![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
50 Cards in this Set
- Front
- Back
|
A patient of Northern European descent presents with gliadin and tissue transglutaninase, blunting of villi and lymphocytes in the lamina propria. The patient also has a history of dermatitis herpetiformis.
|

Celiac sprue; autoimmune mediated intolerane of gliadin (wheat) leading to steatorrhea (excess fat in stool)
Decreased mucosal absorption primarily affects the jejunum; |
|
|
A patient presents with abdominal bloating, floating and foul smelling stools and weight loss with diarrhea. Villi appear normal.
|
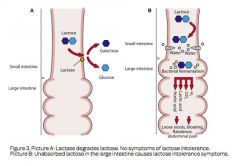
Lactose Intolerance (Disaccharidase deficiency); osmotic diarrhea; since lactase is located at the tips of intestinal villi, self limited lactase deficiency can occur following injury (viral diarrhea)
|
|
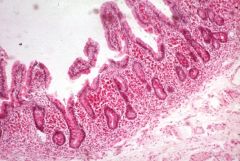
Patient presents with diarrhea, steatorrhea, weight loss and weakness. ROS is also notable for arthralgias, cardiac and neurologic symptoms. Biopsy reveals PAS-positive macrophages in intestinal lamina propria, mesenteric nodes.
|
Whipple's diesase; infection with Tropheryma whippelii (gram positive)
|
|
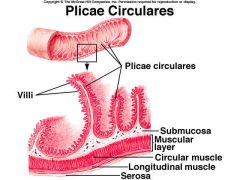
What is the function of intestinal plica?
|
Mixing of intestinal content to prevent absorption diffusion issues
|
|
|
Which part of the small intestine is the major site of digestion and absorption?
|
Jejunum
|
|
|
Which part of the small intestine is the site of intrinsic factor and bile absorption?
|
Ileum; thinnest mucosa of the three segments (12-14 ft in length)
|
|
|
Which part of the small intestine is the site of pancreatic and biliary secretion?
|
Duodenum; thickest mucosa, only 12-15 inches in length
Pyloric junction -> ligament of Treitz Chyme and digestive enzymes mixed here |
|
|
If you remove a patient's ileum what must you supplement with?
|
Vitamin B12 shots; ileum is site of intrinsic factor absorption and will be excreted otherwise
|
|
|
What is the correlation between the height of intestinal villi and renewal rate?
|
Increased renewal rate = higher villi
Renewal rate is highest in duodenum; slowest in colon |
|
|
Where do the stem cells for villi renewal originate?
|
The crypts
|
|
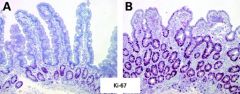
Why can't you just start eating lots of food if you haven't eaten for awhile?
|
Villi will be blunted and food will be poorly absorped = GI problems
|
|
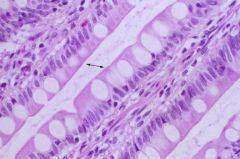
What structure is at the apical surface of the villi?
|
Brush border/microvilli; responsible for the most surface area amplification
|
|
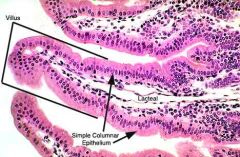
What is the function of the central lacteal?
|
Large fats are absorbed here; bypass liver and go straight to heart via subclavian vein
|
|
|
What molecules are absorbed by intestinal blood vessels contained in the villi?
|
amino acids, carbohydrates, and small fatty acids; travel to liver for processing
|
|
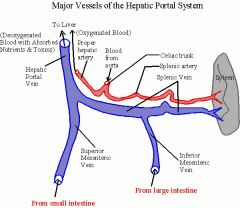
What structure provides oxygenated blood with metabolites from peripheral tissues to the liver?
|
Hepatic Artery
|
|
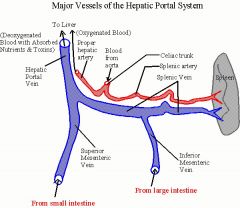
What structure provides blood rich in absorbed nutrients from the GI tract as well as hemoglobin breakdown products from the spleen?
|
Hepatic Portal Vein
|
|
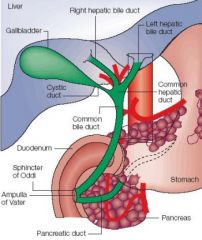
Where is bile synthesized and stored?
|
Synthesized in liver; secreted into the common hepatic duct for storage in the gallbladder; secrted into the lumen of the intestine through the common bile duct
|
|
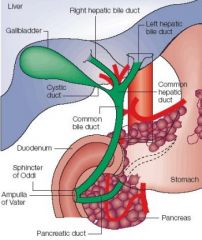
What is the significance of the hepatopancreatic ampulla?
|
Its the site of union between the pancreatic duct and the common bile duct; important anatomical landmark that marks the anatomical transition from foregut to midguit (point where celiac trunk stops supplying the gut and superior mesenteric artery takes over)
|
|
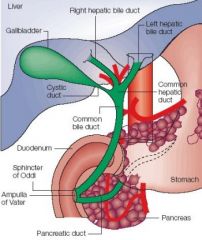
What is the significance of the sphincter of oddi?
|
Controls the introduction of bile and pancreatic secretions into the duodenum prevents entry of duodenal contents into the ampulla
|
|
|
What is the total amount of input vs output of fluid in the GI tract?
|
9L total input; 8.9 L absorbed
0.1L excreted in feces |
|
|
Describe the nature of small intestinal motility
|
Since unmixed layers must be prevented, the chyme is tossed by nonperistaltic random contractions
|
|
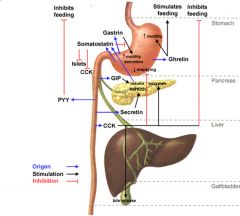
Which hormone stimulates pancreatic acinar cells to release their enzymes for digestion?
|
Cholecystokinin (CCK); also slows gastric emptying and contracts gall bladder at the top and relaxes the lower tube right at the small intestine so it can release its contents
|
|
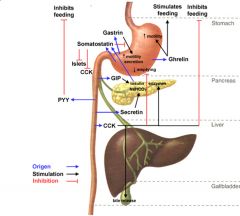
Which hormone stimulates the molecules for acid neutralization in the duodenum?
|
Secretion; stimulates pancreatic and biliary ducts to release HC03 which neutralizes acid into CO2 and water
|
|
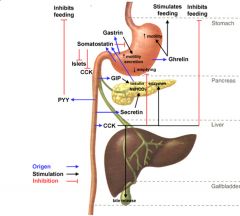
What would happen if secretin was not released from the small intestinal S cells?
|
No neutralization of acids; digestive enzymes have a pH optimum between 6.5 and 8 so you would also have enzyme dysfunctions
|
|
|
Which intestinal cells release secretin?
|
S cells
|
|
|
Which intestinal cells release CCK?
|
I cells
|
|
|
Which molecules stimulate the release of CCK?
|
Acid from stomach released secretin from wall of duodenum; also fats and amino acids
|
|
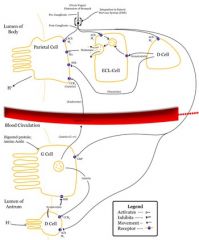
What is the source, target, and action of gastrin?
|
S: G cells in antrum of stomach
T: Parietal cells in stomach A: Increases acid Secretion |
|
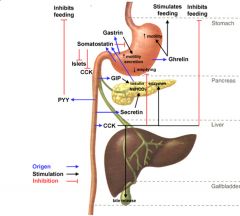
What is the source, target, and action of CCK?
|
S: I cells in duodenum and jejunum
T: Pancreas, gall bladder, sphinceter of oddi A: Enzyme secretion from acinar cells; contract gall bladder; relax sphincter of Oddi |
|
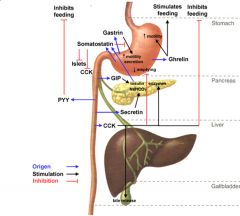
What is the source, target, and action of secretin?
|
S: S cells in duodenum and jejunum
T: Ducts of pancreas and gall bladder A: Increases bicarbonate ion secretion |
|
|
Which two hormones are not secreted from the jejunum?
Gastrin; CCK; Secretin; GIP; Motilin |
CCK and Gastrin
|
|
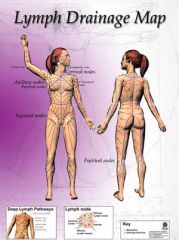
where do lymphatics in the region above the umbilicus drain?
|
Axillary lymph nodes
|
|
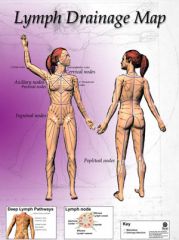
Where do lymphatics in the region below the umbilicus drain?
|
Superficial inguinal nodes
|
|
|
What is the protective function of the greater omentum?
|
Adheres to areas of inflammation; wraps itself around inflammed organs thus preventing diffuse peritonitis
|
|
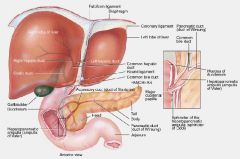
What is the function of the falciform ligament?
|
Connects the liver to the diaphragm and the anterior abdominal wall
|
|
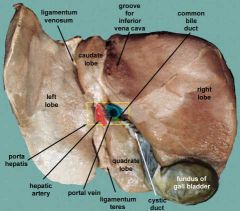
Which abdominal ligament serves no function in adults?
|
Ligamentum teres hepatis (round ligament of the liver); lies in the free margin of the falciform ligament and is formed after birth fro mthe remnant of the left umbilical vein
|
|
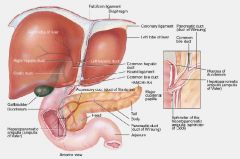
Where does the coronary ligament attach and what does it form?
|
Attaches at the diaphragmatic surface of the liver; encloses a triangular area of the lobe, the bare area of the liver (left right extensions form left and right triangular ligaments)
|
|
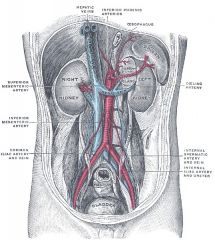
Which condition is characterized by compression of the left renal vein between the abdominal aorta and the superior mesenteric artery?
|
Nutcracker Syndrome; classically left flank pain
|
|
|
What is the potential area between the liver and right kidney?
|
Hepatorenal recess
|
|
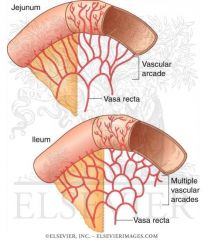
Compare and contrast the arcades and recta of the jejunum and ileum.
|
Jejunum: 1-2 arcades (arterial bridges/cross links between the channels) and long vasa recta (straight vessels)
Ileum: Many arcades and short vasa recta |
|
|
Compare and contrast from where the systemic veins vs the portal system veins form
|
Systemic V (those that drain trunk and limbs) form from cardinal veins
Portal System V: form from vitelline veins (that drain yolk sack) |
|
|
The inferior vena cava pretty much drains everything in the abdominal cavity EXCEPT what four things
|
Gut, pancreas, gall bladder, spleen; these organs first drain into the portal veins which pass to the liver before draining into the vena cava
|
|
|
What four organs input into the portal veins?
|
Gut, gall bladder, pancreas, spleen
|
|
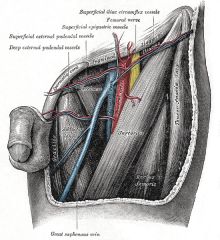
Where is the site of a direct inguinal hernia?
|
Inguinal Triangle
|
|
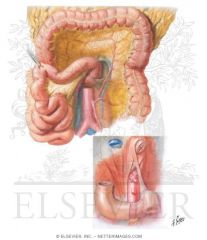
What structure connects the duodenum to the diaphragm?
|
Ligament of Treitz
|
|
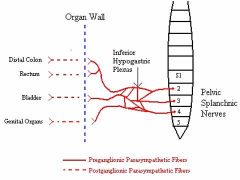
From which sacral nerves are the parasympathetics of the hindgut derived from?
|
S2-S4 (pelvic splanchnic nerves)
|
|
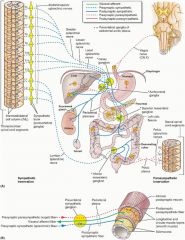
From which spinal nerve section is the sympathetic innervation of the hindgut along with visceral afferents derived from?
|
Lumbar Splanchnic nerves
|
|
Which vertebral levels are the epigastric (foregut) structures associated with?
|
T6-T9 (T5 = level of xyphoid process)
|
|
Which vertebral levels are the lingual ligament and pubis associated with?
|
L1
|
|
What vertebral level is the umbilicus associated with?
|
T10
|

