![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
85 Cards in this Set
- Front
- Back
|
Effusion classifications
-(general contents) |
-Pure transudate (low protein, low TNCC)
-Modified transudate -Exudate, Septic (high protein, high TNCC, bacteria) -Exudate, nonseptic (high protein, high TNCC, no bacteria) |
|
|
Pleural & Peritoneal fluid formation in health
-formed by -returned how |
-formed by processes involving Starling's Law
-returned to blood via lymphatic vessels |
|
|
Animals with enough pleural and peritoneal fluid in health to collect a sample
|
-horses
-cattle |
|
|
Pleural & Peritoneal fluid composition in health
|
Plasma constituents (most)
-H2O -Electrolytes -"Other" solutes (glucose, urea, creatinine) Proteins -low [albumin] -small proteins |
|
|
Refractive index
-depends on |
-# of particles/volume
-type of particles |
|
|
Refractive index
-used to measure |
-[TP]
-SGref |
|
|
Refractive index of urine
-mostly determined by |
-electrolytes
-urea -creatinine |
|
|
Refractive index of plasma
-mostly determined by |
-electrolytes
-proteins |
|
|
Effusion
-define |
-accumulation of fluid in a body space or cavity
-rate of fluid formation >> rate of fluid removal |
|
|
Ascites
-define |
-accumulated fluid in a serous cavity (peritoneal)
-transudate, exudate, or "other" type |
|
|
Transudation
-define |
-passage of fluid or solute through a membrane due to changes in hydraulic or oncotic pressure gradients
|
|
|
Transudate
-define |
-effusion produced by changes in mechanical factors
|
|
|
Hydrostatic pressure
-define |
-energy/pressure of a fluid at rest
-pressure due to gravity |
|
|
Hydraulic pressure
-define |
-energy/pressure of a fluid in motion
-pressure due to pump (heart) |
|
|
Exudation
-define |
-the act of oozing out through pores
|
|
|
Exudate
-define |
-an effusion produced by increasing permeability to plasma proteins because of inflammation
|
|
|
Hemorrhage
-define |
-the escape of loss of blood from blood vessels/heart
|
|
|
Lymphorrhage
-define |
-the escape or loss of lymph from lymph vessels
|
|
|
Starlings law
|
Net filtration = LpS [chg. hydraulic pressure - chg. oncotic pressure]
Net filtration = LpS [(Pcap - Pif) - s(Picap - Piif)] |
|
|
Capillaries
-normally permeable to -not permeable to |
Permeable to:
-water -electrolytes -small solutes (urea, glucose water) Not Permeable to: -most protein (excpet for in the liver and lungs) -blood cells |
|
|
Osmolality
-define |
-total solute concentration
|
|
|
2 major factors causing inc. fluid movement into extravascular space
|
-inc. hydraulic pressure
-dec. oncotic pressure gradient |
|
|
Dec. change in oncotic pressure
-due to |
-inc. in oncotic pressure of interstitial fluid from capillary permeability to proteins
-large dec. in plasma [TP] resulting in large dec. of capillary oncotic pressure with slight decrease in interstitial oncotic pressure |
|
|
Reasons for a "safe zone" resulting in no fluid accumulation
|
-dec. [TP]plasma & dec. [TP]if --> no change in oncotic pressure
-inc. lymphatic drainage |
|
|
Pathogeneses of cavitary effusions
|
-transudation
-exudation -hemorrhage -lymphorrhage -rupture of hollow organ -mixed |
|
|
Transudate
-causes of formation |
-inc. vascular hydraulic pressure --> congestion
-dec. plasma oncotic pressure ---> hypoproteinemia -both can't be due to hypoalbunemia by itself |
|
|
Composition of transudates depends on
|
-permeability of capillaries to proteins
|
|
|
Protein poor transudate
-form where -contents |
Most tissue
-H2O -electrolytes -glucose -urea -... |
|
|
Protein rich transudates
-form where -contents |
Liver
-same as protein poor transudate but with plasma proteins too |
|
|
Protein Poor Transudate
-causes |
-hepatic cirrhosis
-protein-losing nephropathy -non-cirrhotic portal hypertension |
|
|
Protein Poor Transudate
-what causes water to accumulate in cavities? |
-inc. blood hydraulic pressure (Na+ & H2O retention)
-dec. plasma oncotic pressure (dec. [TP] & dec. [albumin] |
|
|
Protein Poor Transudate
-what causes cells to accumulate in the effusion? |
-they don't
|
|
|
Protein Poor Transudate
-what causes plasma proteins to enter effusion? |
-they don't
|
|
|
Protein Rich Transudate
-causes |
Congestive heart failure
-Right side -- >hepatic congestion --> hepatic sinuses permeable to protein -Left side --> pulmonary congestion --> pulmonary capillaries slightly permeable to protein |
|
|
Transudate formation due to liver congestion where
-protein poor -protein rich |
Poor:
-Presinusoidal: portal vein -Sinusoidal: early in sinus Rich -Post-sinusoidal: central vein congestion, hepatic vein congestion |
|
|
Protein rich transudate
-what causes the water to accumulate in cavities? |
-inc. hydraulic pressure
|
|
|
Protein rich transudate
-what causes the cells to accumulate in the effusion? |
-?????
-inflammation???? |
|
|
Protein rich transudate
-what causes the plasma proteins to enter the effusion? |
-inc. hydraulic pressure in vessels permeable to plasma proteins
|
|
|
Exudate formation
-causes |
-inc. vascular permeability to protein --> lower oncotic pressure gradient to bring fluid back in
|
|
|
Exudate
-fluid composition |
-similar to plasma w/ concurrent migration of inflammatory cells
|
|
|
Exudate
-types |
-infectious (septic)
-noninfectious (nonseptic) |
|
|
Septic exudate
-causes |
-Bacteria
-Viral -Fungal -Protozoan -Parasitic |
|
|
Nonseptic exudate
-causes |
-Neoplasia, foreign body, necrotic tissue (spleen, pancrease)
-urine & bile |
|
|
Exudate
-what causes water to accumulate in cavities? |
-dec. oncotic pressure gradient from proteins leaking into interstitial fluid
-possible slight due to inc. in blood hydraulic pressure |
|
|
Exudate
-what causes the cells to accumulate in the effusion? |
-chemokines cause migration of cells to fluid (neuts, monocytes, others)
|
|
|
Exudates
-what causes the plasma proteins to enter the effusion? |
-cytokines inc. vascular permeability to plasma proteins
|
|
|
Hemorrhagic effusions
-cause |
-blood vessel damage
|
|
|
Hemorrhagic effusion
-composition |
Initial:
-same as peripheral blood Later: -RBC resorption -altered oncotic pressure gradient |
|
|
Acute hemorrhagic effusion vs. Chronic hemorrhagic effusion
|
Acute
-mimics peripheral blood Chronic -fewer RBCs -mild inflammation -erythrophages, siderophages |
|
|
Hemorrhagic Effusion
-causes of blood vessel damage |
-trauma to blood vessels
-neoplasia -hemostasis defects (warfarin) |
|
|
Hemorrhagic effusion
-what causes the water to accumulate in cavities? |
-H2O in blood
-possibly slightly due to dec. in oncotic pressure |
|
|
Hemorrhagic effusion
-what causes the cells to accumulate in the effusion? |
-cells in blood
-secondary inflammation |
|
|
Hemorrhagic effusion
-what causes the plasma proteins to enter the effusion? |
-plasma proteins in blood
|
|
|
Lymphatic effusion
-due to |
-Lymphorrhage (vessel damage/trauma)
-Impaired lymph drainage |
|
|
Lymphatic effusion
-composition of fluid |
Thoracic duct (chylothorax):
-lymphocytes -chylomicrons Afferent vessels -lymphocyte poor Efferent vessels -lymphocyte rich |
|
|
Chylous effusions
-due to |
leakage of lymph containing chylomicrons
-throacic duct damage (cardiac disease in Cats) |
|
|
Nonchylous effusions
-due to |
lymphatic obstruction
-lymphangiectasia -LN disease |
|
|
Lymphorrhagic effusions
-what causes the water to accumulate in cavities? |
-H2O in lymph
-possibly slightly due to dec. oncotic pressure gradient |
|
|
Lymphorrhagic effusions
-what causes the cells to accumulate in the effusion? |
-lymphocyte-rich lymph
-secondary inflammation |
|
|
Lymphorrhagic effusions
-what causes the proteins to enter the effusion? |
-proteins in lymph (lipids--> inc. TP)
-secondary inflammation --> permeability |
|
|
Fluids (w/ composition) that accumulate due to the rupture of hollow organs
|
-urine (composition + inflammatory change)
-bile (composition + inflammatory change) -ingesta + inflammatory change |
|
|
Uroperitoneum
-causes |
-urinary bladder rupture
-damage to ureters or urethra |
|
|
Bile leakage
-causes |
-obstructed bile ducts
-neoplasia of bile ducts -trauma to bile ducts |
|
|
Leakage of gastric or intestinal contents
-causes |
-de-vitalized tissues (vascular lesion)
-trauma (functure, FB) -neoplasia |
|
|
Neoplasia causing effusion from multiple processes
|
-necrosis --> inflammation --> exudate
-damaged vessels --> hemorrhage -block lymphatic vessels --> lymphorrhage |
|
|
Heart failure causing effusion from multiple processes
|
-protein-rich transudate --> inflammation --> exudate
|
|
|
Ruptured urinary bladder causing effusion from multiple processes
|
-uroperitoneum --> exudate
|
|
|
Effusion Tube to use for collection for possible culturing
|
-red top
|
|
|
Something to be aware of when collecting effusion sample in a tube for evaluation
|
-some tubes contain additive that falsely increase [TP]
|
|
|
Effusion tube to use to prevent fibrin clot formation
|
-Purple top --> EDTA
|
|
|
Effusion PCV
-measure when |
-if collected effusion is pink to red
|
|
|
Effusion PCV
-interpretation |
-compared to blood Hct
-indication of the amount of blood in the effusion |
|
|
Effusion PCV
-considerations |
-blood is resorbed
-bloody effusion diluted due to fluid shifts |
|
|
Effusion PCV
-post centrifugation supernantant color --colorless = --red = |
-colorless = fresh blood
-red = hemolyzed blood |
|
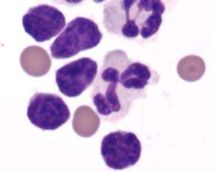
Identify
|
-small lymphocytes
|
|
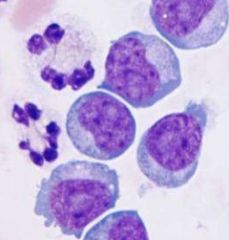
Identify
|
-medium reactive lymphocytes
|
|
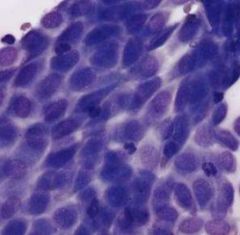
Identify
|
-mesothelial cells, sheet
|
|
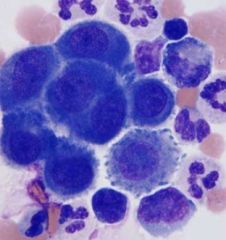
Identify
|
-mesothelial cells, reactive
|
|
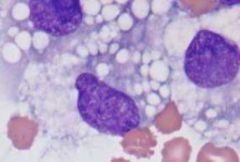
Identify
|
-macrophages
|
|
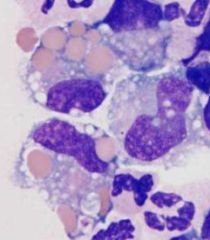
Identify
|
-erythrophages
|
|
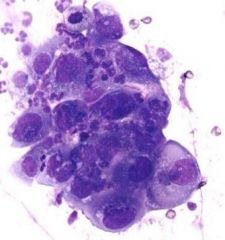
Identify
|
-carcinoma cells (epithelial)
|
|
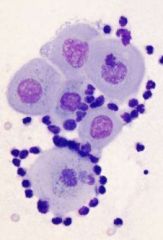
Identify
|
-squamous cells (epithelial)
|
|
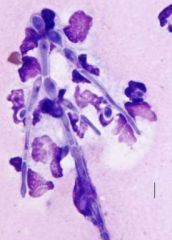
Identify
|
-fungi
|
|
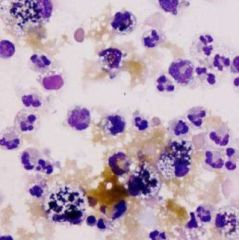
Identify
|
-bile pigment
|
|
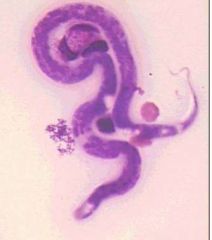
Identify
|
-microfilaria
|

