![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
40 Cards in this Set
- Front
- Back
|
Name 6 cells involved in innate immune responses |
NK cells neutrophils eosinophils basophils mast cells monocytes |
|
|
Give 9 examples of innate immunity, and briefly describe how they offer protection |
mucous membrane (traps foreign bodies) epidermis (barrier) tears (washes things away and contains lysosymes) excretion/urination/vomiting (removal/prevents colonisation) vaginal secretions (removal/prevents colonisation, plus slightly acidic so prevents bacterial growth) sebum (keeps skin pH at 3-5; inhibits growth of microorganisms) perspiration (prevents colonisation and contains lysosomes) - antimicrobial substances (interferons, complement, iron-binding proteins and antimicrobial proteins) |
|
|
Briefly describe the function of each of the antimicrobial substances (4) |
interferons: inhibit viral replication complememt system: enhances immune responses (e.g. cytolysis, phagocytosis and inflammation) iron-binding proteins: inhibit bacterial growth by reducing available iron antimicrobial proteins: short pepides with antimicrobial activity; also recruit mast and denritic cells |
|
|
Briefly describe the function of NK cells and how they may kill microbes |
they recognise cells with abnormal or unusual membrane proteins release perforin (cause lysis by making holes in membranes) and granzymes (initiate apoptosis by digesting intracellular proteins) |
|
|
Describe the 5 stages of phagocytosis |
chemotaxis: chemically stimulated recruitment of phagocytes adherence: attachment of phagocyte ingestion: extensions (psuedopods) engulf microbes, forming a phagosome digestion: phagosome merges with lysosome - forming a phagolysosome killing: microbe is destroyed. Substance unable to be digested remain in residual bodies. |
|
|
What are the three stages of inflammation |
vasodilation emigration of phagocytes tissue repair |
|
|
Where do B and T cells originate and mature respectively? |
both are formed in the red bone marrow B cells mature in the bone marrow T cells move to the thymus and mature there |
|
|
What are the two types of adaptive immunity? |
cell-mediated and antibody-mediated |
|
|
Briefly describe what is meant by clonal selection |
occurs in secondary lymphatic tissue and organs involves proliferation and differentiation of lymphocytes with specificity towards a specific antigen gives rise to effector cells which target the antigen, and memory cells remain in the circulation to respond to future infections |
|
|
Name the 5 different classes of antibody |
IgA IgG IgM IgD IgE |
|
|
What are the 5 functions of antibodies |
neutralizing antigens (e.g. blocking) immobilizing (e.g. binding to cilia or flagella) agglutination and precipitation of antigen complement activation enhance phagocytosis |
|
|
Which antibody classes are most abundant in the primary response? |
IgM and IgG |
|
|
Phagocytes bind to what three types of receptor on cells? |
scavenger receptors carbohydrate receptors toll-like receptors |
|
|
Name the cells of the adaptive immune system (4) |
plasma cells memory B cells T helper cells Cytotoxic T cells |
|
|
In order from most to least abundant, name all the WBCs |
Neutrophils Lymphocytes Monocytes Eosinophils Basophils |
|
|
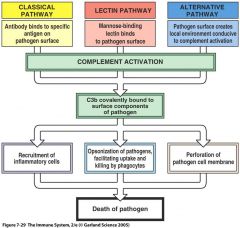
Illustrate the complement system |
|
|
|
Describe what happens in complement system after C3 has been activated |
- inactivated C3 splits into activated C3a and C3b - C3b binds to the surface microbes, and on the surface of phagocytes, increasing opsonisation - C3b splits C5 which, in conjunction with C6-C9, leads to the formation of the membrane attack complex. The membrane attack complex inserts into the plasma membrane of microbes, causing cytolysis C3a and C5a bind to mast cells, causing the release of histamine - increasing vessel permeability and inflammation. C5a also recruits phagocytes (chemotaxis) |
|
|
Describe the classical pathway of the complement system |
- antibody binds to antigen - antigen-antibody complex activates C1. Classical pathway therefore links adaptive and innate immune systems. - C1 can also bind directly to pathogens, and therefore trigger complement without antibodies - pathway converges with the production of C3 convertase - C3 becomes activated and the fragments initiate phagocytosis, cytolysis and inflammation |
|
|
Describe the mannose-binding pathway of he complement system |
- macrophages that digest microbes release chemicals that cause the liver to produce proteins called lectins - lectins bind to mannose and other carbohydrates on the surface of microbes, leading to the production of activation of C3 convertase and activation of C3 |
|
|
Describe the alternative pathway of he complement system |
- does not involve antibodies - initiated by the spontaneous hydrolysis of C3 - involves interaction between lipid-carbohydrate complexes on the surface of microbes, and complement protein factors B, D and P. |
|
|
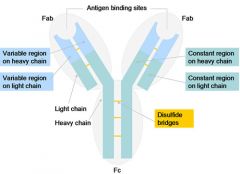
Draw and label standard antibody |
|
|
|
Which cell links the innate and adaptive immune systems and why? |
Dendritic cells. Take up and internalise antigens in the periphery and then present them to T cells |
|
|
Name the primary lymphoid organs and give 3 examples of secondary lymphoid organs |
Primary: bone marrow and thymus Secondary: spleen, lymph nodes andlymphatic nodules |
|
|
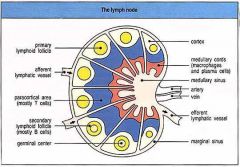
Draw and label a lymph node |
|
|
|
What is the function of a lymph node? |
Sites of immune responses Receive antigen from the periphery and act as immunological filters |
|
|
What three signals do APCs deliver to T cells |
activation survival differentiation |
|
|
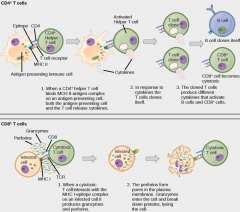
Draw a diagram summarising the activity of T cells |
|
|
|
Draw a diagram summarising the activation of B cells |
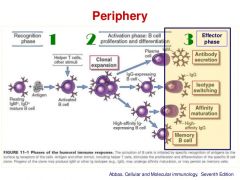
|
|
|
What are the stages of leukocyte trafficking? |
margination and rolling adhesion tight binding diapedesis chemotaxis/migration |
|
|
Describe the pathology of type I hypersensitivity with examples |
- IgE binds mast cells and basophils via Fc portion - cross-linking of IgE induces degranulation, causing histamine release - histamine and other mediators - such as prostaglandins, cytokines and leukotrienes - have various affects, including vascular permeability, bronchodilation and VSMC contraction - common examples of type 1 hypersensitivities are asthma, allergic rhinitis and anaphylaxis |
|
|
Describe the pathology of type II, III, and IV hypersensitivities with examples |
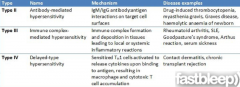
|
|
|
Give 5 examples of organ-specific autoimmune disorders |
organ-specific; type 1 DM (pancreas) Goodpasture's syndrome (basement membrane in lungs and kidneys) Multiple sclerosis (brain and/or spinal cord) Grave's disease (thyroid gland) Vitiligo (skin) |
|
|
Give 5 examples of systemic autoimmune disorders |
vasculitides (Churg Strauss) Rheumatoid arthritis Scleroderma Systemic Lupus Erythromatosus Polymyositis |
|
|
Briefly describe the pathology of the following; psoriasis RA Grave's disease Hashimoto's thyroiditis SLE Sjorgens syndrome Crohn's disease MS Type 1DM |
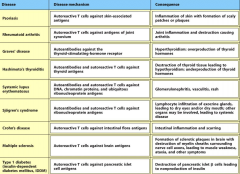
|
|
|
What is the difference a primary and secondary immunodeficiency? |
primary: typically congenital. Caused by a genetic defect affecting the function of the immune system Secondary: acquired due to other diseases or conditions e.g. infections or immunosupression |
|
|
Give three examples of a primary immunodeficiency |
Severe Compromised Immunodeficiency (SCID) Wiskott-Aldrich Syndrome DiGeorge syndrome |
|
|
Give three examples of a secondary immunodeficiency |
Acquired Immunodeficiency Syndrome Leukaemia Malnutrition Aging |
|
|
Defects in which cell type are likely to have the biggest impact on immunodeficiency? Why? |
phagocytes three levels of deficiency: cell prodution, phagocyte interacton (linking adaptive responses) and kiling |
|
|
Explain the life cycle of HIV |
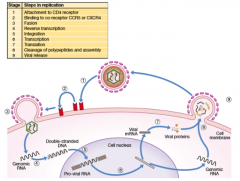
|
|
|
Explain the pathogenesis HIV |
Oninfection, the HIV virus migrates into T-cells from its mucosal siteof inoculation, viamacrophages and/or dendritic cells.
The virus then disseminatesthroughout the systemic circulatory system before replicating(predominantly) in CD4+ T-cell reservoirs and sanctuary sites - suchas the lymph nodes, spleen, liver, gastrointestinal submucosa, andbone marrow. Throughout the course of infection, HIV reduces memoryand naïve CD4-cell populations, with the subsequent loss of CD4T-cell populations, and immunodeficiency. Four mechanisms regardinghow HIV reduces CD4-populations, have been postulated: lysis, immunedestruction, apoptosis, and impaired lymphocyte regeneration. |

