![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
63 Cards in this Set
- Front
- Back
|
0.5 McFarland Standard = ? |
Barium sulfate standard that equals the turbidity of 10^8 bacteria |
|
|
Agar Disk Diffusion/Kirby Bauer Method |
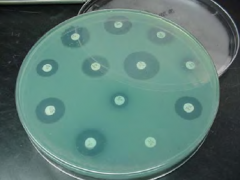
Mueller Hinton agar 150 mm plate diameter 4 mm in depth Specifically calcium and magnesium balanced 6mm paper disk with single antibiotic |
|
|
E Test |
![Calibrated plastic strips impregnanted with antibiotic [ ] gradient
MIC is where ellipse ends](https://images.cram.com/images/upload-flashcards/69/43/76/9694376_m.png)
Calibrated plastic strips impregnanted with antibiotic [ ] gradient MIC is where ellipse ends |
|
|
Broth dilution ? |
0.5 McFarland standard - further diluted to 5 x 10^5 organisms/mL
-Suspension inoculated into tubes/trays containing growth medium and known 2 fold dilutions of antibiotics -Must have 4 or more dilutions to be true MIC |
|
|
Disk test for beta lactamase detection? |
-Add bacteria to filter paper impregnanted with Nitrocefin (chromogenic cephalosporin) -Incubate at RT 30 sec to 60 min (depends on bacteria)
-Positive result is change from yellow to red -Beta lactamase enzyme breaks down beta lactam ring to form hydrolyzed red end product -Detects resistance to Amp/Pen/Ceph |
|
|
MRSA resistance |
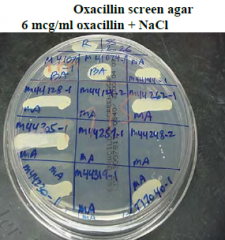
-Resistance by penicillin binding proteins (PBP) via mecA gene
-Test oxacillin in lab (more stable) - if resistant, all cephalosporins are reported as resistant
-Newer method uses cefoxitin for greater sensitivity |
|
|
Clindamycin Induction (D Test) |

-To determine if S. aureus/MRSA is susceptible to Clindamycin -S. aureus/MRSA resistant to erythromycin and susceptible to clinda have to be tested -Zone around clinda disk will be blunted to form D if clinda can be induced by erythro to be resistant |
|
|
Enterococcus resistance + synergy |
Naturally resistant to: Cephalosporins Clindamycin TMP/SXT
Synergy: Ampicillin + Gentamycin |
|
|
Vancomycin resistant enterococcus (VRE) |
Acquired resistance to vancomycin: -plasmid mediated vanA - E. faecium -plasmid mediated vanB - E. faecalis
Drugs of choice: Linezolid & Synercid |
|
|
Extended spectrum beta lactamase (ESBL) production |
E. coli, Klebsiella, and Proteus mirabilis ONLY have CLSI methods for detection
-Via Tem 1 beta lactamase plasmid
-Report all cephalosporins and penicillins as resistant -Drug of choice Imipenem, Pip/Tazo - blocks beta lactamase function
-Clavulinic acid = beta lactamase blocker |
|
|
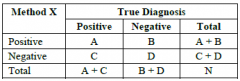
Klebsiella pneumonia carbapenemase |

-Carbapenemase producing -Hyper beta lactamase producer plus resistance to carbapenems (Imepenem)
-Most sensitive screen for KPC is Ertapenem = increased MIC
-Lawn of E. coli, streaks of test GNR -A,B,E positive |
|
|
Streptococcus pneumonia and resistance to penicillin |
1) Oxacillin KB disk test 2) Confirmation of resistance by penicillin MIC testing with E test or broth dilution
Sensitive (<0.06 mcg/mL for CSF infections & <2 mcg/mL for respiratory/blood infections) Resistant (>2 mcg/mL for CSF infections & >8 mcg/mL for respiratory/blood infections)
-If resistant use cefotaxime, vancomycin or a quinolone |
|
|
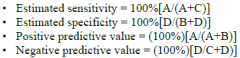
|
|

Chlamydia culture |
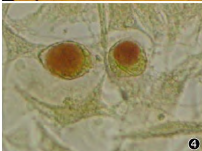
-McCoy cells with iodine or DFA staining vacuole -Elementary bodies = small extracellular bodies |
|
|
Clostridium difficile |
-NAP1 strain = hyper-virulent with increased spore toxin production
-Toxin A (enterotoxin) -Toxin B (cytotoxin)
PCR test of choice |
|
|
Phenylethyl alcohol |
Selects for gram positive cocci |
|
|
MacConkey agar |
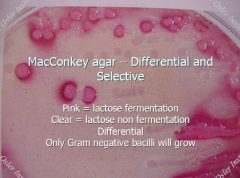
Selects for gram negative bacilli and differentiates lactose fermenters |
|
|
Staphylococcus aureus |
1) Virulence Factors: Protein A - capsular polysarccharides, enzymes (coagulase), toxins and hemolysins
2) Diseases: Toxic shock syndrome (TSST-1), scalded skin syndrome (Exfoliatin, SSS), soft tissue skin infections (Panton Valentine leucocidin - PVL), food poisoning (enterotoxins), bacteremia, and endocarditis |
|

|
S. epidermidis - Novobiocin sensitive -Pathogenesis from cell adhesion factors forming biofilms on biologics & plastic
S. saprophyticus - Novobiocin resistant -UTIs in child-bearing age female |
|
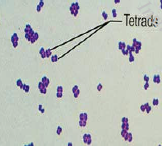
Micrococcus: gram positive cocci in tetrads |

Catalase Negative Bright yellow pigment Bacitracin Susceptible Microdase test + (modified oxidase reaction) Does not ferment glucose (staph does)
|
|
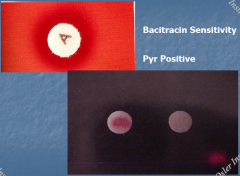
|
S. pyogenes: Beta-hemolytic Group A strep PYR + Bacitracin & Penicillin susceptible SXT resistant |
|
|
Streptococcus pyogenes |
Virulence Factors: M protein - resistance to phagocytosis Capsule - hyaluronic acid - resistant to complement-dependent killing Streptolysin O (oxygen labile) & Streptolysin S (oxygen stable) Streptococcal pyrogenic exotoxins |
|
|
Streptococcus pyogenes |
Diseases: Pharyngitis Impetigo Erysipelas Cellulitis Puerperal sepsis Toxic shock
Sequelae: Rhematic fever & glomerulonephritis |
|

S. agalactiae
-S. aureus strain with camp factor perpendicular to group B strep = flare of hemolysis |
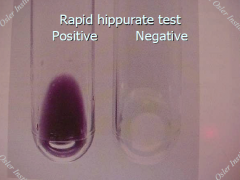
Group B strep = S. agalactiae beta hemolytic Catalase negative CAMP test + Hippurate + (purple) Penicillin, Vanco S |
|

Enterococcus |
Enterococcus: Gamma hemolytic streptococcus Bile esculin + 6.5% salt + PYR + (pink) E. faecium = arabinose fermentation + E. faecalis = arabinose - Natural resistant to cephalosporins Tx with Amp/Vanc |
|
|
Streptococcus Group D, not enterococcus |
S. bovis: Gamma hemolytic Bile esculin + 6.5% salt - PYR - -Associated with bowel carcinoma Always susceptible to penicillin |
|
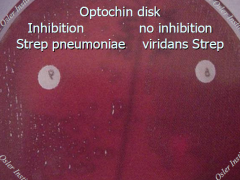
Alpha Hemolytic Streptococcus
-Optochin = ethyl hydrocupreine hydrochloride |
S. pneumonia: Lancet-shaped Optochin sensitive Bile soluble Acquired R to Penicillin by PBP Quellung reaction to type
Viridans strep: S. mutans, S. salivarius, S. sanguis, S. mitis Optochin resistant Bile esculin - Not bile soluble |
|

Nutritionally variant Strep
-Vit B6 provided by S. aureus |
Vitamin B6 (pyridoxal) dependent -Needs S. aureus streak to grow "satellite" or media supplemented with B6
Speciated: 1) Abiotrophia 2) Granulacatilla
Can cause endocarditis, more resistant to antibiotics |
|
|
Gram Negative Cocci
Neisseria
Moraxella catarrhalis |

Positive - turns from pink to yellow |
|
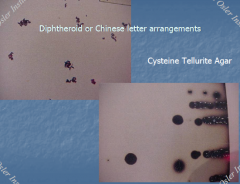
Corynebacterium diphtheriae |
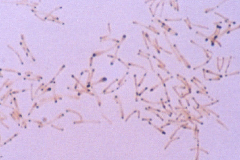
C. diphtheriae: -phage mediated toxin -Cysteine tullerite agar - black colonies with brown halos -Grow on egg containing Loeffler slant then stain with methylene blue = metachromatic granules |
|
|
C. jeikeium: 1) Pts with plastic catheters and indwelling devices 2) R to most antibiotics 3) Tx with Vancomycin & tetracycline |
C. urealyticum: 1) Rapidly urease positive diphtheroid found in urine cultures 2) Alkaline-encrusted cystitis |
|

Bacillus species |
Gram + bacilli, boxcar shaped, spore-forming
B. anthracis: -medusa head colonies on BAP -non-hemolytic, non-motile, Penicillin S
B. cereus: -cereulide = emetic toxin -beta-hemolytic, motile |
|
|
Listeria monocytogenes |
Small gram positive rod Catalase + Beta-hemolytic colony Intracellular pathogen Tumbling motility Cold loving - 4 degrees Celsius |
|
|
Erysipelothrix rhusiopathiae |
Gram + rod Catalase - Alpha hemolytic colony **Only gram + rod that produces H2S (TSI) **Strongly associated with endocarditis in drug addicts |
|
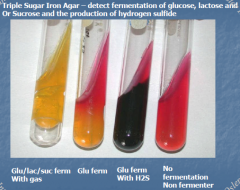
Triple Sugar Iron Agar |
Detect fermentation of glucose, lactose, and/or sucrose and the production of hydrogen sulfide
Pink = no fermentation Glucose at bottom Lactose/Sucrose at top |
|
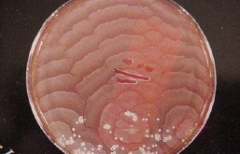
Proteus: non-lactose fermentation P. vulgaris - indole + P. mirabilis - indole -
|
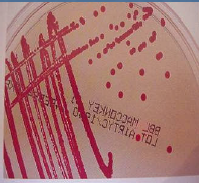
Serratia marcescens: red pigmentation infection in immune suppressed |
|
|
Salmonella diarrhea, polys in stool Selective media - Hektoen and SS Does not ferment lactose Produces H2S Identification based on Kaufman White type scheme O - somatic antigen - cell wall H - flagellar antigens - 2 phases, h1 & h2
|
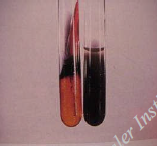
S. typhi: Vi capsular antigen and D somatic antigen Moustache of H2S in the TSI tube Carrier state in gallbladder |
|
|
Shigella |
gram negative bacilli diarrhea, blood in stool non motile no H2S production non lactose fermenter
4 species: S. boydii - group C S. dysenteriae - group A S. flexneri - group B S. sonnei - group D |
|
|
Yersinia enterocolitica |
diarrhea septicemia in iron overload syndromes mesenteric adenitis - mimics appendicitis grows well at 4 degrees C (like Listeria) CIN agar (cefsulodin-irgasan-novobiocin)
|
|
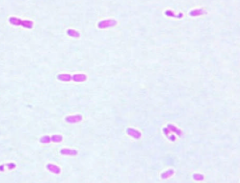
Yersinia pestis
safety pin - bipolar staining |
obligate flea-rodent-flea life cycle Flea bite leads to bubonic form with painful buboes pneumonic form - bacteremic spread or patient to patient southwestern part of US grows on BAP, catalase +, oxidase - gram negative rod |
|
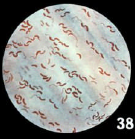
Vibrio cholerae -glucose fermenter -oxidase + |
1)gram negative bacillus - comma-shaped 2) toxin - receptor on endothelial cell - activates adenylate cyclase - increases cAMP - hypersecretion of salt & water 3) Halophilic, 1% salt enhances growth 4) TCBS = thio citrate bile sucrose - turns yellow due to sucrose fermentation 5) 01 most virulent - classic & El Tor - toxin + |
|
|
Other Vibrio species -glucose fermenters, oxidase + |
V. parahemolyticus: 1) sucrose neg - green on TCBS 2) diarrhea from ingestion of raw fish & shellfish
V. vulnificus: 1) painful lower limb bullous lesions 2) septicemia in pts with pre-existing liver disease 3) lactose + - green or yellow on TCBS |
|
|
Glucose non-fermenters Oxidase negative |
Acinetobacter: 1) Nosocomial pathogen 2) Gram neg coccobacillus - big diplococci 3) A. baumannii - glucose oxidizer 4) A. lwoffi - glucose non-oxidizer
Stenotrophomonas: 1) Rapid maltose oxidizer 2) Naturally resistant to Imipenem |
|
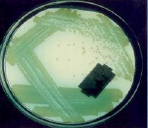
Pseudomonas aeruginosa |
1) Fluorescent pigment & blue-green pigment (pyocyanin) 2) Grape-like odor 3) Grows at 42 degrees celsius (P. fluorescens/putida don't) 4) Major pathogen in CF along with Burkholderia cepacia |
|
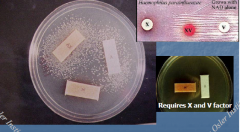
Haemophilus |
H. influenza: 1) Requires X (hemin) and V (NAD) 2) 15-20% R to Amp by beta lactamase production H. parainfluenza: 1) Requires V only H. aphrophilus: 1) Doesn't require X or V H. ducreyi: 1) Requires X |
|
|
HACEK Group |
Haemophilus acrophilus = oxidase -, catalase -
Actinobacillus actinomycetom-comitans = oxidase -, catalase +
Cardiobacterium hominis = oxidase +
Eikinella corrodens = oxidase +, pits on BAP
Kingella kingii = oxidase +, hemolytic on BAP |
|

Bordetella pertussis |
1) Gram negative coccobacillus 2) Direct detection by fluorescent antibody 3) Regan Lowe charcoal agar - bluish colonies 4) Cough caused by toxin adhering to bronchial epithelial cells |
|
|
Pasturella multocida |
1) Small gram negative coccobacilli 2) Cat & dog bites, normal flora in animal's mouth 3) Grows on blood, not MacConkey agar 4) Sensitive to penicillin 5) Oxidase +
|
|
|
Brucella |
1) Small gram negative coccobacilli 2) Fever of unknown origin, joint pain 3) Species related to animal spp exposure: B. abortus = raw cow milk B. melitensis = raw goat milk, feta cheese B. suis = pigs B. canis = dogs |
|
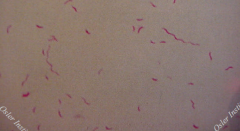
Campylobacter |
Small curved bacilli - like sea gull wings C. jejuni: undercooked poultry ingestion requires selective media containing antibiotics = Skirrow's blood agar significant % Guillain barre syndrome as sequelae -Grows as 37 & 42 degrees celsius C. fetus - blood culture pathogen in immune suppressed host -Grows at 37 & 25 degrees celsius, not at 42
|
|
|
Capnocytophaga |
1) Fusiform shaped gram negative rods - very pleomorphic 2) Oxidase - 3) Catalase - 4) Gliding motility, fingerlike projections from colonies
C. canimorsus - dog bites & bacteremia Other species in the human mouth cause bacteremia in cancer pts on chemotherapy |
|
|
Francisella tularensis |
1) Small gram negative coccobacilli 2) Reservoir - rabbits, rodents 3) Culture media must have cysteine (like legionella) |
|
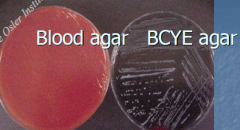
Legionella |
1) Requires cysteine for growth (like francisella tularensis) 2) Media of choice BCYE (buffered charcoal yeast extract) 3) Does not gram stain in direct specimens, use silver impregnation stains in tissue 4) L. pneumophila - urine antigen test 5) Tx: erythromycin |
|
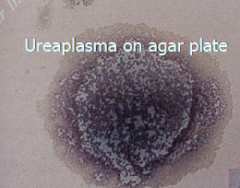
Bacteria without cells walls: 1) Mycoplasma 2) Ureaplasma
-Have cell membrane only -Transport media must contain sterols |
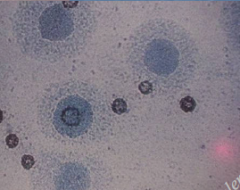
M. hominis - fried egg colony; causes vaginitis, cervicitis, postpartum sepsis, neonatal infections, PPROM U. urealyticum - rapid urea hydrolysis in broth; causes upper genital tract infections, SAB, neonatal infections |
|
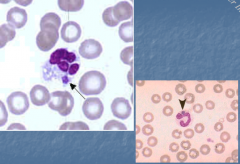
Ehrlichia |
1) Intracellular pathogen, tick-borne 2) Fever, leukopenia, thrombocytopenia, high serum aminotransferases, no rash (unlike RMSF) 3) E. chaffeensis - human monocytes 4) Ehrlichia spp. - human granulocytes 5) Found in midwest 6) PCR & serology for diagnosis |
|
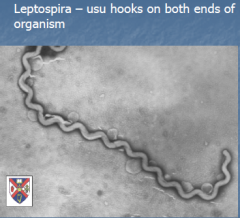
Spirochetes |
1) Borrelia burgdorferi - Lyme's disease -Tick vector (Ixodes) 2) Borrelia recurrentis - relapsing fever -Human body louse 3) Leptospira interrogans - Leptospirosis -Rats & other animals; water association 4) Treponema pallidum - syphilis -RPR, VDRL
Can't culture any of these, need to use serology or molecular |
|
|
Anaerobic Bacteria |
1) Bacteriodes fragilis group 2) Fusobacterium 3) Clostridium species 4) Actinomyces 5) Propionibacterium |
|
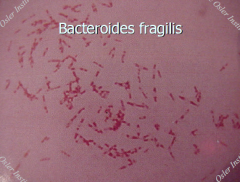
Bacteriodes fragilis group |
1) Grow in presence of bile 2) Esculin + 3) Pleomorphic gram negative bacilli 4) B. fragilis, B. ovatus, B. thetaiotamicron (indole positive), B. uniformis, B. vulgatus |
|

Fusobacterium |
1) Fusiform gram negative bacilli 2) Spindle-shaped with POINTED ends 3) Associated with mouth & respiratory tract abscess 4) F. necrophorum is the type of species |
|

Clostridium |
1) Gram positive bacilli (box car shaped) 2) Spore forming
3) C. perfringens: -double zone of beta hemolysis -reverse camp test +
4) C. botulinum: -food borne toxin ingestion in adults -spore ingestion in small children -causes flaccid paralysis
|
|
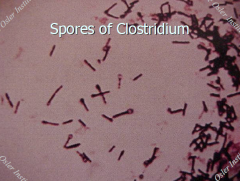
Clostridium continued... |
5) C. tetani: -looks like tennis racket (spore at end) -penetrating skin injury
6) C. septicum: -organism in blood associated with cancer
7) C. difficile: -enterotoxin A; cytotoxin B -NAP1 strain bad |
|
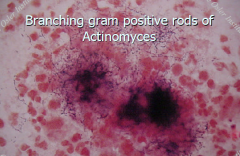
Actinomyces |
1) Branching, gram positive bacilli 2) Capable of forming sulfur granules in tissue 3) Found on normal tonsils
4) A. israelii: associated with oral, thoracic, and abdominal infections -IUD infections -Bread crumb colonies in broth, molar tooth colon on agar plates |
|
|
Propionibacterium acnes |
1) Pleomorphic gram positive rod 2) Can be pathogen in cerebral shunt infections 3) Can cause shunt nephritis
|

