![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
63 Cards in this Set
- Front
- Back
|
Renal Functions |
1. Regulation of body fluid osmolality & volume 2. Regulation of electrolyte balance 3. Regulation of acid-base balance 4. Excretion of metabolic & foreign substances 5. Production & secretion of hormones |
|
|
Which hormones are produced/secreted by renal system? |
Renin Prostaglandins/kinins 1,25-dihydroxyviamin D3 (calcitriol) Erythropoietin |
|
|
Renal circulation - Name all vessels that blood goes through starting with the aorta (bolded names = arteries) |
Aorta - Renal artery - Segmental artery - Interlobar artery - acrucate artery - cortical radiate artery - afferent arteriole - glomerular capillaries - Efferent arteriole - Peritubular capillaries & vasa recta - cortical radiate vein - arcuate vein - interlobar vein - renal vein - inferior vena cava |
|
|
Peritubular capillaries can also branch into... |
Cortical radiate and arcuate veins directly |
|
|
Nephron parts, starting at glomerulus |
Bowman's capsule - Proximal convoluted tubule - Henle's loop (thin descending) - Henle's loop (thick ascending) - Distal convoluted tubule - Connecting tubule - Collecting duct |
|
|
Types of nephrons and their description |
1. Juxtamedullary nephron - Only present at boundary btw cortex and medulla, loops go deep into medulla, *concentrate urine 2. Cortical nephron - Present mostly in cortex, henle's loop touches outer zone of medulla |
|
|
Type of nephrons (in %) found in: Dogs/cats Pigs Humans |
100% Juxtamedullary in dogs/cats 3% Juxtamedullary in pigs 14% Juxtamedullary in humans |
|
|
Basic Renal Processes |
1. Golmerular filtration 2. Tubular Reabsorption 3. Tubular Secretion |
|
|
Blood pressure in: 1. Renal artery 2. Afferent arteriole 3. Glomerulus 4. Efferent arteriole 5. Peritubular capillaries 6. Renal vein |
1. 100 mmHg 2. 100-50 mmHg 3. 50 mmHg 4. 50-20 mmHg 5. 20 mmHg 6. 10 mmHg |
|
|
Tubular reabsorption - locations and what happens at each |
PCT - Nutritents and H20 reabsorbed Thin Descending Limb - H20 reabsorbed Thick Ascending Limb - NaCl reabsorption DCT - Na and H20 reabsorption CT - H20 reabsorption |
|
|
Solute concentration in thin descending limb vs. thick ascending limb |
Thin - High solute concentration (~600-900mOsm/l)
Thick - Low solute concentration (~100mOsm/L) |
|
|
Assessments of renal function |
1. Serum biochemical tests 2. Urine analysis 3. Renal Clearance |
|
|
Serum biochemical tests measure what? |
Blood urea nitrogen (simple, not very accurate) Creatinine Electrolyte concentrations |
|
|
Urine analysis measures what? |
Volume Specific gravity Colour pH Electrolytes, enzymes and proteins |
|
|
Renal Clearance measures what? |
Glomerular function: Glomerular Filtration Rate
Tubular function: 1) Renal clearance rate, 2) Fractional clearance of electrolytes |
|
|
Formula for Amount excreted in Urine |
Amount excreted in urine = Amount filtered (thru golmeruli into PCT) - Amount reabsorbed (into renal vein) + Amount secreted (into tubular luminal fluid) |
|
|
1st step in urine formation |
Ultrafiltrate of plasma by glomeruli |
|
|
Glomerular Filtration Rate (GFR) definition |
Volume of Plasma filtered by the glomerulus per unit time ml/min/kg |
|
|
GFR should be... |
Essentially protein free |
|
|
Ultrafiltration driven by? |
Starling forces across glomerular capillaries and into bowman's space |
|
|
Glomerular filtration barrier formula |
Glomerular filtration barrier = capillary endothelium + basement membrane + filtration slits of podocytes |
|
|
What cells line the DCT |
Macula Densa Cells |
|
|
Which cells are found in the Mesangial Region |
Lacis Cells (aka Extraglomerular mesangial cells) |
|
|
Capillary endothelium is ___________ in the glomerulus |
Fenestrated |
|
|
Glomerular Filtration Pressures |
Plasma Colloid Pressure - 32 mmHg Glomerular Hydrostatic Pressure - 60 mmHg Capsular Hydrostatic + Colloid Pressure - 18 mmHg Filtration Pressure - 10 mmHg |
|
|
Filtration pressure equation |
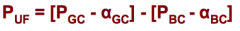
Puf - Ultrafiltration P Pgc - Glomerular Capillary hydrostatic P acg - Glomerular Capillary Oncotic P Pbc - Hydrostatic P abc - Oncotic P |
|
|
GFR equation |
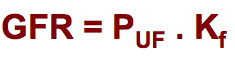
Kf - Ultrafiltration coefficient (filtration barrier permeability x glomerular surface area available for filtration) |
|
|
What does ATP and Adenosine do to GFR (include steps leading up to change in GFR) |
Vasoconstriction of afferent arteriole Increased resistance, Decreased renal blood flow Decreased Capillary BP (Pgc) Decreased GFR |
|
|
What does ANP and Glucocorticoids do to GFR (include steps leading up to change in GFR) |
Vasodilation of afferent arteriole Decreased resistance, Increased RBF Increased Capillary BP (Pgc) Increased GFR |
|
|
What does ANG-2 initially do to GFR (include steps) |
Vasoconstriction of efferent arteriole Increased resistance, Decreased RBF Increased Capillary BP (Pgc) Increased GFR |
|
|
What does NE, EPI, ANG-2, ADH and Endothelin do to GFR (include steps) |
Vasoconstriction of afferent arteriole AND efferent arteriole Increase resistance, Decrease RBF Decrease Capillary BP (Pgc) Decrease GFR |
|
|
What does Dopamine, NO, kinins, PGE2, and PGI2 do to GFR (include steps) |
Vasodilation of both afferent and efferent arterioles Decrease resistance, Increase RBF Increase Capillary BP (Pgc) Increase GFR |
|
|
What is inulin used for? |
Marker to estimate renal clearance |
|
|
Glomerular filtration barrier restricts filtration of molecules on the basis of __________ and _______________ |
Size Electrical Charge |
|
|
Permeability of cations, neutral, and anions (relative to one another) |
Cations > neutral > anions |
|
|
Which substances have extremely low filtrate/filtrand values? Why? |
Hemoglobin and Serum Albumin
High molecular weight and radius |
|
|
Which substances have low filtrate/filtrand values? why? |
Myoglobin and Egg Albumin
High molecular weight and radius (not as high as hemoglobin and serum albumin though) |
|
|
Which substances have a filtrate/filtrand of about 1? why? |
Water, urea, glucose, sucrose, inulin Lower molecular weight and radius
*Inulin is 0.98 Filtrate/Filtrand |
|
|
Pathological Factors affecting GFR |
1. Kidney diseases 2. Inverse relation between alpha GC and GFR 3. Inverse relation between Pbc and GFR |
|
|
Why does kidney disease affect GFR |
Decrease Kf by decreasing number of filtering glomeruli and thus GFR decreases |
|
|
What can over come kidney disease effects? |
Drugs/Hormones that dilate glomerular arterioles and thereby increase Kf |
|
|
Example of kidney disease and what does it do? |
Glomerulonephritis (*chronic)
Cause decrease GFR due to decrease in Kf which leads to an increase in proteinuria |
|
|
What can cause a lowered GFR when looking at the inverse relation between aGC and GFR? |
Acute obstruction of the urinary tract (kidney stone)
Backpressure pushes hydrostatic pressure up |
|
|
Pbc is affected by? |
Changes in protein metabolism occurring in extra-renal organs |
|
|
High protein diets result in? |
Increased renal blood flow and GFR |
|
|
GFR measurement marker characteristics |
1. Freely filtered by glomerulus 2. Not absorbed/secreted by nephron 3. Not metabolized/produced by kidney 4. Does not alter GFR per se |
|
|
Markers used for GFR measurement |
1. Inulin 2. Creatinine 3. Technetium (radioisotope) or Iohexol (contrast agent) |
|
|
Inulin as a GFR measurement marker (include limitations) |
Gold standard Limitation: expensive and impractical bc requires catheterization and timed sampling |
|
|
Creatinine as a GFR measurement marker (include limitation) |
Most commonly used - muscle produces creatinine at a constant rate proportional to muscle Limitations: secreted in PCT (~10% error), not useful at all in birds |
|
|
Definition of renal clearance |
Amount of plasma that needs to be filtered to account for the amount of substance present in urine every minute |
|
|
Renal Clearance formula |
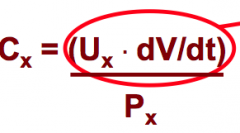
Cx: volume plasma cleared Ux: urine concentration dV/dt: volume urine collected in a time period Px: plasma concentration |
|
|
GFR inulin clearance formula |

*if using creatinine, just substitute creatinine for inulin |
|
|
Renal Plasma Flow measured by? |
Clearance of p-aminohippuric acid (PAH) |
|
|
Why is PAH used? |
Not produced by body, so has to be infused Is filtered by glomeruli, secreted by tubules and excreted in urine |
|
|
Renal Plasma Flow (RPF) formulas |
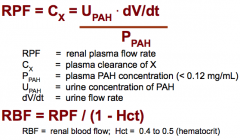
|
|
|
Define filtration fraction (FF). Formula? Normal values? |
Portion of plasma that is filtered
FF = GFR / RPF
0.15 to 0.20 |
|
|
A 50% loss in functioning nephrons, decreases the GFR by ______%.. Why? |
only 20-30%
Compensatory action of remaining healthy nephrons |
|
|
Fractional Excretion (FE) and Fractional Reabsorption (FR) rate equations |

|
|
|
What does Autoregulation do? |
Maintains a nearly constant GFR when MAP is between 80-180 mmHg |
|
|
Mechanisms of Autoregulation |
Myogenic Mechanism
Tubuloglomerular Feedback Mechanims |
|
|
Myogenic Mechanism when MAP increases |
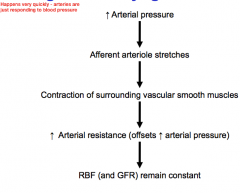
|
|
|
Cells involved with tubuloglomerular feedback |
Macula densa cells Juxtaglomerular cells Lacis cells in mesangial region |
|
|
Steps of Tubuloglomerular feedback starting with and increase in GFR |
1. Increase in GFR 2. Tubular flow increases 3. Flow past macula densa increases 4. Paracrine factors diffuse from macula densa to afferent arteriole (ATP, Adenosine) 5. Decrease in renin and Increase in ATP release 6. Afferent arteriole constriction = increased resistance = decreased GFR |

