![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
98 Cards in this Set
- Front
- Back
|
Function of the male reproductive tract
|
- transports semen (sperm with secretions of accessory glands)
|
|
|
Function of the gonads
|
- Reproductive organs that produce gametes and hormones (testes and ovaries)
|
|
|
Function of the testes
|
- produces spermatozoa (gametes) or sperm
|
|
|
Accessory organs of the male reproductive tract and their functions
|
- Ductus deferens: conducts sperm from epididymis to prostate gland
- Seminal glands: secrete fluid forming bulk semen volume - Prostate gland: secretes fluid and enzymes - Urethra: conducts semen to exterior - Epididymis: site of sperm maturation |
|
|
General function of all accessory organs of the male reproductive tract
|
- secrete fluids into reproductive system or other excretory ducts
|
|
|
Male external genitalia and their function
|
- Penis: deposits sperm into vagina
- Scrotum: surrounds testes |
|
|
What is the pathway of sperm from the testis to the external environment?
|
1) Testes
2) Epididymis 3) Ductus deferens 4) Ejaculatory duct & seminal vesicle 5) Urethra (Prostate and bulbo-urethral glands) |
|
|
6 scrotum structures
|
- Scrotal cavities
- Dartos muscle - Cremaster muscle - Spermatic cords - Superficial inguinal ring - Inguinal canal |
|
|
Scrotal Cavities
|
- houses testes
- separated by the scrotal septum (marked by raised raphe = skin) |
|
|
Dartos muscle
|
- Elevates testes and wrinkles scrotal surface
|
|
|
Cremaster muscle
|
- pulls testes closer to the body during sexual arousal or cold temperatures
|
|
|
Spermatic cords
|
- Extend between testes and abdominopelvic cavity
- each contains layers of fascia and muscle which encloses: ductus deferens, blood vessels, nerves, lymphatic vessels |
|
|
Superficial inguinal ring
|
- Entrance to inguinal canal
|
|
|
Inguinal canal
|
- extends from body cavity into scrotum
|
|
|
What is an inguinal hernia?
|
- protrusions through the inguinal canal
|
|
|
4 testes structures
|
- Tunica albuginea
- seminiferous tubules - rete testis - efferent ductules |
|
|
Tunica albuginea
|
- Outer capsule continuous with the septa subdividing testes into lobules
|
|
|
Seminiferous tubules
|
- coiled tubules within lobules
- site of sperm production |
|
|
Rete testis
|
- Collecting area outside of lobules
|
|
|
Efferent ductules
|
- lead from rete testis to epididymis
|
|
|
Spermatogenesis
|
- sperm production (division)
- Steps: Mitosis, Meiosis I, Meiosis II, spermiogenesis |
|
|
What occurs during mitosis (male)
|
- Somatic cells produce two daughter cells containing 23 identical chromosome pairs (= diploid)
- Occurs in seminiferous tubules |
|
|
What occurs during meiosis I and II (male)
|
- produces four haploid cells each with 23 individual chromosomes
- during fertilization 23 paired chromosomes regained with 23 paternal and 23 maternal ( = synapsis) |
|
|
What occurs during spermiogenesis?
|
- (head, cap, tail added)
- differentiation of immature male gametes into physically mature spermatozoa |
|
|
Spermatozoon structures (5)
|
- Lacks many intracellular structures/organelles
- Acrosomal cap - head - neck - middle piece - tail (flagellum) |
|
|
What does the acrosomal cap of the spermatozoon contain?
|
- enzyme containing compartment
|
|
|
What does the head of the spermatozoon contain?
|
- nucleus with densely packed chromosomes
|
|
|
What does the neck of the spermatozoon contain?
|
- contains both centrioles from original spermatid
|
|
|
What does the middle piece of the spermatozoon contain?
|
- contains mitochondria: ATP generation for flagellum movement
|
|
|
Function of the spermatozoon tail
|
- Whip like organelle that moves the sperm
|
|
|
Seminiferous tubules
|
- organized into lobules
- spermatogenesis and spermiogenesis occur inside tubules (~9 weeks) **each segment at a different stage: tubule continuously producing spermatozoa |
|
|
Seminiferous tubule - cells
|
- Spermatogonia: earliest developmental stage, prior to mitosis division
- Spermatocytes: primary (after mitosis division), secondary (after 1st meiosis) - Spermatids: undergoing spermiogenesis, physical maturation into spermatozoa |
|
|
Seminiferous tubule - tissues
|
- Surrounded by delicate connective tissue capsule
- Areolar tissue fills spaces between tubules (also includes blood vessels and interstitial cells) - Interstitial cells secrete androgens |
|
|
What do androgens do, and where else besides interstitial cells are they produced?
|
- secondary sexual characteristics (puberty)
- zona reticularis of the adrenal gland |
|
|
Seminiferous tubule - layers
|
- Basal compartment: contains spermatogonia
- Luminal compartment: where meiosis and spermatogenesis occurs |
|
|
Activation of spermatozoa
|
- Spermatozoa released from the testes into the lumen are physically (but not functionally) mature. They are immobile and incapable of fertilizing an oocyte
- Other parts of the male reproductive system aid in functional maturing and activation |
|
|
Capacitation
|
- functional maturation of spermatozoa
- occurs in both male and female reproductive systems - Spermatozoa become mobile when in contact with seminal gland secretions - Spermatozoa become capable of fertilization when exposed to female reproductive tract |
|
|
Epididymis
|
- coiled tube bound to posterior border of each testis
- Line with pseudostratified columnar epithelium (with long stereocilia to increase surface area) - sperm undergo functional maturation here (beginning of capacitation) |
|
|
3 parts of the epididymis
|
- Head (receives spermatozoa from efferent ductules)
- Body (extends inferiorly) - Tail (transitions into ductus deferens) (drains) |
|
|
Ductus deferens (vas deferens)
|
- Passes through the inguinal canal
- transports and stores spermatozoa (in the ampulla = primary storage of sperm) |
|
|
Ejaculatory duct
|
- where ductus deferens and urethra meet
|
|
|
Male accessory glands
|
- Seminal glands (a.k.a seminal vesicles)
- Prostate gland - Bulbo-urethral glands |
|
|
Seminal glands
|
- Contribute ~60% of semen
- secretion ejected by smooth muscle lining the gland - Stimulates flagellum movement in spermatozoa (first step of movement) |
|
|
Prostate gland
|
- encircles proximal urethra
- contributes 20-30% of semen - Contains seminal plasmin (antibiotic for male tract) |
|
|
Bulbo-urethral gland
|
- Secrete alkaline mucus for lubrication and pH buffer
**The female reproductive system is usually acidic, this alkaline mucus neutralizes the female system |
|
|
Function of the Penis
|
- conducts urine to exterior and semen to female vagina during intercourse
|
|
|
Regions of the Penis
|
- Root: fixed portion attached to the body wall
- Body or Shaft: movable, tubular part - Glans or head: expanded end around urethral opening - Neck: between shaft and glans - Prepuce: foreskin - Smegma: waxy secretion |
|
|
Penis Layers (superficial to deep)
|
- Outer skin (dermis has smooth muscle continuous with dartos)
- underlying areolar tissue allows skin to move - elastic tissue (well vascularized tissue causing erection) ---in resting state, arterial branches contricted ---corpora cavernosa (dorsal side) ---corpus spongiosum (around penile urethra) |
|
|
3 phases of sexual arousal
|
- arousal
- emission - ejaculation |
|
|
Phases of sexual arousal - arousal details
|
- erotic thoughts or stimulation increase parasympathetic stimulation (breed and feed) through pelvic nerves
- release of nitric oxide causes erection by arterial dilation - bulbo-urethral glands secrete to lubricate penis tip |
|
|
Phases of sexual arousal - emission details
|
- formation and movement of semen internally
- sympathetic stimulation causes contractions of ductus deferens ampullae and other accessory glands |
|
|
Phases of sexual arousal - ejaculation details
|
- males orgasm (contraction of muscles)
- sympathetic stimulation - bulbocavernosus muscle (at the base) push semen toward external urethral orifice - ischiocavernosus muscles (along the sides) stiffen the erect penis |
|
|
Hormonal control of male reproductive system
|
- Hypothalamus: gonadotropin-releasing hormone (GnRH) stimulates release from the anterior pituitary
- The anterior pituitary releases: --Luteinizing hormone (LH): stimulates testosterone secretion from interstitial cells --Follicle-stimulating hormone (FSH): stimulates nurse cells which promotes spermatogenesis |
|
|
What are the testosterone effects?
|
- maintain libido and associated behaviors
- stimulation of bone and muscle growth - maintenance of secondary sexual characteristics - maintenance of accessory glands |
|
|
Functions of the female reproductive system
|
- Produce sex hormones
- Produce functional gametes - Protect and support developing embryo - Maintain growing fetus - Nourish newborn infant |
|
|
Female reproductive tract regions
|
- Uterine tubes (deliver oocyte or embryo to uterus)
- Uterus (site of embryonic and fetal development) - Vagina (site of sperm deposition) - Gonads (produce oocytes and hormones) - External genitalia (Clitoris: erectile tissue producing pleasurable sensations, Labia: contain glands to lubricate vagina) - Mammary glands (produce nourishing milk for infant) |
|
|
Three main functions of the ovaries
|
- Production of immature female gametes (oocytes)
- Secretion of female sex hormones (estrogens and progestins) - Secretion of inhibin (feedback to pituitary) **inhibin decreases pituitary gland secretion |
|
|
Layers of the ovaries
|
- Germinal epithelium (visceral peritoneum)
- Tunica albuginea (dense connective tissue) - Cortex (where oocytes are produced) - Medulla |
|
|
Function of uterine tube
|
- Conducts oocytes from ovary to uterus
- Infundibulum: expanded funnel near ovary |
|
|
Vesicouterine pouch
|
- Above the bladder
- pocket between uterus and posterior bladder wall |
|
|
Rectouterine pouch
|
- Behind, near bowel
- pocket between posterior uterus and anterior colon |
|
|
Vagina location
|
- extends from uterus base to exterior
|
|
|
Clitoris function
|
- pleasurable sensations
|
|
|
Labia function
|
- lubricate vagina
|
|
|
Connective tissues of the female reproductive system
|
- Suspensory ligament: lateral ovary to pelvic wall
- Ovarian ligament: ovary to uterine wall - Broad ligament: mesentery connecting ovaries, uterine tubes, and uterus to pelvic cavity wall - Mesovarium: mesentary supporting ovary |
|
|
Oogenesis
|
- Begins before birth, accelerates at puberty, ends at menopause
- Produces one functional ovum (compared to 4 haploid in male) - Also produces two or three polar bodies: nonfunctional, broken down as excess genetic material, non used, removed from body |
|
|
Steps of oogenesis
|
1) Mitosis gives primary oocyte (occurs before birth)
2) Meiosis I gives secondary oocyte (occurs during puberty) 3) Meiosis II gives one functional ovum (only complete after fertilization |
|
|
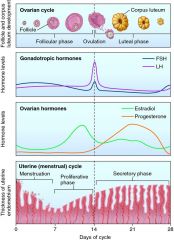
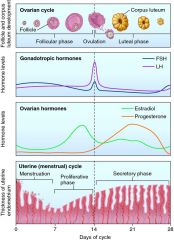
Function of the ovarian cycle
|
- Maturation of ovarian follicles
|
|
|
What is a follicle?
|
- Inactive primary oocyte + follicular cells
- Follicular cells are the support system for the egg, they provide protection and nutrition |
|
|
Stages of the ovarian cycle
|
- Formation of primary follicles
- Formation of secondary follicles - Formation of tertiary follicles - Ovulation - Formation of corpus luteum - Formation of corpus albicans |
|
|
Stages of the ovarian cycle - Formation of the primary follicle
|
- Follicular cells enlarge and form several layers
- Zona pellucida (clear layer) forms around oocyte |
|
|
Stages of the ovarian cycle - Formation of the secondary follicle
|
- Follicle wall thickens and follicular cells secrete fluid
|
|
|
Stages of the ovarian cycle - Formation of the tertiary follicle
|
- Mature follicle
- One secondary becomes a tertiary (day 10-14 of cycle) - Has antrum (fluid filled chamber) - Granulosa cells form corona radiata (protective layer) |
|
|
Stages of the ovarian cycle - Ovulation
|
- Release of the secondary oocyte by the tertiary follicle
- marks the end of the follicular phase and the start of the luteal phase |
|
|
Stages of the ovarian cycle - Formation of corpus luteum
|
- remaining granulosa cells secrete estrogen and progesterone
- Hormones stimulate the maturation of the uterine lining |
|
|
Stages of the ovarian cycle - Formation of corpus albicans
|
- Only occurs with out fertilization
- Degeneration of corpus luteum when not fertilized |
|
|
Uterine tube characteristics
|
- Extend from near ovaries to connect to uterus
- Lined with ciliated epithelium to move oocyte to uterus - Peristaltic contractions of smooth muscle in tube wall also propel oocyte |
|
|
Uterine components
|
- Fimbriae: fingerlike extensions that drape near the ovary
- Ampulla: muscular middle segment where fertilization occurs - Isthmus: short segment attached to uterine wall, where the tube narrows and attaches to the uterus |
|
|
Uterus function
|
- site of embryo implantation
- provides mechanical protection, nutritional support, and waste removal for embryo and fetus |
|
|
Layers of the uterus
|
- Perimetrium: thin tissue layer that protects the uterus
- Myometrium: muscle layer, produces contractions (oxytocin) - Endometrium: inner epithelial lining whose characteristics change monthly due to hormone changes (where embryo implants) |
|
|
Uterus - Lumen regions
|
- Uterine cavity: large superior cavity continuous with isthmus or uterine tube
- Internal os: opening connecting cavity to cervical canal - Cervical canal: constricted inferior passageway - External os: curving inferior tip within vagina |
|
|
Uterus regions
|
- Fundus: rounded superior portion connecting to uterine tubes
- Body: largest portion ending at cervical canal - Cervix: inferior portion surrounding cervical canal, projects into vagina |
|
|
Uterine vasculature
|
- Uterine artery
- arcuate arteries (encircle endometrium) - radial arteries (supply endometrium) - straight arteries (supply basilar zone) - spiral arteries (supply functional zone) **Straight and spiral influence menses **Functional: removed during menses, Basilar: stays the same |
|
|
Uterine (or menstrual) cycle
|
- Monthly changes in functional zone of uterus in response to sex hormone levels
- Averages 28 days in length - First cycle (menarche) begins ~11-12 years - Cycles continye until menopause ~45-55 years |
|
|
Phases of the uterine cycle
|
- Menses
- Proliferative phase - Secretory phase |
|
|
Phases of the uterine cycle - Menses
|
- Destruction of the functional zone
- caused by contricted spiral arteries reducing the flow of blood and nutrients (kill off) - Menstruation (process of endometrial sloughing) |
|
|
Phases of the uterine cycle - Proliferative phase
|
- Repair and regeneration of functional zone
- Increased estrogen levels from ovary |
|
|
Phases of the uterine cycle - Secretory phase
|
- Must be in this stage to support pregnancy
- Secretion of glycoproteins by uterine glands (supports embryo) - Effected by progestins and estrogen - Begins at ovulation and lasts until progesterone levels decrease (menses) |
|
|
Functions of the vagina
|
- Passageway for menstrual fluids
- Receives penis and temporarily holds spermatozoa - Forms inferior portion of the birth canal |
|
|
Female external genitalia regions
|
- Vulva or pudendum: area containing external genitalia
- Mons pubis: adipose tissue superficial to pubic symphysis - Prepuce: extensions of labia minora encircling clitoris - Clitoris: erectile tissue projection - Labia majora: prominent folds encircling labia minora - Labia minora: surround vestibule - Greater and lesser vestibular glands: mucous glands, analogous to bulbo-urethral glands in male |
|
|
Mammary gland functions
|
- Give nourishment from milk to infant
- Controlled mainly by hormones from reproductive system and placenta - Interaction of hormones causes milk production (Lactation) - Oxytocin = release, Prolactin = production |
|
|
Mammary gland location
|
- Directly over pectoralis major muscle
|
|
|
Mammary gland components
|
- Pectoral fat pad: subcutaneous fat deep to skin
- Suspensory ligaments: surround duct system and connect tubes - Lobes: organizational units consisting of multiple lobules with many secretory alveoli (secrete milk) stimulated by prolactin - Lactiferous duct: drains milk from lobe - Lactiferous sinus: milk storage - Nipple: conical projection containing 15-20 sinuses (stimulated by oxytocin) - Areola: skin around the nipple with many sebaceous glands |
|
|
What occurs with ovarian and uterine cycles do not operate synchronously?
|
- Infertility
|
|
|
Step 1 in hormonal regulation of reproductive cycles
|
- Release of gonadotropin releasing hormone (GnRH) from the hypothalamus
- Causes production and release of FSH - Causes production of LH |
|
|
Step 2 in hormonal regulation of reproductive cycles
|
- Follicular phase of the ovarian cycle
- Begins when FSH stimulates some secondary follicles to become tertiary - As tertiary develops. FSH levels decline due to inhibin release - Developed follicles secrete estrogens (estradiol) which inhibits LH secretion and stimulates endometrial growth and secretion |
|
|
Step 3 in hormonal regulation of reproductive cycles
|
- Luteal phase of ovarian cycle (begins after ovulation)
- GnRH and elevated estrogen levels stimulate LH release - Large increase in LH causes: completion of primary oocyte in meiosis I, rupture of follicular wall, ovulation, formation of corpus luteum - progesterone levels increase while estrogen decreases (if no pregnancy, progesterone levels drop and cycle repeats) |
|
|
|

