![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
173 Cards in this Set
- Front
- Back
|
Half-life of mast cell tryptase? A. 1 hour B. 2 hours |
B Half life of 2 hours with peak at 15-60mins |
|
|
Best single predictor of difficult intubation in obese patient? A. Mallampati score B. Interincisor distance C. Severe OSA |
C Predictors: OSA, neck circumference, pre-tracheal soft tissue |
|
|
Best aspiration prophylaxis for urgent surgery? A. Na Citrate B. Ranitidine C. Omeprazole D. Metoclopramide E. Cisapride |
A |
|
|
Most common cause of mortality post transfusion? A. TRALI B. Contamination/infection C. Mismatched blood D. GvHD E. Anaphylaxis |
A |
|
|
Most common cause of awareness? |
A. Failure to check apparatus |
|
|
Apnoeic oxygenation in obese patients is best aided by? A. Sniffing position B. Head up tilt |
B Ramped position improves laryngoscopy |
|
|
Best renal protection for endoluminal AAA repair? A. NaCl B. NAC |
A IV volume expansion = reduced of failure No evidence for NAC |
|
|
White cylinder with grey shoulder? A. CO2 B. Air C. O2 D. N2O E. N2 |
A Air = white body with black and white shoulder O2 = white N2O = white body with blue shoulder |
|
|
Photograph of an Arndt endobronchial blocker. Orifice labelled 'X'. What goes in 'X'? A. Bronchoscope |
A |
|
|
Indicator in sodalime? A. Ethyl violet B. Potassium permangenate C. Blue ? D. ? E. ? |
A |
|
|
Desflurane vaporiser heated because: A. High SVP |
A |
|
|
What is NOT a disadvantage of drawover vaporizer? A. Basic temperature compensation B. Basic flow compensation |
Both disadvantages Advantage = ?cannot use sevo for gas induction as need 2 in series to achieve the required concentration |
|
|
FOB - can see a trifurcation. Where are you? A. RUL B. Lingula C. LUL D. RML E. RLL |
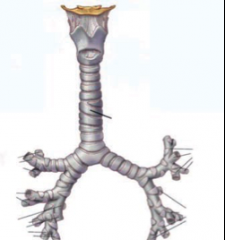
A. All bifurcations except RUL |
|
|
A Full Size C oxygen cylinder has pressure downregulated from? A. 16,000 kPa to 400 kPa B. 16,000 kPa to 240 kPa C. 11,000 kPa to 400 kPa D. 11,000 kPa to 240 kPa |
A |
|
|
Intubating over a bougie. Rotate ETT? A. 90 degrees anticlockwise B. 90 degrees clockwise C. 180 degrees anticlockwise D. 180 degrees clockwise |
A |
|
|
Air bubble leads to decreased: A. Damping coefficient B. Resonant frequency |
B |
|
|
At what valve area do you begin to get symptoms, at rest, with mitral stenosis?
A. 1.5 cm2 B. 1.0 cm2
|
B <1cm = critical stenosis |
|
|
New: With regard to Digoxin toxicity which of the following is NOT a feature? A. Atrial flutter |
Changes with dig toxicity: SVT (inc automaticity) with slow VR (dec AV conduction) VEBs and bigeminy Sinus brady or slow AF Any type of AV block VT ST dep TWI in V5-6 Prolonged PR Short QT |
|
|
Rpt: What is not associated with ulcerative colitis? A. Psoriasis B. Cirrhosis C. Arthritis D. Sclerosing cholangitis E. Iritis |
A |
|
|
75 yo non-valvular AF. Off warfarin. What is his daily risk of stroke? A. 0.01% |
A 5% per year/365 |
|
|
ECG - Which does NOT have abnormal Q waves? A. Digoxin toxicity B. WPW C. Anterior MI D. Previous MI |
A |
|
|
cTnI remains elevated for up to? A. 5-14 days |
A 6-10 days Peak 12-16hrs Elevated for 2 weeks |
|
|
Inverted PW's in lead II may be caused by? A. Junctional rhythm |
?A RPA notes: Lead misplacement, retrograde P waves in junctional rhythm usually during or after the QRS |
|
|
Hb 80 g/L with reticulocyte 10%: A. Hereditary spherocytosis |
A |
|
|
Pulsus paradoxus in constrictive pericarditis: A. Decreased BP with inspiration B. Decreased BP with inspiration greater than normal |
B (> 10mmHg drop) Normal = <10mmHg drop with inspiration |
|
|
Cause of visual loss in spinal surgery? A. Optic ischaemia B. Compression of eye |
A ischaemic optic neuropathy = most frequent cause of blindness arterial hypotension + inc venous/intra ocular congestion = inc resistance to flow and red O2 delivery. Pressure on eye > arterial pressure = ischaemia |
|
|
Which type of aortic dissection is typically managed non-operatively? A. Debakey Type I B. Debakey Type II C. Stanford A D. Stanford B E. Stanford C |
D |
|
|
Absolute CI to the sitting position in neurosurgical patient? A. Patent VA shunt B. Small PFO C. Pacemaker D. Small patent foramen ovale E. Oesophageal stricture contraindicated for transoesophageal echocardiogram |
A Risk of air embolism (Has to be a large PFO) |
|
|
When do most patients with SAH rebleed? A. 0-24 hours |
A Peak incidence is first day after SAH With 1.5% inc per day for the next 4/52 Occurs in 20% patient |
|
|
Unstable patient. Suspect aortic dissection. Most appropriate investigation? A. TOE B. MRI |
A |
|
|
Contraindication to IABP? A. AR |
A Absolute CI: AR, Aortic dissection, Severe aorto-iliac occlusive disease Relative: prosthetic grafts in aorta, aortic aneurysm, sepsis |
|
|
Prolonged trendelenberg position results in? A. Increased myocardial work |
A |
|
|
Scoliosis surgery. Which tract is being monitored with SSEPs? A. Dorsal column |
A. sensory column |
|
|
Estimate GCS post head-trauma. E - Response to pain V - Mumbling incoherently M - Withdraws to pain (attempted IV cannulation) A. 8 B. 9 |
A E2M4V2 |
|
|
Incidence of headache in first week post-partum? A. 38% |
A |
|
|
Oxycodone 20mg SR / Naloxone 20 mcg: A. Decreased constipation B. Reduced risk of drug misuse/abuse |
A |
|
|
Bowel surgery patient. Best method for intraoperative optimization of fluid therapy? A. Arterial pulse pressure contour analysis B. CVP C. PAOP D. UO |
A |
|
|
In what proportion of people is the AV node supplied by the R coronary artery? |
Right dominant 80%: RCA --> post intraventricular art --> AV node Left dominant 20%: Left circumflex Other sources say 85-90% |
|
|
Less blood wastage if: A. Lower transfusion threshold |
restrictive transfusion strategies are assoc with red transfusion rates and volumes |
|
|
How long prior to a spinal anaesthetic should dabigatran be ceased? A. 7 days |
A. 5days ASRA guidelines Restart 6hours after spinal or removal of catheter
QLD Guidelines - CrCl>80 --> 2 days, CrCl 50-80 --> 3 days, CrCl 30-50v--> 4 days
NB. Apix/Rivaraox (DFXa inhib) - similar periop Rx as dabig (similar drug, but with less renal elim 20-30%) Dabig: peak effect 2-3 h, EHL12-14h, 80% renal elimination Discontinue 1-2 days prior to surg, 3-5 if CKD (CrCl<50ml/min. Longer (5-7 days) AND check APTT or TT if major surgery, spinal puncture, need for complete haemostasis
Should not be restarted within 24h of spinal / removal of epidural catheter |
|
|
Day 4 epidural. On 40 mg SC enoxeparin daily postoperatively (8 pm). When is the most appropriate time to remove the epidural? A. Day 5 at 12 midday B. Day 5 at 6 am C. Day 5 at 6 pm D. Day 6 at ? |
POW = A RNS = A RPA = A or B LVP = B
B - international guidelines say 10-12 At RPA it would be 20hr post LMWH
CEACCP 2012 RA and antithrombs: Proph LMWH - 12h before CNB, 2-4hrs after
Therap LMWH - 24h before CNB, 2-4h after Therap UFH - discontinue 2-4h before (short t1/2), 1h after Proph UFH - 4-6h before, 1h after
|
|
|
What drug should NOT be used for tocolysis in 32/40 female? A. Indomethacin B. Magnesium C. Nifedipine D. Salbutamol |
A |
|
|
Following an eclamptic seizure the dose of MgSO4 is? A. 1 gram B. 4 grams |
B and then 1-2g/hr |
|
|
At what gestation should intraoperative monitoring of the fetus occur? A. 20/40 weeks. |
? when viable = 24 weeks |
|
|
Trauma patient. CXR (not given): air fluid levels adjacent to heart/diaphragm/ribs. A. Ruptured diaphragm B. Hiatus hernia |
A |
|
|
Endocarditis prophylaxis in patient with MVR appropriate for? A. Dental procedure ?which B. Rigid bronchoscopy C. Upper endoscopy with biopsy D. D&C E. Lithotripsy |
E |
|
|
Photograph of TOE transgastric SAX image of LV. Which artery supplies [anterior wall of LV arrowed] region? A. LAD B. RCA C. PDA D. LCx |
A |
|
|
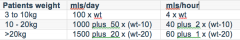
A 20kilogram child suffered 15% full thickness burns 6 hours ago. Optimumcrystalloid resuscitation for the first hour is: A. 160ml B. 260ml C. 360ml D. 460ml E. 660ml |
C. Parkland Formula 20kg x 15%TBSA x 4mL = 1200mL in the first 24 hours (1/2 in first 8 hours, 1/2 in next 16 hours) So, 600mL in the first 8 hours SINCE TIME OF BURN. i.e. over the next 2 hours. =300mL/hr Plus maintenance (4/2/1 rule) =60mL/hr TOTAL = 360mL/hr in the first hour. |
|
|
Incarcerated inguinal hernia in a child with a mild URTI. Most appropriate course of action? A. Postpone for 2 weeks B. Continue without ETT C. Continue with careful monitoring |
C |
|
|
Congenital prolonged QT syndrome treated with propranolol. How do you confirm an adequate response? A. HR <60 /min B. Decreased QT interval in response to a valsalva manoeuvre C. Normal QT interval |
B |
|
|
Meconium stained liquour but neonate delivered is vigorous. Rationale for NOT suctioning the neonate? A. May aspirate meconium B. May cause bradycardia C. May cause hypertension |
B |
|
|
Patient with subdural hematoma and PPM for ?AV ablation. PPM technician >1 hour away. Surgeon wishes to proceed immediately. Do you? A. Postpone and await a cardiologist review B. Postpone and await arrival of PPM technician C. Postpone and insert a transvenous temporary PM D. Proceed after institution of transcutaneous pacing E. Proceed with a magnet handy. |
RNS and RPA = E |
|
|
Which of the following does NOT occur following bilateral lung transplant? A. Impaired mucociliary clearance B. Impaired lymphatic drainage C. Impaired HPV |
C |
|
|
The thoracodorsal nerve arises from A. A Medial cord of brachialplexus B. Lateral cord of brachialplexus C.Posterior cord of brachial plexus D. Dorsal scapular nerve E. Long thoracic nerve |
C |
|
|
Perform a brachial plexus block however the medial forearm is NOT numb. Which nerve has been missed? A. Medial brachial cutanous nerve |
A. Medial ANTEbrachial cutaneous nerve, which is branch of medial cord. |
|
|
Buprenorphine patch taken off. Time taken for plasma concentration to halve?
|
12hours RNSH - Norspan product info = bup. conc fall approx 50% in 12 hours. - Elimination half life 24-37hrs
RPA - Half life of transdermal patch is 26hours while insitu, but 12 hours half life after removing
POW - MIMS = plasma half life of bup. = 12hrs - CEACCP 2005: offset after patch removal is slower dueto the high affinity of buprenorphine for opioid receptors. Patients withsevere side-effects should be observed for 30 h after removal of thepatch. - http://www.butransrems.com. After removal of Butrans, the mean buprenorphineconcentrations decrease approximately 50% in 12 hours (range 10-24 hours) withan apparent terminal half-life of approximately 26 hours.
|
|
|
Incidence of fat embolism following closed femoral fracture? A. 0-3% B. 4-7% C. 8-11% D. 12-15% E. 16-19% |
A. RNSH - 0-3% POW - 1-2% for 1 bone up to 33% for multiple fractures RPA 1-3% |
|
|
Appropriate postoperative maintenance fluid in a child [can't recall situation, but something to do with head injury]: A. 3% and 1/3 NS B. 1/2 NS C. Normal Saline D. Hartmanns E. Hartmanns with glucose |
C. Kerry adds - RCH says: Use 0.9% NaCl (normal saline) plus dextrose as 'maintenance fluid' for any child who has:A brain injury of any sort (meningitis, encephalitis, trauma, febrile convulsion). Boluses: NS Maintenance: 0.45% + 1/5 (or 0.9% + 1/5) |
|
|
Which is a specific PDE inhibitor? A. Theophylline B. Dipyridimole C. Milrinone |
C. Milrinone - PDE3 Theophylline - non-selective |
|
|
Maximum dose of local infiltration of 0.5% bupivacaine in an x kg child? |
A. [dose corresponding to 2.5 mg/kg; there was no option corresponding to 2 mg/kg] RPA = A - but pick 2mg/kg if available RNSH = 3mg/kg |
|
|
Loading dose of IV paracetamol in x kg child?
|
A. ?[dose corresponding to 20 mg/kg]
FRAC article: Oral = 20mg/kg IV loading = 15mg/kg Rectal 30mg/kg
dose for neonates <10 kg is 7.5mg/kg
|
|
|
Performing a caudal block in a child. What is the first sign of a total spinal anaesthetic? A. Hypotension B. Bradycardia C. Desaturation D. Tachycardia E. Loss of consciousness |
C. RPA = There is an Update in Anaesthesia article saying hypotension is uncommon in spinals in children under 5 and respiratory depression more commonly seen! |
|
|
Performing a caudal block in a child and add clonidine to prolong duration of block. What significant complication is increased? A. Sedation B. Urinary retention |
A
POW = CEACCP 2006: Clonidine 1–2 µg kg−1 and ketamine 0.5–1 mg kg−1increase the duration of analgesia by ∼5–10 h when combined with bupivacaine 0.1–0.25% or ropivacaine 0.08–0.2%.4 The combination of S+ ketamine and clonidine isreported to provide satisfactory analgesia for up to 20 h. Both agents, at a higher dose, are associated with a greater risk of sedation, apnoea (particularly neonates and infants) or nausea.
|
|
|
New onset AF. For what period of time is it safe to perform DCCV without prior TOE to exclude thrombus? A. <24 hours B. <48 hours |
B. |
|
|
Regarding remifentanil. All of the following are true EXCEPT:
|
A. Metabolized by plasma cholinesterase = false
RNSH = non-specific tissue and plasma esterase's POW = non-specific plasma esterase's RPA = Metabolised by red cell esterase? Esmolol? |
|
|
Off-label use of a drug refers to all of the following EXCEPT: A. Different age-group B. Different indication C. Different concentration D. Different route of administration |
C NSW health discussion paper: Age, indication, dose or frequency, route of administration, formulation. "‘Off-label’ prescribing occurs when a drug is prescribed for an indication, a route of administration, or a patient group that is not included in the approved product information document for that drug.” Day 2013 "Off-label prescribing" Australian Prescriber.--Farnsworth 09:24, 8 June 2014 (CDT) |
|
|
Regarding mixed venous oxygen saturations: A. 60% is normal B. Can be used to calculate the CO |
B. Normal SvO2 = 65-75% Fick equation: CO = VO2 / a-v O2 |
|
|
Cerebral oximetry measures? A. Arterial saturation B. Mostly arterial saturation and some venous saturation C. Capillary saturation D. Mostly venous saturation and some arterial saturation E. Venous saturation |
D. Venous saturation = 70-75% Arterial = 30-25% |
|
|
Normal systolic BP at birth? A. Something less than 70 mmHg B. 70 mmHg C. 85 mmHg D. Something more than 85 mmHg E. 115 mmHg |
B. 70-80mmHg |
|
|
Epidural block to T2 causes all of the following EXCEPT: A. Bradycardia B. Vasodilatation C. Reduced circulating catecholamines D. Dyspnoea E. Elevated PaCO2 |
E
POW = Thoracic epidural provides thoracic sympathectomy and blockade of cardiac plexus T1-T4 with resultant hypotension, bradycardia and reduction in catecholamines. Dyspnoea is a subjective feeling from blockade of intercostal muscles, however an increase in PCO2 does not occur as adequate ventilation is maintained by the intact function of the diaphragm |
|
|
Preoperative autologous blood donation results in less: A. Cost B. Incompatible transfusion C. Less blood wastage D. Less unnecessary transfusion |
B |
|
|
Penetrating injury to chest. What part of the heart most likely injured? A. RV B. LV C. RCA |
A. RV: 43% LV: 33% RA: 14% LA: 5% |
|
|
TMP-Jul10-056 Regarding a Thallium scan: A. High NPV B. Less useful in comparison to a DSE |
A. |
|
|
What is NOT a contraindication to MRI? A. Pulmonary artery catheter B. Arterial line C. Scissors D. Coiled ECG cable E. Laryngoscope |
B |
|
|
Skin between iliac crest and greater trochanter supplied by? |
A. Subcostal nerve RPA = A (T12) RNSH = iliohypogastric - suprapubic skin ilioinguinal - scrotum and upper thigh |
|
|
Regarding pyloric stenosis: A. More common in females B. Occurs most commonly in [some incorrect age group] C. Acidic urine D. Cause of hypokalemia is vomiting |
C. More common in males Usually occurs in 2nd to 6th week of life Urine: initially alkaline urine to maintain serum pH, then acidic urine with depletion of electrolytes and hypovolaemia --> conserve Na+ and excrete H+ Hypokalaemia --> due to renal losses to maintain Na+ |
|
|
In comparison to Mallampati test, the TMD is: |
A. Less sensitive, more specific RNSH - mallampati - poor sensitivity 49% and moderate specificity 80% - TMD sensitivity 20% and specificity 94% |
|
|
Systematic review. What is NOT a weakness? A. Systematic review author bias B. Publication bias C. Duplicate publication D. Heterogeneity E. Inclusion of historic studies |
A. In using a rigorous process to determine what types of studies will be included in a systematic review, author bias is usually eliminated, andgreater credibilitycan be placed in the findings from the review. ?but what about the author of the systematic review and their bias? |
|
|
Traumatic liver laceration. Conservative management is indicated if? |
A. Haemodynamically stable |
|
|
Initial dose of IV GTN to relax the uterus is? A. 5 mcg B. 50 mcg C. 200 mcg |
B. RHW: Diluteinto 50mcg/ml. Give 1ml every 1-2 mins as needed up to a maximum of 10mls. |
|
|
Dilated CM (LVEF 30%). No dyspnoea with ADLs. Best management? A. Start ACEI B. Stop beta-blocker |
A. |
|
|
CTG [pictured] demonstrating late decelerations. Most likely cause? A. Fetal asphyxia B. Head compression C. Cord compression D. Uteroplacental insufficiency |
A. Head compression = early decels Cord compression = variable decels Uteroplacental insufficiency = chronic condition, tested for by foetal size and umbilical doppler |
|
|
C6/7 muscle movements: |
A. Wrist flexion and extension |
|
|
Paraesthesia in little finger during supraclavicular block. Likely contacting? |
Ans on black bank = Medial cord RPA - Medial cord gives off Ulnar but you should be around the trunks with a supraclav block so likely inferior trunk RNSH - ?lower trunk - medial cord in axilla |
|
|
Rpt: Sensitivity 90% and Specificity 99%. |
A. False positive rate 1% |
|
|
SVRI. A. SVR x BSA B. SVR / BSA |
A |
|
|
PP22 Features of Pierre-Robin syndrome include cleft palate, micrognathia, and? A. Glossoptosis B. Microstomia |
A |
|
|
Ratio of MAC incision to MAC awake for sevoflurane? |
A. 0.34 |
|
|
Rpt: Essential feature of LBBB includes? A. Loss of QW's in V5-6 B. RSR in V1 C. Deep SW in V6 D. QRS duration > 0.2 secs |
A Absent Q waves in Lead 1, V5-V6 Wide S wave in V1 Wide notched R wave in V5/V6 QRS > 120msec (0.12sec) |
|
|
Rpt: Best indicator of opioid induced respiratory depression? A. Sedation score B. RR C. SpO2 D. HR |
A |
|
|
Rpt: Intraoperative pediatric arrest during scoliosis surgery most likely due to? A. A delay in delivery ofblood from the blood bank B. Inadequate intravenousaccess C. Underestimated intra-operative blood loss D. Underestimatedpre-operative hypovolaemia E. Complication oftransfusion |
C. |
|
|
Rpt: Residual Current Device installed. Electricity mains remains on. Touch neutral and ground. |
A. Nothing will happen RCD - disconnects circuit whenever current is not balanced - prevents electrocution. |
|
|
TMP-Jul10-043 Severe asthma attack. Given continuous nebs & IV hydrocortisone but not responding. PaCO2 low. SpO2 low. Next appropriate treatment? A. IV Magnesium B. IV Aminophylline C. Heliox D. IV salbutamol infusion E. Intubate/ventilate |
A. |
|
|
Rpt: ASD murmur is due to flow through which valve? |
A. Pulmonary valve Flow murmur due to inc RH volume/pressures |
|
|
Rpt: Best position for IABP is 1-2 cm: A. Distal to Left SCA B. Proximal to Left SCA C. Distal to artery of Adamkiewicz D. Distal to renal artery E. Proximal to renal artery |
A |
|
|
Rpt: Blood flow across which valve is used to estimate PASP during echocardiography examination? |
A. TV |
|
|
Rpt: Cephalothin spectrum of activity does NOT cover? |
A. Pseudomonas (need a 4th gen)
Covers strep and staph Not enterococci or lysteria Covers gram -ve: ecoli and most kelbsiella Not serratia, enterobacter, pseudomonas |
|
|
Rpt: With regard to CHADS2 score. All EXCEPT? |
A. Gender C - CCF H - HTN A - Age >75 D - DM S2 - Hx of stroke / TIA (2 points) |
|
|
Rpt: 60kg female given 50mg rocuronium. Dose of sugammadex to reverse? |
A. 960 mg (16mg / kg) |
|
|
Rpt: Serum c/Ca++ 2.05 mmol/L in CKD patient. Most likely cause? |
A. Secondary hyperparathyroidism |
|
|
Rpt: Post CEA seizure. In order to prevent further seizures? A. Add/start antihypertensive B. Start anticonvulsant |
A Hyperperfusion synderome - dramatic inc in CBF after CEA --> ipsilateral headache, HTN, seizures, focal neurology. Rx = aggressively reduce BP |
|
|
Rpt: According to ANZCA-endorsed labelling standards a brachial plexus catheter should be labelled? A. Pink B. Blue C. Yellow. D. Beige E. Red |
A. Yellow Yellow = nerves Beige = s/c Pink = misc Blue = IV Red = IA |
|
|
Rpt: Conn's syndrome? A. Hypernatremia, hypokalemia, normoglycemia |
A Primary hyperaldosteronism: -HTN due to Inc Na+ and extra cellular volume -Low K+ and alkalosis due to renal excretions |
|
|
Rpt: Area burnt? (1/2 upper limb + anterior abdomen + whole lower limb) |
A. 32% |
|
|
Rpt: Dural Sac ends at what level in a neonate? A. L1 B. L3 C. L5 D. S1 E. S3 |
E. Conus medullaris L2-3 (adults L1) --> LP below L2-3 Dural sac ~ S3 (adults S1) |
|
|
Rpt: SpO2 90%. No IV access. Place LMA and laryngospasm. Most appropriate course of action? A. Increase inhaled sevoflurane concentration with LMA in situ B. Increase inhaled sevoflurane concentration after removing LMA C. Intralingual suxamethonium (no dose stated) D. Intramuscular suxamethonium (no dose stated) E. Intramuscular atropine (no dose stated) |
B. Remove irritants Deepen anaesthesia Muscle relaxation |
|
|
Rpt: Clopidogrel half-life? |
A. 6 hrs |
|
|
Rpt: Which of the following is not a MAJOR complication following mediastinoscopy? A. Air embolism B. Cardiac laceration C. PTX D. Tracheal compression |
B |
|
|
Rpt: What sign most suggests a significant murmur in a child? A. 4/6 loudness B. vibratory/flutter sound |
A |
|
|
Rpt: Thermoneutral zone in 1 month old child? A. 26-28 degr C B. 29-31 degr C C. 32-34 degr C |
C 34-36 for a neonate |
|
|
Rpt: Indicative of severe AS? A. Palpitations B. Fatigue C. PND D. Angina E. Syncope |
C |
|
|
Rpt: Risk factor for PPH? A. Prolonged labour B. Age <20 yrs old C. Primiparity D. FV Leiden Deficiency E. Oligohydramnios |
A |
|
|
Rpt: Muscle observed when monitoring the NMJ and stimulating ulner nerve? A. Adductor pollicis B. Abductor pollicis brevis C. Flexor pollicis brevis |
A |
|
|
Rpt july 2007: The correct ranking of Fat/Blood partition co-efficients, in order of increasing solubility in fat, for sevo, des, iso and N20? A. N2O< Des < Sevo = Iso B. N2O = Des < Sevo <Iso C. N20 < S <D < I D. D< N20 < S < I E. D < N20 = S < I |
A N2O > Des > Sevo~Iso
N2O 1.4 Des 29 Sevo 80 Iso 98 |
|
|
Rpt: Induction/LMA in ?kg child. Develops SVT. Most appropriate course of action? |
A. Adenosine 100 mcg/kg POW - OHCA (paeds): If inshock and no IV access – DC shock. If have IV asccess give 50mcg / kg, then100mcg / kg, then 250mcg / kg. |
|
|
Rpt: Clinically the most significant murmur in pregnancy is? |
A. MS |
|
|
Rpt: Required for diagnosis of Neuroleptic Malignant Syndrome? A. Muscle rigidity B. Elevated CK |
A Severe muscle rigidity, inc temp, plus 2 or more of: confusion, inc HR, tremor, incontinence, reduced speech, inc BP, inc WCC, inc CK. |
|
|
Rpt: Hyponatremic child intubated/ventilated in ICU following seizure. Treatment? |
A. Hypertonic saline (no dose/infusion rate given) Give 3%NaCl until Na+ is >125 or until seizures stop. Give 4ml/kg over 15-20min. |
|
|
Rpt: Weakness of proximal and distal muscles following an URTI 10/7 ago. No sensory involvement. T 37.8 degr C. Most likely diagnosis? |
A. Guillain-Barre Progressive bilateral weakness in legs and arms over 2-4 weeks Areflexia Mild sensory changes with no level CN involvement Spontaneous recovery 2-4weeks ANS dysfunction No fever at onset |
|
|
Rpt: Post-operative develops severe CP and ST elevation in PACU. Most appropriate initial treatment? A. ASA B. beta-blocker C. IV heparin infusion |
A. ASA = Aspirin |
|
|
Rpt: Circuit disconnect during spontaneous breathing may be detected by? A.Will be reliably detected by a fall in end-tidal carbon dioxide concentration B.Will be detected early by the low inspired oxygen alarm C. Will be most reliably detected byspirometry with minute volume alarms D. May be detected by an unexpecteddrop in end-tidal volatile anaesthetic agent concentration E. Canbe prevented by using new, single-use tubing |
D. An unexpected drop in ET agent or C? |
|
|
Time-constant? [formula] |
A. Resistance x Compliance |
|
|
Rpt: Neonate - main resistance in circle is due to? |
A. ETT |
|
|
Rpt: Iron deficiency anaemia: A. Low ferritin, low serum iron B. Low ferritin, low TIBC C. Elevated ferritin, low marrow iron D. Elevated ferritin, ? E. Elevated ferritin, ? |
A. Iron def anaemia: Low serum iron, low retic count, low ferritin, low transferrin saturation. High transferrin and TIBC - inc production in liver = attempt to carry as much of the little iron that is available. |
|
|
Rpt: Long-standing T6 paraplegia. Which is INCORRECT? A. Flaccid paralysis B. Poikilothermia C. Labile BP |
A. = involuntary spasms due to overactive SNS Poikilothermia is the inability to maintain constant core temp. |
|
|
Rpt: Lap chole on citalopram. What is NOT relatively contraindicated? A. Omeprazole B. Clonidine C. Pethidine D. Tramadol E. Midazolam |
RNS = E>B POW = B>E RPA = B
Omeprazole - may inc serum conc of SSRI via in of CYP219 Clonidine - [RNSH - case report in BJA]
SSRIs may interact with MAOIs or methylene blue and cause serotonin syndrome. Common causative agents: Tramadol, Pethidine, and care with indirect acting sympathomimetics. Fluoxetine also a potent inhibitor of CYP450 enzymes – 2D6 (Codeine), 2C19 (Plavix) and CYP 3A4 (Midazolam and Omeprazole)
|
|
|
Rpt: Most effective treatment for post-sevoflurane agitation following grommets in a 4yo child? A. 1 mg/kg propofol B. 1 mcg/kg fentanyl C. 1 mcg/kg clonidine D. ?dose midazolam E. Sucrose |
POW = A RPA = B>A less n/v than fentanyl but better with increase prolific dose of 2.5mg/kg in tittered aliquots RNSH = A. or B if higher dose. [2.5mcg/kg fentanyl causes significant red. in emergence] |
|
|
Rpt: What is NOT useful in the treatment of Torsades? A. Isoprenaline B. Procainamide C. DCCV D. Electrical pacing |
B. Prolongs QT |
|
|
Rpt: MS and tachyarrhythmia; hypotension? What management? |
A. DCCV |
|
|
Rpt: Little space between epiglottis and posterior pharyngeal wall. Modified C&L classification? |
A. IIIa Grade I = most glottis Grade II = (a) some of glottis (b) Only posterior extremity of glottis seen or only arytenoid cartilages Grade III = (a) only epiglottis lifted off the wall (b) only epiglottis with no space Grade IV = no laryngeal structures |
|
|
2 similar Rpts involving: Numb tongue and impaired taste sensation post LMA anaesthesia. A. Facial Nerve B. Mandibular division of CNV C. Lingual Nerve |
C. Facial nerve = taste Mandibular division of CNV = sensory ant 2/3 tongue Lingual nerve (branch of V3)= mucosa ant 2/3 |
|
|
Rpt: Lateral approach to popliteal block. A. Passes through semimembranosis B. May be performed supine or prone C. Adequate for ankle surgery D. Less effective in comparison to posterior approach E. Eversion is an endpoint for nerve stimulation |
B.
A. Passes through Biceps femoris B. May be performed supine or prone [NYSORA describes both approaches] C. Adequate for ankle surgery [Need femoral branches as well (or at least saphenous branches)] D. Less effective in comparison to posterior approach [RPA = true, RNSH = both are comparable] E. Eversion is an endpoint for nerve stimulation [RPA Eversion for common peroneal but you'll also seek inversion (and plantarflexion) for Tibial]
|
|
|
Rpt: Risk factors for postoperative ulnar nerve injury? |
A. Contralateral arm RPA - Often have subclinical palsy contralat POW - say main RF is diabetes RNSH - RF = male, DM, inc age, thin, prolonged hospital stay |
|
|
Risk factors for postoperative ulnar nerve injury? A. is more common in diabetics B. is more common in women C. is often associated with contralateral clinical neuropathy D. isusually found to be the result of excess external pressure E. usually presents within 24 hours |
A [POW] |
|
|
Rpt July 2007 Q35: In a rotameter the: A. Bobbin spins inside a tube that has parallel sides B. Flow is laminar at high flow rates C. Height of the bobbin is proportional to the pressure drop across the bobbin D.Pressure drop across the bobbin is constant at varying flows E. Resistance increases with increasing gas flow
|
D Pressure drop across the bobbin is constant at varying flows Read from the middle of the ball |
|
|
Rpt: SAH. Hyponatremia. Elevated urinary Na concentration. Most likely cause? A. CSW B. SIADH |
B CSW = low serum Na, high serum osmol, high or norm urine osmol, hypovolemic. SIADH = hypotonic hypoNa+, urine osmol>serum osmol, urine Na >18, normovolemia. |
|
|
Rpt: Urgent reversal of INR 4.5. Intern already gave vitamin K. A. FFP B. Prothrombinex C. Prothrombinex AND FFP |
C. If warfarin related reversal: PTX 25-50units/kg FFP 150-300ml to provide factor 7 |
|
|
Rpt: Major cause of death following difficult intubation with perforated oesophagus? A. Sepsis B. Failure to intubate C. Failure to ventilate |
A. is consensus |
|
|
Rpt: Labour epidurals may cause maternal fever. This leads to: |
A. Increased investigations for neonatal sepsis |
|
|
Rpt: ASA grading was introduced in order to: |
A. Standardize description of physical status |
|
|
Rpt: Lignocaine vs bupivacaine potency: |
A. Four times |
|
|
Rpt: Best agent to decrease both gastric volume and gastric acidity? A. Omeprazole B. Ranitidine C. Metoclopramide D. Cisapride E. Na citrate |
B |
|
|
Rpt: Cholecystectomy. A. Most likely to get gas embolism at initial CO2 insufflation |
A |
|
|
Rpt: Diastolic dysfunction is NOT caused by? A. Adrenaline B. Constrictive pericarditis |
A |
|
|
Rpt: AFE early cause of death? A. Pulmonary HTN |
A |
|
|
Rpt: Nerve block anterior 2/3rds of ear? |
A. Auriculotemporal nerve. |
|
|
Rpt: Fixed, dilated pupil in trauma patient? |
A. Transtentorial herniation |
|
|
Rpt: Central anticholinergic syndrome, INCORRECT statement? A. Neostigmine will reverse |
A Requires physostigmine |
|
|
Rpt: MH diagnosis? |
A. Muscle rigidity |
|
|
1) Indication for IE prophylaxis in pt with CHD: a) Gastroscopy with biopsy b) Dental with RCT C) D&C |
B. Indications: Prosthetic valve Previous IE CHD if: unrepaired cyanotic defect, 6months after repair, repair with residual defects Cardiac transplant and vavuloplasty RHD in indigenous patient |
|
|
List of other questions: 2) Repeat: Indication for IE pro - Uncorrected CHD 3) Half life of Clopidogrel - 6 hrs 4) TRALI 5) CHADS2 6) Nerve block cathetre colour code 7) Penetrating injury of chest - RV |
:) |
|
|
8) Meconium stain liquor - Suction Trachea 9) Time constant - RXC 10) Dura in child ends at -S3 11) GCS calculation 12) Pirrer robins syndrome 13) Adductor pollicis |
:) |
|
|
14) Post endaretrectomy with seziure -Add antiHT 15) Severity of AS - pnd 16) Neonate Loss of heat - Radiation 17) Circuit disconnection -End tidal agent 18) FAT: BLOOD 19) Mallampatti vs Thyromental |
18) N2O < D < S > I 19) less sensitive and more specific |
|
|
20)Thallium role in prediction of perioerative MI 21) PPH - Prolonged labour 22) ( ME 47)Features of Conn synd 23) ( ez 94)Handyman with neutral and ground - Nothing will happen 24)( ru12) Paraesthesia in little finger - Lower trunk IC97 Bleeding in trauma - Tranexamic acid |
22) Hyperaldosterone, Inc Na+, Low K+, normal BSL TXA - Crash2 study |
|
|
26) Optimal dose of GTN - 50 MCG 27) Sever MS with tachy and hypo - DC shock 28) MAC Awake : MAC Sevo - 0.34 29) PCA monitoring - Secation score 30) 50 mg Rocuronium - Reversal with 960 mg Suggamadex 31) Post hyponatremia sezuire in child - Hypertonic Saline |
:) |
|
|
32) ( EZ79) Circuit resistance in neonate -ETT 33) PA pressure across which valve in ECHO - Tricuspid 34) Monitoring in Preg beat to beat variablit - 24 wks 35) SE of cyclosporin - Alopecia 36) ( q 122) Diagnosis of NMS - Diaphorosis 37) Cepahlothin not efffective against - Pseudomonas |
36) Major: rigidity, fever, inc CK. Minor: Inc HR, BP, and RR. Diaphoresis, leucocytosis. |
|
|
38) Dialated cardiomyopathy with no symp -ACE inhibitors 39) Child with WPW syndrome with intraop tachy , drug of choice - Amiodarone 40) Haemophilia A patient will have - Nml PT and Abnml aPTT 41) Cause of hypoxia in OLV - Blood flow to upper lung 41) Compairing New instrument of BP measurement with gold std - choice of test 42) Air bubble in IA line - decreased RF |
39) NOT dig, BBlocker, Ca blocker, adenosine (risk of VF with last) |
|
|
43) LBBB in ECG features 44) Tip of IABP - 2 CM distal to lt subclavian 45) 70 yrs post hip with crusing chest pain - aspirin 46) Feature of long standing cord paralysis all except - paraplegia 47) SVRI - SVR X BSA 48) ( AT 27) Left sided pneumonectomy , for chest drain - |
46) flaccid paralysis |
|
|
49) ETT over bougie - rotate anticlockwise 50) SSEP monitors - Dorsal column 51) Death in esophageal perforation - Sepsis 52) Role of C6-7 - Wrist flexion and extension 53) Modified CM score for laryngoscopy - 3a 54) Iron deficinecy - Low ferretin , Increased TIBC |
:) |
|
|
55) Popliteal by lateral approach - Foot eversion 56) ( EZ93) Chemical for sodalime change - Ethyl Voilet 57) Pathological Murmur in child - 4/6 58) FOB see trifurcation - RT UL 59) Consent/ Ethics question 60) Not a disadv of flow over vaporiser - |
:) |
|
|
61) All need reduced dose in renal failure except -Bupernorphine 62) Post induction larungospasm in child - Increase sevo and remove LMA 63) Investigation of choice in dissection of aorta in hemodynamic unstable adult - Aortogram 64) Peak incidence of vasospam post SAH - 65) Risk of stroke in pt with AF per day - 0.01 % 66) Absent q wave feature of all except - Digitalis toxicity |
63) ?TOE 64) 6-10days |
|
|
67) Sever asthma with all treatment given - Magnesium 68) Most cause of awareness - 69) Post cervical spine op distress in recovery - inhalation innduction 70) Most effective way to reduce renal failure in AAA surgery - Minimize cross clamp time 71) CO2 is used in pneumoperitoneum - less effect if venous air emboism 72) Malignant hyperthermia most common sign - Tacy |
68) human error |
|
|
73) Best indicator for trauma resus - Lactate 74) ASD murmur across - Pulmonary valve 75) Method to improve aponic oxygenation - Head up 76) Finding against AFE - 77) Nerve injury following LMA with loss of sensation in ant 2/3rd - Branch of Mandibular nerve 78) Loss of taste and sensation in ant 2/3 - Lingual / Corda tympani |
:) |
|
|
79) Mode of monitoring in neuro surgery - PTC 80) Termoneutral zone in 1 mth old neonate - 81) Supply of carotid sinus - Glossopharyngeal nerve 82) Weakness of systemic reivew all except - 83) All used to prolong preg except - Indomethacin 84) Absolute C/I for sitting position surgery - Small PFO vs/ Shunt |
:) |
|
|
85) Drug must be given based on IBW - 86) Supply of skin between greater trochanter and _ : subcostal 87) Thraco dorsal is branch of posterior cord 88) Pt on diabigatram for AF coming surgery after 10 day , most appropriate thing to do - 89) Conservative mgtm in aortic dissection - Stanford B 90) Low serum sodium with high urinnary sodium - |
:) |
|
|
91) Plasma glu vs Blood glu 92) First sign of total spinal in neonate 93) Arndt blocker ( Pic) 94) RCA supply AV node in how many persantage of population 94) Artery suppling anterion papillary muscle ( Pic) 95) CTG corresponds to - ( pic) |
:) |
|
|
96) Best agent to decrease the gastric volume - H2 blocker 97) Exact loading dose of iv paracetamol - 98) Percentage of women get post partal headche - 99) Histamine causes all except - Myocardial depression 100) All can cause injury during MRI except - IA line 101) SE 99, SP 90 - FP 1 |
:) |
|
|
102) Effect of trendelenburg - increased myocardial work 103) Pyloric stenosis kid can present with - Acidification of urine 104) 12 yrs old had eaten and trauma - RSI with ETTT 105) Maintenance Fluid of choice for child on ventilator in ICU with closed head injury 106) Most common cause of post op visual loss - ION 107) ( MZ Q96 AUG 08) Feauture of AS all except - Anemia > 85% |
:) |
|
|
108) ( NH Q 139 AUG 08) Ciliary ganglion - parasympathetic fibre from EW nucleus 109) Thoracic epidural helps with all except - circulating catecholamine levels 110) Witnessed VF - Defib 111) Motor cyclist RTA with chest Xray suggestive of gas with fluid level in Left thorax - Rupture diaphragm 112) Best inndicator for difficult intubation in obesity - increased soft tissue in suprathyroid region 113) Low venous oxygen does not affect? |
:) |
|
|
114) 40 mg Oxycodone + 20 mg Naloxone combined tabalet, useful for- 115) ?? about what would exclude a child from MH 116) Larger area of back to be resected in 25 kg child surgeon wants to use 0.5% bupivacaine - volume allowed? 117) COX inhibitor ? 118) Absolute CI for ECT - Increased ICP VS Resent MI 119) Complication of Mediastinoscopy all except - Cardiac laceration |
:) |
|
|
120) Entropy with difference in SE and RE - 121) Rotameter with circular bobbin - pressure drop across in constant 122) Lung transplant preserved function - HPV 123) Percentage area of Burns in Half of upper arm, full lower leg and ant abdominal wall - 32 124) PONV?? 125) Pressure range allowed for type c cylinder - Different range |
:) |
|
|
126) Cylinder with grey shoulder and white body - Air/ Co2/ N2o/Nitrous 127) True about remifenatly all except - 128) ? GABA 129) ( Aug 2005)Caused of inverted P wave in lead 2 includes all except - 130) All associated with Ulcerative colitis except - Psoriasis 131) Muscles which separate vocal cords - Post cycricaretyenoids ??? |
:) |
|
|
132) Constant sparing of medial aspect of fore arm sensation following brachial plexus block is indicative of sparing of - 133) 20 kg child suffered 15% burns 6 hrs after amt of fluid to be given? 134) When will palsma bupernorphine level ll fall to half after discontinuation of cutaneous patch? 135) Time till cardiovesion can be comfortably done after new onset AF without ECHO- 24, 48, 72 hrs |
:) :) |

