![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
26 Cards in this Set
- Front
- Back
|
What does an ECG show?
|
- Action potentials of the cardiomyocytes
- Electrical events manifest as electrocardiographic events |
|
|
What are the components of a basic 3 lead system and what is their placement and what is its purpose?
|
-3 bipolar electrodes placed on RA, LA, LL.
- Leads sense and record electricity |
|
|
What is color placement and charge of Lead II?
Why is it preferred and what does it identify? |
"White (-) on the right and smoke (ground) over fire (+)"
- Displays a waveform that has +P waves and +QRS complexes - Used to identify arterial arrhythmia |
|
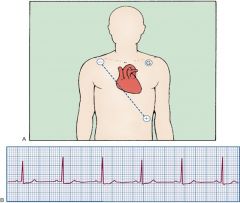
|
Basic Placement and NSR in lead II
|
|
|
What is a 12-lead EKG and its components?
|
- has 10 electrodes that create 12 different leads
|
|
|
What are the 3 augmented vector leads?
What are they used to indicate? Why are they referred to as "augmented"? |
-aVR, aVL, aVF
- Used to indicate MI or Infarction - Augmented because the way they are placed causes the leads to come out tiny and the machine must augment them to get what we need |
|
|
What are Precordial Leads (277)?
|
- V1-V6
|
|
|
How do you know which leads are important to monitor?
|
- Important to choose a lead that tailors to the patients needs
|
|
|
What are the 4 ways to count the rate of a strip?
|
1. Count the QRS complex and multiply by the amount of seconds
2. Start with the QRS on a big box and count down by 300, 150, 100, 75, 60 3. Count number of big boxes between R-R and divide by 300 4. Count the number of small boxes between R-R and divide by 1500. |
|
|
How do you find out the rhythm of an EKG?
|
Regular only if the R-R is the same throughout the strip.
|
|
|
What determines NSR?
|
A ratio 1:1 ratio of P wave to QRS complex.
|
|
|
What does a wide QRS complex mean?
What does a normal QRS complex mean? |
-The ventricle is taking longer to contract because its not getting the normal signal from the SA node.
- QRS complex is getting the proper signal from the SA node. |
|
|
What is a normal QTc?
How is it calculated? |
A corrected QT interval
Normal QTc < 0.48 QTc = QT/ square root of R-R |
|
|
What is the time of a normal:
P wave P-R Interval QRS complex QT Interval T Wave U Wave Q Wave |
P wave: <0.12 sec
P-R Interval: 0.12-0.20 sec QRS complex: 0.06-0.10 sec QT Interval: < 1/2 (R-R Interval) T Wave (3x Pwave) U Wave: indicates that the pt had an MI Q Wave |
|
|
What comes first ST elevation or ST depression?
What does ST elevation mean? What does ST depression mean? |
ST depression occurs first
>1 mm indicates injury >1mm indicates ischemia |
|
|
What are the 3 changes in an EKG related to an MI?
|
1. Inverted T wave
2. ST-segment > 1mm 3. Pathological Q wave (deeps much below the isoelectric line) |
|
|
What are the bpm from the:
sinus: SA node- Junc: AV node/bundle of His- Vent: Ventricular rate- |
Sinus: SA node- 60-100 bmp
Junc: AV node/bundle of His- 40-60 bpm Vent: Ventricular rate- 20-40 bpm |
|
|
What is NSR?
|
Impulses originate at the SA node at normal rate 60-100 with normal P waves and QRS complexes.
|
|
|
What is the action for Sinus Bradycardia?
What drug are given? What are the possible causes? |
Oxygen, notify
|
|
|
How do you calculate the MAP?
What MAP is needed to purfuse the organs? |
SBP + 2(DBP)/3 = MAP
>60 mmHg |
|
|
What are the indications for temporary pacing?
|
1. Bradydysrhythmias
A. Sinus Bradycardia and Arrest B. Sick Sinus syndrome C. Heart blocks 2. Tachydysrhythmias A. SVT B. V tach 3. Permanent pacemaker failure 4. Support of cardiac output after cardiac surgery 5. Diagnostic studies A. Electrophysiology studies (EPS) B. Atrial electrograms (AEG) |
|
|
What are the 4 routes of temporary pacing?
|
1. Transcutaneous: Pacing by depolarizing the heart through the chest with skin electrodes
2. Transthoracic: Pacing wire is inserted emergently by threading it through a transthorac needle into the RV 3. Epicardial: Electrodes are sewn to the epicardium during cardiac surgery 4. Transvenous (endocardial): Electrode is advanced through a vein into the RA or RV or both |
|
|
What are the 3 types of pacemakers?
|
1. Fixed rate (asynchronous): pacing at a fixed rate regardless of the occurrence of spontaneous myocardial depolerization; non sensing modes
2. Demand (synchronous): Pacing only when the heart's intrinsic pacemaker fails to function at a predetermined rate; pacing is stimulated by intrinsic activity 3. Atrioventricular sequential (dual-chamber): pacing to both atrium and ventricle in sequence |
|
|
What is the 3 letter generic code for pacing and what does it stand for?
|
I: Chambers paced: A, V, D, 0
II: Chambers sensed: A, V, D, 0 III: Response to sensing: 0, T, I, D IIIa: none, triggered, inhibited, dual (T + I) |
|
|
What are the goals in medical management of a pacemaker?
|
- Establishing and maintaining CO
1. Determine pacing route based on situation 2. Determine lead placement, pacing rate, and mode 3. Evaluate patient's response to pacing |
|
|
What are the 4 roles in nursing management of a pacemaker?
|
1. Assessment and prevention of pacemaker malfunction
2. Protect from microshock 3. Surveillance for complications 4. Patient and family education |

