![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
97 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Direct thrombin inhibitors
|
the -rudin's
|
|
|
|
A 65 amino acid peptide obtained from leeches and is a thrombin inhibitor
|
Hirudin
|
|
|
|
Recombinant yeast-derived form of hirudin
|
Lepirudin
**Leper who also has a yeast infection |
|
|
|
1st agent approved for anticoagulation in patients with Heparin-induced Thrombocytopenia (HIT)
|
Lepirudin
|
|
|
|
2 new recombinant hirudin analogs that may be used instead of heparins in the future
|
Desi-rudin
Bivali-rudin |
|
|
|
2nd agent approved for HIT and unlike Lepirudin, it is cleared by the liver and can be used in patients with end-stage renal disease
|
Argatroban
*an "Argentine Trojan" who has HIT and End-stage Renal Disease |
|
|
|
The only oral anticoagulant given in the US
|
Warfarin
|
|
|
|
Warfarin:
- __1__ derivative -hemorrhagic substance found in __2__ and used as __3__ |
1. Coumarin
2. spoiled sweet clover 3. rodenticides |
|
|
|
What accounts for the low volume of distribution of Warfarin?
|
>99% binds to plasma proteins
|
|
|
|
What is the half-life of Warfarin?
|
36 hours!!!
**due to extensive plasma protein binding |
|
|
|
What is the active form of Warfarin?
|
S isomer
|
|
|
|
Warfarin is metabolized to inactive metabolites by _____ in the liver
|
CYP 2C9
*site of numerous drug interactions |
|
|
|
What clotting factors does Warfarin inhibit the synthesis of?
|
2, 7, 9, 10, and 12
|
|
|
|
Explain the mechanism of Warfarin
|

-Factors 2, 7, 9, 10, and 12 are zymogens which become activated via Vitamin K-dependent Carboxylation
-Warfarin inhibits Vitamin K Epoxide Reductase, which normally frees up just-used Vitamin K's = stops the process of Carboxylation |
|
|
|
Warfarin:
1. Target 2. Resistance 3. Speed of onset 4. Antidote (2 options) |
1. Vitamin K Epoxide Reductase
2. mutations in Vitamin K epoxide reductase 3. Slow 4. Vitamin K (Phytonadione) and fresh, frozen plasma or Factor 9 concentrates containing Prothrombin Complex |
|
|
|
What is the pharmacokinetic and the pharmacodynamic as to why the onset of Warfarin action is slow?
|
Kinetic -> takes ~ 1 week to reach steady state
Dynamic -> time to replace the normal clotting factors with incompletely gamma-carboxylated factors |
|
|
|
Warfarin:
Takes __1__ (time) for the initial anticoagulant effect and several days to reach maximum __2__ |
1. 8-12 hours
2. Hypoprothrombinemia |
|
|
|
What drug inhibits Oral Warfarin absorption?
What other thing does it affect? |
Cholestryramine
Vitamin K absorption |
|
|
|
What 6 things induce hepatic microsomal enzymes and diminish the response to Warfarin? (hint)
|
1. Barbiturates
2. Carbamazepine 3. Phenytoin 4. Primidone 5. Rifampin 6. St. John's Wort **1-4 are anticonvulsants |
There is low WARfare when BARB eats CARBS and is not a PRIMADONNA. When she doesn't, it causes a RIF with her husband St. John so he hits her in the PHANNY-toin
|
|
|
What stimulates Clotting Factor synthesis in the liver and diminishes Warfarins effects?
|
Estrogen
**this is why Oral Contraceptives increase risk of thromboembolism |
|
|
|
Explain how eating more green vegetables can diminish the effects of Warfarin
|
Veggies contain Vitamin K
- Vitamin K is involved in activating Clotting Factors |
|
|
|
What drug displaces Warfarin from plasma albumin and enhances its effects?
|
Sulfonamides
|
|
|
|
What 8 drugs inhibit Warfarin metabolism and enhance its effects?
|
1. Amiodarone
2. Allopurinol 3. Cimetidine 4. Ciprofloxacin 5. Erythromycin 6. Co-trimoxazole 7. Metronidazole** 8. Fluconazole** **selective for S-warfarin |
CoME CACA F = increased plasma Warfarin
|
|
|
What would reduce the availability of Vitamin K and therefore enhance the effects of Warfarin?
|
Broad-spectrum antibiotics
-gut bacteria produce Vitamin K |
|
|
|
Treatment for Arterial and Venous thrombi:
__1__ is used for the first 7-10 days with a 3-5 day overlap with __2__, which may be continued for up to 6 months |
1. Heparin
2. Warfarin |
|
|
|
Aside from treating Arterial and Venous Thrombi, Warfarin is also used to prevent __1__ in patients with __2__
|
1. blood clots
2. chronic atrial fibrillation |
|
|
|
The therapeutic goal of Warfarin is to prolong ______ above normal
|
Prothrombin time (PT)
|
|
|
|
Warfarin:
Low-intensity anticoagulation is used for __1__ Moderate-intensity anticoagulation is used __2__ High-intensity anticoagulation is used for __3__ |
1. Long term
2. initially 3. mechanical prosthetic heart valves |
|
|
|
The therapeutic goal of Warfarin is achieved after how long?
|
1 week (4-5 doses with a 1.5 day half-life) = SLOW ONSET
|
|
|
|
Adverse effect of Warfarin: Serious and possibly fatal bleeding can occur in these 4 places
|
1. Brain
2. Pericardium 3. Stomach 4. Intestines |
|
|
|
Under what 3 conditions is Warfarin Contraindicated?
|
1. Pregnancy
2. patients with bleeding disorders 3. Liver disease (impaired drug metabolism)*** ***seem to forget this one |
|
|
|
Why is Warfarin contraindicated with Pregnancy?
|
1st trimester = Teratogen
1-3 trimester = fetal hemorrhage |
|
|
-
|
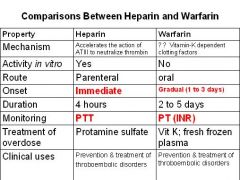
-
|
|
|
|
Thrombolytic drugs:
-therapy is directed towards the conversion of __1__ to __2__, which degrades fibrin and lyses thrombi -Circulating __3__ preclude the possibility of using plasmin itself for thrombolytic therapy -Plasma does not contain inhibitors of __4__ or the comblex formed betwen plasminogen and __5__ |
1. Plasminogen
2. Plasmin 3. Antiplasmins 4. Urokinase 5. Streptokinase |
|
|
|
Why are Urokinase and Streptokinase not inhibited by circulating Antiplasmins?
|
B/C they convert Plasminogen -> Plasmin INSIDE the Thrombus, where plasmin is protected from the inhibitory effects of circulating antiplasms
|
|
|
|
List 6 indications for Anticoagulant Therapy
|
1. MI
2. Rheumatic heart disease 3. Cerebrovascular disease 4. Venous thrombosis 5. Pulmonary embolism 6. DIC |
|
|
|
What is the definition of Thrombolytic drugs?
|
lyse thrombi by catalyzing the formation of the serine protease Plasmin from its precursor Plasminogen
|
|
|
|
Describe the selectivity of tissue plasminogen activator (t-PA)
|

preferentially converts fibrin-bound plasminogen over free plasminogen = more likely to select for plasminogen in a clot
|
|
|
|
t-PA is more efficacious than streptokinase or anistreplase for thrombolytic therapy in __1__, but carries a higher risk of __2__
|
1. MI
2. Hemorrhage stroke |
|
|
|
What are the 2 disadvantages of t-PA compared to Streptokinase or Urokinase?
|
1. more expensive
2. higher risk of hemorrhagic stroke |
|
|
|
Streptokinase:
-__1__ protein produced by __2__ -facilitates thrombolysis through the formation of __3__ |
1. Nonenzymatic
2. group C beta-hemolytic streptococci 3. activator complex with plasminogen |
|
|
|
What 4 things does Plasmin degrade?
|
Fibrin
Fibrinogen Factor 5 Factor 8 |
|
|
|
What 2 drug combo may be as effective as t-PA?
|
Aspirin
Streptokinase |
|
|
|
What adverse effect of Streptokinase may occur?
|
Hypersensitivity
**protein from Group C Strep |
|
|
|
What is Antistreplase?
|
Acylated form of Plasminogen-Streptokinase-Activated Complex (APSAC)
*increases the duration of action relative to Streptokinase alone |
|
|
|
-Parenteral thrombolytic agent derived from human cultured KIDNEY CELLS
-Hypersensitivity reactions OCCUR LESS FREQUENTLY than with Streptokinase |
Urokinase
|
|
|
|
What uses is Urokinase indicated for?
|
Lysis of Pulmonary emboli
Lysis of coronary artery thrombi associated with evolving transmural MI |
|
|
|
List the 3 recombinant Thrombolytic agents
|
1. Alteplase
2. Reteplase 3. Tenecteplase |
|
|
|
List 2 properties of Alteplase
|
1. considerably more expensive than streptokinase
2. not associated with Hypersensitivity reactions |
|
|
|
List a property of Reteplase
|
Longer half-life than Alteplase
**Re-Re-Re = keep re-doing things takes longer = longer half-life |
|
|
|
Compared to Alteplase:
-prolonged half-life -increased specificity for fibrin -resistance to plasminogen activator inhibitor-1 |
Tenecteplase
|
|
|
|
Thrombolytic therapy should be followed with anticoagulant therapy with __1__ and then __2__
|
1. Heparin
2. Warfarin |
|
|
|
For Myocardial Infarction, this may be used as an adjuvant therapy in combination with Thrombolytic agents
|
Aspirin due to its anti-platelet effect
|
|
|
|
List 7 Contraindications for Thrombolytic Therapy
|
1. Surgery within 10 days
2. Serious GI bleeding within 3 months 3. History of HTN (diastolic pressure > 110 mm Hg) 4. Active bleeding or hemorrhagic disorder 5. previous Cerebrovascular accident or active intracranial process 6. Aortic dissection 7. Acute pericarditis |
|
|
|
Vitamin K:
-Is a __1__ soluble vitamin found in __2__ -also produced by bacteria colonizing the human intestine; need __3__ for absorption |
1. fat
2. leafy green vegetables 3. bile salts |
|
|
|
What process is Vitamin K required for?
|
gamma-carboxylation of glutamate residues in Prothrombin and Factors 7, 9, and 10
|
|
|
|
List 4 drugs used to treat Bleeding Disorders
|
1. Vitamin K
2. Plasma Fractions/Clotting Factors 3. Antihemophilic Factor 4. Aminocaproic acid |
|
|
|
What discourages the use of plasma fractions in the treatment of patients with Hemophilia?
|
AIDS and Viral Hepatitis
|
|
|
|
What is Aminocaproic Acid's mechanism of action?
|
It binds to Plasminogen and inhibits its binding to Fibrin, preventing conversion to Plasmin
|
|
|
|
Antihemophilic Factor is commercially prepared using genetically altered mammalian cells to secrete _______
|
Factor 8
|
|
|
|
Aminocaproic Acid is used to treat these 3 things
|
1. Systemic or urinary hyperfibrinolysis (aplastic anemia, abruptio placentae, hepatic cirrhosis)
2. Bleeding associated with neoplastic diseases (carcinoma of the prostate, lung, stomach, or cervix) 3. Bleeding following cardiac surgery |
|
|
|
In what 2 ways can anemia arise?
|
1. from failure to make sufficient RBC's
2. failure to synthesize adequate quantities of Hemoglobin |
|
|
|
What are 5 symptoms of Anemia?
|
1. Paleness
2. Fatigue 3. Shortness of breath 4. exercise intolerance 5. increased heart rate |
|
|
|
Anemia due to a decrease in the amount of Hemoglobin per RBC
|
Microcytic, hypochromic anemia
|
|
|
|
Anemia due to a decrease in the number of circulating RBC's
|
Megaloblastic, Hyperchromic anemia
|
|
|
|
Anemia due to a decrease in hemopoietic growth factors, especially Erythropoietin
|
Normocytic anemia or mixed
|
|
|
|
Microcytic Hypochromic Anemia:
__1__ deficiency -> impaired __2__ synthesis -> __3__ red cells with insufficient __4__ -> Microcytic Hypochromic Anemia |
1. Iron
2. Hemoblobin 3. small 4. hemoglobin |
|
|
|
What is Megaloblastic Anemia due to a deficiency of?
What does that cause an impaired synthesis of? |
Vitamin B12 or Folate
DNA |
|
|
|
What are the 3 physiological functions of Iron?
|
1. Required for Hemoglobin synthesis
2. Co-factor in such enzymes as Cytochromes 3. Required for Myoglobin synthesis |
|
|
|
Where is Iron absorbed?
|
Duodenum and Proximal Jejunum
|
|
|
|
Iron Absorption:
-involves active transport of __1__, which is oxidized to __2__ in the intestinal mucosa -Ferric iron can be stored as __3__ in the intestinal mucosa, or it can be transported by __4__ to other sites |
1. ferrous iron
2. ferric iron 3. ferritin 4. transferrin |
|
|
|
What percent of dietary elemental iron is absorbed?
|
5-10%
|
|
|
|
Heme-iron from meat can be absorbed with iron in the _______ state
|
Ferric
|
|
|
|
What increases iron absorption and the rate of erythopoiesis?
|
Low iron stores = low ferritin in the intestinal mucosa
|
|
|
|
What 5 things decrease iron absorption?
|
1. food
2. metal chelators 3. antacids 4. Fluoroquinolones 5. Tetracycline |
|
|
|
What 2 things increase the absorption of Iron?
|
1. Hydrochloric acid
2. large amounts of ascorbic acid (Vitamin C = OJ) |
|
|
|
Iron Distribution:
-__1__ is a specific ferric iron transport protein -Erythroid cells have __2__, thus, iron is actively transported into hemoglobin-synthesizing cells in the bone marrow -__3__ converts ferrous iron into the ferric state, and this copper-containing, plasma protein appears to be important for cellular uptake of iron |
1. Transferrin
2. Transferrin receptors 3. Ceruloplasmin |
|
|
|
Iron Distribution:
-10-20% total iron store in __1__ -70% in __2__ -10% in __3__ -1% in __4__ |
1. ferritin and hemosiderin, which are stored in macrophages in the liver, spleen and bone marrow
2. hemoglobin (RBCs) 3. myoglobin (muscle) 4. cytochromes and transferrin |
|
|
|
What is iron balance regulated by?
|
Intestinal absorption
*there is no specific mechanism for excreting iron |
|
|
|
About 1 mg of iron is lost daily by such processes as __1__ of mucosal cells, which contain __2__
|
1. exfoliation
2. ferritin |
|
|
|
What are 4 possible causes of Iron Deficiency?
|
1. Inadequate intake: rare in US
2. Malabsorption 3. Increased requirements: growth, pregnancy, menstruation 4. Blood loss: bleeding, CA |
|
|
|
What are 3 indicators of Iron Deficiency?
|
1. Serum ferritin decreases (<10 ųg/L)
2. Serum iron decreases (<40 ųg/dL) 3. Total iron-binding capacity of transferrin increases (>400 ųg/dL) = due to decreased saturation |
|
|
|
What are the DOC's for Iron deficiency anemia?
|
Ferrous Salts (ORAL)
-ferrous sulfate -ferrous gluconate -ferrous fumarate |
|
|
|
Iron deficiency anemia:
-treatment results in a rapid increase in __1__, and a measurable response to iron therapy should be detectable within __2__ -normal hemoglobin levels should be reachedd in __3__ -treatment should last 3-6 months or longer if the dose of iron was decreased due to __4__ |
1. reticulocytosis
2. 1 week 3. 1-3 months 4. intolerance |
|
|
|
Normal hemoglobin levels for:
1. men 2. women |
1. 14-18 g/dL
2. 12-16 g/dL |
|
|
|
What is the Parenteral form of treatment for Iron deficiency anemia?
|
Iron Dextran
|
|
|
|
When should Iron Dextran be used?
|
1. patients with Gastric or Small Bowel resections
2. patients with Inflammatory Bowel Disease involving the proximal small intestine |
|
|
|
What is the antidote for Acute Toxicity from Oral Iron?
|
Deferoxamine = iron-chelating drug
**De-ferrous |
|
|
|
What are some symptoms of Acute toxicity from Oral Iron?
|
1. GI irritation
2. GI necrosis 3. nausea 4. cyanosis 5. Hematemesis 6. Green and tarry stools 7. CV collapse 8. Metabolic acidosis GI = irritation, necrosis, nausea, hematemesis, green stools (5) Others = Cyanosis, CV collapse, Metabolic acidosis |
|
|
|
What are some symptoms of Acute Toxicity from Iron Dextran?
|
1. Headache
2. Light headedness 3. Fever 4. Arthralgia 5. N/V 6. Back pain 7. Flushing 8. Urticaria 9. Bronchospasm 10. Anaphylaxis -> can cause death (very rare) |
|
|
|
What should be done before administering Iron Dextran?
|
give small doses to check for signs of immediate hypersensitivity
|
|
|
|
This is an inherited disorder where there is excessive iron absorption
|
Hemochromatosis = iron overload
|
|
|
|
What can Hemosiderosis be the result of?
|
numerous blood transfusions
|
|
|
|
Iron overload may also occur in the presence of anemia other than that caused by iron deficiency, such as the anemia of __1__ or __2__
|
1. chronic disease
2. hemolytic anemia |
|
|
|
Excess iron is deposited in these organs
|
1. heart
2. liver 3. pancreas |
|
|
|
In the absence of anemia, Iron overload is treat by _______
|
Phlebotomy
*one unit of blood removed 250-mg of iron |
|
|
|
What would a loss of Hemosiderin granules in Bone Marrow indicate?
|
Iron deficiency
|
|

