![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
174 Cards in this Set
- Front
- Back
|
What are the three general functions of the kidneys?
|
- Excretion
- Homeostasis - Endocrine |
|
|
How much urine is produced per day by the kidneys?
|
1500 ml urine
|
|
|
What does the kidney produce? What does it excrete?
|
- Produces ultra-filtrate as blood passes through kidney
- Excess water and ions, some drugs, toxins, toxin byproducts, and metabolic breakdown products (urea, creatinine) excreted in urine |
|
|
What are the homeostatic functions of the kidney?
|
- Regulates and maintains extracellular fluid volume and composition
- Selective secretion and reabsorption of water, ions (Na, K, H, Ca/PO4) - Maintains acid-base balance by generating bicarb and selective secretion of H+ ions |
|
|
What are the endocrine functions of the kidney?
|
- Monitors O2 carrying capacity of blood
- Regulates BP through renin-angiotensin system - Converts 25-OH Vitamin D3 to active form via hydroxylation |
|
|
Macroscopically, what is the kidney subdivided into?
|
- Cortex
- Medulla |
|
|
What kinds of tissues does the kidney consist of?
|
- Mostly parenchyma (functional tissue)
- Little stroma (supportive tissue) |
|
|
What is the appearance and consistency of the cortex of the kidney?
|
- Granular appearance
- Homogenous in consistency - Linear arrays of tubules extending into cortex = medullary rays |
|
|
What are medullary rays?
|
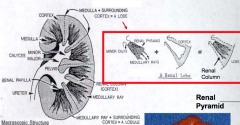
Linear arrays of tubules extending into the cortex
|
|
|
What is the appearance of the medulla of the kidney?
|
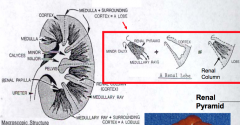
- Striated appearance
- Consists of renal pyramids - Renal Papilla = apex or tip of a renal pyramid |
|
|
What is the apex of tip of a renal pyramid?
|
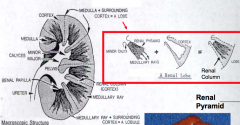
Renal Papilla
|
|
|
What is a kidney lobe?
|
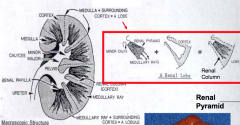
- Macroscopic subdivision
- Consists of a renal pyramid and its surrounding cortex - Lobar structure is usually indistinct externally as well as internally |
|
|
What is a kidney lobule?
|
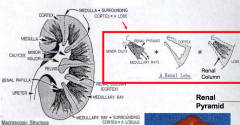
- Microscopic subdivision
- Consists of a medullary ray and the cortical tissue (primarily nephrons) on either side - Tubules of these nephrons connect w/ collecting ducts within medullary rays |
|
|
What is the difference between a kidney lobe and a kidney lobule?
|
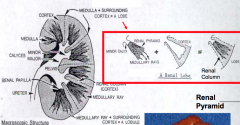
Lobe: macroscopic subdivision
- Consists of a renal pyramid and its surrounding cortex Lobule: microscopic subdivision - Consists of a medullary ray and the cortical tissue (primarily nephrons) on either side |
|
|
What is in the capsule of the kidney?
|
Fibrous CT that surrounds the kidney
|
|
|
Is the parenchyma of the kidney subdivided by septa?
|
No
|
|
|
What percent of the total body weight is kidney? How much of the cardiac output / minute do the kidneys receive?
|
- 0.5% of total body weight
- 20-25% of total cardiac output / minute |
|
|
How often does the total blood volume of the body pass through the kidneys?
|
Every 4-5 minutes
|
|
|
How much fluid is extracted from the blood in the kidney per minute as filtrate? Per day?
|
- 125 mL/minute (180L/day) but 124 mL/minute is reabsorbed
- Net: 1 mL/minute is excreted as urine |
|
|
How many capillary plexuses are associates with the nephron?
|
2
|
|
|
What is the glomerulus? What supplies it? What drains it?
|
- Tuft of capillary loops
- Supplied by afferent arteriole - branch of the interlobular artery - Drained by efferent arteriole that supplies capillaries associated with tubules of nephron |
|
|
What drains the glomeruli of Cortical Nephrons? Where does this go?
|
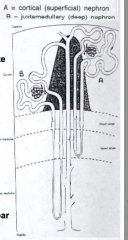
Drained by efferent arterioles that go to Peritubular Capillary Plexus (surrounds tubules of nephron) = A
|
|
|
What drains the glomeruli of Juxtamedullary Nephrons? Where does this go?
|
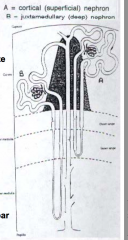
Drained by efferent arterioles that form long capillary loops, called Vasa Recta (extends into medulla) = B
|
|
|
What supplies the Peritubular Capillary Plexus?
|
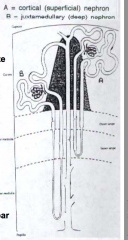
Efferent arterioles that drain the glomeruli of the Cortical Nephrons
|
|
|
What supplies the Vasa Recta?
|
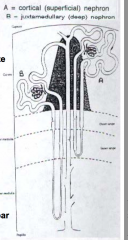
Efferent arterioles that drain the glomeruli of the Juxtamedullary Nephrons
|
|
|
How do Cortical nephrons compare to Juxtamedullary nephrons?
|
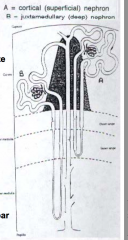
- Juxtamedullary nephrons have a long thin segment of Henle's Loop (Vasa Recta)
- This is important for maintaing osmotic gradients in the interstitial compartment of the medulla |
|
|
What lines the descending loop of the Vasa Recta? Ascending loop?
|
- Descending loop: continuous endothelium
- Ascending loop: fenestrated endothelium |
|
|
What is the pattern of the venous drainage of the kidney?
|
Follows the arterial pattern
|
|
|
How many nephrons are there per kidney?
|
1.3 - 2 million
|
|
|
What is a renal corpuscle? Location?
|
- Spherical, double-layered epithelial sac (renal capsule) that surrounds a network of capillaries (glomerulus)
- Located in kidney cortex - Aka Bowman's Capusle |
|
|
What is the polarity of a renal corpuscle?
|
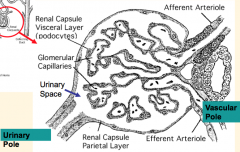
- Vascular Pole: where arterioles enter and exit
- Urinary Pole: continuous with proximal convoluted tubule |
|
|
How does the size of the afferent (supplying) arteriole compare to the efferent (draining) arteriole? Implications?
|
- Afferent arteriole is larger in diameter than the efferent arteriole
- Size difference creates a pressure differential that drives glomerular filtration |
|
|
What drives glomerular filtration?
|
Pressure differential caused by afferent arteriole being larger than efferent arteriole
|
|
|
What are the layers of the renal corpuscle (Bowman's Capsule)? What kind of cells?
|
- Parietal layer (outer) = simple squamous epithelium
- Visceral layer (inner) = simple squamous epithelium composed of podocytes |
|
|
What is the relationship between the parietal and visceral layers of the renal corpuscle?
|
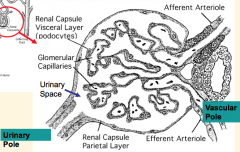
Parietal layer reflects at vascular pole to become the visceral layer
|
|
|
What are podocytes? Where are they found?
|
- Cells with several primary cell processes which branch into secondary foot processes called pedicles
- Found in visceral layer of renal corpuscle (Bowman's capsule) |
|
|
What are pedicles?
|
- Secondary foot processes coming off of podocytes
- Aligned along the glomerular capillary basement membrane |
|
|
What is the space between two epithelial layers of the renal corpuscle (Bowman's capsule)?
|
Urinary Space (continuous with proximal tubule)
|
|
|
What enters the urinary space?
|
Glomerular filtrate
|
|
|
What is the name of the filtration membrane of the kidney? What are the components?
|
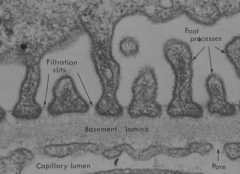
Glomerular Filtration Barrier:
- Glomerular capillary endothelium - Glomerular basement membrane - Visceral layer of Bowman's capsule |
|
|
How does the glomerular capillary endothelium contribute to the filtration barrier of the glomerulus?
|
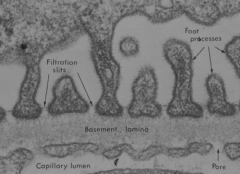
- Discontinuous endothelium with numerous 70-100nm pores with no diaphragm
- Pores are freely permeable to water and solutes ≤ 6-8kD and moderately permeable to molecules 8-16kD - Luminal surface has a negative charge coated w/ glycocalyx (consists of neg. charged proteoglycan) |
|
|
How does the glomerular basement membrane contribute to the filtration barrier of the glomerulus?
|
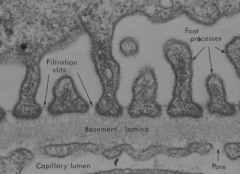
- 300-370 nm thick (2-3x thicker than a normal BM)
- Prevents protein from entering glomerular filtrate - Physical size barrier prevents proteins >70kD from passing - Charge barrier prevents proteins <70kD from passing |
|
|
What are the layers of the glomerular basement membrane?
|
- Lucent layer: lamina rara interna (rich in polyanions)
- Dense basal lamina (type IV collagen) - Lucent layer: lumina rara externa (rich in polyanions) |
|
|
What is the innermost layer of the glomerular basement membrane? What does it contain?
|
- Lucent layer: lamina rara interna
- Rich in polyanions |
|
|
What is the middle layer of the glomerular basement membrane? What does it contain?
|
- Dense basal lamina
- Type IV collagen |
|
|
What is the outermost layer of the glomerular basement membrane? What does it contain?
|
- Lucent layer: lamina rara externa
- Rich in polyanions |
|
|
How does the visceral layer of Bowman's Capsule contribute to the filtration barrier of the glomerulus?
|
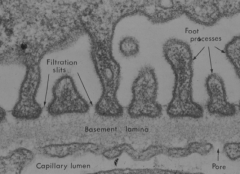
- Consists of epithelial cells called Podocytes because of their primary and secondary foot processes (pedicles)
- Pedicles inter-digitate along glomerular BM - Space between pedicles is the filtration slit (25-40 nm) and bridged by electron dense filtration slit diaphragm - Diaphragm is a modified adherens junction consisting of Nephrin - Podocalyxin, a sialoglycoprotein, covers the subpodocyte space |
|
|
What do the pedicles interdigitate along?
|
Glomerular Basement Membrane
|
|
|
What is the size of spaces/pores in the layers of the glomerular filtration barrier? Presence of a diaphragm?
|
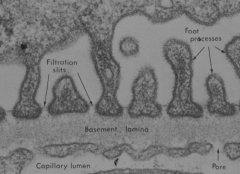
- Glomerular capillary endothelium: 70-100 nm pores (no diaphragm)
- Glomerular basement membrane: size not specified - Visceral layer of Bowman's capsule: 25-40 nm (covered by filtration slit diaphragm) |
|
|
What size of molecules can fit through the layers of the glomerular filtration barrier?
|
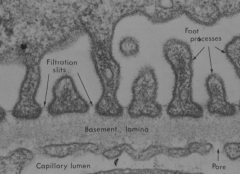
Glomerular capillary endothelium:
- Freely permeable to water and solutes ≤ 6-8 kD - Moderately permeable to solutes 8-16 kD Glomerular basement membrane: - Physical barrier limits proteins >70 kD - Charge barrier limits proteins <70 kD Visceral layer of Bowman's Capsule: - Not specified |
|
|
What does the diaphragm covering the filtration slits (25-40nm) in the visceral layer of Bowman's capsule consist of?
|
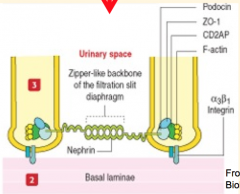
Modified adherens junction consisting of the protein Nephrin
|
|
|
What covers the subpodocyte space?
|
Podocalyxin, a sialoglycoprotein
|
|
|
What structure abuts the inner surface of the glomerular BM?
|
Renal Mesangium: consists of cells and ECM
|
|
|
What kind of cells are in the Renal Mesangium? Receptors? Secretions?
|
- Cells are modified pericyte / smooth muscle cells
- Receptors for ANP (atrial natriuretic peptide) and AngII - Secrete Endothelin, Cytokines, and Prostaglandins |
|
|
What does the ECM in the Renal Mesangium contain?
|
Fibronectin and collagen
|
|
|
What are the functions of the Mesangium?
|
- Physical support for the glomerulus
- Regulation of glomerular flow - Phagocytic activity regulates turnover of glomerular BM and anything (eg, immune molecules) that enter the mesangial matrix |
|
|
What is the term for injury to or disease of the glomerulus? What can cause this?
|
Glomerulonephritis
- Inflammation injures one or more components of the glomerular filtration barrier - Mediated by immune mechanisms like Abs directs to glomerular filtration components or circulating Ab-Ag complexes (d/t infection or auto-immune condition) |
|
|
What are the outcomes of Glomerulonephritis?
|
- Proteinuria (protein in urine)
- Hematuria (blood in urine) - Oliguria (decreased urine production) - Edema - HTN (sometimes) - Renal failure (if rapidly progressive) |
|
|
What are the components of the proximal tubule?
|
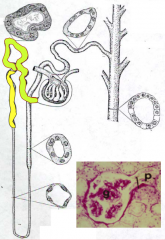
- Convoluted portion - green
- Straight portion (aka Thick Descending Limb) - yellow |
|
|
Where does the convoluted portion of the Proximal Tubule begin? Location?
|
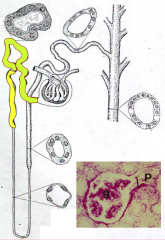
- Starts at Urinary Pole
- Located in Cortex |
|
|
What type of cells line the convoluted and straight portions of the Proximal Tubule? What are the characteristics of these cells?
|
Convoluted:
- Cuboidal to columnar epithelial cells - Brush border on apical side coated in glycocalyx (infoldings increase surface area for endocytosis) - Lysosomes and apical vesicles in cytoplasm - Inter-digitation of lateral cell membrane and basal cell processes make borders indistinct - Lots of mitochondria at base of cell for energy for transport Straight: - Cuboidal epithelial cells - Similar but less prominent features as convoluted portion (In general: "high cuboidal" epithelium with indistinct cell borders and few, basally located nuclei) |
|
|
Proximal Tubule:
- Type of epithelium? - Cell borders? - Nuclei? - Cytoplasmic staining? |
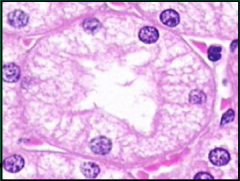
- High cuboidal epithelium
- Indistinct cell borders - Few basally located nuclei - Eosinophilic, granular cytoplasmic staining |
|
|
What is reabsorbed in the proximal tubule?
|
- 65-70% of Na+
- H2O via AQP-1 channels (ADH not required) - All glucose, AAs, protein (<70kD) - HCO3, K+, Cl-, PO4 |
|
|
What is excreted in the proximal tubule?
|
- H+ ions
- Organic acids and bases |
|
|
How does the fluid leaving the proximal tubule compare to the plasma?
|
Iso-osmotic
|
|
|
What are the components of the Loop of Henle? Location?
|
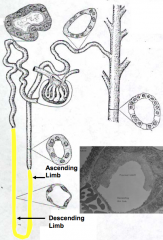
1. Straight portion of Proximal Tubule (thick descending limb)
2. Thin descending limb 3. Thin ascending limb / segments 4. Straight portion of Distal Tubule (thick ascending limb) - Primarily located in medulla |
|
|
What determines the length of the loop's thin segment(s)?
|
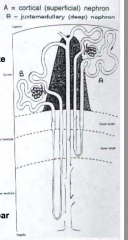
Location of renal corpuscle:
- Cortical nephrons have short loops that have only a descending thin limb - Juxtamedullary nephrons have long loops that have ascending and descending thin limbs |
|
|
What kind of epithelium lines the Loop of Henle? Other characteristics?
|
Thick portions: cuboidal epithelium
- PT (thick descending): high cuboidal - DT (thick ascending): low cuboidal Thin portions: simple squamous epithelium - Thin Ascending: cell membranes between epithelial cells are interdigitated, resulting in water impermeability - Thin Descending: permeable to water |
|
|
Which part of the Loop of Henle is impermeable to water? Why?
|
Thin Ascending Limb - cell membranes between epithelial cells are interdigitated, resulting in water impermeability
|
|
|
How does the tubular fluid in the thin ascending limb compare to the plasma?
|
Iso-osmotic
|
|
|
How does the tubular fluid in the thin descending limb compare to the plasma?
|
Hyper-tonic
|
|
|
What kind of reabsorption/secretion occurs in the thin descending limb? Outcome?
|
- H2O permeable (less for Na+/urea)
- Water diffuses out - Urea in - Leads to hypertonic fluid |
|
|
What kind of reabsorption/secretion occurs in the thin ascending limb? Outcome?
|
- H2O impermeable
- Na+, Cl- diffuse out - Urea enters - Leads to hypertonic interstitium and iso-osmotic tubular fluid |
|
|
What are the parts of the Distal Tubule?
|
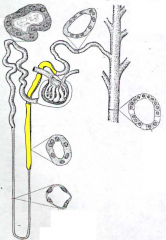
- Straight Portion (Thick Ascending limb) - yellow
- Convoluted Portion (Early Distal Tubule) |
|
|
What kind of epithelium lines the parts of the Distal Tubule? Characteristics?
|
Straight portion: simple cuboidal epithelium
- Apical surface has a few microvilli and efficient tight junctions at lateral cell borders - Adjacent cells have extensive inter-digitations of lateral and basal cell membrane - Abundant mitochondria by basolateral membrane Convoluted Part: simple cuboidal epithelium - Fewer microvilli, mitochondria, and basal inter-digitations than in straight section |
|
|
When does the "straight portion" end and the "convoluted portion" begin in the Distal Tubule?
|
Straight portion ends when the Distal Tubule contacts the renal corpuscle at the Macula Densa (located at arterial pole)
|
|
|
What kind of reabsorption/secretion occurs in the straight portion of distal tubule (thick ascending limb)? Outcome?
|
- Impermeable to H2O
- Na+, Cl-, Ca2+, Mg2+, K+, HCO3 reabsorbed - H+ ions secreted - Iso-osmotic fluid |
|
|
What kind of reabsorption/secretion occurs in the convoluted portion of distal tubule (thick ascending limb)? Outcome?
|
- Na+ (aldosterone responsive) reabsorbed
- Cl-, K+, HCO3 reabsorbed - H2O (ADH required) reabsorbed - K+, urate, H+ ions, NH3 secreted - Ammonia --> ammonium ions - Initially iso-osomotic, but becomes hypo-osmotic as it enters collecting duct |
|
|
Distal Tubule:
- Type of epithelium? - Cell borders? - Nuclei? - Cytoplasmic staining? |
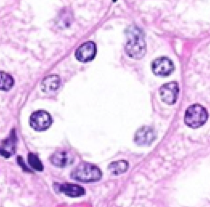
- Low cuboidal epithelium
- Indistinct cell borders - Many, centrally located nuclei - Pale staining cytoplasm |
|
|
What piece of the tubular system of the nephron is between the distal tubule and the collecting duct?
|
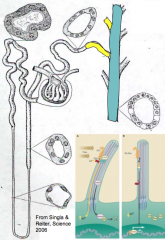
"Collecting Tubule" aka Late Distal Tubule = yellow
|
|
|
What are the characteristics of the Collecting Tubule / Late Distal Tubule? What is it dependent on?
|
- Transition segment
- ADH-dependent segment where Na+ is reabsorbed and K+ is secreted - Made of principal cells |
|
|
What kind of cells are in the Collecting Tubule / Late Distal Tubule?
|
Principal cells - ADH-dependent - Na+ is reabsorbed and K+ is secreted
|
|
|
What kind of cells are in the Collecting Ducts? Characteristics?
|
- Cuboidal to columnar epithelium
- Principal (light) cells have one primary cilium and ADH sensitive AQP-2 water channels - Intercalated (dark) cells have apical folds, microvilli, apical vesicles, basal membrane infoldings, and numerous mitochondria |
|
|
Collecting Duct:
- Type of epithelium? - Cell borders? - Nuclei? - Cytoplasmic staining? |
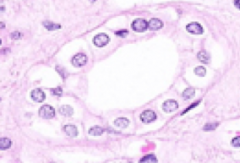
- Cuboidal to columnar epithelium
- Distinct cell borders - Many, centrally located nuclei - Pale staining cytoplasm |
|
|
What happens in the collecting duct in the presence of ADH? Outcome?
|
- ADH-sensitive AQP-2 water channels open and lets water diffuse out
- Urea also diffuses out - Increases urine tonicity and inhibits diuresis |
|
|
What happens in the collecting duct in the absence of ADH? Outcome?
|
- AQP-2 water channels remain closed, preventing reabsorption of H2O
- Leads to polyuria and hypotonic urine (Diabetes Insipidus) |
|
|
What is the function of the single non-motile cilium on the principal cells of the collecting duct?
|
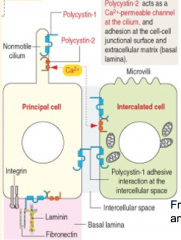
Acts as a flow sensor mediated by Polycystin 1 and 2
|
|
|
What happens if there are defects in Polycystin 1 and 2?
|
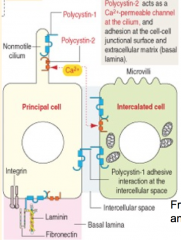
Leads to Polycystic Kidney Disease (single non-motile cilia on principal cells are unable to detect flow in collecting duct)
|
|
|
What can cause tubular disease?
|
- Toxins
- Drugs - Infections - Metabolic disturbances - Ischemia |
|
|
What does tubular disease affect? Outcome?
|
- Affects reabsorptive and secretory functions of the tubules
- Results in either polyuria (frequent urination) or oligo/anuria (infrequent/absence of urination) - May cause renal failure d/t accumulation of toxic substances - Acidosis results because of a failure to excrete H+ ions |
|
|
What is the space between the tubules? What does it contain?
|
Renal Interstitium - contains fibroblasts that produce interstitial CT and capillaries derived from efferent arterioles (cortex) and vasa recta (medulla)
|
|
|
Where is the renal interstitium most abundant? Sparse?
|
- Most abundant: Medulla
- Sparse: Cortex |
|
|
What are the capillaries derived from in the Renal Interstitium?
|
- Cortex: Efferent Arterioles
- Medulla: Vasa Recta |
|
|
What is the mechanism of modifying and concentrating urine?
|
Counter-current Multiplier Effect
|
|
|
What is the outcome of the Counter-current Multiplier Effect?
|
Concentrates urine
|
|
|
What is the basis of the Counter-current Multiplier Effect?
|
- Ascending limb of Loop of Henle is impermeable to water, while descending limb is somewhat water permeable
- Urea, Na+, and Cl- concentrations are high in the interstitium - Arterioles around the descending limb of loop have continuous endothelium and the venules around the ascending limb of loop have fenestrated endothelium - Mechanism to modify and concentrate the urine |
|
|
What are the components of the Counter-current Exchanger? Function?
|
- Vasa Recta
- Arcuate Arteries - Tubules - Collecting Ducts - Protects ion gradient |
|
|
What are the components of the Juxtaglomerular Apparatus?
|
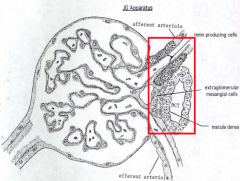
- Renin-Producing (JG) cells
- Extraglomerular Mesangial (Iacis) cells - Macula Densa |
|
|
What kind of cells in the juxtaglomerular apparatus produce renin? Location?
|
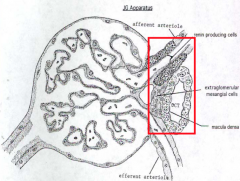
Modified smooth muscle cells in wall of afferent arteriole
|
|
|
Where is Angiotensinogen produced? How is it converted?
|
- Produced in liver
- Converted by Renin to to Angiotensin I |
|
|
Where is Angiotensin I converted? How is it converted?
|
Converted in lungs to Angiotensin II by ACE (converting enzyme)
|
|
|
What are the effects of Angiotensin II?
|
- Vasoconstriction
- ↑ Aldosterone production / secretion - Na+/H2O reabsorption in collecting ducts - ↑ BP and blood volume |
|
|
How are the extraglomerular mesangial (iacis) cells connected to each other and to the juxtaglomerular apparatus
|
Gap Junctions
|
|
|
What kind of cells are in the Macula Densa? Location?
|
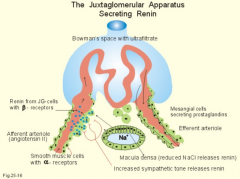
Columnar cells in the distal convoluted tubule adjacent to the afferent arteriole at renal corpuscle of origin
|
|
|
What is the function of the Macula Densa?
|
- Detects Na+ (primarily) and Cl- concentration
- Passes information onto the Juxtaglomerular apparatus cells - Results in alterations of the filtration rate and auto-regulation of blood volume |
|
|
What is the function of Erythropoietin?
|
- Stimulates division of RBC (erythrocyte) precursors
- Increases release of RBC from bone marrow |
|
|
What stimulates production of Erythropoietin?
|
Hypoxia (low tissue O2 tension) as in anemia, high altitude, hemorrhage, or impaired pulmonary function
|
|
|
What kind of cells produce Erythropoietin?
|
Interstitial cells of the renal cortex
|
|
|
What happens in Renal Failure?
|
Kidneys are unable to remove accumulated metabolites from blood d/t impairment of the glomerular filtration rate
|
|
|
What can cause Acute Kidney injury / failure?
|
- Pre-renal (vascular) injury
- Intrinsic (kidney) injury - Post-renal (obstructive) injury |
|
|
What happens in Acute Kidney injury / failure?
|
- GFR decreases as detected by increased serum creatinine
- Can lead to Azotemia (increased nitrogenous substance in blood), oliguria, ischemia, and an increase of toxins in the blood |
|
|
How do you detect a change in GFR?
|
Decreased GFR equates to an increased serum creatinine
|
|
|
What happens in end-stage renal disease?
|
- Irreversible injury to kidneys
- Leads to uremia and hematuria (blood in urine) |
|
|
What can cause end-stage renal disease?
|
- Caused by glomerular injury
- Autosomal dominant polycystic disease - Other problems |
|
|
What structures collect urine from the kidney and transport it to the urinary bladder?
|
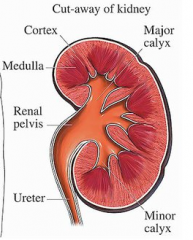
- Calyces
- Pelvis - Ureters |
|
|
What are the layers of the calyces, pelvis, and ureters?
|
- Mucosa
- Muscularis - Adventitia |
|
|
What kind of cells line are in the mucosa / lining of the urinary passages?
|
Transitional Epithelium (aka Urothelium)
- Apical plasma membrane contains thicker, specialized areas called plaques - Plaques are associated with actin filaments in cell cortex Lamina Propria - Underlies the epithelium - Contains abundant elastic tissue and collagen |
|
|
What are the plaques in the excretory / urinary passages?
|
- Thicker, specialized areas on apical plasma membranes of transitional epithelium in the mucosal layer
- Associated w/ actin filaments in cell cortex |
|
|
What is the function of plaques?
|
- Relaxed state: plaques form infoldings called fusiform vesicles whose lumen is continuous w/ the lumen
- Destended state: plaques can unfold, allowing the apical membrane to expand |
|
|
What is the middle layer of the excretory passages?
|
Muscularis
- Thin layers of smooth muscle |
|
|
What are the layers of muscle in the muscularis layer of the excretory passages?
|
Upper 2/3 has 2 layers:
- Inner: longitudinal muscle - Outer: circular muscle Lower 1/3 has 3 layers (similar to urinary bladder): - Inner: longitudinal muscle - Middle: circular muscle - Outer: longitudinal muscle |
|
|
What is the outer layer of the excretory passages?
|
Adventitia - consists of fibrous CT
|
|
|
What kind of mucosa is in the urinary bladder?
|
Thick transitional epithelium
|
|
|
What makes up the muscularis layer of the urinary bladder?
|
Detrusor muscle - 3 layers of smooth muscle interlaced with each other and with the surrounding fibrous CT
|
|
|
At the bladder outlet (neck), what does the smooth muscle of the urinary bladder form?
|
Internal urethral sphincter around the opening to the urethra
|
|
|
What is the superior surface of the urinary bladder covered with?
|
Peritoneum forming a serosa
|
|
|
What is the exterior layer of the sides and base of the urinary bladder covered with?
|
Adventitia
|
|
|
What innervates the urinary bladder?
|
Sympathetic (vascular control)
- Kidney: T10-L1 - Ureter: T11-L2 - Bladder: T11-L2 Parasympathetic (micturition) fibers - Vagus nerve (kidneys and ureter) - Pelvic splanchnics (ureter and urinary bladder) |
|
|
How long are the male and female urethras?
|
- Male: 15-20 cm
- Female: 3-5 cm |
|
|
What are the components of the male urethra?
|
- Prostatic
- Membranous - Penile |
|
|
What lines the different portions of the male urethra?
|
- Prostatic: transitional epithelium
- Membranous & Penile: stratified to pseudostratified columnar epithelium - Navicular fossa (distal tip of penile urethra): non-keratinized stratified squamous epithelium |
|
|
What lines the different portions of the female urethra?
|
- Initial portion: transitional epithelium
- Later: non-keratinized stratified squamous epithelium |
|
|
Who is affected by Benign Prostatic Hypertrophy (nodular hyperplasia)? What happens?
|
- Males >45yo
- Hypertrophy of glands of prostate surrounding the urethra - Can cause urethral obstruction |
|
|
What is the fancy term for kidney stones?
|
Renal Calculi
|
|
|
How common are Renal Calculi (kidney stones)? Who most commonly gets them?
|
- 7-21/1000
- Especially in sedentary men |
|
|
What factors enhance renal calculi (kidney stone) formation?
|
- Hypercalcemia
- pH change - Supersaturation of ions |
|
|
What is the 6th most common malignancy in the USA? What is it associated with?
|
Bladder cancer, associated w/ smoking
|
|
|
Where are kidneys located?
|
- Abdomen (T12-L3)
- R kidney is slightly lower than L kidney (d/t liver) - Primarily retroperitoneal - Adjacent to posterior abdominal wall |
|
|
How long, wide, and thick are the kidneys? How do they compare to one another?
|
- Length: 10-11 cm (L kidney is slightly longer)
- Width: 5-6 cm (L kidney is slightly narrower) - Thickness: 2.5-3 cm (about the size of your fist) |
|
|
What is the description of the lateral and medial borders of the kidneys?
|
- Lateral: convex
- Medial: concave |
|
|
How much do kidneys weight in males and females?
|
- Males: 150g
- Females: 135g |
|
|
What is the organization of the renal vessels leaving the kidney from anterior to posterior?
|
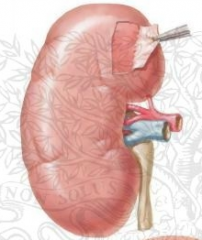
Renal vein - renal artery - ureter
|
|
|
What are the divisions of the vascular supply to the kidney?
|
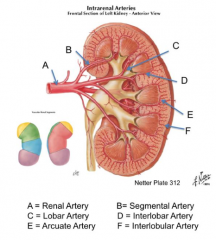
Biggest to smallest branches:
- Renal Artery - Segmental Artery - Lobar Artery - Interlobar Artery - Arcuate Artery - Interlobular Artery |
|
|
What happens if you resect a part of the kidney?
|
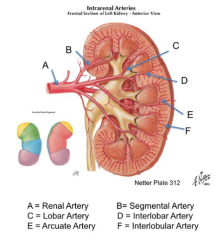
It should be fine because there are no anastomoses of arteries
|
|
|
What structures do the autonomic nerve fibers forming the renal plexus come from?
|
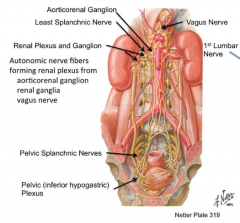
- Aorticorenal ganglion
- Rengal ganglia - Vagus nerve |
|
|
Sympathetic innervation of these structures is from which levels:
- Kidney? - Ureter? - Urinary bladder? |
- Kidney: T10-L1
- Ureter: T11-L2 - Bladder: T11-L2 |
|
|
Sympathetic innervation of the ureter is from what levels?
|
T11-L2
|
|
|
Sympathetic innervation of the kidney is from what levels?
|
T10-L1
|
|
|
Sympathetic innervation of the urinary bladder is from what levels?
|
T11-L2
|
|
|
What ribs protect the kidneys?
|
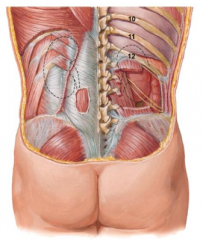
- L: 11 and 12
- R: 12 |
|
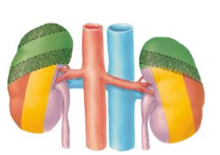
What structures in the abdomen have a relationship to the kidneys?
|
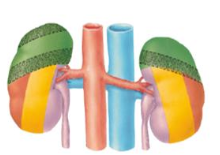
- Respiratory diaphragm (green)
- Transversus abdominis aponeurosis (orange) - Quadratus lumborum (yellow) - Psoas major (purple) |
|
|
Where is the transpyloric plane in relation to the kidneys?
|
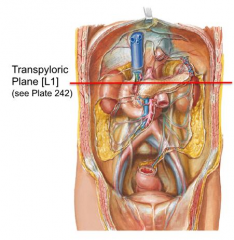
Passes through hilum of kidneys at L1
|
|
|
How long are the ureters?
|
25-30cm
|
|
|
What are the sites of ureter narrowing?
|
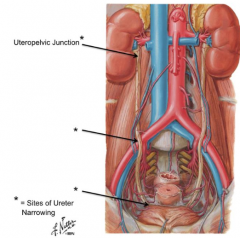
- Uteropelvic junction
- Ureter crossing over iliac arteries/veins - Entrance to bladder |
|
|
Which arteries/veins run over the ureter? Under?
|
- Vessels over ureter: renal a/v, gonadal a/v, some going to bladder
- Vessels under ureter: iliac a/v |
|
|
How does the ureter enter the bladder?
|
- At R angle to prevent reflex of urine back up into ureter
- Site of ureter narrowing |
|
|
Can you feel the kidneys?
|
No, normally they are non-palpable
|
|
|
What supports the position of the kidneys? Can they move?
|
- Well supported by fascia
- Change position slightly during inhalation and exhalation as well as while changing body position |
|
|
How much of the cardiac output goes to the kidneys?
|
20-25%
|
|
|
How common is an additional renal artery?
|
30% of population
|
|
|
What provides the blood supply to the ureters?
|
Branches of arteries encountered along its course from kidney to urinary bladder
|
|
|
Referred pain from the kidneys and ureter will be felt where?
|
T10-L2 spinal cord level distribution
|
|
|
What is the developmental view of a nephron?
|
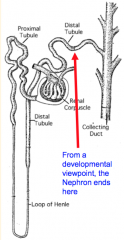
- Renal corpuscle
- Proximal tubule - Loop of Henle - Distal tubule * Does not include collecting ducts |
|
|
What is the functional view of a nephron?
|
- Renal corpuscle
- Proximal tubule - Loop of Henle - Distal tubule * Includes collecting ducts |
|
|
Case: 60yo AA non-diabetic woman comes in w/ BP of 160/100 and elevated creatinine and BUN. You suspect she has a nephropathy secondary to uncontrolled HTN.
In what component of the glomerulus would you expect to see a change responsible for this woman's problem? |
Glomerulus
|
|
|
What are the components of the Renal Corpuscle?
|
- Glomerulus
- Visceral layer of Renal Capsule - Parietal layer of Renal Capsule - Mesangium |
|
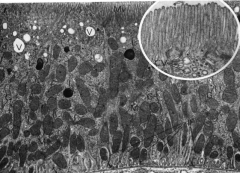
What is the primary function of this cell?
|
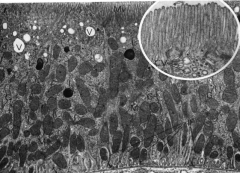
Reabsorption (microvilli increase surface area)
|
|
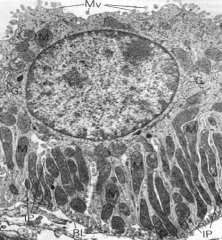
What is the primary function of this cell?
|
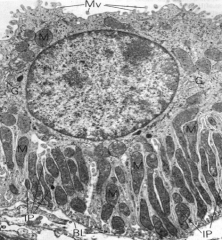
Ion Transport
|
|
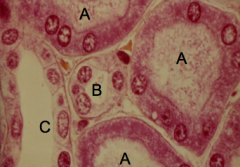
What tubule is labeled A?
|
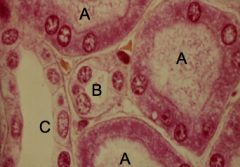
Proximal Tubule (A)
|
|
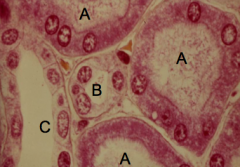
What tubule is labeled C?
|
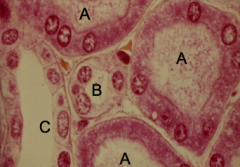
Collecting Duct (C)
|
|
|
What parts of the nephron are only found in the cortex?
|
- Renal Corpuscles
- Convoluted parts of tubules |
|
|
What parts of the nephron are found in both the cortex and the medulla?
|
Straight parts of proximal and distal tubules
|
|
|
What parts of the nephron are only found in the medulla?
|
- Loops of Henle
- Collecting Duct system |
|
|
Case: 35yo woman presents w/ 3-day hx of suprapubic pain which has recently shifted to the back (costovertebral angle). She has a temperature of 102, is a little dehydrated, and is experience dysurea (painful urination).
What might be causing this woman's distress? |
Urinary Tract Infection
|

