![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
134 Cards in this Set
- Front
- Back
|
What is a MUCOCELE?
|
common lesion resulting from rupture of a salivary gland duct and spillage of mucin into the surrounding soft tissues
|
|
|
A MUCOCELE is often the result of _______.
|
local trauma
|
|
|
What is the MOST COMMON NON-NEOPLASTIC LESION OF SALIVARY GLANDS?
|
mucocele
|
|
|
What is the most common site of MUCOCELE?
|
Lower lip
|
|
|
What is the clinical presentation of a mucocele?
|
- dome-shaped mucosal swelling
- soft and fluctuant - some may be firm |
|
|
What is the treatment of MUCOCELE?
|
- (chronic lesion) local excision along with adjacent granular tissue feeding into it
- submit for microscopic examination - good prognosis - superficial variants are short lived and heal on their own |
|
|
What is a RANULA?
|
mucocele of the floor of mouth
|
|
|
RANULA usually arises from which gland?
|
sublingual gland
|
|
|
What is the clinical presentation of a RANULA?
|
- blue
- dome shaped - fluctuant swelling |
|
|
What is PLUNGING / CERVICAL RANULA?
|
unusual clinical variant of ranula, spilled mucin dissects through the mylohyoid muscle and produces swelling within the neck and swelling of FOM may be present
|
|
|
What is the treatment sequence for RANULA?
|
- initial treatment is marsupialization
- further treatment involves removal of the salivary gland |
|
|
Define "MARSUPIALIZATION"
|
cannulation of the duct to re-establish communication with oral cavity
|
|
|
What is SIALOLITHIASIS?
|
occurence of calcified deposits in the salivary ductal system
|
|
|
SIALOLITHIASIS arises from what?
|
- deposition of calcium salts around nidus of debris within the lumen
- not related to systemic condition |
|
|
SIALOLITHS most often develop where?
|
Submandibular gland duct
|
|
|
MAJOR GLAND SIALOLITHS most commonly present with:
|
- episodic pain or swelling of gland, especially at mealtime
|
|
|
MINOR GLAND SIALOLITHS most commonly present with:
|
- often asymptomatic
- local swelling or tenderness - hard moveable nodule within submucosa |
|
|
What is the treatment of SIALOLITHS?
|
- small stones may be expressed from the duct
- large stones require surgical removal - gland may need to be removed if significant inflammatory damage has occurred |
|
|
Inflammation of the salivary glands can arise from what two causes?
|
INFECTION
- viral - bacterial NON-INFECTIOUS - Sjorgens - sarcoidosis - radiation therapy |
|
|
Define SIALODENITIS:
|
Inflammation of the salivary glands
|
|
|
What is the most common viral infection of salivary glands?
|
Mumps (epidemic parotitis)
|
|
|
Patients with MUMPS are contagious from which period?
|
1 day before clinical appearance of infection to 14 days after resolution.
|
|
|
Incubation period of MUMPS is how long?
|
16- 18 days
|
|
|
In Canada the MMR vaccine is recommended for:
|
all children 12-15 months,
with a second dose at 18 months |
|
|
Most cases of BACTERIAL SIALADENITIS result from:
|
- ductal obstruction (sialolithiasis, congenital structure, compression by tumour)
- decreased salivary flow (dehydration, debilitation, medication) |
|
|
More common causes of BACTERIAL SIALADENITIS result from:
|
recent major surgery
|
|
|
Most cases of BACTERIAL SIALADENITIS are caused by which bacteria?
|
Staphylococci aureus
|
|
|
ACUTE BACTERIAL SIALADENITIS is most common in which gland?
|
Parotid
|
|
|
What is NECROTIZING SIALOMETAPLASIA?
|
an uncommon locally destructive inflammatory condition of the salivary glands that clinically and histologically may mimic malignancy
|
|
|
What are some potential predisposing factors for NECROTIZING SIALOMETAPLASIA?
|
- trauma
- dental injection - ill-fitting dentures - adjacent tumours - upper respiratory tract infection - previous surgery |
|
|
Most common location of NECROTIZING SIALOMETAPLASIA are:
|
posterior hard palate
anterior soft palate |
|
|
NECROTIZING SIALOMETAPLASIA is easily mistaken for:
|
- mucoepidermoid carcinoma
- squamous cell carcinoma |
|
|
What is the treatment of NECROTIZING SIALOMETAPLASIA?
|
biopsy indicated to rule out malignancy
no specific treatment needed once diagnosis established |
|
|
What is SIALADENOSIS?
|
an unusual non-inflammatory disorder characterized by salivary gland enlargement, particularly the parotid
|
|
|
SIALADENOSIS is usually in association with what three causes?
|
- endocrine (diabetes mellitus)
- nutrition (malnutriotion) - neurogenic medications (antihypertensives, sympathomimetic drugs) |
|
|
What are the clinical features of SIALADENOSIS?
|
slowly evolving swelling of the parotid glands
|
|
|
What is BLEL?
|
benign lymphoid epithelial lesion
- autoimmune process which results in infiltration of the parotid gland with lymphocytes resulting in parenchymal destruction and enlargement of the area |
|
|
What is Sjogrens Syndrome?
|
SS is a chronic, systemic autoimmune disorders that principally involves the salivary and lacrimal glands
- continuation of BLEL |
|
|
What are the two forms of SJOGRENS?
|
Primary: xerostomia and xeropthalmia
Secondary: sicca syndrome plus any other autoimmune disease eg: rheumatoid arthitis, SLE, Hashimoto's, |
|
|
Define SIALADENITIS:
|
inflammation of salivary glands
|
|
|
Define CHRONIC SCLEROSING SIALADENITIS:
|
chronic inflammatory infiltrate with associated acinar atrophy, ductal dilatation and fibrosis
|
|
|
Define SIALOLITH:
|
calcified structures that develop within ductal system
|
|
|
Define XEROSTOMIA:
|
dry mouth
|
|
|
Define XEROPTHALMIA:
|
dry eyes
|
|
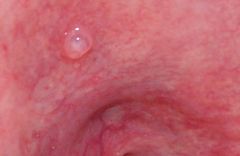
IDENTIFY THE LESION:
|
MUCOCELE
|
|
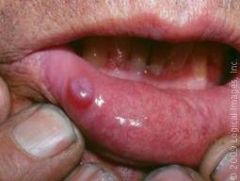
IDENTIFY THE LESION:
|
MUCOCELE
|
|
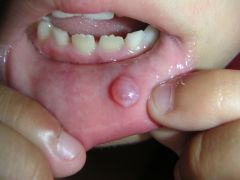
IDENTIFY THE LESION:
|
MUCOCELE
|
|
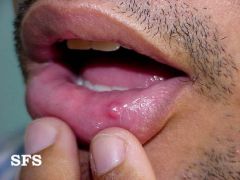
IDENTIFY THE LESION:
|
MUCOCELE
|
|
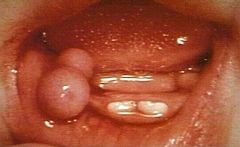
IDENTIFY THE LESION:
|
MUCOCELE
|
|
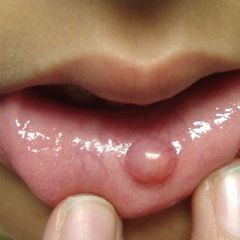
IDENTIFY THE LESION:
|
MUCOCELE
|
|
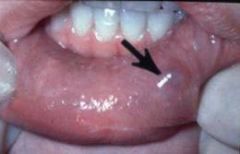
IDENTIFY THE LESION:
|
MUCOCELE
|
|
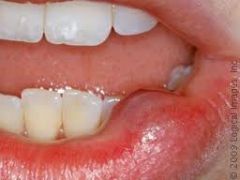
IDENTIFY THE LESION:
|
MUCOCELE
|
|
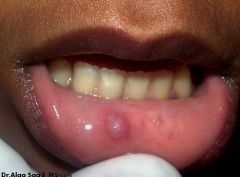
IDENTIFY THE LESION:
|
MUCOCELE
|
|
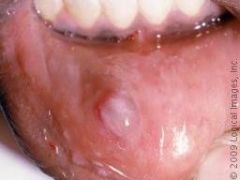
IDENTIFY THE LESION:
|
MUCOCELE
|
|
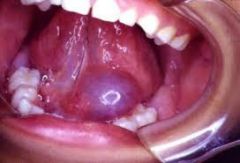
IDENTIFY THE LESION:
|
RANULA
|
|
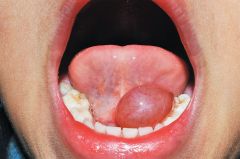
IDENTIFY THE LESION:
|
RANULA
|
|
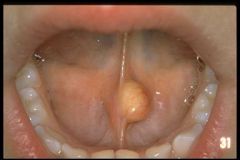
IDENTIFY THE LESION:
|
RANULA
|
|
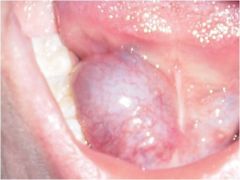
IDENTIFY THE LESION:
|
RANULA
|
|
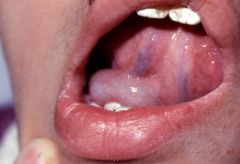
IDENTIFY THE LESION:
|
RANULA
|
|
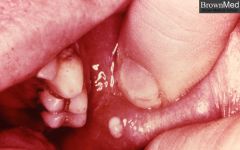
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
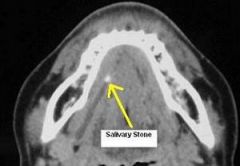
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
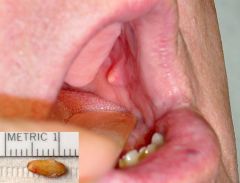
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
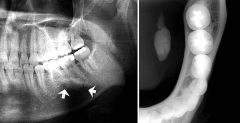
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
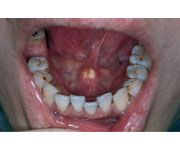
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
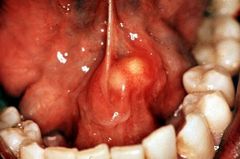
IDENTIFY THE LESION:
|
SIALOLITHIASIS
|
|
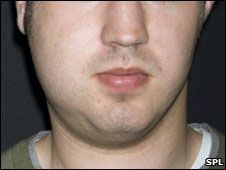
IDENTIFY THE LESION:
|
MUMPS
|
|
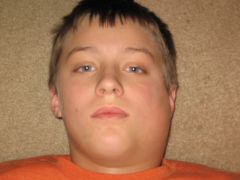
IDENTIFY THE LESION:
|
MUMPS
|
|
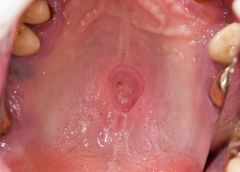
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
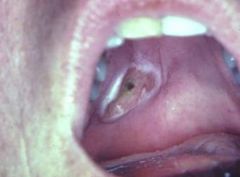
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
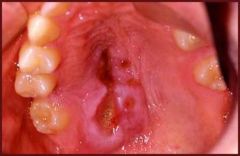
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
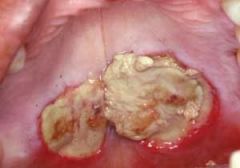
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
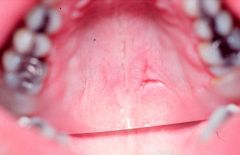
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
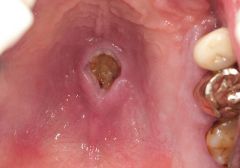
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
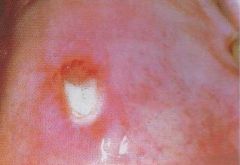
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
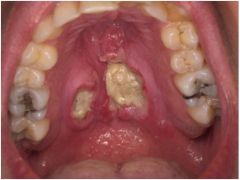
IDENTIFY THE LESION:
|
NECROTIZING SIALOMETAPLASIA
|
|
|
What is the basic unit of the salivary gland consist of?
|
- secretory component (acinus and myoepithelial cells)
- ductal component (intercalated duct, striated duct, and excretory duct) |
|
|
BENIGN parenchymal tumours are classified as what?
|
ADENOMAS
|
|
|
MALIGNANT parenchymal tumours are classified as what?
|
ADENOCARCINOMAS
|
|
|
What is the etiology of NEOPLASTIC SALIVARY GLAND DISEASE?
|
- unknown
- risk factors include: - radiation exposure - genetic predisposition - tobacco use - exposure to certain industrial chemicals - viruses |
|
|
What is the MOST COMMON SITE of salivary gland neoplasm?
|
PAROTID GLAND
|
|
|
NEOPLASMS of parotid gland are usually what kind?
|
BENIGN
|
|
|
NEOPLASMS developing within sublingual glands are ___ , but when they do occur they are usually ______ .
|
RARE, MALIGNANT
|
|
|
Where is the most frequent area to have malignancy of salivary tumour?
|
SUBLINGUAL
|
|
|
What is the SECOND most common site for salivary tumours?
|
MINOR SALIVARY GLANDS
|
|
|
What is the most frequent location of MINOR SALIVARY GLAND TUMOURS?
|
Palate
|
|
|
What is the SECOND most common area for MINOR SALIVARY GLAND TUMOURS?
|
LIPS
|
|
|
Which lip more commonly has minor salivary gland tumours?
|
UPPER LIP more common
|
|
|
Which MINOR SALIVARY GLAND sites have the HIGHEST frequency of MALIGNANT SALIVARY GLAND TUMOURS?
|
- Retromolar
- FOM - Tongue - LOWER lip |
|
|
What is the usual presentation of BENIGN salivary gland neoplasms?
|
- slow enlargin
- painless - circumscribed - firm mass - freely moveable |
|
|
What is the treatment of choice for all benign salivary gland tumours?
|
SURGICAL EXCISION with a cuff of surrounding normal tissue
|
|
|
What is the MOST COMMON SALIVARY GLAND NEOPLASM?
|
PLEOMORPHIC ADENOMA (Benign Mixed Tumour)
|
|
|
What are the most common INTRA-ORAL sites of PLEOMORPHIC ADENOMA?
|
PALATE > upper lip > buccal mucosa
|
|
|
What complication may arise if you DON'T remove a PLEOMORPHIC ADENOMA?
|
May undergo malignant transformation (5% of cases)
|
|
|
How is MONOMORPHIC ADENOMA different from PLEO?
|
Tumour characterized by proliferation of one cell type only
|
|
|
What are a few different types of MONOMORPHIC ADENOMA?
|
- Canalicular
- Basal cell adenoma - Oncocytoma - Papillary Cystadenoma Lymphomatosum |
|
|
Define "WARTHIN TUMOUR"
|
- SECOND MOST COMMON benign parotid tumour
- exclusively in parotid gland - MONOMORPHIC adenoma - |
|
|
What are some characteristic features of BENIGN SALIVARY GLAND TUMOURS?
|
- slow growing
- no ulceration - no fixation - no facial nerve palsy - encapsulated - history of slow growth - no metastasis - treatment LOCAL EXCISION |
|
|
What are some characteristic features of MALIGNANT SALIVARY GLAND TUMOURS?
|
- growth rate varied, usually rapid
- ulceration - fixation - facial nerve palsy - non-encapsulated tumours - history of slow grow to rapid growth of lesion - metastasis - treatment is surgery WITH or WITHOUT radiation |
|
|
What is the SECOND MOST COMMON BENIGN PAROTID TUMOUR?
|
- Warthin tumour
|
|
|
What is the MOST COMMON OF THE SALIVARY GLAND MALIGNANCIES?
|
Mucoepidermoid Carcinoma
|
|
|
What are the most common sites of MUCOEPIDERMOID CARCINOMA?
|
PALATE > retromolar > FOM > buccal mucosa > Lower lip
|
|
|
What is the 5 year survival rate of MUCOEPIDERMOID CARCINOMAS?
|
LOW GRADE - 89% cured
HIGH GRADE - 86% died |
|
|
List the "HIGH GRADE" malignancies of SALIVARY GLANDS ?
|
- MUCOEPIDERMOID CARCINOMA
- ADENOID CYSTIC CARCINOMA |
|
|
List the "LOW GRADE" malignancies of SALIVARY GLANDS:
|
- MUCOEPIDERMOID CARCINOMA
- ACINIC CELL CARCINOMA - POLYMORPHOUS LOW GRADE ADENOCARCINOMA |
|
|
The major and minor salivary glands develop from which embryological structure?
|
Oral ectoderm
|
|
|
Salivary gland consists of which two components?
|
SECRETORY
- acinus - myoepithelial cells DUCTAL - intercalated duct - striated duct - secretory duct |
|
|
Tumours arising from salivary glands are generally derived from one of two structures:
|
- salivary epithelium (parenchyma)
- supportive stroma (mesenchymal) |
|
|
Define ADENOMA:
|
benign parenchymal tumours
|
|
|
Define ADENOSARCOMA:
|
malignanry salivary gland tumours
|
|
|
Which site has the higher occurence of PRIMARY EPITHELIAL SALIVARY GLAND TUMOURS:
|
Parotid gland
|
|
|
The frequency of malignancy is highest in which salivary gland area?
|
sublingual
|
|
|
The highest occurence of MINOR salivary gland tumours occurs in the:
|
palate
|
|
|
Highest percentage of MALIGNANCY for intraoral minor salivary glands is:
|
- lower lip
- FOM - tongue - retromolar |
|
|
Most common location of LABIAL salivary gland tumours are in:
|
upper lip
|
|
|
What is the usual clinical presentation of BENIGN SALIVARY GLAND NEOPLASMS?
|
slow enlarging
painless circumscribed firm mass freely moveable |
|
|
What is the treatment of choice for all benign salivary gland tumorus?
|
surgical excision with a cuff of surrounding normal tissue
|
|
|
What is the MOST COMMON salivary gland neoplasm?
|
Benign Mixed Tumour (Pleomorphic Adenoma)
|
|
|
What is it called Mixed Tumour?
|
combination of neoplastic ductal epithelial and myoepithelial cells
|
|
|
PLEOMORPHIC ADENOMA most commoonly occurs in:
|
parotid gland
|
|
|
What is the treatment of PLEOMORPHIC ADENOMA?
|
parotid - remove lesion with involved lobe
submandibular - remove lesion and gland hard palate - remove lesion down to bone soft palate, labial, buccal mucosa - enucleation |
|
|
What may occur if PLEOMORPHIC ADENOMA is not removed?
|
may undergo malignant transformation in small percentage of cases
|
|
|
What is MONOMORPHIC ADENOMA?
|
proliferation of one type of cell of the salivary gland
|
|
|
What are the different forms of MONOMORPHIC ADENOMA?
|
- Cannalicular adenoma
- basal cell adenoma - oncocytoma - papillary cystadenoma lymphomatosum |
|
|
Describe the clinical features of BENIGN SALIVARY GLAND TUMOURS:
|
- slow growth
- no ulceration - no fixation - no facial nerve palsy - encapsulated - no metastasis - treatment is local excision |
|
|
Describe the features of MALIGNANT SALIVARY GLAND TUMOURS:
|
- growth rate varied
- usually rapid - ulceration - facial nerve palsy - non-encapsulated tumours - slow grow to rapid growth history - metastasis - treatment is surgery w or w/o radiation |
|
|
What is the MOST COMMON of the salivary gland malignancies?
|
mucoepidermoid carcinoma
|
|
|
What are the most common sites of MUCOEPIDERMOID CARCINOMA?
|
- palate
- retromolar region - FOM - buccal mucosa - lower lip |
|
|
What are the treatment modalities of MUCOEPIDERMOID CARCINOMA?
|
- low-grade (5-year survival: 89%): wide surgical excision
- high-grade (5 year survival 14%): wide surgical excision plus radiation |
|
|
Which are the LOW-GRADE MALIGNANCIES of SALIVARY GLANDS?
|
- acinic cell carcinoma
- polymorphous low-grade carcinoma (PLGA) - mucoepidermoid carcinoma |
|
|
What are the HIGH GRADE MALIGNANCIES of SALIVARY GLANDS?
|
- adenoid cystic carcinoma
- mucoepidermoid carcinoma |
|
|
What are the BENIGN SALIVARY GLAND TUMOURS?
|
- pleomorphic adenoma
- myoepithelioma - basal cell adenoma - canalicular adenoma - warthin tumour - oncocytoma - sebaceous adenoma - sebaceous lymphadenoma |
|
|
What are some MALIGNANT salivary gland tumours?
|
- Malignant mixed tumours
- mucoepidermoid carcinoma - acinic cell adenocarcinoma - adenoid cystic carcinoma - PLGA - basal cell adenoma - salivary duct carcinoma - myoepithelial carcinoma - cystadenocarcinoma |
|
|
Define CARCINOMA EX PLEOMORPHIC ADENOMA:
|
- malignant transformation of EPITHELIAL component of pre-existing benign mixed tumour.
- most common of the malignant mixed tumours - mostly within parotid gland - TWO SETTINGS: 1) benign mixed tumour that has been treated and has had multiple recurrences 2) benign tumour present for many years without treatment |
|
|
What are the most common salivary gland tumours seen in children?
|
- hemangioma
- lymphangioma - neurofibroma |

