![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
22 Cards in this Set
- Front
- Back
|
Oesophagus
|
25 cm long muscular tube from pharynx (C6) to stomach (T11)
|
|
|
Cricopharyngeus muscle
|
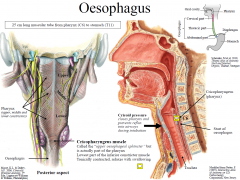
Called the “upper oesophageal sphincter” but is actually part of the pharynx
Lowest part of the inferior constrictor muscle Tonically contracted, relaxes with swallowing |
|
|
Oesphagus Histology
|
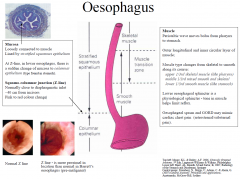
Mucosa
Loosely connected to muscle Lined by stratified squamous epithelium At Z-line, in lower oesophagus, there is a sudden change of mucosa to columnar epithelium (type found in stomach). Squamo-columnar junction (Z-line) Normally close to diaphragmatic inlet ~40 cm from incisors Pink to red colour change |
|
|
Oesphagus Transitions
|
|
|
|
Oesophagus - relationships
|
Anterior relationships: trachea to T4, left main bronchus, pericardium & heart
Posterior relationships: vertebrae in upper 2/3rds, then aorta passes behind oesophagus. |
|
|
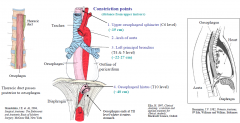
Significance of constriction points
|
foreign bodies tend to lodge; common sites of carcinoma, scarring & strictures after swallowing
|
|
|
Oesophagus - relationships & constrictions
|
|
|
|
Stomach
|
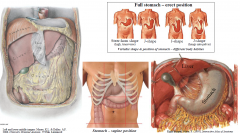
Stomach is expanded part of digestive tract between oesophagus and duodenum
Function: food reservoir & food blender; storage (1.5-3L); chemical & mechanical breakdown of food; chyme (semi-liquid mixture) passes through pyloric orifice to duodenum. In supine position stomach commonly lies in left hypochondrium, epigastrium, umbilical and left flank (see lower middle image) |
|
|
Stomach – external features
|
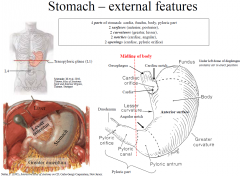
4 parts of stomach: cardia, fundus, body, pyloric part
2 surfaces (anterior, posterior), 2 curvatures (greater, lesser), 2 notches (cardiac, angular), 2 openings (cardiac, pyloric orifice) |
|
|
Stomach – internal features
|

Mucous membrane of empty stomach is thrown into folds called rugae. Rugae flatten as stomach distends.
Muscular wall – 3 layers (rest of GIT has only 2 layers, inner circular & outer longitudinal) Circular layer thickens to form the pyloric sphincter Pyloric stenosis (stenosis due to thickened pyloric sphincter) projectile vomiting |
|
|
Stomach & peritoneal relationships
|
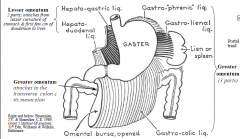
Stomach is intraperitoneal - anterior and posterior surfaces are covered by peritoneum At the greater and lesser curvatures, peritoneum forms the greater and lesser omentum
|
|
|
Lesser omentum
|
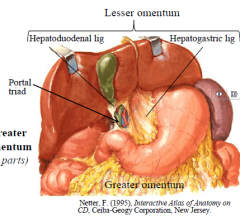
Lesser omentum passes to liver and has two parts: hepatogastric ligament and hepatoduodenal ligament (contains the portal triad)
|
|
|
Greater omentum
|
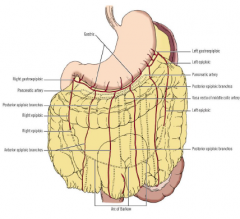
Greater omentum is the gastrophrenic, gastrolienal and gastrocolic ligaments collectively
Gastrocolic part is most often simply called the greater omentum It folds back on itself to form an apron-like structure (4 layers of peritoneum) “Policeman of abdomen” – adheres to & seals off sites of inflammation in peritoneal cavity |
|
|
Stomach Relationships
|
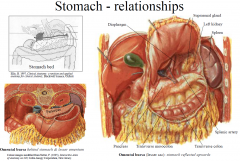
Anterior: liver, diaphragm, anterior abdominal wall
Posterior (“stomach bed”): through the lesser sac it is related to: diaphragm, left suprarenal gland, left kidney, pancreas, splenic artery, transverse colon & transverse mesocolon; and through the greater sac it is related to the spleen. |
|
|
Duodenum (Latin = twelve)
|
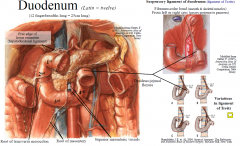
(12 fingerbreadths long = 25cm long)
Duodenum is first part of small intestine, and is the shortest (25cm), widest and most fixed part of small intestine. L1-L3 vertebral levels Function: digestion & absorption; 2nd part of duodenum receives secretions from liver and pancreas (via bile & pancreatic ducts). Relationship to peritoneum: retroperitoneal, except first few cms of superior part, which has omenta attached Root of transverse mesocolon crosses 2nd part, root of the mesentery crosses 3rd & 4th part |
|
|
Duodenum – internal features
|
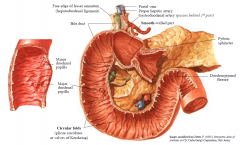
Circular folds in all but first few cms of duodenum, which is called the duodenal cap on radiographs
Bile duct and main pancreatic duct open at major duodenal papilla Accessory pancreatic duct opens at minor duodenal papilla (approx 2 cm above) |
|
|
Arterial supply – stomach & duodenum
|
Remember: Stomach derived from foregut; duodenum is derived from foregut and midgut
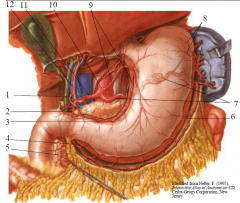
Stomach is supplied by all 3 branches of the coeliac trunk. Lesser curvature by left & right gastric arteries, greater curvature by left & right gastroepiploic (gastro-omental) and fundus by short gastric arteries Duodenum is supplied by branches of coeliac trunk and SMA - the superior and inferior pancreaticoduodenal arteries respectively (each have anterior and posterior branches) |
|
|
1. R. gastric a.
2. Gastroduodenal a. 3. R. gastric a. 4. R. gastroomental (gastroepiploic) a 5. Superior pancreaticoduodenal a. 6. L. gastroomental (gastroepiploic) a 7. Splenic a. 8. Short gastric as. (4-5). 9. L. Gastric a. 10. Coeliac trunk 11. Common hepatic a. 12. Proper hepatic a |
|
|
Neurovascular supply – stomach & duodenum
|
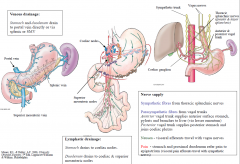
|
|
|
Neurovascular supply – oesophagus
|
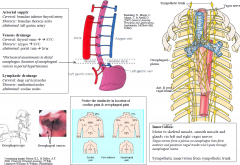
|
|
|
Barium Meal
|
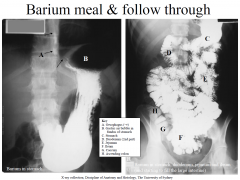
|
|
|
Achalasia
|
(lower oesophageal sphincter fails to relax normally with swallowing)
|

