![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
19 Cards in this Set
- Front
- Back
|
Pigmented lesion usually seen on attached gingiva that usually has a history of long duration.
- May be increased in pregnancy |
Physiologic (racial) Pigmentation (Melanoplakia)
HISTO - Melanin is secreted by the melanocytes and accumulates in the basal cell layer. |
|
|
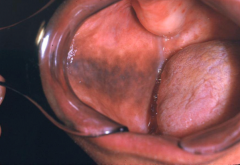
Smokers Melanosis
- seen in 21% of smokers - appears as brown patch several cm in diameter - Most common area is mandibular anterier gingiva, buccal mucosa, palate, etc. - Amount of pigmentation appears to be related to amount of tobacco consumed - May disappear months to years after cessation of smoking. Not pre-malignant. |
|
|
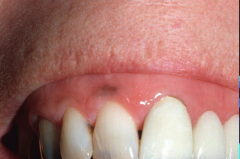
Oral Melanotic Macule
- Occurs on oral mucosa (vermillion border and gingiva) - Usually < 7mm - 2:1 Female predilection - Do not usually enlarge after diagnosis - Not related to sun exposure. |
|
|
An area of increased melanin pigmentation mainly within the basal cell layer (w/out an increase in the number of melanocytes) That is related to sun exposure.
|
Ephelis (Freckle)
- usually > 5 mm in diameter - usually occurs on lip (85% lower lip) |
|
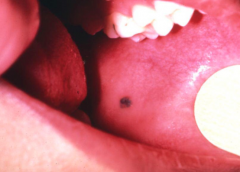
Present for a long time
|
Pigmented Cellula Nevus (mole)
- Does not blanch (may not be pigmented) - Most frequently on palate (most common intraoral site), gingiva, Buccal mucosa (2nd most common intraoral site) and lips. - Usually less than 6 mm Most common of all human "tumors" but really rare in the oral cavity. |
|
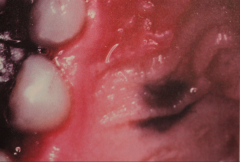
later stage: Nevus cells are no longer within epithelium but are within the underlying connective tissue.
|
Intramucosal nevus (pigmented cellular neveus, mole)
- Most common intraoral nevi |
|
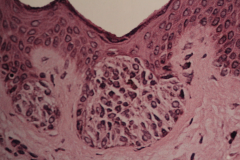
nevus cells are located at the junction of epithelium and CT
|
Junctional nevus
Other variants - Blue nevus (2nd most common oral nevi) usually hard palate - Congenital melanocytic nevus - Halo nevus - Spitz nevus (Benign juvenile melanoma) |
|
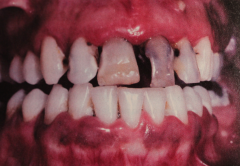
|
Smoker melanosis
|
|
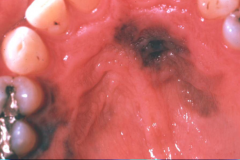
|
Malignant Melanoma
- 3rd most common cancer of skin (83% of all deaths due to skin cancer) - Sunlight is an important etiologic factor - Ulceration is common Two phases of growth. - Radial-growth phase: cells spread laterally but stay confined to epithelium - better prognosis. - Vertical growth phase -Malignant cells begin to invade underlying connective tissue. |
|
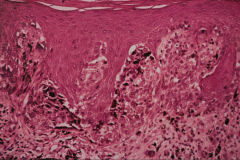
|
Acral lentiginous melanoma
- most common form in the oral cavity - This palatal melanoma demonstrates numerous atypical melanocytes in the basilar portion of the epithelium with invasion into the superficial lamina propria. |
|
|
Three common types of Melanoma
|
Superficial spreading melanoma (70% of all melanomas)
- Most common on backs of males and legs of females. Nodular melanoma (15%) Lentigo Melanoma (5-10%) Remember ABCDE |
|
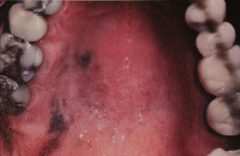
|
Oral malignant melanoma
- Uncommon neoplasm of the oral mucosa (primary melanoma of the oral cavity is rare. Melanoma that aries on the skin metastasize to the oral cavity. - 80% on the maxillary ridge and palate -Frequently see focal pigmentation of mucosa several months or years before malignancy - Poor prognosis for oral melanoma Treatment = radical surgery, chemotherapy, & radiation |
|
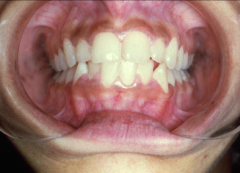
|
Addison's disease
- Generalized weakness, fatigue. Hypotension. - Generalized abnormal pigmentation (bronzing of skin and mucous membranes. Oral pigmentation varies from light brown to almost black, especially gingiva, lateral tongue, buccal mucosa and lips. |
|
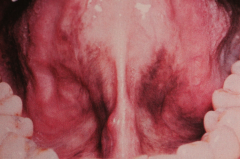
|
Addison's Disease
- Destruction of adrenal cortex due to autoimmunity, TB, tumors, AIDS, etc. - Decreased steroid levels stimulate pituitary ACTH output with increased levels of MSH (melanocyte stimulating hormone) Treatment - exogenous steroids. |
|
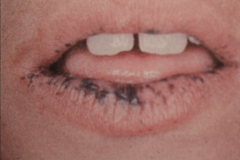
|
Peutz-Jeghers syndrom
- Childhood onset, familial condition - Oral perioral melanotic macules - intestinal polyposis - Pigmentation of 1-5 mm found around lips, eyes, nose... - Oral pigmentation includes buccal mucosa, gingiva, palate (seldom tongue) - Polyps may cause abdominal pain and cause obstruction due to intussusception. |
|
|
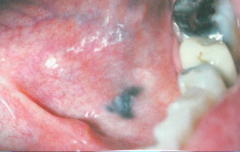
Amalgam Tattoo.
- Blue/black, most common intraoral soft tissue pigmentation - Several ways of implantation (including flossing) HISTO - black granular material, usually lying free in the connective tissue. - Must identify by radiograph or biopsy |
|
|
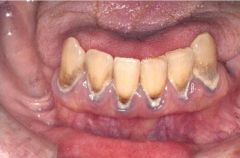
Lead (Plumbism)
- GI disturbance, Peripheral neuritis, encephalitis, hypochromic anemia with basophilic stippling of RBC's, deposition of lead into growing bones. Oral Manifestation - Lead line in gingiva (due to formation of lead sulfide) - Excess salivation and metallic tast - Swelling of salivary glands - May be deposited in deciduous teeth |
|
|
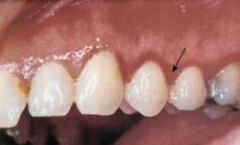
Bismuth
- "Bismuth Line" may be seen in gingiva, buccal mucosa, lips and ventral tongue - hydrogen sulfide, produced by oral bacteria, causes proliferation of granules of bismuth sulfide - Prevention by good oral hygiene - disappears after discontinuance of bismuth |
|
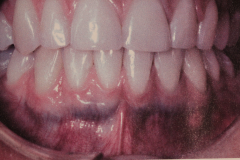
Caused by drug used to treat acne
|
Pigmentation Associated with Drug Minocycline Staining
- Staining of tissue due to ingestion of Minocycline (synthetic tetracycline). - Generalized darker stain in alveolar, palate, vestibule... - may be focal or generalized - may affect roots of teeth No treatment needed. |

