved in bone formation? |
wnt - Beta catenin signalling. |
|
|
What happens when the wnt signalling pathway is inactive? |
Beta catenin is phosphorylated by glycogen synthase kinase 3 (GSK-3) |
|
|
What is the effect of an inactive wnt - beta catenin signalling pathway? |
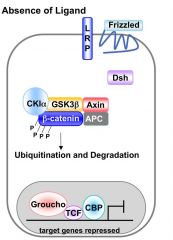
B catenin is targeted for degradation. Thus it does not enter the nucleus and therefore there is no target gene expression. |
|
|
What happens when wnt is present in the ECM? |
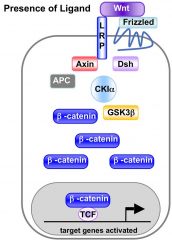
Wnt binds to the surface receptors - LRP/Frizzled complex. This causes B-Catenin to no longer be targeted for degradation as a key part of the inactivation complex - Axin becomes bound to LRP. Beta catenin subsequently enters the nucleus and activates target genes. (TCF) |
|
|
What is excessive bone growth termed as? |
Scelerosteosis. |
|
|
What type of genetic condition is sclerosteosis? |
An autosomal recessive condition. |
|
|
What causes sclerosteosis? |
A defect in the SOST gene results in decreased transcription and thus decreased translation of 'Sclerostin'. |
|
|
What is the role of sclerostin in the wnt signalling pathway? |
Sclerostin inhibits wnt signalling by acting as an LRP agonist. |
|
|
What is the molecular effect of decreased sclerostin expression? |
Reduced sclerostin expression = increased wnt signalling and thus increased bone formation via increases in osteoblast differentiation. |

