![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
57 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Efferent Neuron – Moving toward a central organ or point
Relays messages from the brain or spinal cord to the muscles and organs |
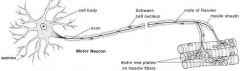
Motor Neuron
|
Short dendrites and long axons
Dendrites and the cell body are located in the spinal cord; the axon is outside of the spinal cord Conduct impulse to an effector (muscle or gland) |
|
|
Afferent Neuron – Moving away from a central organ or point
Relays messages from receptors to the brain or spinal cord |
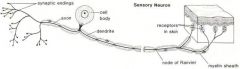
Sensory Neuron:
|
Long dendrites and short axon
Cell body and dendrite are outside of the spinal cord; the cell body is located in a dorsal root ganglion Conduct impulse to the spinal cord |
|
|
Axons
|
Take information away from the cell body
Smooth Surface Generally only 1 axon per cell No ribosomes Can have myelin Branch further from the cell body |
|
|
|
Dendrites
|
Bring information to the cell body
Rough Surface (dendritic spines) Usually many dendrites per cell Have ribosomes No myelin insulation Branch near the cell body |
|
|
|
List the three types of neurones:
|
Sensory neurones have long axons and transmit nerve impulses from sensory receptors all over the body to the central nervous system.
Motor neurones also have long axons and transmit nerve impulses from the central nervous system to effectors (muscles and glands) all over the body. Interneurones (also called connector neurones or relay neurones) are usually much smaller cells, with many interconnections. |
|
|
|
Sympathetic System
|
Dilates pupil
Inhibits saliva production Dilates bronchi Speeds up heart rate Inhibits peristalsis Stimulates glucose production Inhibits urination |
|
|
|
Parasympathetic System
|
Constricts pupil
Stimulates tear secretion Stimulates saliva production Constricts bronchi Slows down heart rate Stimulates peristalsis Stimulates bile production Stimulates urination |
|
|
|
The synapse consists of:
|
a presynaptic ending that contains neurotransmitters, mitochondria and other cell organelles,
a postsynaptic ending that contains receptor sites for neurotransmitters and, a synaptic cleft or space between the presynaptic and postsynaptic endings. |
|
|
|
Synapse
|
The synapse is a small gap separating neuronsInformation from one neuron flows to another neuron across a synapse.
|
|
|
|
Neurotransmitters
|
Chemicals called neurotransmitters. These chemicals are made by the cell that is sending the impulse (the pre-synaptic neurone) and stored in synaptic vesicles at the end of the axon. The cell that is receiving the nerve impulse (the post-synaptic neurone) has chemical-gated ion channels in its membrane, called neuroreceptors
|
|
|
|
The Resting Membrane Potential
|
When a neurone is not sending a signal, it is at ‘rest’. The membrane is responsible for the different events that occur in a neurone. All animal cell membranes contain a protein pump called the sodium-potassium pump (Na+K+ATPase
|
|
|
|
The Action Potential
|
An action potential occurs when a neurone sends information down an axon. This involves an explosion of electrical activity, where the nerve and muscle cells resting membrane potential changes.
In nerve and muscle cells the membranes are electrically excitable, which means they can change their membrane potential, and this is the basis of the nerve impulse. The sodium and potassium channels in these cells are voltage-gated, which means that they can open and close depending on the voltage across the membrane. |
|
|
|
Action Potential has two main phases
|
Depolarisation:the normal voltage polarity (negative inside) is reversed (becomes positive inside).
Repolarisation: The resting membrane potential is restored by the Na+K+ATPase pump. |
|
|
|
Spinal Cord Reflexes
|
Stretch Reflex: (a muscle that is stretched automatically contracts)
Flexor reflex: Automatic withdrawl from painful stimuli (withdrawl reflex) Flexor Withdrawal Reflex |
|
|
|
Location & function of White Matter
|
Spinal cord: nerve impulse paths
Brain: consists of myelated axons or sheaths |
|
|
|
Gray matter
|
Receives and integrates incoming and out going information
|
|
|
|
Cerebellum:
|
Posterior to the medulla and pons
-Voluntary and involuntary movement |
|
|
|
What does the medulla oblongata contain?
|
Above spinal cord, extends to the pons.
-Regulates: HR, RR, and BP. -Refexes: Coughing, sneezing, swallowing, and vomiting |
|
|
|
Cranial Nerve I
|
(Olfactory) Bilateral decreased sense of smell occurs with age, tobacco smoking, allergic rhinitis, cocaine use. Unilateral loss of sense of smell (neurologic anosmia) can indicate a frontal lobe lesion
|
|
|
|
Cranial Nerve II
|
(Optic)
Check visual acuity (have the patient read newspaper print) and visual fields for each eye. Unilateral blindness can indicate a lesion or pressure in the globe or optic nerve. Loss of the same half of the visual field in both eyes (homonymous hemianopsia) can indicate a lesion of the opposite side optic tract as in a CVA |
|
|
|
Cranial Nerve III
|
(Oculomotor)
Assess pupil size and light reflex. A unilaterally dilated pupil with unilateral absent light reflex and/or if the eye will not turn upwards could indicate an internal carotid aneurysm or uncal herniation with increased intracranial pressure. |
|
|
|
Cranial Nerve IV
|
(Trochlear) and Cranial Nerve VI (Abducens)
Have patient turn eyes downward, temporally, and nasally. If the eyes will not do this the patient may have a fracture of the eye orbit or a brain stem tumor. (Note: Cranial Nerves III, IV, and VI are examined together because they control eyelid elevation, eye movement, and pupillary constriction.) |
|
|
|
Cranial Nerve V
|
(Trigeminal)
Motor – Palpate jaws and temples while patient clenches teeth. |
|
|
|
Cranial Nerve VI
|
(Abducens)
Moves eye |
|
|
|
Cranial Nerve VII
|
(Facial)
Check symmetry and mobility of face by having patient frown, close eyes, lift eyebrows, and puff cheeks. Sensory Asses the patient’s ability to identify taste (sugar, salt, lemon juice) An asymmetrical deficit can be found in trauma, Bell’s palsy, CVA, tumor, and inflammation. |
|
|
|
Cranial Nerve VIII
|
(Acoustic or Vestibulocochlear)
This tests hearing acuity. Impairment indicates inflammation or occlusion of the ear canal, drug toxicity, or a possible tumor. |
|
|
|
Cranial Nerve IX
|
(Glossophraryngeal) - Touch and taste
Depress the tongue with a tongue blade and have the patient say “ahh” or yawn. Uvula and soft palate should rise. Gag reflex should be present and the voice should sound smooth. Deficits can indicate a brain stem tumor or neck injury. |
|
|
|
Cranial Nerve X
|
(Vagus)
Sensory/motor control of abdominal organs, heart and lungs Gag reflex should be present and the voice should sound smooth. Deficits can indicate a brain stem tumor or neck injury |
|
|
|
Cranial Nerve XI
|
(Spinal Accessory)
Innervate Trapezius and Sternocleidomastoid Have the patient rotate the head and shrug shoulders against resistance. If the patient is unable to do this it may indicate a neck injury. |
|
|
|
Cranial Nerve XII
|
(Hypoglossal)
Moves tongue Assess tongue control. Wasting of the tongue, deviation to one side, tremors, and an inability to distinctly say l,t,d,n sounds can indicate a lower or upper motor neuron lesion. Reflex Testing |
|
|
|
Thalamus
|
Above the hypothalamus and below the cerebrum.
-Sensation pathways (intergration) |
|
|
|
Dysarthria
|
Slurred speech caused by damage to the cerebellum
|
|
|
|
Apraxia
|
Inability to carry out purposeful movements despite normal muscle coordination and power. It is associated mostly with damage to the parietal lobe
|
|
|
|
Ataxia
|
Jerky, staggering gait and other uncoordinated movements caused by damage to the cerebellum
|
|
|
|
Nystagmus
|
Jerky eye movements and an inability to fix the gaze in one direction and can be produced by damage to the cerebellum
|
|
|
|
Effects of aging on nervous system
|
Reduced blood flow to brain = decreased mental function
Deposition of aging pigment lipofuscin in verve cells & amyloid in blood vessles = impaired cognition Decreased norepinephrine = Altered sleep patterns Decreased Acetylcholine & loss of dendrites = imapired short-term memory Decreased dopamine = deceased motor function leading to increased falls |
|
|
|
Glasgow Coma Scale
|
-Eye Opening
-Verbal Response -Motor Response Numerically scored according to ability to respond to stimuli ranging from 3 - 15. |
|
|
|
Laboratory Tests associated w/ neurological assessment
|
Thyroid
B12 ESR CBC: Infection such as meningitis Electrolytes Hormone Levels: pitutitary dysfunction Creatine Liver fx |
|
|
|
Lumbar Puncture
|
The removal of a small amount of the fluid that protects the brain and spinal cord. The fluid is tested to detect any bleeding or brain hemorrhage, diagnose infection to the brain and/or spinal cord, identify some cases of multiple sclerosis and other neurological conditions, and measure intracranial pressure
|
|
|
|
Hypothalmus
|
Above pituitary gland & thalmus. Produces ADH & Oxytocin, GHRH, regulation of body temp & fliud/food intake, integration of ANS, & stimulation of visceral responses in emotional situations
|
|
|
|
Pons
|
Anterior to the cerebellum and superior to the medulla.
Produce normal breathing rhythm |
|
|
|
Midbrain:
|
Extends from the pons to the hypothalamus and encloses the tunnel that connects 3rd and 4th ventricles.
-Regulates visual reflexes -Auditory reflexes -Righting reflexes |
|
|
|
Lumbar Puncture nursing care
|
Pre-Procedure Nursing Care
Verify Informed Consent Assist with Positioning Post-Procedure Care Maintain Flat Bedrest 6 – 8 Hours Encourage Fluids Monitor Puncture Site Monitor Movement, Sensation, Headache |
|
|
|
Dorsal Root
|
Each spianl nerve has 2 roots consisting of neurons entering or leaving the spinal cord. Dorsal root carries impulses to the spinal cord & contains an enlarged area called called the ganglion that houses cell bodies of sensory neurons.
|
|
|
|
Ventral Root
|
Is the motor root; made up of motor neurons that carry impulses from the spinal cord to muscles or glands found, cell bodies are found in the grey matter of the spinal cord.
|
|
|
|
Spinal Cord Reflex
|
A reflex is an involunary predictable response to a stimulus and do not depend directly on hte brain.
|
|
|
|
Reflex Arc
|
The pathway nerve impulses travel when a reflex is elicited.
|
|
|
|
CT Scan
|
Noninvasive, painless process used to produce rapid, clear two-dimensional images of organs, bones, and tissues. Neurological CT scans are used to view the brain and spine. They can detect bone and vascular irregularities, certain brain tumors and cysts, herniated discs, epilepsy, encephalitis, spinal stenosis (narrowing of the spinal canal), a blood clot or intracranial bleeding in patients with stroke, brain damage from head injury, and other disorders. Many neurological disorders share certain characteristics and a CT scan can aid in proper diagnosis by differentiating the area of the brain affected by the disorder.
|
|
|
|
CT Scan Nursing Care
|
Pre-Procedure
Administer Contrast if Ordered Check Allergies (iodine, shellfish) Check BUN, Cr Request order for sedation if indicated Teach Contrast may cause feeling of warmth S&S of allergic reaction to report Post Procedure Encourage Fluids if Dye Used |
|
|
|
MRI
|
uses computer-generated radio waves and a powerful magnetic field to produce detailed images of body structures including tissues, organs, bones, and nerves. Neurological uses include the diagnosis of brain and spinal cord tumors, eye disease, inflammation, infection, and vascular irregularities that may lead to stroke. MRI can also detect and monitor degenerative disorders such as multiple sclerosis and can document brain injury from trauma.
|
|
|
|
MRI Nursing Care
|
Pre-Procedure Nursing Care
Assure no pacemaker or metal on patient Administer analgesic or sedative as ordered Teach relaxation Post-Procedure Care No Special Care |
|
|
|
Angiogram
|
Test used to detect blockages of the arteries or veins. A cerebral angiogram can detect the degree of narrowing or obstruction of an artery or blood vessel in the brain, head, or neck. It is used to diagnose stroke and to determine the location and size of a brain tumor, aneurysm, or vascular malformation. This test is usually performed in a hospital outpatient setting and takes up to 3 hours, followed by a 6- to 8-hour resting period.
|
|
|
|
Angiogram Nursing Care
|
Pre-Procedure Nursing Care
Verify Informed Consent Give Clear Liquid Diet Insert IV Needle Check BUN/Cr Check PT and PTT Administer Sedation as Ordered Post-Procedure Care Keep Flat in Bed 6 – 8 h Monitor VS Catheter Insertion Site Pulses Encourage Fluids |
|
|
|
Myelogram
|
Involves the injection of a water- or oil-based contrast dye into the spinal canal to enhance x-ray imaging of the spine. Myelograms are used to diagnose spinal nerve injury, herniated discs, fractures, back or leg pain, and spinal tumors.
The procedure takes about 30 minutes and is usually performed in a hospital. Following an injection of anesthesia to a site between two vertebrae in the lower back, a small amount of the cerebrospinal fluid is removed by spinal tap (see cerebrospinal fluid analysis, above) and the contrast dye is injected into the spinal canal. |
|
|
|
Myelogram Nursing Care
|
Pre-Procedure Nursing Care
Check Allergies to Contrast Assess History of Seizures Verify Informed Consent Post-Procedure Care Similar to LP Encourage Fluids |
|
|
|
Electroencephalogram
|
EEG, monitors brain activity through the skull. EEG is used to help diagnose certain seizure disorders, brain tumors, brain damage from head injuries, inflammation of the brain and/or spinal cord, alcoholism, certain psychiatric disorders, and metabolic and degenerative disorders that affect the brain. EEGs are also used to evaluate sleep disorders, monitor brain activity when a patient has been fully anesthetized or loses consciousness, and confirm brain death.
|
|
|
|
Electroencephalogram Nursing care
|
Pre-Procedure Nursing Care
Assure Hair Clean and Dry Check Medication Orders Post-Procedure Care Wash Hair |
|

