![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
83 Cards in this Set
- Front
- Back
|
What is erythropoiesis?
|
The process of red blood cell formation
|
|
|
Generally, what is the balance between creation and destruction of RBCs? What's the turnover rate?
|
Equivalent
1% |
|
|
What's the main stimulus for erythropoiesis?
|
O2 deficiency
|
|
|
What's the sensor in oxygen deficiency that causes erythropoiesis?
|
The kidney
|
|
|
What system removes old RBCs from the circulation?
|
Reticluendotheilial system
|
|
|
What is hemolysis?
|
Accelerated destruction and/or clearance of RBCs
|
|
|
What are the secondary effects of hemolysis?
|
Decreased O2 delivery to tissues--> hypoxia --> erythropoietin --> increased RBC production by marrow
|
|
|
What's typically released from RBCs during hemolysis?
|
Hgb
LDH |
|
|
What protein does free Hgb bind to in the serum?
|
Haptoglobin
|
|
|
What is the breakdown product of hemoglobin?
|
Iron + unconjugated bilirubin
|
|
|
What are the laboratory findings during hemolysis?
|
Elevated serum free Hgb
High serum LDH Low serum haptoglobin High unconjugated bilirubin High reticulocyte count |
|
|
What are some of the ways that bilirubin is excreted?
|
Fecally: urobilinogen
Urine: urobilinogen |
|
|
What is the pathway that bilirubin takes to be excreted?
|
1. Breakdown in blood
2. Unconjugated bilirubin (or bilirubin conjugated to Z protein,glucuronic acid) transported toliver 3. Enters biliary system 4. In small intestine broken down by a bacterial protease 5. 90% excreted inFECES If lots and lots of bilirubin, you can have excretion in the kidney |
|
|
What is the definition of compensating hemolysis?
|
Hemolysis without anemia/mild decrease in Hg
Accelerated destruction is matched by increased production |
|
|
How much of the RBC volume can the marrow compensate for?
|
10%
|
|
|
What is the definition of a hemolytic anemia?
|
The destruction of RBC >> production
|
|
|
What are the different types of congenital anemias?
|
Sickle cell
Thalassemia Spherocytosis G6PD deficiency |
|
|
What are some of the different types of acquired hemolytic anemias?
|
Autoimmune hemolysis
MAHA Drug induced |
|
|
What are some of the differences that you'll find between an intravascular hemolytic anemia and extravascular?
|
Intravascular: hemoglobinemia, hemoglobinuria, consumption of the haptoglobin
|
|
|
What are some of the intrinsic causes of hemolytic anemias?
|
RBC membranes
RBC cytoplasmic enzymes Abnormal Hgb |
|
|
What are some of the extrinsic factors that can cause hemolytic anemias?
|
Acquired coditions
Oxidation Immune-mediated Mechanical destruction |
|
|
What are some labs that you should order up to determine the etiology of a hemolysis?
|
Blood smear
Hgb electrophoresis RBC fragility test RBC enzyme level assay Specific mutation studies Coomb's test |
|
|
What congenital hemolytic anemias show abnormalities in hemoglobin? What's the test for this?
|
Thalassemias
Sickle cell disease Test: Hgb electrophoresis |
|
|
What congenital hemolytic anemias show abnormalities in the RBC membrane? What's the test for this?
|
Hereditary spherocytosis
Hereditary elliptocytosis Test: osmotic fragility test |
|
|
What congenital hemolytic anemias show abnormalities in RBC enzymes? What's the test for this?
|
G6PD deficiency
Pyruvate kinase deficiency Test: enzyme levels |
|
|
Where are the thalassemias typically found?
|
Where malaria is endemic
Possibly protective |
|
|
What are the different kinds of hemoglobin chains found?
|
Alpha
Beta Gamma Delta |
|
|
What are the types of hemoglobin that are normally found in adults?
|
Hg A: Alpha2, Beta2 (96-98%)
Hg A2: Alpha2, Delta2 (2-3%) Hg F: Alpha2, Gamma2 (0-1%) |
|
|
How many copies of each of the Hgb genes does each person have?
|
Beta chain: 2 copies
Alpha chain: 4 copies |
|
|
What are the different kinds of thalassmias?
|
Beta
Alpha |
|
|
What types of mutations typically cause the thalassmias?
|
Point mutations
|
|
|
What does a peripheral blood smear look like for a thalassemia?
|
Hypochromia
Microcytosis Also, you can have hemolysis |
|
|
Who typically gets beta thalassmias?
|
Mediterannean people
Africans |
|
|
What type of a mutation happens in Beta thalassemias?
|
Mutation; not a deletion
|
|
|
What are the different subtypes of beta thalassemias?
|
2 phenotypes:
Thalassemia beta minor (trait): heterozygous Thalassemia beta intermediate: homozygous mutated; not as severe Thalassemia beta major: homozygous mutated; very severe |
|
|
What are the symptoms of thalassema beta major?
|
Severe anemia
Multi-organ failure at a young age |
|
|
What population does not show the effects of a beta thalassemia?
|
Fetus/infants:
Switching to the beta chain causes the symptoms to come out. |
|
|
What are the findings on Hg electrophoresis in beta thalassemias?
|
HgA is decreased
HgA2 is mildly increased HgF is mildly increased |
|
|
What are the typical numbers for Hg in a person who is normal, trait, and major?
|
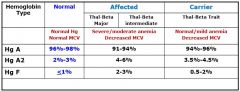
|
|
|
What are the subtypes of alpha thalassemia?
|
Silent carrier: "-a/aa"
Thal-alpha trait: "-a/-a" OR "--/aa" Hg H disease: "--/-a" Hydrops fetalis: "--/--" |
|
|
What are the findings in thal-alpha trait?
|
"-a/-a" OR "--/aa"
Mild decrease of alpha chain production No "new" Hg Mild anemia/low-normal Hg Marked microcytosis (decreased MCV) |
|
|
What are the findings in HgH disease?
|
"--/-a"
Severereduction in alpha chain production Hg (4 beta chains); decreased O2affinity Mild-severe hemolytic anemia Hg Bart's (4 gamma chains) in infants; severe disease |
|
|
What are the findings in hydrops fetalis?
|
"--/--"
Absence of alpha Intrauterine hypoxia Hg bart's: 4 gammas Not compatible with life |
|
|
What's the pattern of hemoglobin amounts in the alpha thalassemias?
|
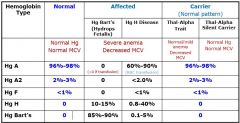
|
|
|
What are the typical lab findings in someone with a thalassemia?
|
Microcytosis +/- anemia
Hemolysis Hg electrophoresis findings Positive FH Molecular genetics confirm |
|
|
What are the findings of thalassemias on peripheral blood smears?
|
Microcytosis
Hypochromia Target cells Heinz bodies |
|
|
What's the treatment for thalassemias?
|
Chronic transfusions
Folic acid supplementation BOne marrow treatment |
|
|
What complications result from chronically transfusing people?
|
Iron overload!
-Multiorgan failure -CHF, liver cirrhosis Treatment: Iron chelators |
|
|
What are some of the iron chelators used in this disease?
|
Defroxamine
Deferasirox They're used for the beta thalassemias |
|
|
What population is most commonly affected by sickle cell syndrome?
|
African american population
|
|
|
What mutation takes place in sickle cell anemia?
|
V->E (valine-->glutamic acid) at 6th position of the beta globin gene
|
|
|
What is the effect of the sickle cell mutation?
|
Less soluble hemoglobin leads to precipitation of the Hgb-->sickling of the cells
|
|
|
What is the effect of sickling on RBCs?
|
Shorter lifespan
Infarction all over the body |
|
|
What is the typical presentation of someone with sickle cell trait?
|
It's asymptomatic.
|
|
|
What is hemoglobin C?
|
Similar disease to sickle cell, except that it's an E for K (glutamic acid for lysine) substitution at position 6
|
|
|
What are thesymptoms of hemoglobincarriers?
|
Anemia
Ulcers Splenomegaly |
|
|
What are the different sickle cell diseases?
|
Hg SS: homozygous S
Hg SC: heterozygous S, heterozygous C Hg S/B. thal disease: heterozygous S+B0/homozygous B+ |
|
|
When do people present with sickle cell disease?
|
As infants, when the Hgb F declines to less than 50%
|
|
|
What are some types of sickle cell crises?
|
Pain/vaso-occlusive crisis
Visceral sequestration crisis Aplastic anemia Hyperhemolytic crisis |
|
|
What are some other kinds of problems that sickling blood cells can cause?
|
Recurrent infections
Pulmonary HTN Renal failure |
|
|
What are some infections that sickle cell people are more prone to?
|
Parvovirus B19
Encapsulated bacteria: (strep, h. flu, meningococcus) |
|
|
What are some of the vaso-occlusive crises that can happen with sickle cell disease?
|
When there's vasoocclusion due to the sickling of blood cells inside the vasculature; normally pain
-Bones -Spleen -Stroke -Skin ulceration |
|
|
What is the management for sickle cell pain crises?
|
Pain meds
Correcting the precipitating factors: (dehydration,infection, etc.) |
|
|
What is the treatment of people with sickle cell in relation to their increased number of infections?
|
Prophylactic penicillin until 18
Immunizations |
|
|
What is the treatment ofr an acute chest syndrome in a person with sickle cell disease?
|
Blood exchange
|
|
|
What's the treatment for sickle cell disease?
|
Hydroxyurea: increases HbF; decreased HgS
Exchange transfusion (acute management) Pain management Blood transfusions |
|
|
What are some of the reasons that people with sickle cell don't comply with meds?
|
The side effects are quite severe.
|
|
|
What is the cause of hereditary spherocytosis?
|
Defect in vertical interactions:
-Spectrin -Protein 3 -Protein 4.2 Defect in Spectrin-Protein 4.2 binding |
|
|
What is the cause of hereditary elliptocytosis?
|
Defects in horizontal interactions:
-Protein 4.1 -Protein 3 -Glycoprotein C, D Defects in spectrin/spectrin-ankyrin binding |
|
|
Who gets hereditary elliptocytosis more commonly?
|
Africans/mediterraneans
|
|
|
What problems happen in people with HS/HE?
|
The RBCs get stuck in the spleen and then get destroyed
|
|
|
What tests do you order up to diagnose hereditary elliptocytosis or spherocytosis?
|
Negative Coomb's test
Abnormal osmotic fragility test Family history |
|
|
What's the inheritance of Hereditary spherocytosis, elliptocytosis?
|
Autosomal dominant
|
|
|
What are the clinical findings of HS/HE?
|
Anemia
Jaundice Chronic hemolysis Severe: -Splenomegaly -Gallstones |
|
|
What are the treatments for HS/HE?
|
If asymptomatic, don'ttreat
Folic acid supplementation Splenectomy (delay as long as possible.) |
|
|
What are some of the immunizations that people with HS/HE should get? What meds should they be on?
|
Immunizations:
-H. influenza -Meningococcus -P. pneumoniae Penicillin prophylaxis |
|
|
What are the two most significant enzyme defects in RBCs?
|
G6PD
Pyruvate kinase deficiency |
|
|
What's the inheritance of G6PD?
|
X-linked
Multiple mutations |
|
|
What different variants of G6PD exist?
|
African-American
Mediteranean Southeast asian |
|
|
What is the function of G6PD?
|
Maintain glutathione levels
Prevent free radical damage |
|
|
What's the cause of RBC damage in people with pyruvate kinase deficiency?
|
Decreased ATP-->rigid red cells-->hemolysis
|
|
|
What's the inheritance of pyruvate kinase deficiency?
|
Autosomal recessive
|
|
|
What are the symptoms of pyruvate kinase deficiency?
|
Hemolysis
Splenomegaly Neonatal jaundice |

