![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
25 Cards in this Set
- Front
- Back
|
Functions of the blood
|
- Transportation of dissolved gases, nutrients, hormones, and metabolic waste
- Regulation of the pH and ion composition of interstitial fluid - Restriction of fluid loss at injury sites - Defense against toxins and pathogens - Stabilization of body temperature |
|
|
Components of blood
|
- Plasma
- Formed elements |
|
|
What is whole blood?
|
- Removed blood when composition remains unaltered
|
|
|
What is hematocrit?
|
- a.k.a PCV
- Percentage of whole blood contributed by formed elements - 99% red blood cells |
|
|
Components of Plasma
|
- water (92%)
- Plasma proteins (7%) - Plasma proteins include: - Albumins (major contributor to the osmotic pressure of plasma - Globulins (include antibodies and transport globulins, transport globulins allow hormones to "last longer") - Fibrinogen (clotting, forms fibrin strands) - Active and inactive enzymes and hormones - other solutes (electrolytes, organic nutrients, organic waste) |
|
|
Formed elements
|
- Red blood cells (RBC) 99.9%
- Platelets - White blood cells (WBC) |
|
|
Red blood cell characteristics
|
- a.k.a erythrocytes
- Essential to O2 transport - Biconcave disc: increases surface area causing greater O2 exchange rate - Large in size and flexible: allows for movement in capillaries - Can form stacks: rouleaux - Lose most organelles during development - Contain hemoglobin molecules |
|
|
Platelets
|
- Important to the process of clotting
- First to arrive and stop bleeding (initial plug) - flattened discs that appear round when viewed from above, and spindle shaped in section or in a blood smear - functions: clump together and stick to damaged vessel walls, release chemicals that stimulate blood clotting - megakaryocytes --> platelets |
|
|
White blood cells
|
- Participate in the body's defense mechanism
|
|
|
Development of erythrocytes
|
- Hemoglobin: each molecule has 4 chains (globular protein subunits) 2 alpha and 2 beta chains
- Each chain contains a single heme pigment molecule (each heme, with iron, can reversibly bind one molecule of oxygen) - Each hemoglobin = 4 chains = 4 heme = 4 O2 |
|
|
Stem cells associate with formed elements
|
- Hemocytoblasts --> lymphoid stem cells (production of lymphocytes)
- Hemocytoblasts --> myeloid stem cells (all types of formed elements except lymphocytes) |
|
|
5 white blood cell types
|
- Granular leukocytes (neutrophils, eosinophils, basophils)
- Agranular leukocytes (monocytes, lymphocytes) |
|
|
Neutrophils
|
- Highest concentration
- engulfs pathogens or debris, will attack anything foreign |
|
|
Eosinophils
|
- Engulf antibody labeled materials
- increase in abundance in allergies and parasitic infections |
|
|
Basophils
|
- release histamines and other chemicals that promote inflammation
|
|
|
Monocytes
|
- largest of the 5
- enter tissue and become macrophages, engulf pathogens and debris - waste removal |
|
|
Lymphocytes
|
- provide defense against specific pathogens or toxins
- will only attack specific targets - multiple different for different targets |
|
|
3 phases of hemostasis (clotting response)
|
- Vascular phase
- Platelet phase - Coagulation phase |
|
|
3 phases of hemostasis (clotting response) - Vascular phase
|
- Endothelial cells contract exposing underlying basal lamina to bloodstream
- Endothelial cells release chemical factors, local hormones, and endothelins - Endothelial cells become sticky which causes platelets to attach |
|
|
3 phases of hemostasis (clotting response) - Platelet phase
|
- Platelets attach to endothelial cells, basal lamina, exposed collagen fibers and each other
- Release chemicals - Required for more stable clotting: platelet factors (proteins), Platelet derived growth factor (PDGF) (promotes vessel repair), calcium ions |
|
|
3 phases of hemostasis (clotting response) - coagulation phase
|
- Conversion of circulating fibrinogen to insoluable fibrin
- Two pathways that lead to common pathway (extrinsic and instrinsic) |
|
|
How are clots dissolved?
|
- Proenzyme plasminogen is activated
- Plasminogen becomes plasmin which erodes the clot (plasmin actually erodes the clot) |
|
|
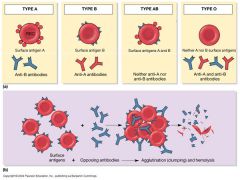
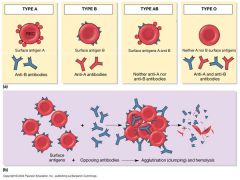
Blood typing
|
- Type A: has A surface antigens, and anti-B antibodies
- Type B: has B surface antigens and anti-A antibodies - Type AB: has AB surface antigens and neither anti-A or anti-B antibodies (universal receiver) - Type O: has no A or B surface antigens and both anti-A and anti-B antigens (universal donor - Rh surface antigen: present= "+" and absence = "-" - If one blood type is exposed to corresponding antibodies clumping (agglutination) occurs |
|
|
Newborn hemolytic disease
|
- Rh negative mother is pregnant with first Rh positive fetus
- During delivery blood is exchanged and the mother develops Rh antibodies - Subsequent babies (Rh+) allow mothers Rh+ antibodies to cross the placenta and attack the fetus |
|
|
|

