![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
213 Cards in this Set
- Front
- Back
|
Functions of blood |
1.distribution of O2 nutrients metabolic waste and hormones 2. Regulation Body temp oh adequate fluid volume 3. Protection Blood loss Infection thro antibodies wbc proteins |
|
|
Blood composition |
55% plasma 45% formed elements |
|
|
Protein in blood |
Albumin 54 Globulins 38 Fibrinogen 7 |
|
|
Adjusts blood |
Kidney lungs liver |
|
|
Granulocyte |
Neutrophils Eosinophil Basophil |
|
|
Agranulocyte |
Lymphocyte Monocytes |
|
|
Wbc in order of abundance |
Neutrophils Lymphocytes Monocytes Eosinophil Basophil |
|
|
Which is complete rbc or wbc |
Wbc are complete Rbc have no nuclei organelles or mitochondria |
|
|
Hematocrit |
Percent of blood volume that is red blood cells Hydration changes in production and disease affect hematocrit |
|
|
Hemoglobin structure |
2 alpha and 2 beta chain. Carry 4 o2 iron in heme. |
|
|
OxyHemoglobin |
O2 to lungs Bright red |
|
|
Deoxyhemoglobin |
O2 unloading tissue Dark red |
|
|
Carbinohemoglobin |
Co2 load tissue Purplish dark |
|
|
Hematopoiesis |
Blood cell formation Red bone marrow of skeleton Liver spleen; thymus for fetus |
|
|
Hemocytoblasts or hematopoietic stem cells |
Gives rise to all formed elements Becomes any cell Chosen by protein or growth factor |
|
|
Growth factors that determine hemocytoblasts succession |
Erythropoietin Thrombopoietin Leukopoietin |
|
|
Tissue hypoxia |
Not enough o2 in blood |
|
|
Erthropoiesis |
Formation of red blood cells |
|
|
Pernicious anemia |
Anemia from lack of intrinsic factor so you can't absorb b12 |
|
|
Erythropoietin |
Stimulus for erytrhopoiesis From kidney in response to hypoxia (Kidney is responsible for fluid lvls and blood lvls |
|
|
Effects of epo |
More rapid maturation of bone marrow cells Increased circulating reticulocyte count in 1 or 2 days |
|
|
How rbc is destroyed |
Heme and globin are separated Heme is degraded to bilirubin and globin is metabolized into amino acid |
|
|
Anemia |
Low o2 carrying capacity Sign not disease Symptoms are tired sob pale light headed chills and easily bruised |
|
|
Hemolytic anemia |
Blood cells breaking apart |
|
|
Aplastic anemia |
Can be caused by meds Destruction of bone marrow |
|
|
Causes of anemia |
1. Insufficient erythrocytes 2. Low hemoglobin contact 3.abnormal hemoglobim |
|
|
Thalassemias |
Absent of faulty globin chain Rbc thin and delicate and deficient in hemoglobin Mostly meditarian |
|
|
Sickle cell anemia |
Defect In gene code for abnormal hemoglobin Sickle called in low o2 situations Fragile clump and block small blood vessels Common subsaharan African descent |
|
|
Polycythemia |
Excess of rbc Results from bone marrow cancer |
|
|
Leukocytes move |
Move in amoid motion Leave capillaries via diapedeis and move thro tissue spaces by amoid motion |
|
|
Granulocyte characteristics |
Cytoplasmic granulyte Lobed nuclei Phagocytic Shorter lived then rbc |
|
|
Neutrophils |
Most numerous Polymorphonuclie leukocytes Multilobed nucleus Very phagocytic "bacteria slayer" |
|
|
Eosinophil |
Red staining bilobed nuclei Digest parasitic worms that are too phagosize |
|
|
Basophil |
Rarest Histamine dilated allergic reactions Large purplish black granules contain histamine acts of vasodilation attracts other wbcs to infected sites Are last cells when out of blood stream |
|
|
Agranulocytes characteristics |
Large dark purple circular nuclei with thin rim of blue cytoplasm Smooth Mostly lymphoid tissue 2 types T cells act against virus infected cells and tumors B cells give via to plasma cells antibodies |
|
|
Monocyte |
Largest leukocyte kidney beans nuclei Leave circulation enter tissue and turns into macrophages Very phagocytic |
|
|
Leokopoiesis |
Produce and Stimulated by chemical messengers from bone marrow and mature wbcs Interleukin Colony stimulating factors |
|
|
Leukocytes come from |
Bone marrow Hemocytoblasts |
|
|
Leukopenia |
Abnormally low wbc count |
|
|
Leukemia |
Overproduction of wbc Cancerous Lots of immature wbc |
|
|
Platelets from |
Small fragments of megakaryocyte |
|
|
Thrombopoietin |
Growth factor for thrombocyte |
|
|
Thrombocytpoesis |
Platelets production from red bone marrow. Megakaryoblasts undergo endimitosis to make huge cell to break off. It is largest cell in body |
|
|
Hemostasis |
Fast series of reactions for stoppage of bleeding 1. Vascular spasm which is vasoconstriction 2. Platelets plug formation 3. Coagulation |
|
|
Vascular spasm |
Vasoconstriction of damaged blood cell triggered by direct injury Chemicals released by endothelial cells and platelets Pain reflexes |
|
|
Platelets plug formation |
Positive feedback cycle At site of blood vessel injury platelets Stick to exposed collagen fibers (von willebrand factor) Sweel become spiked and sticky and release chemical messengers Adp causes more platelets to stick and release their contents Serotonin is a neurotransmitter for constriction Thromboxane a2 glues platelets together |
|
|
Regulation of platelet phase |
Aggregation limited to injury since normal endothial cells secrete prostacyclin to inhibit aggregation. Also has circulation enzyme that break down adp |
|
|
Coagulation |
Set of reactions in which blood is transformed from liquid to gel Reinforces the platelet plug sith fibrin threads |
|
|
Remember about coagulation |
Factor x complexes with ca2 pf3 and factor v Form prothrombin activator |
|
|
Phase 1 coagulation |
2 pathways to prothrombin activator. Each pathway cascades toward factor x. Factor x complexes with calcium pf3 and factor v to form prothrombin activator. The intrinsic pathway is triggered by negatively charged surfaces and uses factors present within blood The extrinsic pathway is triggered by exposure to tissue tf or factor 3 |
|
|
Phase 2 coagulation |
Prothrombin catalyzed into thrombin |
|
|
Phase 3 coagulation |
Thrombin which converts soluble fibrinogen into fibrin. Fibrin strands form structural basis of clot and causes plasma to become gel like. Thrombin activates factor xiii which crosslinks fibrin and strengthens and stabilizes the clot |
|
|
Clot retraction |
Actin and myosin in platelets contract Platelets pull on fibrin strands squeezing serum from clot |
|
|
Clot repair |
Pdgf(platelet derived growth factor) division of smooth muscle cells and fibroblasts Vascular endothelial growth factor that endothelial cells to multipy |
|
|
Fibrinolysis |
Begins with 2 days Plasminogens converts to plasmin by tissue plasminogens activator factor x11 and thrombin Plasmin digest fibrin |
|
|
Factors limiting clot growth or formation |
2 mechanisms Swift remove and dilution of clotting formation Inhibition of Activates clotting factor |
|
|
Inhibition of clotting factors |
Most thrombin is bound to fibrin threads and prevented from acting elsewhere Antithrimbin 3 protein c and heparin inactivated thrombin and procogulate. Heparin another anticoagulant also inhibit thrombin activity |
|
|
Thromboembolytic disorders |
Undesirable clot formation |
|
|
Bleeding disorders |
Abnormalities that prevent normal clot formation |
|
|
Thrombus |
Clot that develops and persists In an unbroken blood vessel |
|
|
Embolus |
A thrombus freely floating in the blood stream |
|
|
Cerebral emboli |
Can cause stroke |
|
|
Pulmonary emboli |
Impair the ability of the body to obtain oxygen |
|
|
Embolus is prevented by |
Aspirin Heparin Warfarin |
|
|
Thrombocytopenia |
Deficient number of circulating platelets Due to suppression or destruction of bone marrow |
|
|
Impaired liver function |
Inability to synthesize coagulants |
|
|
Hemophilias |
Heredity bleeding disorders Hemophilia a most common type deficiency of factor v11 Hemophilia b deficiency of factor ix Hemophilia c mild type deficiency of factor x1 |
|
|
Blood typing |
Serum containing anti a or anti b agglutinins is added to blood Aggkutination will occur bw the agglutinins and the corresponding agglutinins Positive aggtination |
|
|
Type ab |
Agglutinogen a and b with both serum. So anti a and anti b will clump |
|
|
Type a |
Agglutinogen a Agglutinates with anti a |
|
|
Type b |
Contains agglutinogen b Agglutinates with anti b |
|
|
Type o |
Contains no agglutinogen Does not clump |
|
|
Layers of heart wall |
1. Epicardium thin transparent 2. Myocardium spiral bundled of cardiac muscle cells 3. Endocardium continuous with endothial lining of blood vessels |
|
|
Coronary sulcus |
Atriioventricular groove Encircled the junction of atria and ventricles a |
|
|
Right vs left |
Left cuz it pumps to the left. Oxygenated Body pumps right deoxygenated |
|
|
Semiluner valve |
Prevents backflow into ventricles when ventricles relax |
|
|
Blood return |
1.Blood returns fills right atria, forcing atriioventricular valves to open 2. Right ventricles fill atriioventricular valves are open. 3. Atria contract forcing remaining blood in ventricule. Av valves open ventricles contract atrioventricular valve close while papillary muscle contract and chordae tindineae tighten. 4. Av valves close ventricles contract blood is pushed up semilunar valve forcing them open. 5. Semilunar valves close. Blood flows back from artery closing semilunar valve |
|
|
Pathway of blood. |
Right atrium to tricuspid valve to right ventricle Right ventricles to pulmonary semilunar valve to pulmonary trunk to pulmonary arteries to lungs Lungs to pulmonary veins to left atrium Left atrium to bicuspid valve yo left ventricle Left ventricle to aortic semilunar valve to aorta to system circulation |
|
|
Pulmonary circuit side of heart |
Right side carry blood to and from lungs Short low pressured circulation |
|
|
Systemic circuit side of heart |
Carry blood to and from body tissue Left side of heart Much resistance and long pathway |
|
|
Coronary circulation |
Blood supply to heart itself |
|
|
Angina pectoris |
Thoracic pain caused by deficiency in blood delivered to the myocardium Cells are weakened by lack of o2 |
|
|
Myocardial infarction |
Heart attack Prolonged coronary blockage Non contractions scar tissue |
|
|
Cardiac muscle |
Striated short fat branched and interconnected connective tissue Numerous large mitochondrian Intercalated discs are junctions between cells anchor cardiac cells Have desmosomes and gap functions |
|
|
Cardiac muscle contraction |
Depolarization of the heart is rhythmic and spontaneous |
|
|
Defective sa node |
Ectopic focus: abnormal pacemaker takes over If av node takes over there will be a slower rhythm |
|
|
Defective av node |
Partial or total heart block Few or no impulse from sa node reach ventricles |
|
|
Defects in the intrinsic conduction system |
1. Arrhythmias 2. Uncoordinated atrial and ventricular contraction 3. Fibrillation |
|
|
Extrinsic innervation of heart |
Heartbeat is modified by automatic nervous system Cardiac center in medulla oblongata sets pace and excited heart with sympathetic neurons. Sa and av nodes heart muscle coronary arteries Cardioinhibitory center inhibit sa and av nlde |
|
|
Baroreceptors |
Moniter blood pressure |
|
|
Chemoreceptors |
Moniter blood chemistry |
|
|
Proprioceptors |
Moniter movement |
|
|
Electrocardiogram |
Composite of all action potentials generated at any given time |
|
|
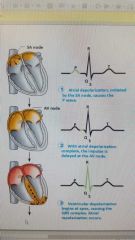
P wave |
Depolarization of sa node |
|
|
Qrs complex |
Ventricular depolarization |
|
|
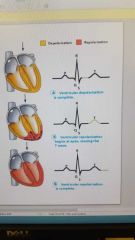
T wave |
Ventricular repolarization |
|
|
Electrocardiogram cycle |
P wave - atrial depolarization P- q interval - time it takes for atrial kick to fill ventricles Qrs wave- ventricular depolarization and atrial repolarization S t segment - time it takes to empty the ventricles before they repolarize t wave |
|
|
Junctional rhythm |
The sa node is nonfunctional p saves are absent and heart is paced by the av node at 40 to 60 beats a minute |
|
|
2nd degree heart block |
Some p saves are not conducted thro the av node hence more p then qrs waves are seen. |
|
|
Ventricular fibrillation |
These chaotic gross irregular ecg deflections are seen in acute heart attack or electric shock |
|
|
Cardiac cycle |
All events associated with blood flow thro the heart during one complete heartbeat |
|
|
Systole |
Contraction |
|
|
Diastolw |
Relaxation |
|
|
First phase of cardiac cycle |
Ventricular filling. Av valves open. Ventricular filling Atrial contraction |
|
|
2nd phase of cardiac cycle ventricular systole |
Isovolumetric contraction phase Ventricular ejection phase Atria relax Ventricles contract |
|
|
3rd phase of cardiac cycle. Isovolumetric relaxation |
Ventricules relax Close sl valves Early diastole |
|
|
Cardio out put is heart rate times stroke volume |
Ye |
|
|
At rest |
Heart rate 75 beats per min 70ml per beat |
|
|
Cardiac reserve |
Difference between resting and maximal cardiac output |
|
|
3 main factors that affect stroke volume |
Preload Contractility Afterload |
|
|
Preload |
Degree of stretch of cardiac muscles before they contract |
|
|
Contractility |
Contraction strength at given muscle length independent of muscle stretch and end diastolic volume |
|
|
Positive inotropics in contractility |
Increase contractility Calcium influx due to sympathetic stimulation Hormones |
|
|
Negative Intopic agents in contratility |
Decrease contractility Acidosis Calcium channel blocker |
|
|
Afterload |
Pressure that must be overcome for ventricles to eject blood Hypertension increases afterload |
|
|
Positive chronotropic factors blank heart rate |
Increase |
|
|
Negative chronic factors blank heart rate |
Decrease |
|
|
Chemical regulation of heart rate |
1. Hormones 2. Maintain intra- and extracellular ion [calcium and potassium] |
|
|
Hormones that affect heart rate |
Epinephrine from Adrenal mea increase heart rate and contractility Thyroxine from thyroid gland increase heart rate and enhances the effects of nonephinephrine and ephinephrine |
|
|
Tachycardia |
Abnormally fast heart rate |
|
|
Bradycardia |
Heart rate slower then 60 |
|
|
Intrinsic cardiac conduction system |
A network of non contractile cells Initiate and distribute impulses to coordinate the depolarization and contraction of the heart |
|
|
Autorhythmic cells |
Unstable resting potentials (pacemaker potential) due to open slow na+ channels |
|
|
Sequence of excitation |
1. Sinoatrial sa node(pacemaker) 2. Atrioventricular av node 3.atrioventricular av bundle 4. Right and left bundle branches 5. Purkinje fibers |
|
|
Sequence of excitation 1. Sa node |
1. Right atrial wall 2. Sets heart pace |
|
|
Sequence of excitation 2. Av node |
Interatrial septum Smaller diameter fibers few gap junctions Delays impulses approximately .1 sec so the atria can complete contraction before ventricles begin |
|
|
Sequence of excitation 3. Atrioventricular av bundle |
Interventricular septum Only electrical connection between atria and ventricles |
|
|
Sequence of excitation 4. Right and left bundle branches |
2 pathways in the interventricular septum Carry impulses toward apex of heart |
|
|
Sequence of excitation 5. Purkinje fibers |
Complete pathway into apex and ventricular walls |
|
|
Sequence of excitation within the heart |
1. Sa node generates impulse 2. Impulse pauses .1 sec at av node 3. Av bundle connects atria to the ventricle 4. Bundle branches conduct the impulse thro the ventricular septum 5. Purkinje fibers depolarize the contractile cells of both ventricles |
|
|
3 layers in vein |
Tunica intima Tunica media Tunica externa |
|
|
Elastic arteries |
Ex aorta Large thick walled arteries Large lumen No vasoconstriction |
|
|
Muscular arteries |
Distal to elastic arteries Deliver blood to organs Active in vasoconstriction |
|
|
Pericyte |
Stabilize their walls and controls permeability |
|
|
Capillaries everywhere except |
Cartilage Epithelial Cornea and lens of eye |
|
|
Continuous capillaries |
Abundant in skin and muscles Right junctions and intracellular clefts In brain it completes blood brain barrier |
|
|
Fenestrated capillaries |
Some endothelial cells contain fwnestrations More permeable to continuous capillaries Function in absorption if filtrate formation in lines intestines and endocrine glands |
|
|
Sinusoid caoillaries |
Fewer tight junctions usually fenestrated Large lumen Blood flow sluggish large molecules and blood cells pass thro Found in liver bone marrow and spleen |
|
|
Types of vessels |
Vascular shunt True capillaries |
|
|
Veins vs arteries |
Veins habe large likes and are full of venous valves and venous sinuses Artery has more of a tunica media so smaller lumen |
|
|
Vascular anastomoses |
Interconnection of blood vessels |
|
|
Blood flow |
Volume of blood flowing thro cess organ or entire circulation in a given period |
|
|
Blood pressure |
Force per unit area exerted on wall of blood vessel by blood |
|
|
Resistance |
Opposition to flow Measure of amount of friction blood encounters with vessel walls |
|
|
3 important sources of resistance |
Blood viscosity Total blood vessel length Blood vessel diameter |
|
|
If blood pressure increases then blood flow |
Speeds up |
|
|
If resistance increases the blood flow |
Decreases |
|
|
Systolic pressure |
Pressure exerted in aorta during ventricular contraction |
|
|
Diastolic pressure |
Lowest lvl of aortic pressure |
|
|
Map (mean arterial pressure) |
Pressure that propels blood to tissue Is diastolic pressure plus 1/3 pulse pressure |
|
|
Venous pressure |
Changes lil during cardiac cycle Low pressure due to cumulative effects of peripheral resistance |
|
|
Factors aiding venous return |
1. Muscular pump 2. Respiratory pump 3. Venoconstriction |
|
|
Main factors influencing blood pressure |
Cardiac output Peripheral resistance Blood volume |
|
|
Baroreceptors locations |
Moniter pressure in Carotid sinuses Aortic arch Walls of larger arteries of neck and thoracic |
|
|
Increased pressure baroreceptors |
Increased input to vadomotor Inhibits vadomotor and cardioaccelerarory centers which caused arterial dilatationand venodilation Stimulates cardioinhibitory center Decrease blood pressure |
|
|
Chemoreceptors reflexes |
Detect increase of co2 or drop in ph or o2 Are in aortic arch and larger arteries of neck |
|
|
Atrial natriuretic peptide anp |
Antagonize aldosterone(reclaims salts) Gets rid of salts Lowers tonicityby lowering osmosis Lowers h2o retention Lowers blood volume Lowers blood pressure |
|
|
Kidneys regulate atrial blood pressure by |
Renal regulation 1. Direct renal mechanism (independent of hormones) 2. Indirect renal mechanism (renin-angiotension-aldosterone) |
|
|
Functions of angiotensin 2 |
Increased blood volume by 1stimulating aldosterone secretion (retain salts) 2causes adh release (retention of water) 3triggers hypothalamic thirst center Causes vasoconstriction directly increasing blood pressure |
|
|
Secondary hypertension |
Due to identifiable disorder Obstructed renal arteries Kidney disease Endocrine disorders |
|
|
Orthostatic hypotension |
Temporary low bp and dizziness when standing |
|
|
Chronic hypotension |
Hint of poor nutrition and warning signs for Addison disease or hypothyroidism |
|
|
Acute hypotension |
Important sign of circulatory shock |
|
|
Autoregulation |
Controlled intrinsically by modifying diameter of local arteries feeding capillaries Organs regulate own blood flow 2 types 1 metabolic controls 2 myogenic controls |
|
|
Metabolic controls |
Vasodilation of arteries Relaxation of precapillary sphincters Occur if decline in tissue o2 or inflammatory chemicals or substances from metaboliccaly active tissues (h+, k+, adenosine, and prostaglandins) |
|
|
Myogenic controls |
Keep tissue perfusion constant Passive stretch promotes increased tone and vasoconstriction Reduced stretch promotes venodilation and increases blood flow to tissue
|
|
|
Angiogensis |
Enlarging of existing blood vessels or creating new ones |
|
|
Hypovolemic shock |
Low blood volume due to blood loss |
|
|
Vascular shock |
Inadequate blood flow from changes in extreme dilation Ex anaphylactic shock |
|
|
Cardiogenic shock |
Inadequate blood flow from heart |
|
|
Give rise to all Stem cells |
Hemocytoblasts |
|
|
Tunica media |
Smooth muscle and elastin Sympathetic vadomotor nerve fibers Vasoconstriction and vasodilation |
|
|
Tunica externa |
Collagen fibers Contains nerve fibers lymphatic vessels |
|
|
Venous veins |
Most common in limbs |
|
|
Venous sinuses |
Flattened veins with extremely thin walls |
|
|
If blood pressure increase then blood flow |
Decreases |
|
|
Main factors influencing blood pressure |

|
|
|
Short term neural and hormonal controls affect blood pressure by |
Altering peripheral resistance and cardiac output |
|
|
Long term renal regulation controls blood pressure by |
Altering blood volume |
|
|
Neural controls maintain map by altering |
Vessel diameter so if low blood volume all vessels constricted except those to heart and brain |
|
|
Baroreceptors reflexes decrease in blood pressure due to |
Arterioler venodilation Venodilation Decreased cardiac output |
|
|
If map is low then |
Reflex vasoconstriction Increased co Increased blood pressure |
|
|
Hypothalamus influence |
Increases blood pressure during stress Mediated redistribution of blood flow during exercise Modify material pressure via relays to medulla |
|
|
What 2 structures in the brain modify arterial pressure via relays to medulla? |
Hypothalamus and cerebral cortex |
|
|
What hormones causes increased blood pressure |
Epinephrine and notepinephrine from adrenal gland increase it by increased co and vasoconstriction Angiotension 2 and high adh levels increase it by vasoconstriction |
|
|
What hormones causes lower blood pressure |
Anp(atrial natriuretic peptide caused decreased blood volume by antagonizing aldosterone Reduced blood volume and vasodilation |
|
|
Direct renal mechanism |
Alters blood volume independently from hormones Increased bp or blood volume causes elimination of urine to bring bp down Decreased bp of blood volume causes kidneys go conserve water so bp rises |
|
|
Indirect mechanism (renin-angiotrnsion-aldosterone mechanism) |
Low arterial blood pressure causes release of renin Renin catalyzed conversion of angiotensinogen from liver to angiotensin 1 Angiotensin converting enzyme converts angiotensin 1 to angiotensin 2 |
|
|
Hypertension |
High blood pressure 140 or 90 or higher |
|
|
Prolonged hypertension major cause of |
Heart failure Vascular disease Renal failure Stroke |
|
|
Hypotension |
Low blood pressure |
|
|
Tissue perfusion involved in |
Delivery of o2 and nutrients Removal of wastes Gas exchange Absorption if nutrients Urine formation |
|
|
Metabolic controls effects |
Relaxation of vascular smooth muscle Release of NO(powerful vasodilator) by endothelial cells |
|
|
Endothelins |
Released from endothelium are potent vasoconstrictors |
|
|
Active or exercise hyoeremia |
Blood flow increases in proportion to metabolic activity Local control override sympathetic vasoconstriction |
|
|
Lipid soluble molecules travel how in capillary exchange |
Diffuse directly thro endothelial membranes |
|
|
Water soluble solutes pass thro capillaries by |
Clefts and fenestrations |
|
|
Larger molecules like proteins are exchanged in capillaries by |
Actively transported |
|
|
Circulatory shock |
Blood vessels are inadequately filled Blood cannot circulate normally Results in inadequate blood flow to meet tissue needs |
|
|
Atrioventricular valves |
Prevent backflow into atria when ventricles contract |
|
|
Intercalated discs |
Junctions between cells anchor cardiac cells Desmosomes Gap junctions |
|
|
Cardiac muscle contraction |

|
|

|

|
|
|
Intrinsic cardiac conduction system |
A network of noncontractile (autorhythmic) cells Initiate and distribute impulses to coordinate the depolarization and contraction of the heart |
|
|
Sa node |
Right atrial wall Sets heart pace Depolarize the fastest Generates impulses about 75 times a minute |
|
|
Av node |
Interatrial septum Fewer gap junctions Delays impulses approximately 0.1 second |
|
|
|
|
|
Heart sounds |
The first sound is the av valves closing which begins the systole The 2nd sound is the sl valves close |
|
|
Ventricular filling |
Av valves open 80 percent of blood passively flows into ventricles |
|
|
End diastolic volume edv |
Volume of blood in each ventricle at the end of ventricular diastole |
|
|
Notepinephrine causes the pacemaker to |
Fire more rapidly Also increases contractility |
|
|
Acetylcholine hyperpolarizes pacemaker cells by |
Opening k+ channels |
|
|
Atrial (Bainbridge) reflex |
A sympathetic reflex initiated by increased venous return Stretch of atrial walls stimulates sa node and activates sympathetic reflexes |

