![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
402 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Is diagnosis for anxiety disorders the same or different in adults and children? |
Same |
|
|
|
Is separation anxiety of adults or just children? |
Both |
|
|
|
What is the prevalence of Social Anxiety in children? |
0%-4.6% |
|
|
|
Whats the prevalence for GAD in children |
0.16%-8.8% |
|
|
|
What's the prevalence of separation anxiety disorder in children? |
1.09%-20.2% |
Most prevalent |
|
|
What study showed the biggest prevalence of any childhood anxiety? |
Japan (combined parent and child report) 41.2% |
41.2% |
|
|
What study showed the minimum prevalence of any child anxiety? |
UK (parent and teacher report, only if certain) =3.19% |
3.19% |
|
|
2 reasons to worry about childhood anxiety |
Can have v serious consequences- depression, substance abuse, psychosis, underachievement and poor relationships Often not spotted until v serious |
|
|
|
Having first degree relatives (parents, children, siblings) with panic disorder makes people how many times more likely to have panic disorder |
5x |
|
|
|
Twin and adoption studies show panic disorder is what % heritable? |
30-40% |
|
|
|
Twin and adoption studies show GAD is what % heritable? |
31.6% |
|
|
|
Twin and adoption studies show phobias (including social anxiety) are what % heritable? |
20-40% |
|
|
|
Are estimates of Heritability of child anxiety consistent according to Gregory and Eley? Why? |
No, vary depending on:
The severity of the anxiety measured Type of anxiety being measured Who is reporting on the anxiety (e.g. self/parent) Age - heritability seems to increase with age 'Environmental factors are at least of equal importance' |
|
|
|
What two parenting styles are associated with child anxiety? |
Overcontrol/overprotection Harshness/lack of warmth |
|
|
|
How is overcontrol/overprotection related to child anxiety |
Reduced opportunity to: Develop coping skills Take risks and succeed and fail Learn to cope with feeling scared Can tell/teach children that: They can't cope on their own The worlds a dangerous place Scary things should be avoided |
|
|
|
Does parenting types cause anxiety |
No, relational, chicken/egg |
|
|
|
Evidence parents don't cause child anxiety |
Wood et als meta analysis found that parenting only accounted for 4% of the variance in children anxiety.
Many of the studies in this area suffer from 'shared method variance' (where one parent fills out a Questionnaire, their pattern if filling out suggests a correlation), which can result in overestimating the relationship between variables |
2 |
|
|
Evidence that parents cause child anxiety |
Some children are more sensitive to the effects of parenting, these children may respond strongly to certain parenting styles Parenting is extremely complicated and subtle. We probably haven't measured the right constructs yet. The field is reliant on self-report studies, which can underestimate relationships, in comparison to observational studies Parenting interventions work |
4 |
|
|
What did Kendalls 1994 RCT (randomised controlled trials) show |
CBT vs wait list 9-13yr olds Very encouraging results |
|
|
|
When comparing CBT with a passive control (wait list), whats the effect size? |
-0.76 (moderate to large) |
|
|
|
When comparing CBT with an active control (some treatment but not CBT), whats the effect size? |
-0.35 (small) |
|
|
|
Is it better to treat childhood anxiety for the specific disorder, or more generally? |
Specific |
|
|
|
Is it better to treat childhood anxiety one to one or in a group |
One to one |
|
|
|
Is CBT more effective for adolescents or younger children |
Adolescents |
|
|
|
In Walkup et al's test on treatment for child anxiety, what did they do? |
Compared CBT Sertraline (an SSRI drug) CBT and Sertraline A placebo |
|
|
|
What was Walkup et als findings on treatment for childhood anxiety |
Improvement: CBT = 59.7% Sertraline = 54.9% CBT and Sertraline = 80.7% Placebo pill = 23.7% |
|
|
|
2 Issues with Walkup et als findings on treatment for childhood anxiety |
Sertraline side effects: can increase suicidal thoughts but not suicide Lots of relapse and none of the treatment groups ended up significantly better than the others (even placebo) |
|
|
|
3 parts of the CBT approach for child anxiety |
Explain the fight-flight response Explain the role of avoidance Graded exposure |
|
|
|
What does explain the fight flight response entail |
The dinosaur and the caveman story |
|
|
|
What does explain the role of avoidance entail |
The story of the dragon mountain Villagers hear a dog in mountain- thunderstorms n fear, over years villagers too scared to go up mountain, but over time dog=lion=dragon Villagers start to starve, go up mountain, no dragon |
|
|
|
What does graded exposure entail |
"Break it down" Give tons of praise and little rewards whenever they practice Get the child to practice each step until comfortable with it. Then move up a step Fill in with lots of small steps Put what the child is capable of now, at the bottom Put the goal at the top |
|
|
|
Prevalence of social anxiety disorder in adults |
Around 12% |
|
|
|
Who's more likely to admit to social anxiety disorder |
Women |
|
|
|
What % of British children aged 5-15 met the diagnosis for social anxiety disorder |
32 |
|
|
|
Whens the onset of social anxiety disorder? |
Theoretically in adolescents, Often signs are there much younger |
|
|
|
What are 2 outcomes of social anxiety disorder? |
Risk of substance misuse Depression |
|
|
|
6 criteria for diagnosis of social anxiety disorder? |
Marked and persistent fear of 1 or more social or performance situation where there's exposure to unfamiliar people or possible scrutiny by others. Exposure evokes an immediate reaction. Fear is irrational Feared situation is avoided (interfering with normal life)- necessary Minimum duration is 6 months Not better explained by another diagnosis |
|
|
|
A meta-analysis of twins studies reveal a mean heritability of what for social anxiety disorder? |
0.65 |
|
|
|
2 early enviroments that are related to social anxiety disorder |
Early parenting styles - overprotection and modelling social avoidance Early shaming experiences |
|
|
|
How did social anxiety disorder used to be treated |
Social skills programmes |
|
|
|
How do new models differ from social skills programmes |
Propose social anxiety is not always a function of social skills deficits People often just believe they have deficits, causing them to act and think in ways that maintain the anxiety |
|
|
|
What is Clark and Wells' Model for social anxiety disorder |

|
|
|
|
What are the somatic symptoms of anxiety |
Sweating, trembling, butterflies in stomach |
|
|
|
What are the cognitive symptoms of social anxiety disorder |
Attentional biases, misinterpretation of ambiguous info |
|
|
|
Evidence of attentional biases in social anxiety disorder Only use hint if rly struggling |

Selective attention to socially threatening stimuli The dot probe design Socially anxious people have attention drawn to the angry face, click quicker when dot is congruent with angry face Studies using faces (not words) have shown tentative support for both vigilance and avoidance (if photo left up a little longer) Little evidence for causal role (this doesn't prove it causes social anxiety) |
Dot probe |
|
|
What tasks shows processing self as a social object |
Perspective Taking Rating task |
|
|
|
What is done in the perspective taking rating task |
Picturing a social situation that was potentially anxiety provoking Asked if looking at yourself through someone elses eyes (observer perspective) or own eyes (field perspective) |
Not the results |
|
|
Which perspective shows what for the perspective taking rating task |
Looking at self through someone elses eyes = observer perspective = most common in people with social anxiety disorder. Have to makeup what the audience saw, no real info so use own judgement Own eyes = field perspective = less common in socially anxious people |
|
|
|
How can safety behaviours make things worse? |
Make the person's behaviour appear unnatural Stops them finding out that the feared consequence wasn't going to happen anyway Distracts the person, meaning they don't give the situation their full attention |
3 things |
|
|
Before the social interaction (in anxious people) is called what? |
Pre-mortem |
|
|
|
Whats included in pre-mortem social interaction |
Social phobics review the likely run of events Recollection of past failures Can lead to avoidance |
|
|
|
What's included in post-mortem social interactions (post-event processing) |
Makes matters work (increase anxiety) Intrusive thoughts Distorted memories |
|
|
|
4 things CBT for social anxiety does |
Identify and modify assumptions ('im boring', evidence of not being boring) Identify and modify safety behaviours (stop them saying nothing, going on phone, rehearsing what to say) Behavioural experiments (test out whether predicted catastrophes come true e.g. see if people laugh/walk away/talk about them after an interaction, not what happens) Dealing with the pre and post-mortem (pls dont do that, upbeat music instead of worry, prevent rumination go for a run) |
|
|
|
What did Stewart and Chamberless' 2009 meta-analysis do and show for the efficacy of CBT for social anxiety |
Pooled data from 11 studies measuring pre-post treatment change Large effect of CBT on social anxiety symptoms (against nothing/placebo) |
|
|
|
What is the efficacy of CBT for social anxiety for children |
Much less evidence for what works vs adults CBT probably fairly good, but needs to be focussed on social anxiety rather than on anxiety in general |
|
|
|
DSM5 criteria for GAD |
Excessive anxiety and worry more days than not Difficult to control 3 or more of •Restlessness •Easily fatigued •Difficulty concentrating •Irritability •Muscle tension •Sleep disturbance Clinical significant impairment in social/occupational functioning |
|
|
|
4 DSM GAD exclusion criteria |
Focus of the anxiety and worry is confined to another axis 1 disorder e.g. spiders (specific phobia) Disturbance result of medical condition Disturbance result of effects of a substance Worry occurs exclusively during a mood disorder, pervasive disorder or a psychotic disorder |
|
|
|
Lifetime comorbidity of GAD |
81% |
If diagnosed with GAD, what % meet criteria for another diagnosis |
|
|
What is a long term effect of anxiety |
Impact on cardiovascular health |
|
|
|
CBT is effect for what % people |
Approx 50% |
|
|
|
3 cognitive models for GAD |
Cognitive model of pathological worry Intolerance of uncertainty The cognitice avoidance theory of worry |
|
|
|
Who created the cognitive model of pathological sorry |
Hirsch and Matthews |
|
|
|
2 key processes in the cognitive model of pathological worry |
Cognitive biases Attentional control |
|
|
|
2 cognitive biases in the cognitive model of pathological worry |
Attentional bias Interpretation bias |
Just names |
|
|
What is pathological worry |
Clinical type of worry shown by those with anxiety Not day to day worry |
|
|
|
What is the attentional bias |
Selective attention to threat at the cost of attending to positive or benign info |
|
|
|
What is the interpretation bias |
Tending to make more threatening/negative interpretations of ambiguous situations, leads into seeing the world as a threatening place |
|
|
|
What does the cognitive model of pathological worry look like |

|
|
|
|
Who created the intolerance of uncertainty model of GAD n when |
Dugas Freeston And Ladouceur 1997 |
|
|
|
3 elements of the intolerance of uncertainty model of GAD |
Positive beliefs about worry Negative problem orientation Cognitive avoidance |
|
|
|
What does the intolerance of uncertainty model of GAD look like |
|
|
|
|
The 3 premises of the cognitive avoidance theory of worry |
i) Worry focuses on possible but non existent future bad things ii) because the perceived danger doesn't exist yet, no effective fight/flight response iii) humans are left with only mental attempts to solve the problems |
|
|
|
Cognitive avoidance in IU model for GAD |
Emotional arousal (often implicit) Suppress negative intrusive thoughts |
|
|
|
3 things avoided in the cog avoidance theory of worry |
Distressing negative imagery associated with more distress in short term Avoid physiological arousal Avoid thinking about more distressing topics |
|
|
|
Who created the cognitive avoidance theory of worry n when |
Borkovec et al 2004 |
|
|
|
What does the avoidence model of GAD look like |

|
|
|
|
In the NICE guidelines, what step is CBT/drug treatment suggested for GAD |
3 |
|
|
|
How many sessions for CBT targeting IU |
12-16 |
|
|
|
7 parts of IU- based CBT treatment |
Psychoeducation Worry awareness training Coping with uncertainty Re-evaluating beliefs about the usefulness of worry Improving poor problem orientation and problem solving ability Processing core fears through imaginal exposure Relapse prevention |
|
|
|
How to increase tolerance to uncertainty |
Behavioural experiments to seek out uncertainty |
|
|
|
4 common diagnoses after trauma |
PTSD/ C-PTSD (complex-PTSD) EUPD = emotionally unstable personality disorder Psychosis Bipolar disorder |
|
|
|
What is PTSD |
Type of anxiety disorder may develop after being involved in or witnessing traumatic events |
|
|
|
What is Trauma |
An inescapably stressful event that overwhelms people's existing coping mechanisms Shatters a persons beliefs about self, world and other people |
|
|
|
4 main classifications of common symptoms in PTSD |
Re-experiencing Alertness/feeling on edge Avoidance of feelings or memory Negative beliefs |
|
|
|
5 re-experiencing symptoms |
Flashbacks Nightmares Intrusive thoughts or images Intense distress following real or symbolic reminders of the trauma Physical sensations (pain, trembling, nausea) |
|
|
|
Difference between flashback and intrusive thoughts/images |
Flashback = vivid experience, relive aspects of event, feel as if its happening rn Intrusive image = less re-experiencing |
|
|
|
What is extreme alertness sometimes called |
Hypervigilance |
|
|
|
Criterion A of PTSD in DSM5 |
Exposure to trauma |
|
|
|
Criterion B of PTSD in the DSM5 |
Intrusion symptoms |
|
|
|
Criterion C of PTSD in DSM5 |
Avoidance symptoms |
|
|
|
Criterion D of PTSD in DSM5 |
Negative alterations in cognition and mood |
|
|
|
Criterion E of PTSD in DSM5 |
Alterations in arousal and reactivity |
|
|
|
Criteria to meet for PTSD in the DSM5 |
A 1 or more symptoms from B and from C 3 or more from D and from E F-H |
|
|
|
Average of traumatic events per person |
3.2 |
|
|
|
Where is Complex PTSD diagnoses |
ICD 11 |
What manual |
|
|
How is CPTSD classified differently to PTSD |
Exposure to event or series of events |
|
|
|
Difference in symptoms of PTSD and CPTSD |
CPTSD has core members of PTSD but with: Affect dysregulation Negative self-concept Interpersonal difficulties |
|
|
|
When is CPTSD more likely |
Early developmental trauma Trauma lasted for a long time Escape or rescue were unlikely/impossible Multiple traumas (persistent) Trauma in close interpersonal relationships |
|
|
|
What is the cognitive model of PTSD |
Individuals are remembering trauma in a way that poses current threat in the here and now |
|
|
|
Parts of the brain involved in PTSD in the cognitive model |
Amygdala - threat system (F&F) Hippocampus- store and remember info |
|
|
|
How does traumatic event effect hippocampus |
Hippocampus doesn't work very well, often unable to put a time stamp on the memory |
|
|
|
What is trauma memory like |
Fragmented and not organised Recalled involuntarily Triggered by reminders Not time tagged (trauma happens here n now) It is frozen in time (not updated as you learn new info) |
|
|
|
3 systems from the compassionate minds approach |
Drive, achieving, wanting, pursuing, goal-focused Soothe, safeness/kindness, recharge and unwind Threat - to keep us safe |
|
|
|
How does the compassionate mind systems change in traumatic mind |
Trauma increases threat After the trauma Matching triggers activates threat, so in threat mode most of the time Perceived sense of current threat, feel as though it is in the here and now |
|
|
|
How does the window of tolerance change for people who have experienced trauma |
Reduces it |
|
|
|
Three areas outside of the window of tolerance |
Hyperarousal - anxious/angry/F&F Dysregulation - Hypoarousal - zoned out/numb/tired extreme = dissociation, completely detatched, extreme numbness |
|
|
|
How is dissociation helpful |
Protects us from feeling the overwhelming emotions linked to the trauma |
|
|
|
Different types of dissociation |
Environment Body Flashbacks |
|
|
|
4 types of psychological therapy for PTSD |
Cognitive processing therapy Cognitive therapy for PTSD Narrative exposure therapy Prolonged exposure therapy |
|
|
|
What is EMDR |
Eye movement desensitization and reprocessing |
|
|
|
Who was EMDR made for |
Veterans |
Stopped being suggested for them |
|
|
Who is EMDR suggested for? |
Adults with a diagnosis of PTSD for non-combat related trauma |
|
|
|
8 factors suggesting a clients readiness for therapy |
Current safety factors (social circumstances - abuse, enviroment- housing) Dissociation - not a reason not to offer, but needs to be assessed (wont go anywhere) Self-harm and suicidal thoughts Therapeutic relationship Substances - not excluded, but knowledge Medication Avoidance |
|
|
|
How does the cog model of PSTD (treatment included) look like? |

|
|
|
|
Step 1 in Ehlers and Clark 2000 therapy component to trauma |
Thorough client history and treatment planning |
|
|
|
3 goals in Ehlers and Clark 2000 therapy for trauma |
Reduce re-experiencing symptoms (trigger discrimination) Modify -ve appraisals of the trauma and its consequences (CBT) Drop maintaining behaviours (behavioural experiments) |
|
|
|
Last stage in Ehlers and Clarks 2000 therapy components treatment for trauma |
Reclaiming life |
|
|
|
8 stages in EMDR |
1:client history and treatment planning 2:preparation 3: assessment (of specific target memories), worst moment identify, SUD 4: desensitization (bilateral stimulation) 5: installation (positive cognition) 6: body scan (for tenseness) 7: closure 8: re-evaluation |
|
|
|
What does SUDs mean in EMDR |
Subjective units of distress (1-10) |
|
|
|
What is TF-CBT |
Trauma focused CBT |
|
|
|
How long should TF-CBT and EMDR be offered for |
At least 8-12 weekly sessions (usually more for C-PTSD) for 90 mins |
|
|
|
Why is readiness for trauma-focussed work important? |
Therapy can be traumatic |
|
|
|
DSM5 9 symptoms of depression |
Depressed mood Reduced interest or pleasure in activities (anhedonia) Psychomotor retardation Fatigue or loss of energy Feelings of worthlessness or excessive or inappropriate guilt Diminished ability to think or concentrate or indecisiveness Recurrent thoughts of death, recurrent suicidal ideation with or without a specific plan, or a suicide attempt |
|
|
|
Criteria for depression |
5 or more symtpoms during the same 2 week period No history of mania or hypomania (part of bipolar) Not SAD or Dysthymia (chronic slightly lower level of depression over 2yrs, can lead to dep) |
|
|
|
Lifetime prevalence of depression |
20% |
|
|
|
How many people of all ages suffer from depression |
At least 350 million |
|
|
|
Relationship between bereavement and depression |
Bereavement can include/lead to depression - not a clear cut difference |
|
|
|
Whats the gender ratio of depression? |
2:1 more females than males diagnosed |
|
|
|
Relationship between suicide and depression |
Depression is the leading cause of suicide |
|
|
|
Gender ratio for suicide from depression |
2:1 more males |
|
|
|
For what % of depressed people is dep a one-off |
50% |
|
|
|
Is the 2nd episode of depression another 1 off |
No, greatly increases risk of further recurrence |
|
|
|
For people who's depression is recurrent, whats the average amount of lifetime major depressive episodes of 20 weeks duration each |
4 |
|
|
|
If an individual has 3 or more episodes of depression, whats the likelihood for another episode in the next 12 months |
70-80% |
|
|
|
Whats the mean age at onset for depression |
26 years |
|
|
|
Whats the modal age for depression |
13-15 years |
|
|
|
Whats the monoamine hypothesis for depression |
Low levels of serotonin (5-HT) and noradrenaline (NA) produce depressed mood |
Which 2 neurotransmitters |
|
|
What is age of onset of depression a predictor of |
Persistence and severity |
|
|
|
Name of first drug found to treat depressive symptoms |
Isoniazid (for TB) |
|
|
|
How do antidep drugs work |
Increase synaptic levels of 5-HT and NA |
|
|
|
How many prescriptions for antidepd in the UK in 2016 |
64.7 mil |
|
|
|
What does a meta-analysis show on the causal relationship between monoamine depletion and depressed mood |
Monoamine depletion does not decrease mood in healthy humans |
|
|
|
3 problems with antidepressant theory |
Timescale problem Specificity problem The myth of reserpine-induced depression |
Just names |
|
|
Whats the timescale problem with antidepressant theory |
Once you start giving antidepressants, monoamine levels normalise within matter of days but mood doesn't lift until weeks after |
|
|
|
What's the specificity problem with antidepressant theory |
Using monoamines don't just help depression but other disorders |
|
|
|
Who created the myth of reserpine-induced depression |
Baumeister |
|
|
|
Whats the name of the big trial examining the effects of antidepressants? |
STAR*D trial |
|
|
|
Whats the cumulative response rate for depression in the STAR*D trial |
47% over 1 year |
|
|
|
Are antidepressants better than placebo for severe depression |
Possibly Best estimate 50-60%₩ |
|
|
|
Are antidepressants better than placebo for mild/moderate depression |
No |
|
|
|
Are antidepressants popular with patients? |
No |
|
|
|
What are antidepressants linked to in young people |
Violent crime and suicide risk |
|
|
|
When you come off antidepressants, does the risk for recurrence of episodes decrease? |
No Still 60-70% for people with 3 episodes and 90% for people with 5 |
|
|
|
2 influential models of depression |
Learned helplessness (Seligman et al) Clinical cognitive model (Beck et al 1979) |
|
|
|
3 parts of learned helplessness model to depression |
Uncontrollable aversive events Sense of helplessness Depression |
|
|
|
Seligmans experiment to learned helplessness |
Exposure to uncontrollable shock in one experiment Led to helplessness in subsequent experiment (would not find way to escape shock, would just lie down and accept random shocks) Unexposured dogs jumped over easily |
|
|
|
Experiment of learned helplessness in humans |
Hiroto 1964 - same experiment as shocking dogs but with aversive tone in humans |
|
|
|
Real life evidence of learned helplessness |
Whitehall studies: British civil servants Inverse association between job status and risk of depression Within same pay level and status, degree of control predicted likelihood of depression People with no input on job structured more likely to get depression |
|
|
|
Motivational symptoms of learned helplessness |
Lower response initiation and sensitivity to reinforcement |
|
|
|
Whats the cognitive symptom of learned helplessness |
Dampened ability to learn that responding produces reinforcement |
|
|
|
When depressed people listen to positive music, what do they report feeling and what does this show |
Both positive and negative affect Shows they are different and the symptoms may be different |
|
|
|
Evidence suggesting there are 2 distinct capacities for pleasure |
When would you like to receive a kiss from favourite celebrity? Most people say 3 days Recieve pleasure from looking to things and enjoying things in the moment (consummation) |
|
|
|
Method of 'the risks of playing it safe' by Rawal, Collishaw, Thapar and Rice 2013 |
Phase 1: choose colour to find hidden token (ratio between colour varies - 9:1,8:2,7:3,6:4) Phase 2: reward-sensitivity (how many points willing to bet at high reward probability) |
|
|
|
Results of 'the risks of playing it safe' by Rawal, Collishaw, Thapar and Rice 2013 |
Reduced reward-sensitivity and adjustment in depressed |
|
|
|
Reduced reward-sensitivity predicts what |
Depression onset after a year |
|
|
|
What does increasing reward-sensitivity do |
Reduce depression |
|
|
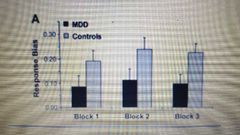
What does this show? |
Depressed individuals don't work out which response is more rewarding (no response bias to rewarding behaviour) |
|
|

What does this show |
Stress in healthy ppts induced the same deficit in response bias (loss of reward sensitivity) as depressed ppts |
|
|
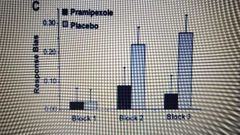
What does this show? |
Drug blocking signalling of dopamine in the brain induces fail of response bias |
|
|
|
What shows mere exposure to uncontrollability is not sufficient to render humans helpless |
Life stress is not necessarily associated with onset of depression |
|
|
|
What is helplessness dependent on |
Attributions/inferences people make about events |
|
|
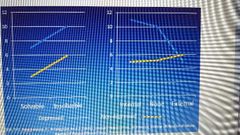
What does this show |
By telling people failure to do with external issues, you eliminate the effect of uncontrolability on helplessness |
|
|
|
Attribution of failure and success in depressed individuals |
Failure is internal, success is external |
|
|
|
What does attribution style predict |
Severity and onset of depression |
|
|
|
How is attribution style different between males and females |
Women have more depressive attribution style |
|
|
|
Who's work superseded Seligmans on depression |
Beck |
|
|
|
Becks clinical cognitive model of depression |
Early adverse events give rise to depressive schemas (e.g. dysfunctional attitudes) which biases cognitions leading to depressive symptoms which feeds back into depressive schemas |
|
|
|
CBT vs antidepressants improvement %s |
78.8% vs 22.7% |
|
|
|
CBT vs antidepressants % return treatment |
16% vs 68% |
|
|
|
Cognitive changes differences between antidepressants and CBT |
No difs |
|
|
|
Is CBT more effective than other psychological treatments |
No, reduces -ve thinking to a similar extent |
|
|
|
Have differences been found in dysfunctional attitudes between recovered depressed subjects and controls? |
No |
|
|
|
Example of context-dependent learning |
Diving experiment Godden and Baddeley 1975 |
|
|
|
How does context-dependent learning relate to depression and what theory does it relate to |
Mood acts as the context, acting as a reminder of the context-dependent state for patterns of processing Differential Activation Hypothesis |
|
|
|
Difference in affective vs devaluative adjectives for when feeling low in never depressed vs former depressed |

|
|
|
|
Diagnosis of OCD |
Obsessions or compulsions that Cause distress Are time consuming and/or Interfere markedly with daily life |
|
|
|
What % of the population does OCD affect |
1-2% |
|
|
|
What are intrusive thoughts |
Involuntary thoughts Unpleasant content Are ego-dystonic (inconsistent with own values and ideal self) |
|
|
|
Opposite of ego-dystonic |
Ego-syntonic |
|
|
|
3 types of intrusive thoughts |
Verbal Images Urges |
|
|
|
Operant conditioning theory of OCD |
Compulsions are negatively reinforced |
|
|
|
Evidence for the 2 factor theory for OCD |
Foe et al 32 OCD patients in 3 conditions Exposure to feared object/event - reduced anxiety (classical conditioning) Disengaging from compulsions - reduced anxiety Exposure and disengagement reduced anxiety to a greater degree than either alone |
|
|
|
2 theories for how exposure based therapies work |
Emotional processing theory (EPT) Inhibitory Learning Theory (ILT) |
|
|
|
What is the emotional processing theory for how exposure-based therapies work? |
Prolonged exposure of triggers with response prevention leads to habituation so old fear memory gradually decreases. New non-fear memory integrates with and then replaces the old fear memory |
|
|
|
Evidence against the EPT |
The degree of habituation is generally not correlated with exposure treatment outcomes Suggests habituation may not be primary mechanism through which exposure therapies have their effect. Also relapse following exposure and response prevention is common |
|
|
|
Whats the inhibitory learning theory to how exposure-based therapies work for OCD |
New non-fear memory does not replace or modify the old fesr memory, stored as a separate memory. New mem context dependent- cues in learning, thus homework outside of sessions needed |
|
|
|
3 Evidence supporting the inhibitory learning theory to OCD |
There isn't a string association between the degree of habituation and exposure based therapy outcomes
Exposure and response prevention appear to be more effective when tasks are performed in a variety of contexts
Relapse rates following exposure based therapy for OCD are high |
|
|
|
3 limitations with behaciour therapy |
People refuse ERP (exposure response prevention) >16% People drop out 16% People don't fully engage in ERP tasks (>75% of tasks need to ve completed for the best therapy outcomes) |
|
|
|
Whats the 2 main points of the cognitive model of OCD |
Everyone has intrusive thoughts, so they are not the problem OCD is caused and maintained by what people believe about their intrusive thoughts |
|
|
|
4 components of the cognitive formulation of OCD |
Intrusive thought IT ⬇️ Beliefs about IT⬅️ ⬇️ Anxiety ⬇️ Compulsive behaviour ⤴️ |
|
|
|
6 cognitive factors (beliefs) in OCD |
Importance of thought control Importance of thoughts Intolerance of uncertainty Overestimation of threat Personal responsibility for causing/preventing harm Perfectionism |
|
|
|
What did a factor analysis show the 3 factors were that replaced the 6 OCD beliefs |
Importance of thought control/thoughts Intolerance of uncertainty/perfectionism Personal responsibility for causing or preventing harm/overestimation of threat |
|
|
|
Which cog factors do OCD ppl score significant higher than ppl with other anxiety conditions |
Importance of thought control/importance of thoughts Personal responsibility for causing or preventing harm/overestimation of threat |
|
|
|
Evidence of causal influence of responsibility beliefs and OCD |
Decreasing responsibility - decreased urge to check in people with OCD Increased responsibility leads to greater checking behaviour in people with OCD |
|
|
|
Evidence of causal role of beliefs about the importance of thoughts control and OCD |
Manipulating beliefs about importance of thought control led to more intrusion and greater distress |
|
|
|
4 limitations of the cognitive model to OCD |
Limited research that beliefs about intrusive thoughts play a causal role in OCD (beliefs may be secondary). Cognitive therapy for OCD may be no more effective or acceptable than exposure based therapies (not clear what the cog model adds). Developmental origins of OCD-related beliefs not well understood. Most people with OCD are concerned aboutsome of their intrusive thoughts but not all. |
|
|
|
What are the 2 primary emotions triggered in OCD apart from anxiety |
Disgust Shame |
|
|
|
4 Problems with habituation for OCD |
Degree of habituation doesn't predict treatment outcomes for exposure-based therapies. Some ppl don't experience a fall in levels of anxiety (fear of feeling anxious) Anxiety isn't always troubling emotion in OCD - disgust/shame = primary emotion triggered Info learnt may be more important than habituation e.g. anxiety isn't dangerous, person can cope with high levels of anxiety and the feared outcome doesn't occur |
|
|
|
3 parts of cognitive therapy for OCD |
Identify beliefs about intrusive thoughts for the person Develop a shared formulation with the person (chain of events diagram) Develop behavioural experiments to test the accuracy of beliefs (prediction and actual outcome discussed) |
|
|
|
Who conducted a RCT comparing ERP with CT for OCD |
Whittall et al |
|
|
|
What does Whittall et al show for OCD therapy? |
No significant differences between ERP and CT Both over 1/2 recovered post-therapy |
|
|
|
Who meta-analysed RCTs comparing ERP to CT for OCD |
Ougrin 2011 |
|
|
|
What did Ougrin's meta analysis for OCD treatment show |
No significant dif between ERP and CT at post-therapy or at follow up |
|
|
|
What has been suggested to improve effectiveness of therapies |
Mindfulness |
|
|
|
How does mindfulness based interventions relate to depression |
Reduce depressive relapse Reduce depressive symptom severity |
|
|
|
A mindful based ERP approach might help to improve engagement by... (3) |
Tolerate feelings of anxiety during ERP tasks and thereby not avoid or disengage with the task Lessen conviction in beliefs about the importance of intrusive thoughts Consciously choose to disengage from compulsions, rather than doing this on automatic pilot |
|
|
|
Name of pilot RCT for mindfulness-based ERP for OCD |
BeMind |
|
|
|
Findings of BeMind |
No difs between reductions in OCD symptoms over time for ERP and ERP with mindfulness |
|
|
|
What did Schaie 1985 find on cog abilities |
In the absence of specific disease, cognitive abilities change v little before the age of 75 Fluid ability (STM capacity and rapid processing of info) and some aspects of language deteriorate around this age Crystallised intelligence (gen knowledge, lang skills, problem solving skills) unimpaired in majority |
|
|
|
3 age related diseases |
Stroke Parkinson's disease Dementia |
|
|
|
What's the main cause of hospitalisation |
Dementia 7/10 acute beds occupied by frail elderly |
|
|
|
What % of those with dementia are 65 to 69 |
10 |
|
|
|
What % of those with dementia are 80 to 84 |
25 |
|
|
|
What is the lifetime prevalence of dementia |
26% |
What % of people will get dementia at some point |
|
|
What is the gender difference in dementia |
65% women |
|
|
|
Is dementia a major or minor neurocognitive disorder |
Major |
|
|
|
Difference between dementia and delirium |
Delirium = begin over a few hours or a few days |
|
|
|
In dementia, how much does cog perfomance neee to drop by |
2 SDs or 3rd percentile |
|
|
|
Dementia may be due to what 4 things |
Alzheimer's disease Vascular disease Traumatic brain injury Lewy body disease |
|
|
|
Difference between primary and secondary dementias |
Primary = dementia is main symptom/condition experienced Secondary = dementia emerges late |
|
|
|
6 types of primary dementias |
Vascular (multi-infarct) Alzheimer's Mixed Dementia with lewy body Fronto-temporal dementia Prion-relater dementia |
|
|
|
4 types of secondary dementias |
Parkinson's HIV Huntingtins Chorea Down's syndrome |
|
|
|
When can alzheimers disorder diagnosis be definite? |
Autopsy |
|
|
|
3 types of tests for detecting Alzheimer's and the age used |
Cerebrospinal fluid (CSF) test - 20yrs before symptom onset Brain imaging tests (PET, MRI) - 15yrs Memory tests - 10 years |
|
|
|
Is age a determinant in quality of life for a person with AD |
No |
Banjeree et al |
|
|
What factor did Clare et al find correlated with QOL for dementia patients |
Psychological characteristics and psychological health E.g. loneliness, optimism |
|
|
|
What does the brain wasting away show |
Brain atrophy |
|
|
|
Where is there much brain atrophy in Alzheimer's patients? |
Hippocampus |
|
|
|
What is braak pathology |
Senile plaques (SPs) (beta-amyloid protein+) Neurofibrillary tangles (NFTs) tau protein |
|
|
|
What are neurofibrillary tangles (NFTs) |
Abnormal form of TAU protein in thw cytoplasms and nerve endings of neurons in a number of different brain regions These paired hilacal filaments = pathology |
|
|
|
Are neurofibrillary tangles specific to alzheimers? |
No |
|
|
|
What is the spread of neurofibrillary tangles? |
Hippocampus - neocortex - subcortex |
|
|
|
What is the presence of neurofibrillary tangles association with? |
Progressive degeneration of the neuron, reduced efficacy of function, and eventually neuronal cell death Number of NFTs correlates with clinical severity of the dementia |
4 things |
|
|
What are senile Plaques (SPs) |
Complex structures made up of extracellular beta - AMLOID - a cell membrane protein - occuring in the spaces between neurons |
|
|
|
What are the two earliest and most consistent sites of A beta deposition? |
Posterior parietal cortex Medial prefrontal cortex |
|
|
|
Ultimately how is Abeta distributed across brain in Alzheimer's |
Diffusely |
|
|
|
Can beta amyloid or tau be large in normal brains |
Beta amyloid, tau causes the dementia |
|
|
|
What system shows the most significant neurochemical changes from Alzheimer's? |
Cholinergic system |
|
|
|
What is the cholinergic system related to |
Memory and learning |
|
|
|
What is the cholinergic system related to |
Memory and learning |
|
|
|
How does alzheimers change the cholinergic system (2) |
Reduced cortical ChAT activity (which converts choline into Acetylcholine) correlates with clinical dementia rating Chronic subcortical cell loss of cholinergic neurons in the basal forebrain bundle also obserced in AD patients |
|
|
|
What % of AD cases have no obvious family history |
95% |
|
|
|
3 chromosomes that have links with dementia |
21, 19 and 14+1 |
|
|
|
How does chromosome 21 link to dementia |
Amyloid protein overexpression Increased risk of downs syndrome in families with AD Increased risk if AD in families with DS Gene coding for beta amyloid protein is located on Chr 21 Link to over-expression of beta amyloid in the brain |
|
|
|
How does chromosome 14+1 link to dementia |
Presenilin protein mutations. Observed in familial cases of AD. PSEN genes alter specificity of gamma secretase enzyme that cuts amyloid precursor protein abnormally, resulting in Ab 42 over-expression and aggregation. Implicated in transportation failures leading to build up of gamma-APP intra and extra cellularly. |
|
|
|
How does chromosome 19 link to dementia |
E proteun regulating cholesterol levels in the brain Allelic variations = e2/e2, e2/e3, e2/e4, e3/e3, e3/e4, e4/e4 60% of population have e3/e3 Having e3/e4 or e4/e4 = increased risk |
|
|
|
Which is the biggest genetic vulnerability factor in all populations |
Chromosome 19 e3/e4 or e4/e4 As all pops have an expression of some sorts |
|
|
|
What did Fratiglioni et al find to increase risk of dementia? |
Both being single and living alone almost doubled the risk The lower the frequency of social contact the higher the risk Having children with frequent but unsatisfying contact |
|
|
|
What did Amieva et al show to be a predictive risk factor of dementia |
Poor quality of relationships |
|
|
|
What are the 2 personality characteristics linked to increased risk of dementia |
High neuroticism Low concientiousness |
|
|
|
In person with AD, higher cognitive reserve is associated with what |
Fewer behavioural consequences - reduced clinical severity |
|
|
|
How can cognitive reserve be increased |
Education |
|
|
|
What effect does education have on dementia? |
Does not protect the development of dementia but it offers functional protection and reduces the expression of dementia |
|
|
|
? Is to correct for the deficiency in the cholinergic neurotransmitter system |
Cholinergic augmentation |
|
|
|
What is used to inhibit the action of acetylcholinesterase (AChE) |
Cholinesterate inhibitors (ChEIs) |
|
|
|
What is used to inhibit the action of acetylcholinesterase (AChE) |
Cholinesterate inhibitors (ChEIs) |
|
|
|
How could immunisation be possible for dementia |
Genetic modification to produce AD as shown in mice. Challenged by a vaccine against beta amyloid. If vaccinatrd early, did not develop AD and showed reduced cog deficits. |
|
|
|
How successful is vaccination agaibst AD in humans |
Minimal success E.g. bapineuzumab trial = some evidence of reduced amyloid burden but no evidence for clinical change |
|
|
|
What is PARO for dementia |
A robot seal able to learn and recognise things that comforts people in later stages of dementia |
|
|
|
What changes happen in the brain from 11-13 yrs |
Pruning of prefrontal cortex ('thinking brain') Loss of up to 40% of neural branches to allow for more efficient connection Higher order thinking Limbic system develops earlier and faster Control of functions (emotion, memory, reward seeking) thinking and reacting brain |
|
|
|
What age does the brain reach full maturity |
25 years |
|
|
|
A theory of social contexts that affect the individual |
Ecological systems theory by Bronfenbrenner |
|
|
|
Cultural influence example for adolescents and mental health |
Youth in India When households engaged in practices that favoured men = females worse MH, males better Family violence and restrictions to independence associated with MH problems Behaviours breaking gender norms = MH probs |
|
|
|
What % of adolescents live in low and middle income countries |
90% |
|
|
|
What is the leading cause of death for adolescent females |
Self-harm |
|
|
|
Most common 3 mental disorder in adolescents world wide in order |
Anxiety Any disruptive behaviour disorder Any depressive disorder |
|
|
|
What % of mental disorders onset prior to age 25 years |
70% |
|
|
|
What is the prevalence of any mental disorder in adolescents worldwide |
13.4% |
|
|
|
What mental disorder is the most disabling? |
Depression |
|
|
|
What is an example for understanding adolescent MH in context? |
Qualitative study of daily stressors and coping among adolescents in Delhi and Goa: part of the PRIDE adolescent MH programme |
Schools in india |
|
|
What are the 3 research qs for the PRIDE research programme |
What are the common stressors affecting school-going adolescents? How do adolescents react to and cope with these stressors? What are the implications for a guided self-help intervention? |
|
|
|
What is the setting of New Delhi for the PRIDE research programme? |
India's capital and 1 of 11 districts in national Capital Territory of Delhi Second largest city, one of the most polluted places in world |
|
|
|
What is the setting of Goa for the PRIDE research programme? |
Indias smallest and richest state |
|
|
|
What term is used for 'stress' in India? |
Tension |
|
|
|
What stress what a cross cutting theme in both Goa and Gelhi |
Academic |
|
|
|
What was an important protective function for children and Goa and Delhi |
Positive peer relationships |
|
|
|
What % of adolescents with emotional disorders remain symptomatic after 3 years |
30% |
|
|
|
What % of adolescents shore recurrence of emotuonal disorders within 12 yrs |
60% |
|
|
|
What % of 16-24 year olds who commit suicide are clinically anxious or depressed at time of death |
60% |
|
|
|
Subthreshold symptoms affect up to 1/? Of adolescents |
1/3 |
Symptoms not severe enough for diagnosis |
|
|
What did Klasen and Crombags 2013 broad systematic review of RCTs testing child and adolescent mental health interventions find |
There were no treatment studies from LMICs that focused specifically on adolescents Research instead focused on mental health promotion and at risk/traumatised samples in conflict affected areas |
|
|
|
2 ways to go forward with psychological interventions in high income countries |
Overcome access barriers on global scale Optimise effectiveness (beyond 40-60% response rate) |
|
|
|
What is the elements approach to new intervention of MH in adolescents |
Looking at all treatments in world evaluated and distilling them into constituent therapeutic activities, techniques or strategies Look at which essential Grade in importance/effectiveness And for what age - 'relevance mapping' |
|
|
|
What is the transdiagnostic approach to new intervention of MH in adolescents |
Use a core set of elements to address a range of MD, given shared risk factors, common comorbidity and overlap in disorder-specific protocols Apply treatment to different disorders more generally |
|
|
|
What is the developmental uniformity myth for adolescents? |
Seeing adults as big kids or young adults Assuming treatment can be generalised |
|
|
|
Does parental involvement have a significant effect on treatment effectiveness in adolescents? |
No |
|
|
|
Where were students a little older and more of them - Goa or Dehli |
Dehli |
|
|
|
The PRIDE research programme takes which approach? |
Both transdiagnostic risk factors conceptualised and practice elements (CB practice elements selected) implemented within stepped care model |
Elements or transdiagnostic |
|
|
What were the 3 steps in the stepped care model for the PRIDE research programme |
Step 0 = sensitization activities: classroom sessions, posters, staff consultations Step 1 = low intensity problem solving, face to face in school and POD booklet Step 2 = higher intensity modular CBT |
|
|
|
What does POD stand for |
Problem Option Do-it |
|
|
|
What was the first change in the PRIDE intervention |
Changed POD booklets to POD adverture books - comic strips |
|
|
|
Second changes of the PRIDE intervention |
Further modification of eligibility criteria (more clear cut MH probs, screening, focus on older adolescents) Brief face to face therapy rather than guided self-help Simplification of concepts (3 steps instead of 5, original 7) Developed more appealing and accessible materials More sessions in shorter time Step 1 delivered by lay counsellors |
|
|
|
Findings of the Pilot 2 of PRIDE |
Improved acceptability of materials (Only 11.3% where studebt didn't do homework, and 5% where they didn't bring POD booklet) Improved feasibility of delivery Clinical outcomes 44.8% if pilot 2 were fully remitted, average, similar to rich countries, wasn't more effective than 1 but 2 was much more liked |
|
|
|
What does dementia praecox mean? |
Senility of the young |
|
|
|
Criteria for diagnosis of schizophrenia |
2 or more: Delusions Hallucinations Disorganised speech Grossly disorganised or catatonic behaviour (positive = additional symptoms) Negative symptoms (loss of symptoms) e.g., emotional flattening and apathy Deterioration of work, relationships or self-care Continuation for at least 6 months |
|
|
|
What other MH disorders have symptoms of distressing voices |
Bipolar PTSD Dissociative identity disorder Borderline personality disorder |
|
|
|
How common is schizophrenia |
1:100 |
|
|
|
How common is schizophrenia if there is 1 parent with it |
10:100 |
|
|
|
How common is schizophrenia if you have 2 parents with it |
45:100 |
|
|
|
What % of cases of schizophrenia have neither first not second degree relative with it |
37% |
|
|
|
Mean age range of onset of schizophrenia in men |
20-24 |
|
|
|
Mean age range of onset of schizophrenia in women |
25-29 |
|
|
|
2 reasons men have a younger onset for schizo |
Oestrogen has some antipsychotic properties Men become independent earlier traditionally but not ready socially |
|
|
|
6 treatments for schizophrenia |
Sent to asylums/institutions Long baths Sedation Insulin coma ECT (electroconvulsive therapy) Antipsychotic medidation |
|
|
|
5 myths of schizophrenia |
Delusions and voices are meaningless symptoms of schizophrenia. If you hear voices or hold delusional beliefs, you have schizophrenia. Schizophrenia makes people violent. Medication is the solution. People don't recover from schizophrenia. |
|
|
|
Why aren't delusions meaningless |
They are reflective of prominent themes in people's lives. Protective of low self-esteem. Maintained by normal biases in information processing, so once believe people out to harm you, info processing continues this. |
|
|
|
Why are voices not meaningless symptoms of schizophrenia |
Common against people who have experienced trauma. Reflective of opinion that people have about themselves (self-esteem). Similar to interpersonal encounters in the 'real' world. |
|
|
|
What % if american say that most people can be trusted |
33% |
|
|
|
What % of students in a study heard someone call name |
71% |
|
|
|
What % of students in a study heard voices whilst falling asleep? |
30% |
|
|
|
What % of students in a study heard conversations with dead relatives |
5% |
|
|
|
What % of the population experience hallucinations (not just auditory) |
11% |
|
|
|
What are the 3 actual links between schizophrenia and violence? |
A diagnosis of schizo is significantly associated with the risk of criminal and family violence. Even schizophrenia patients without comorbid substance-use disorders were significantly more likely than controls to have been found guilty of violent offences. The association between violence and schizo is stronger for women than men |
|
|
|
What % of schizophrenia patients report being victims of violence within inner cities |
16% |
|
|
|
Why is medication not the solution for schizophrenia |
Side effects can be very distressing Up to 74% of patients discontinue medication over 18 months |
|
|
|
7 types of schizophrenic antipsychotic side effects |
Sedation Weight gain Diabetes Extra-pyramidal symptoms (disorders of movement) Anti-cholinergic (dry mouth, constipation, confusion, impaired memory) Hypotension (low blood pressure) Prolactin elevation (sexual dysfunctions) |
|
|
|
Is the evidence much stronger for antipsychotics or psychological treatments for schizophrenia? |
Psychological treatment |
|
|
|
What % of Trusts meet obstacles offering psychological therapies for schizophrenia |
94% |
|
|
|
What % of patients are offered CBT for schizophrenia |
26% |
|
|
|
How many sessions should CBT be for schizophrenia |
At least 16 |
|
|
|
3 possible solutions for offering CBT to more patients |
Offer less than 16 sessions (can still be effective) Group approaches e.g. mindfulness-based CBT = 7hrs per client Simpler therapies targeting a specific problem that maintains psychotic experiences e.g. paranoid delusions or distressing voices |
|
|
|
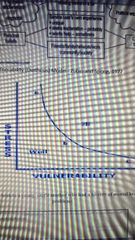
What maximises likelihood patients with schizophrenia will recover? |
Intense help early in first 3 years of difficulties |
|
|
|
What does the stress- vulnerability (diathesis) model look like |
|
|
|
|
Issue of identical twins study for schizophrenia |
Mz twins of parents with diagnosis = 16.8% of children disgnosed MZ twins of parents with no diagnosis = 17.4% of children diagnosed |
Not shared environment |
|
|
Obstretic complications increase risk of child developing schizophrenia by how much |
2× or 3× |
|
|
|
If you're a women diagnosed with schizophrenia, you're more likely to experience birth complications due to what 3 things |
Poor prenatal care Higher rates of smoking, alcohol ans substance use Poverty |
|
|
|
3 theories for how schizophrenia is caused by family problems |
Schizophrenogenic mother Double bind theory Communication deviance |
(Wrong) |
|
|
How can family actually influence schizophrenia |
Expressed emotion can influence relapse Increased criticism, hostility or over-involvement increased relapse |
|
|
|
Internal attributions of discrepancy between actual and ideal self leads to what disorder |
Depression Depression Depression |
|
|
|
Extrenal personal attribution of discrepancy between ideal and actual self leads to what |
Schizophrenia |
|
|
|
What test is commonly used to help us know more about paranoia? |
The beads test |
|
|
|
What does the bead test show |
Jumping to conclusions |
|
|
|
What % of patients with schizophrenia use safety behaviours |
96% |
|
|
|
Evidence employment links to schizophrenia |
As UK unemployment rates increased, schizophrenia rates also increases |
|
|
|
How does the cognitive therapy approach tackle a bias in schizophrenia |
Encourages people to look closely at the facts to prevent the confirmation bias |
|
|
|
What % of a schizophrenic sample report moderate to high levels of self stigma |
42% |
|
|
|
What is the insight paradox |
Greater insight (accepting do have a schizophrenia diagnosis) leads to greater self-stigma and decreased quality of life |
|
|
|
What are the five Ps of CBT formulation |
Presenting Precipitating Perpetuating Predisposing Protective |
Just the names |
|
|
What is the Presenting P of CBT formulation |
What are the problems? |
|
|
|
What is the Precipitating P of CBT formulation |
What triggers the problems? |
|
|
|
What is the Perpetuating P of CBT formulation |
What keeps the problem going? |
|
|
|
What is the Predisposing P of CBT formulation |
What led to the problem starting? |
|
|
|
What is the Protective P of CBT formulation |
What are the persons strengths? |
|
|
|
What does the top half of CBT look at |
Root causes |
|
|
|
What does the bottom half of CBT entail |
Factors maintaining disorder |
|
|
|
What were the findings of the study where currently depressed, previously depressed and never depressed adolescents completed the Dysfunctional Attitudes Test |

No depression not distinguishable from previous depression :o Reaction time shows both current depression and previously depressed are faster at agreeing eith dyfunctional attitudes Only reaction time predicted the onset of dep 1 year later |
Self report score and agreement reaction time |
|
|
What was the difference in dyfunctional attitudes pre and post CBT and pharmacotherapy |
No difference |
|
|
|
What was the difference in dyfunctional attitudes in remission from CBT and pharmacotherapy (PT) after they went through a sad mood provocation |
PT had increase in dyfunctional attitudes aa a response CBT doing something to cog reactivity? |
|
|
|
Mood-linked cog reactivity predicted what in dep individuals |
Relapse over next 18 months |
|
|
|
2 types of self focus |
Experiential/direct Conceptual/simulation |
|
|
|
What is experiential/direct self focus |
Focus on our bodily senses |
|
|
|
What is the conceptual/simulation self focus |
Focus on conceptualising senses e.g. labelling elaborating planning judging |
|
|
|
Which type of self focus is enhanced with people who have depression |
Conceptual/narrative self-focus |
|
|
|
What part of conceptual self focus predicts onset and duration of depression |
Rumination |
|
|
|
How can distraction help in depression |
Short lived benefits, rumination occurs after distracted |
|
|
|
What reduces activation of mood linked cognitive reactivity |
Contextual awareness |
|
|
|
How can mindfulness help depression |
Shift from thinking self focus to sensing self focus Monitor toughts, deem them as mental events |
|
|
|
Who is Mindfulness-based Cognitive Therapy designed for |
Patients in remission from recurrent depression to reduce relapse |
|
|
|
What does mindfulness do for sadness |
Changes the expression in the brain Uncouple narrative vs experiential processing |
|
|
|
How does MBCT (mindful) affect relapse rates for dep patients with >=3 previous episodes vs treatment as usual |
Halves (37% vs 66%) |
|
|
|
MBCT does better than what in terms of maintenance (of treated) |
Antidepressants |
|
|
|
NICE recommends MBCT to who |
People with 3 or more episodes of depression |
|
|
|
In the assumption of CBT, the way that you think and behave in response to experiences determines what 3 things |
Distress Function Need |
|
|
|
Psychological models view delusions as what 6 things |
On a continuum with normal beliefs Multidimensional Attempts to make sense of anomalous experiences Mediated by appraisals Involve reasoning and attributional biases Influences by emotional processes |
|
|
|
What shows that delusions are on a continuum with normal beliefs |
The structure of paranoia (Freeman et al - at least of weekly frequency: "strangers and friends look at me critically" - "there is a conspiracy against me") |
|
|
|
What are the 3 dimensions of delusions (names) |
Conviction Preoccupation Distress |
|
|
|
What is conviction |
Strength of beliefs |
|
|
|
What is preoccupation |
How much time thinking/worrying about something |
|
|
|
Evidence that delusions are attempts to make sense of anomalous experience |
Nielsen experiment Ppts explain discrepancies between planning and actual motor movements as: My hand was controlled by an outside physical force Couldn't see electrodes on hand, were there but couldnt see If it was because i am homosexual |
|
|
|
Evidence that delusions are attempts to make sense of anomalous experience |
Nielsen experiment Ppts explain discrepancies between planning and actual motor movements as: My hand was controlled by an outside physical force Couldn't see electrodes on hand, were there but couldnt see If it was because i am homosexual |
|
|
|
Evidence for delusions being mediated by appraisals |
Undiagnosed group makes more normalising, spiritual and psychological appraisals for anomalous experiences (e.g. tired) Diagnosed made more personal appraisals (e.g. someone else is doing this to me) |
|
|
|
Evidence for involving reasoning and attributional biases in delusions |

Jump to conclusions bias Say they're certain which jar the bead comes from much quicker |
|
|
|
Evidence delusions are influenced by emotional processes |
Hallucinations + distress = delusions 18.75% Hallucinations - distress = delusions 4.35% 4 fold increase in distress group Emotions involved at formation stage |
|
|
|
What is the mean effect size of CBT on positive symptoms |
0.4 (small to moderate) |
|
|
|
Which dimension of psychosis does effectiveness measure normally |
Conviction (how often hear voices) |
|
|
|
Which dimensions of psychosis are addressed with CBT |
Distress, preoccupation |
|
|
|
What do RCTs measure |
Symptom change |
|
|
|
Which is the standardised scale for RCTs |
The PANSS Positive and Negative Syndrome Scale |
|
|
|
Out of behaviour mood and belief change, which may CBT not target |
Belief change |
|
|
|
4 internal conditions in service user concept of recovery |
Hope Healing Empowerment Connection |
|
|
|
3 external conditions in service user concept of recovery |
Human rights Positive value of healing Recovery oriented services |
|
|
|
Name of psychological recovery including CBT priorities and general recovery |
CHOICE |
|
|
|
Effects of CBT on worry in psychosis |
Significantly reduce Also reduce persecutory delusion Significant improvements in well-being, CHOICE and overall symptoms |
|
|
|
Name of CBT for worry in psychosis |
Winning against worry |
|
|
|
6 components to winning against worry |
Monitoring worry Normalising worry Worry cycle Building motivation to give up worry Worry periods Boosting worry periods and other activities |
|
|
|
4 parts of the worry cycle |
Feeling under threat⬅️ ⬇️ Positive beliefs/reasons for worry ⬇️ Worry ⬇️ Dwell on worst thing that could happen (what if) ⤴️ |
|
|
|
2 parts of worry periods |
Planning a time and place to worry Planning how to postpone worry until the worry period |
|
|
|
How do worry periods help |
Helps patients see that worry is in their control |
|
|
|
5 other activities boosted in winning against worry |
Activities Making contact with someone Thinking of something different Relaxation Problem solving |
|
|
|
Other new approach besides winning against worry for psychosis |
Treatment of insomnia |
|
|
|
Are new methods like winning against worry longer or shorter than normal CBT |
Shorter |
|
|
|
The multi-component treatment for pscyhosis (putting it all together, CBT+) is how many months |
6 |
|

