![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
36 Cards in this Set
- Front
- Back
|
What causes iron deficiency anemia? |
- Inadequate levels of iron for synthesis of various proteins such as hemoglobin and myoglobin
- Also inadequate for use as a cofactor for enzymatic reactions |
|
|
What are the iron sources?
|
Heme Iron
- Red meat - Shellfish and fish Non-heme iron - Enriched cereals - Beans - Tofu - Seeds - Potatoes - Green vegetables - Dried fruits |
|
|
How much iron is absorbed in the diet? Where?
|
- 1 mg
- Duodenum |
|
|
How is heme iron absorbed?
|
Heme iron is taken up by the heme transporter
|
|
|
What is required for non-heme iron absorption?
|
Vitamin C is required in diet for efficient uptake of dietary non-heme iron
|
|
|
What happens to dietary iron before it can be taken up into the epithelial cells of the duodenum?
|
Duodenal cytochrome B - a ferrireductase - on epithelial cell membrane reduces Fe3+ (ferric) to Fe2+ (ferrous) through a Vitamin C dependent mechanism
|
|
|
What happens after ferric iron (Fe3+) is converted to ferrous iron (Fe2+) in the duodenum?
|
Fe2+ is transported into intestinal epithelial cells by DMT1 (divalent metal ion transporter 1)
|
|
|
What can happen to Fe2+ after being taken up by DMT1 in duodenum?
|
- Directly transported across basal lateral membrane into portal vein by Ferroportin 1
OR - Stored until needed in the cells by Ferritin present in the cells |
|
|
How is Fe2+ oxidized back to Fe3+?
|
Hephaestin on basal lateral epithelial cell membrane
|
|
|
What happens after Fe3+ is made again by hephaestin?
|
- Fe3+ is transported out of epithelial cell by Ferriportin
- Next, it binds to Transferrin and is distributed to the rest of the body - All cells that take up Fe3+ use the Transferrin Receptor for uptake through endocytosis |
|
|
What molecule does Fe3+ bind in the plasma for transport through the rest of the body?
|
Transferrin
|
|
|
What peptide regulates the release of iron from the duodenal epithelial cells? Where is it synthesized?
|
- Hepcidin
- Synthesized by liver |
|
|
What influences the levels of Hepcidin?
|
When iron levels in the liver increase, Hepcidin is released and binds to Ferroportin inducing endocytosis and degradation of Ferroportin (preventing additional release of iron into the plasma)
|
|
|
Where is iron stored?
|
- Liver takes up iron and stores it inside the hollow ball structure of the protein Ferritin
- 1 ferritin can contain ~5000 Fe(OH)3 molecules - Iron can also be stored in Hemosiderin granules made up of partially degraded ferritin-iron complexes |
|
|
What happens to Hemosiderin under normal iron conditions? Excess iron?
|
- Normal conditions, very little iron is found in Hemosiderin granules
- Iron overload conditions, excess iron is mainly stored in this form |
|
|
What happens to iron in degrading RBCs?
|
- Most of it is recycled
- Macrophages recycle iron back to bone marrow for synthesis of new RBCs |
|
|
What are the ways to lose iron? How much?
|
- Normally through shedding of intestinal and skin cells (~1 mg/day)
- During menstrual cycle, women lose ~0.5 mg iron / day - During pregnancy, women lose 500-1000 mg of iron - Abnormal bleeding (variable loss) |
|
|
What are the locations of iron?
|
- Hemoglobin (~60% or ~2500 mg)
- Myoglobin (~8%) - Ferritin in liver (~25%) - Remaining is bound to Transferrin or enzymes (eg, cytochromes, catalase, and aconitase) |
|
|
What causes Megaloblastic Anemia?
|
- Inability to synthesize adequate amounts of purines and thymidylate triphosphate for DNA synthesis
- Deficiency of folate, Vitamin B12, or a methionine synthase leads to impaired DNA synthesis |
|
|
How is synthesis of purines and thymidylate triphosphate implicated in the basis of Megaloblastic Anemia?
|
- Synthesis of these molecules involves 1C units attached to folate derivative Tetrahydrofolate
- Deficiency of folate, Vitamin B12, or a methionine synthase |
|
|
How is folate converted to the form which can donate 1C units for DNA synthesis?
|
- Folate is converted to THF by sequential reduction reactions by Dihydrofolate Reductase
- Folate → Dihydrofolate → Tetrahydrofolate |
|
|
How is folate critical to the synthesis of Thymidylate Triphosphate?
|
- Methylene-THF donates a 1C group to dUMP → dTMP using enzyme Thymidylate Synthetase
- THF reductase is oxidized to dihydrofolate, which must be reduced by DHF reductase to form THF |
|
|
What drug inhibits purine and thymidylate synthesis? Implications?
|
Methyltrexate - causes drug induced Megaloblastic Anemia
|
|
|
What are the sources of a 1C unit for the folate and S-adenosylmethionine pathways?
|
- Serine is the major source
- Histidine, glycine, and formate can also contribute 1C units |
|
|
How is folate critical to the synthesis of Purines?
|
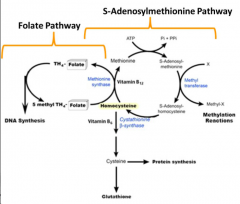
De novo synthesis of purines (Adenine and Guanine) depends upon donation of two 1C units in the form of formate from formyl-tetrahydrofolate
|
|
|
Why is Vitamin B12 critical for the synthesis of purines and dTMP?
|
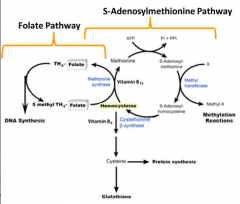
- Synthesis of methionine requires methyl-THF (from folate pathway) and Vitamin B12 as cofactor
- Without Vitamin B12 methyl-THF is not utilized, methionine synthesis is inhibited, and THF is not regenerated - Leads to megaloblastic anemia |
|
|
How is Methionine synthesized?
|
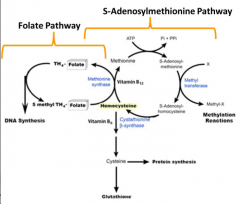
- Methionine Synthase - transfers a methyl group for methyl-THF to vitamin B12 which acts as a co-enzyme
- Methyl group is then transferred to Homocysteine forming Methionine - Methionine Synthase is the only known enzyme to use Methyl-THF as a substrate and thus the only way to regenerate THF |
|
|
What are the implications of deficient Vitamin B12?
|
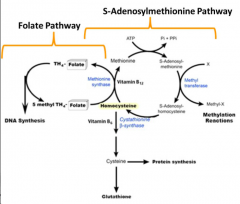
- Methyl-THF is not utilized
- Methionine synthesis is inhibited - THF is not regenerated |
|
|
What is the necessity of Methionine?
|
Formation of S-adenosylmethionine required for methylation of DNA, RNA, and for synthesis of creatinine, melatonin, and epinephrine
|
|
|
What are the sources of folate in the diet?
|
- Most vegetables (especially dark leafy greens)
- Fruits - Grains - Nuts - Beans - Dairy products - Seafood and meats Since 1998: cereals, flour, rice, and their products are fortified w/ folate |
|
|
What happens to dietary folate (folic acid) once ingested?
|
- Converted from polyglutamic folate to monoglutamic folate in intestine by Folate Hydrolase
- Folate is released into blood in complex w/ Folate Binding Protein as either monoglutamate folate or monoglutamate THF |
|
|
What are the sources of Vitamin B12 in the diet?
|
- Meat
- Shellfish - Milk - Eggs (not at significant levels in vegetables and fruits) |
|
|
How do vegans obtain folate and Vitamin B12 in their diet?
|
Folate through food:
- Most vegetables (especially dark leafy greens) - Fruits - Grains - Nuts - Beans - Dairy products Vitamin B12 often needs to be supplemented because it is not found in significant levels in fruits and vegetables) |
|
|
What happens to dietary Vitamin B12 once ingested?
|
- Vitamin B12 is bound to proteins in diet and released in stomach at acid pH
- Absorbed in process involving salivary Haptocorrin (R-protein), Intrinsic Factor, and Cubulin |
|
|
What can cause a Vitamin B12 deficiency?
|
- Low intake of vitamin
- More often d/t impaired absorption or transport of vitamin (eg, Pernicious Anemia) |
|
|
What happens in Pernicious Anemia?
|
- Lack of intrinsic factor
- Leads to vitamin B12 deficiency |

