![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
56 Cards in this Set
- Front
- Back
|
What is it called when there are too FEW platelets? Cuses?
|
Thrombocytopenia
Decreased production Increased degradation |
|
|
What is it called when there are too many platelets?
|
Thrombocytosis
|
|
|
How are platelets produced from megakaryocytes?
|
Budding
|
|
|
What's the lifespan of a platelet?
|
5-9 days
|
|
|
What is the normal platelet count?
|
150-400E9/L
|
|
|
What protein regulates platelet production?
|
Thrombopoietin
|
|
|
What organs recycle platelets?
|
Spleen
Liver |
|
|
What cells in the liver destroy platelets?
|
Kupffer cells
|
|
|
What is a storage site for platelets?
|
Spleen
|
|
|
What causes platelets to be released by the spleen?
|
Sympathetic activation
|
|
|
What levels of platelets are associated with increased risk of spontaneous hemorrhage? Spontaneous intracranial hemorrhage?
|
Spontaneous: <20,000
Intracranial: <10,000 |
|
|
What is the platelet cutoff for general surgery?
|
60,000/uL
|
|
|
What are some causes of prolonged bleeding in the context of a normal platelet count?
|
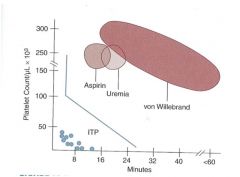
Asprin (think decreased thromboxane-->decreased activation )
Uremia (altered prostaglandins/thromboxane-->decreased activation) von Willebrand |
|
|
What are some causes of decreased production of platelets?
|
Bone marrow problems!
-Primary failure -Invasion of the marrow -Injury to bone marrow -Nutritional problems -Megaloblastic anemia -Hereditary platelet disorders |
|
|
What is the effect of alcohol on bone marrow?
|
Inhibition
|
|
|
What are the causes of increased platelet destruction?
|
Immune mediated
Non-immune mediated |
|
|
What are some of the non immune-mediated causes of platelet destruction?
|
DIC
TTP Hypersplenism |
|
|
What is the effect of having a large spleen on blood platelet levels?
|
Sucks up the platelets from the circulation
Can get levels as low as 40,000-60,000 |
|
|
What are some of the immune mediated causes of increased platelet destruction?
|
Immune thrombocytopenia
Neonatal autoimmune thrombocytopenia Drug induced Heparin induced |
|
|
What are the different types of autoimmune thrombocytopenia?
|
Acute
Chronic Secondary |
|
|
Who gets acute autoimmune thrombocytopenia?
|
Children
|
|
|
What are the symptoms of acute autoimmmune thrombocytopenia?
|
Viral illness 3 weeks ago
Severe bleeding symptoms; self limited |
|
|
Who gets chronic autoimmmune thrombocytopenia?
|
Women
20-40 |
|
|
What does the bone marrow look like in chronic autoimmmune thrombocytopenia?
|
Normal
|
|
|
What diseases is secondary autoimmmune thrombocytopenia associated with?
|
Disordered lymphoid function:
SLE Lymphoma CLL |
|
|
What is a good therapy for ITP?
|
Splenectomy!
|
|
|
What are some concerns for splenecomy in people with ITP?
|
Are the antibodies produced in the marrow?
It could be the case that the platelets are destroyed somewhere else |
|
|
Other than splenectomy, what are some of the other therapies for ITP?
|
IVIg
Anti CD 20 immunotherapy Immune modulators Platelet growth factors |
|
|
What is the cause of neonatal allo immune thrombocytopenia?
|
Antibodies from mom are put into the circulation of the baby
It can be when there's a mismatch in an antigen status: mom is Pla1- and the fetus is Pla1+ |
|
|
What's the timeline for platelet levels to recover after a drug-induced thrombocytopenia?
|
7 days - 3 weeks
YOu need to wait until all of the drug is out of the body |
|
|
What are the two forms of heparin induced thrombocytopenia?
|
Mild
Severe: -Platelet count decreases more than 30% form baseline |
|
|
What's the treatment for heparin induced thrombocytopenia?
|
Treat the thrombosis!
|
|
|
What's the mechanism of heparin induced thrombocytopenia?
|
1. Heparin comes into body
2. Heparin PF4 complexes form 3. Antibodies that bind to the platelets also bind to the heparin-PF4 complexes cause more activation of platelets 4. More release of PF4 (it becomes a cycle, here) 5. Endothelial cell injruy |
|
|
How long do antibodies in heparin induced thrombocytopenia stick around?
|
3 months!
Beware! |
|
|
What are the causes of primary thrombocytosis?
|
Clonal myeloproliferative disorders
-Chronic myelogenous leukemia -Essential thrombocytosis -Polycythemia vera |
|
|
Why is there often bleeding in the setting of primary thrombocytosis?
|
It's often the case that despite their large numbers, the platelets are still dysfunctional
|
|
|
What levels is defined as secondary thrombocytosis?
|
>700,000/uL
|
|
|
What are causes of secondary thrombocytosis?
|
Inflammation
Hemorrhage Post splenectomy Iron deficiency |
|
|
What are some ways that you can assess platelet function?
|
Peripheral smears
Counts: NL = 150k - 450k Bleeding time: NL < 9 minutes Platelet aggregation: main tool |
|
|
What are some different substances you can use to assess platelet aggregation?
|
Thrombin
ADP Epinephrine Collagen |
|
|
What are the properties of the qualitative platelet disorders?
|
Platelet function abnormalities
Normal count Bleeding symptoms |
|
|
What are the receptors that cause interplatelet links?
|
GPIIb
|
|
|
What molecules cause the release reaction in platelets?
|
Thromboxane
This is blocked with asprin! |
|
|
What are the different kinds of inherited disorders of platelet function?
|
Platelet-vessel
Platelet-platelet Granules, secretion, signal transduction |
|
|
What are the congenital disorders of adhesion?
|
Von Willebrand's disease
Bernard soulier syndrome |
|
|
What defect is present in vWD?
|
Missing a linker molecule between the platelet and the vascular endothelium
|
|
|
What defect is present in Bernard Soulier?
|
GpIb defect
|
|
|
What are the findings in Bernard Soulier Syndrome?
|
Thrombocytopenia
Giant platelets found on the smear |
|
|
What platelet aggravating factor won't vWD or Bernard Soulier patients respond to?
|
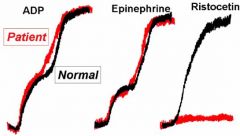
Ristocetin
|
|
|
What is afibrinogemia?
|
Platelet and coagulation factor defect type bleeding
Fibrin just isn't there |
|
|
What protein is mutated in Glanzmann's thrombocytopenia?
|
Autosomal disorder
Absent/defective GpIIbIIIa |
|
|
If you have thrombasthenia/afibrinogenemia, what platelet aggravants aren't effective?
|

ADP
Epinephrine |
|
|
What are the different kinds of disorders of activation and secretion of platelets?
|
Storage pool deficiency
Defectsin platelet stimulus response coupling pathways Primary secretion defects |
|
|
What is the difference between the aggravation patterns between Glanzmann's and Bernard-Soulier?
|
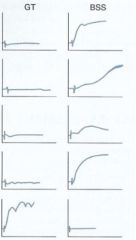
They're the opposite!
|
|
|
What are the different kinds of acquired platelet function defects?
|
Urmia
Myeloproliferative disorders Myeodysplastic disorders, leukemia Dysproteinemias Cardiopulmonary bypass Antibodies Lung disease Drugs |
|
|
How does uremia cause an acquired platelet function defect?
|
Toxins in the wall cause abnormalities in the wall, abnoramlities in the platelet prostaglandin pathways
|

