![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
29 Cards in this Set
- Front
- Back
|
Name two basic Ab resistance factors in s.aureus
|
1. beta lactamase resistance- eno Secrete enzyme into ECM which cleaves carbon-nitrogen bond of beta lactam ring
2. PBP mutation (PBP2a)-- mecA gen... allows for MRSA |
|
|
#1 cause of CA skin infections?
|
CA-MRSA
|
|
|
CA-MRSA compared to HA
6 main differences |
1. more virulent strains
2. PVL and mec type IV mutations 3. PSM 4. USA3000 5. Easier to treat than HA 6. No healthcare risk factors |
|
|
What is the theory that explains how CA-MRSA occured?
|
PVL (panton valentine leukocidin) cytotoxin that poke holes in leukocytes, infects MSSA, changes to MRSA with gene SCCmecIV
|
|
|
Name the many virulence factors of CA-MRSA
|
1. PVL
2. PSM- tend to have more than in HA-MRSA 3. USA300 4. ACME 5. Alpha hemolysin |
|
|
How does a fool prevent MRSA??
|
1. Wash hands dope!
2. Reduce nose picking 3. wash genitals with dial sope |
|
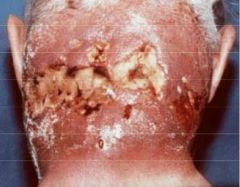
|
infected sebaceous cyst
|
|
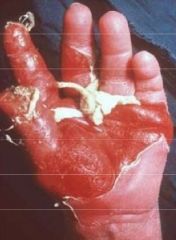
|
staph scalded skin syndrome
|
|
|
If pt complains of pain way out of proportion to the physical exam with a slight red rash what might you suspect skin wise?
|
1. necrotizing fasciitis!- has to be opened to cut the dead stuff off, may require skin grafting
- U/S sees tissue plains |
|
|
This type of skin problem tends to occur in diabetics and on the scrotum and butt
|
fournier's gangrene
|
|
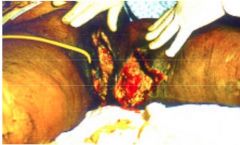
|
fournier's gangrene
|
|
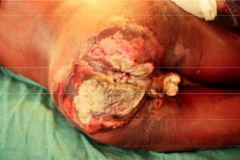
|
fournier's gangrene
|
|
|
Dry vs wet gangrene?
|
wet is bad!
wet- i.e. gas gangrene due to c. perfringens, hard to treat with Abs due to deep locations in tissue dry- ischemic tissue wait to see black vs pink |
|
|
What two drugs do you need to know interact with almost all drugs?
|
warfarin and phenobarbitol
|
|
|
Beta Lactam antibiotics general
a. MOA b. Resistance c. Static/cidal d. A/E, |
a. inhibit cell wall synthesis by bind to penicillin binding protein and inhibit transpeptidation step of petidoglycan synthesis
b. BETA-LACTAMASE, inactivation, reduced affinity for PBP, porins c. cidal d. allergic rxn, neurologic due to K+ increased in IV form (watch for kidney pts) |
|
|
PARP (penicillinase resistant penicillins)
Which on is oral? a. MOA b. Resistance c. Static/cidal d. A/E, |
dicloxacilin (oral), nafcillin, oxacillin
a. cell wall synth (see beta lactam general) b. PBP c. cidal d. Rash, diarrhea |
|
|
Beta lactam antiB's Cephlasporins
a. MOA b. Resistance c. Static/cidal d. A/E, Which is workhorse? Which is for pseudomonas? |
a. inh cell wall synthesis
b. PBP c. cidal d. billiary sludge (cholesistitis- w/ ceftrioxone), fever (common), kernicteris, bleeding Cephalexin= workhorse and oral Cephtazodone= pseudomonas |
|
|
Amoxicillin used with what to gain beta lactamase inh?
a. MOA b. Resistance c. Static/cidal d. A/E, |
used w/clavunate
a. cell wall inh b. w/o clavunate beta lactamase and always PBP c. cidal d. if used on viral infection--> "amp rash" and cramping/nausea due to Clavunate |
|
|
Clindamycin
a. MOA c. Static/cidal d. A/E, |
a. 50s binder inh. dna synthesis
c. static but penetrates bone d. C. diff colitis (MCC) due to killing natural flora of colon allowing c. diff to colonize and cause massive inflammation |
|
|
Tetracyclines
a. MOA c. Static/cidal d. A/E, |
Doxycycline (mc used)
a. aatRNA to Asite AT 30S c. static so do not use if pt. is neutropenic d. GI- diarrhea (if taken on empty stomach), , Tooth discoloring, enamel hypoplasia, Photosensitivity, AVOID W/DAIRY |
|
|
Sulfa drugs when is it given IV?
a. MOA b. Resistance c. Static/cidal d. A/E, |
TMP-SMZ (sulfaethoxazole) only IV for PCP treatment
a. SMZ inh DHF synthesis (folic acid), and TMP inh. DHFR which inh. THF (utlization of folic acid) b. ? c. cidal with both TMP and SMZ d. Steven Johnson's syndrome, Kernicterus, increase in Bilirubin w/o disease, bone marrow suppression |
|
|
Glycopeptides
a. MOA b. Resistance c. Static/cidal d. A/E, |
Vanc
a. d-ala binding inh. cell wall synthesis b. terminal d-ala replaced by d-lactate in enterobacter (VRE) c. cidal, slow acting d. nephro/ototoxic, red man syndrome |
|
|
Macrolides
a. MOA b. Resistance c. Static/cidal d. A/E, |
azith, clarith, Erythromycin- remember mother in law drug, because she makes u vomit and nauseous
a. 50s b. efflux (low levels), altered binding site (high levels) c. static d. prolonged QTsyndrome, torsades, GI |
|
|
Fluroquinolones
a. MOA b. Resistance c. Static/cidal d. A/E, |
Ciprofloxacin- good oral for pseudomonas
a. DNA structural breakage by inhibiting DNA gyrase c. few statics that can penetrate bone d. cartilage damage, achilles tendon rupture, HA (seizures due to GABA disruption in cipro use) |
|
|
Treatment plan for the following type of infection...
MSSA |
a. PARP (dicloxacillin oral or naf/oxa iv), strongest when sensitive to methacylin
b. Ceph c. Amox/clav |
|
|
Treatment plan for the following type of infection...
CA-MRSA |
a. clindamyacin
b. doxycycline c. TMP/SMX |
|
|
Treatment plan for the following type of infection...
HA-MRSA Osteomyelitis MRSA |
a. vanc -+gentamcin or +-rifabutin...
six week therapy for osteomyelitis |
|
|
Treatment plan for the following type of infection...
GABHS (strep pyo) |
a. PCN or ceph first generation
b. allergy to PCN use macrolide (z-pack) |
|
|
Treatment plan for the following type of infection...
c. perfringens |
a. PCN, if allergic use clindamycin as backup
|

