![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
133 Cards in this Set
- Front
- Back
|
What are the 3 layers of skin?
|
1) Epidermis
2) Dermis 3) Subcutaneous tissue |
|
|
What are two things contained the epidermis? What function do they serve?
|
Keratin= provides waterproofing
Melanin= provides color to skin |
|
|
What type of glands are contained in the dermis layer of skin? What functions do they lend?
|
Sebaceous glands= contributes oil to skin
Sweat glands= contributes sweat to skin |
|
|
The ___________ layer supports the ____________ layer.
|
dermis, epidermis
|
|
|
What insulates the subcutaneous layer?
|
fatty cells
|
|
|
What is the largest organ in the body?
|
Skin
|
|
|
A skin assessment also includes:
|
hair and nails
|
|
|
T/F You can assess skin while performing other parts of the health assessment?
|
True. While checking pulses, edema, or chit chatting with patient you can assess for lesions and their locations, the condition and characteristics of the skin, and for ulcers.
|
|
|
What are 9 characteristics of skin?
|
1) is it intact 2) color or discoloration
3) moist/dry 4) temperature 5) ecchymosis 6) oiliness/dryness 7) edema 8) elasticity/tenting 9) nutrition of patient |
|
|
What are 5 functions of skin?
|
1) Protection 2) Thermoregulator 3) Secretions 4) Sensation 5) Provides vitamin D 6) Electrolyte regulator
|
|
|
What's thermoregulation balance?
|
Heat production = heat loss
|
|
|
As muscle activity goes up (exercise); ___________ _______ goes up.
|
Generated heat
|
|
|
Why is thyroxine output important?
|
Because increased thyroxine levels lead to increased cell metabolism. This is called Chemical Thermal Genesis
|
|
|
What's the normal body temperature?
|
36-38 degrees Celsius.
96.8- 100.4 degrees Fahrenheit |
|
|
How is the sympathetic nervous stimulated?
What happens? |
Norepinephrine and epinephrine
Cellular metabolism is increased. |
|
|
A fever results in 2 things?
|
Increased cellular metabolism and increased body temperature
|
|
|
What occurs with decreased BMR?
|
Decreased heat production
|
|
|
Shivering leads to what?
|
Increased heat production
|
|
|
Shivering increases _______ ___________ by ____ times
|
heat production; 45
|
|
|
What are the 4 types of heat loss?
|
1) Radiation
2) Conduction 3) Convection 4) Evaporation |
|
|
What is radiation?
What is it affected by? |
Transfer of heat from one surface to another without direct contact
body surface area--the greater the surface area, the greater the heat loss |
|
|
heat loss in fetal position is _________
heat loss in the standing position |
less than
|
|
|
T/F heat loss and heat production can occur simultaneously?
|
True
|
|
|
Vasoconstriction leads to ________ heat loss
|
decreased
|
|
|
Vasodilation leads to __________ heat loss
|
increased
|
|
|
What is conduction?
|
Heat transfers through direct contact
|
|
|
What is convection?
Example? |
Transfer of heat by way of air current
A fan blowing air around; Cuisinart convection oven. |
|
|
What is evaporation?
Example? |
Loss of heat via fluid evaporation
Sweating or water vapor in exhalation. |
|
|
Who is most at risk for deficient thermoregulation?
Why? |
Infants and the elderly (>75 yr)
Decreased fat tissue, skin wasting, decreased nutritional diet intake, decreased activity, decreased thermoregulating efficiency. |
|
|
As level of exercise increases, the body temperature __________?
|
Increases
|
|
|
Who is most affected by hormones? When is this group most affected?
What hormone is it linked specifically to? |
Females.
During ovulation and after menopause. "Hot flashes" teperature swing and sweats for 10-15 minutes. Progesterone |
|
|
How does stress affect temperature?
Why does it affect temperature? |
Stress increases body temperature because stress stimulates the sympathetic nervous system.
|
|
|
How does environment affect body temperature?
|
The warmer the climate; the warmer the patient's body temperature.
|
|
|
How does Circadian Rhythm impact body temperature?
How long might it take for a 3rd shift to adjust to 3rd shift? |
The highest temps. are from 8 pm to 12 am. The lowest are from 4 am to 6 am.
Up to a year. |
|
|
What is pyrexia?
|
It's a fever over 38 degrees Celsius 100.4 degrees Fahrenheit.
|
|
|
What is a subnormal temperature?
What is a low grade fever? What is hyperpyrexia? |
temperature below normal
temperature above normal an extremely high temperature over 105.8 degrees Fahrenheit. |
|
|
What are the 4 types of fevers?
|
1) Constant/subtained 2) Intermittent 3) Remittent 4) Relasping
|
|
|
A constant/substained fever is a body temperature that is __________ _______ __________.
|
always above normal
|
|
|
An intermittent fever is a that _______ and _____ _______ __ __________.
|
spikes; then returns to normal
|
|
|
A remittent fever is a fever that ______ _________ __________ __ _________.
|
spikes without returning to normal
|
|
|
A relasping fever _______ ______ _______ __ __ ____________ _________ __ __ __________ _____ __ _______.
|
that spikes and returns to an acceptable temperature in a time over 24 hours.
|
|
|
What are the 5 causes of a fever?
|
1) Inflammatory response 2) Allergies
3) Infection 4)Cerebral/Neurological Injury 5) Drug/Blood reaction |
|
|
Which part of the brain is known as the "body's thermostat?"
|
The hypothalamus
|
|
|
What's the important job of the hypothalamus?
|
It's the body's thermostat. It controls the body's set temperature point.
|
|
|
Where is the hypothalamus located?
|
Between the cerebral hemispheres.
|
|
|
What part of the brain controls heat loss?
What part of the brain controls heat production? |
anterior portion of the hypothalamus= heat loss
posterior portion of the hypothalamus=heat production |
|
|
What happens if the there is a brain stem injury?
|
The body temperature can climb and climb and climb up. Eventually it can "burn itself out" and lead to death.
|
|
|
What are pyrogens?
|
Fever producing bacteria that occur with infections
|
|
|
The hypothalamus will raise the set temperature point when _____________.
|
it is triggered by hormone-like substances
|
|
|
What will the patient experience while experiencing pyrexia?
|
chills
|
|
|
How do WBCs affect body temperature?
|
increases body temp
|
|
|
How do chills affect body temperature?
|
Increases body temperature. The shivering increases muscle activity.
|
|
|
How does the body release heat?
|
Vasodilation, sweating, breathing
|
|
|
The physiological causes of a fever?
|
hypothalamus pyrogens
WBCs chills heat release: through vasodilation, diaphoresis, afebrile |
|
|
Symptoms of a fever?
|
aches headaches
diaphoresis malaise patient is warm to touch patient feels cold delerium tachycardia tachypnea |
|
|
Nursing diagnoses related to thermoregulation?
|
Dehydration r/t.......
Ineffective thermoregulation r/t,,,,,,,,, Hypo-/Hyperthermia r/t........ Risk for imbalanced body temperature r/t........... |
|
|
Nursing interventions for a fever?
|
cooling blanket, ice bags, get cultures then give antibiotics, PRN pyretics, assess mental status, get VS, give oral fluids, change bed linens/clothing, frequent oral care, maintain I/O, patient to be on bedrest
|
|
|
What is Malignant Hyperthermia
|
hereditary condition of uncontrolled heat production occuring when susceptible persons receive anesthetic drugs. It's usually fetal.
|
|
|
Why does malignant hyperthermia happen?
|
The patient has a rxn to anesthetic given during surgery
|
|
|
What happens when a patient experiences malignant hyperthermia during surgery?
|
The surgery stops, a hypothermia blanket is put on them, the patient will wake up and feel the pain from surgery, 20 bottles of meds will need to be opened.
|
|
|
What should a nurse do before a patient goes in for surgery?
|
A nurse should perform a thorough patient hx prior to surgery. Ask if they or any family members have had any problems with anesthesia in the past. A blood test can be done for 8-10K--only 8 institutions perform the test in the US.
|
|
|
What is Dantrolene used for?
|
It is a medication that is used for malignant hyperthermia. It's expensive.
|
|
|
How is the test for malignant hyperthermia perfomed?
|
A biopsy of muscle tissue is needed.
|
|
|
What is succinylcholine used for?
What condition does succinylcholine increase the risk for? |
Paralytic intubation.
Malignant hyperthermia. |
|
|
What is a heat stroke?
|
When a person is exposed to extremely high temperatures for extended periods of time causing the hypothalamus to malfunction.
|
|
|
What precedes a heat stroke.
|
Heat exhaustion.
|
|
|
Who is most at risk for a heat stroke?
|
Infants, the eldery, people suffering from cardiovascular disease, alcoholism, diabetes, or hypothyroidism, strenuously working people (construction, farmers, athletes)
|
|
|
What medications make a person more susceptible to heat strokes?
|
Phenothiazides, antihistamines, anticholinergics (Parkinson's disease), antiemetics (Phenergan), cogentin, diuretics, amphetamines, and beta-adrenergic receptor antagonists
|
|
|
Signs and symptoms of a heat stroke?
|
Flushed skin, not sweating, confusion, visual disturbances, muscle cramps, increased thirst, nausea, delirium, dry hot skin, low BP, high heart rate, temperature as high as 113.
|
|
|
What can a heat stroke lead to?
|
loss of consciousness, fixed pupils, and permanent neurological damage.
|
|
|
How do you treat a heat stroke?
|
Put the patient in a cooler environment, replace fluids and electrolytes. (Want isotonic soln if IV)
|
|
|
What are the signs and symptoms of heat exhaustion
|
profuse diaphoresis which leads to fluid deficits
|
|
|
What are the types of hypothermia?
|
Accidental: examples: fall into a cold body of water, lack of shelter, inadequately dressed.
Induced: example: surgerically induce for cardio. or neuro. surgeries. |
|
|
What is hypothermia?
|
heat loss during a prolonged exposure
|
|
|
What are the signs and symptoms of hypothermia?
|
decreased heart rate, decreased BP, cyanotic, cardiac dysrhythmias, lost level of consciousness, unresponsive to painful stimuli, clinical signs of death.
|
|
|
At ______ degrees F, the body starts to shiver and patient's ___ levels _______ because the ______ are using ____ to ________ _____.
|
95, O2, decrease, muscles, O2, generate heat.
|
|
|
Why do they surgerically induce hypothermia?
|
To reduce the O2 needs of the body.
|
|
|
What causes frostbite?
|
Ice crystals form inside cell d/t exposure to extreme cold. It's a localized freezing of the skin and subcutaneous tissues. It leads to permanent circulation and tissue damage.
|
|
|
What are signs and symptoms of frostbite?
|
Area appears white and waxy, area is firm to touch,and the patient lost sensation to the area.
|
|
|
Which areas are prone to frostbite?
|
earlobes, nose tip, fingers, toes
|
|
|
How do you tx frostbite?
|
gradually warm areas with a warming blanket or layers of clothing, get VS, put frostbitten person next to another person, support cardio. function, raise BP, protect injured tissue, and frequently assess temperature
|
|
|
Fahrenheit to Celsius
|
(F-32) x (5/9)
|
|
|
Celsius to Fahrenheit
|
[(9/5) x C] + 32
|
|
|
How do antipyretic medications affect thermoregulation?
|
They reduce fever by increasing heat loss
|
|
|
Antipyretics include?
|
Acetaminophen (Tylenol)
NSAIDS (salicylates like ASA, ibuprofen, naprosyn), corticosteriods |
|
|
Which medication acts like an antipyretic but is not usually used to treat fevers?
Why isn't it used? |
Corticosteriods
Because it masks signs of infection |
|
|
What are the indications of using an antipyretic?
|
prevent shivering and to prevent using oxygen stores
|
|
|
What is the classification of antipyretics?
|
analgesic and antiinflammatories
|
|
|
What are the indications to use antipyretics for?
|
mild-moderate pain, inflammation, and fever
|
|
|
What are the objectives need to be addressed when a patient has a fever?
|
increase heat loss, decrease heat production, and prevent complications
|
|
|
What are the side effects of antipyetics?
|
GI bleed, nausea, vomiting, dizziness, flushing, drowsiness, epigastric distress, ringing in the ears.
corticosteriods mask s/s of infection. |
|
|
How are antipyretics administered?
What's the usual dose? |
orally and rectally
Depends on the size and age of the individual. |
|
|
Tylenol dose is usually _________?
Give ____ and/or ____ with _____? Why? |
325-600 mg q 4hrs PRN
milk, food, ASA or corticosteriods. In case you are concerned about GI bleed |
|
|
Heat has what effects?
|
It increases: circulation, cell metabolism, and blood flow. It promotes healing, vasodilation, and movement of waste products. It relieves muscle stiffness, and muscle spasms.
|
|
|
Why should heat therapy be ceased after 45 minutes?
|
Because the reflux vasoconstriction response that will ultimately decrease circulation.
|
|
|
What's the result of continuous heat?
|
epithelial cell damage that will lead to tenderness, edness, and blisters
|
|
|
How often should check the site heat is applied to?
|
every 10 minutes
|
|
|
Cold has what effects?
|
Vasonconstriction, diminishes pain and swelling, promotes blood coagulation, decreases cell metabolism, bacterial growth and oxygen needs of cells.
|
|
|
Prolonged exposure to cold therapy leads to?
|
inadequate blood flow and nutrients to tissue. 1st site is reddened, then area has blue-purplish mottlling with numbness and burning pain
|
|
|
Cold should be applied for no longer than?
|
Every hour because of the vasodilation reflux effect
|
|
|
Examples of moist heat are?
|
Warm soaks, warm bath, sitz bath (used for hemorrhoids, whirlpools, dampening the felt pad of a aquathermic pad
|
|
|
Moist heat is good for?
What needs to be checked with moist heat? |
Hemorrhoids, episiotomy. rectal surgery, and vaginal inflammation.
Check water temp and add hot water if water cools. |
|
|
Examples of dry heat are?
|
Water bottles, hot packs, heating pad, hyperthermic blankets
|
|
|
Contraindications of heat therapy?
|
trauma if after 1st 24 hours, extensive blood loss, malignant tumor, erythemia , blisters, abdominal pain
|
|
|
Contraindications of cold therapy?
|
open wounds, hypersensitivity to cold, neuropathy, impaired circulation
|
|
|
Contraindications to both heat and cold?
|
Neurosensitivity, impaired mental status, impaired circulation, open wounds
|
|
|
What condition is an examples of a condition that will impair circulation?
|
PVD. Lack the ability to dissipate heat via circulation. Pt is at risk for tissue damage b/c of poor circulation and blood pooling.
|
|
|
If you suspect a circulatory problem, what should you assess?
|
Capillary refill, color of extremities, compare the color of left side of body to the right side of the body, touch patient's skin and palpate pulses.
|
|
|
Why should heat and cold not be applied to an open wound?
|
Cold= lessens blood flow and inhibits healing
Heat= increases blood flow and could lead to a hemorrhage |
|
|
Guidelines for applying heat or cold include
|
get a baseline, assess the pt for temp. sensitivity, heat/col tol., assess the area, explain th eprocedure, apply a barrier btwn device and skin, reassess q 15 minutes, remove at appropriate time, examine area and document response. Inspect equip. for frayed wires and exposed heating components.
|
|
|
Other cautions to be aware of in heat or cold therapy?
|
Age (young/old)
Renal Insuff./Failure Edema New tissue Abdominal pain Spinal injury |
|
|
Developed neuropathies from renal insufficiencies or failure can?
|
lower tolerance to heat or cold
|
|
|
New tissue is ________________ to heat and cold therapy?
|
More sensitive
|
|
|
You should cautiously apply heat to abdominal pain or oral pain because?
|
Abdominal pain may be sign of appendicitis and heat could cause appendix to rupture. Oral pain may be an abscess and applied heat would could sepsis.
|
|
|
Why do the elderly have less tolerance for heat and cold?
|
Thinner skin layers and wasting. They are more at risk for burns.
|
|
|
Why should you be cautious with heat and cold therapy with a patient with a spinal injury?
|
Because they have altered nerve pathways, decreased sensation, and decreased pain reception.
|
|
|
When you palpate the skin you should assess what?
|
dry/moist, smooth/rough, color of, edema present, intact/nointact, temperature of
|
|
|
Preferred lighting to inspect skin in?
|
Indirect light
|
|
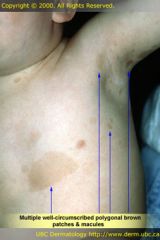
|
macule
|
|
|
What is a papule?
|
A palpable firm solid in skin <1cm
Examples: wart, pimple, |
|
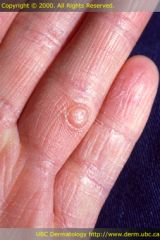
|
Palpule
|
|
|
What's a plaque?
|
A primary skin lesion that's palpable solid in skin that doesn't extend into lower skin layers and is >1cm
|
|
|
What's a nodule?
|
A primary skin lesion that's a solid, hard mass deeper in the dermis and between 0.5 - 2 cm
|
|
|
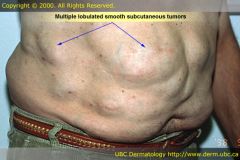
What's a tumor?
|
A primary skin lesion that's a solid, hard mass that extends through the subcutaneous tissue and is >2 cm. It has irregular borders.
|
|
|
What's a cyst?
|
A primary skin lesion that's encapsulated, semi-solid or fluid-filled it can be >1cm
|
|
|
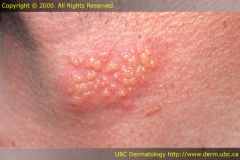
What's a vesicle?
|
Circumscribed round or oval translucent mass that's <0.5 cm. Filled with sebaceous fluid or blood.
example= chicken pox, blisters, cold sores |
|
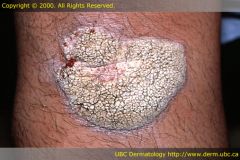
|
Plaque
|
|
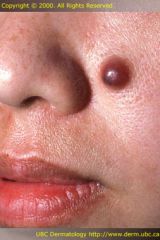
|
Nodule
|
|
|
Tumor
|
|
|
Vesicules
|
|
|
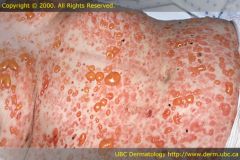
Bulla
|
|
|
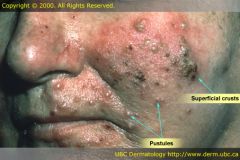
Pustule
|
|
|
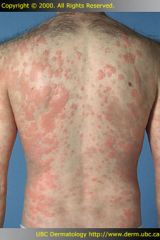
Wheal
|

