![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
52 Cards in this Set
- Front
- Back
|
What is the definition of a myeloproliferative neoplasm?
|
Group of clonal myeloid neoplasms in which a genetic alteration occursin a hematopoietic progenitor cell leading to its proliferation resulting in an increase in the number of peripheral WBCs, RBCs, platelets, or a combination thereof
|
|
|
What cells come from the myeloid cells?
|
RBCs
Platelets WBCs (not lymphocytes, though) |
|
|
What are the feature of chronic myeloid leukemia?
|
Leukocytosis with a left shift
Other findings: Mild anemia Normal-elevated platelet count Peripheral blood basophilia |
|
|
What are the features of polycythemia vera?
|
Elevated RBC indices (RBC count, Hgb, Hct)
Also: Mild leukocytosis Thrombocytosis |
|
|
What are the features of essential thrombocytosis?
|
Elevated platelet count
Also: Mild leukocytosis Polycythemia |
|
|
What are the findings in primary myelofibrosis?
|
Leukoerythroblastic blood smear:
-Tear drops -Nucleated RBCs -Early myeloid precursors Symptoms: -Hepatomegaly -Splenomgaly -Lymphadenopathy |
|
|
What is the age of people who get CML?
|
65
|
|
|
What are risk factors for CML?
|
Prior radiation
Exposure to organic solvents Age Gender: male > female However: 99% of people have no risk factors |
|
|
What are the three phases of CML?
|
Chronic phase
Accelerate phase Blast phase |
|
|
How do you distinguish between the phases of CML?
|
The number of blasts: increased number of blasts, you go to a different phase.
Based on the phase, you have different treatments and outcomes |
|
|
What percentage of blasts is found in the accelerated phase of CML? Blast phase?
|
Accelerated: 10-19%
Blast phase: >20% In the peripheral blood or in the bone marrow |
|
|
What is the hallmark genetic finding of CML?
|
The PHILLY CHROMOSOME!
A balanced chromosomal translocation: -Break near TRK on chromsome 9 (long arm) -Break near BCR on chromsome 22 You get chronic expression of Bcr-Abl |
|
|
What gene product is sufficient and necessary for CML?
|
Bcr-Abl
|
|
|
What's the clinical presentationof CML?
|
15% asymptomatic
Fatigue, weight loss, fever Abdominal fullness, pain, early satiety due to splenomegaly Easy bruising/purpura (dysfunctional platelets) Leukostasis (only when WBC>250K) (thick blood.) |
|
|
In what abnormal location do RBCs develop in CML? Why?
|
Speen (this is the cause of splenomegaly)
They develop there because the marrow gets too full and they return to the place where they developed in the embryo. |
|
|
What does a blood smear of CML look like?
|
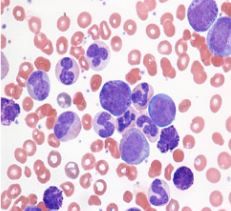
1. Leukocytosis with a left shift
2. Normocytic anemia 3. Thrombocytopenia in 50% of pts 4. Absolute eosinophilia 5. Absolute increase in basophils |
|
|
What is required for a diagnosis of CML?
|
The philly chromosome: t(9,22)
|
|
|
What are mechanisms of diagnosing the philly chromosome?
|
Karyotyping
FISH RT-PCR for Bcr-Abl |
|
|
When you do fish for the philly chromosome, what's a positive result?
|
Yellow!
Shows overlapping of 9 and 22 which are tagged with either red or green; they shouldn't overlap normally |
|
|
What's the best test for CML diagnosis?
|
RT-PCR
|
|
|
What were the early therapies for CML?
|
Interferons: they're horrid for patients, though...lots of side effects.
|
|
|
What is the mechanism of the drugs that best treat CML?
|
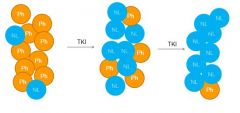
Prevent ATP binding to the Acr TK. No activity FTW!
Slow dying off of the cells that produce the TK? |
|
|
What is the most common mechanism of resistance to the tyrosine kinase inhibitors?
|
Mutation of the site that the inhibitors bind to.
|
|
|
What is the typical way that CML is treated?
|
1st line:
1. Imatinib (gleevec) Second line: different TK inhibitors 1. Dasatinib 2. Nilotinib 3. Bone marrow transplant 4. Clinical trial |
|
|
What is the enzyme that underlies the myeloproliferative disorders other than CML?
|
JAK2
Janice associated kinase, a tyrosine related kinase |
|
|
What protein is almost always mutated in polycythemia vera?
|
JAK2
Lower rate in EMT,other disorders |
|
|
What is the impact of a mutation in JAK2 in the myeloproliferative disorders?
|
Constituitive activation
|
|
|
What's the definition of a relative polycythemia?
|
High concentration of red cells due to a non-proliferative cause
|
|
|
What are common causes of relative polycythemia?
|
Dehydration: depletes plasma volume-->relative polycythemia
Stress erythrocytosis: contraction in plasma volume in hypertensive obese men. |
|
|
What are causes of absolute polycythmia?
|
1, Intrinsic to the bone marrow, more red cells are made
2. Stimulus to the bone marrow from the body to make more red cells |
|
|
What are common causes of absolute polycythemia?
|
1. Primary polycythemia vera
2. Hypoxia (CO poisoning) 3. Carboxyhemoglobinemia 4. Cushing's/corticosteroids 5. Erythropoietin secreting tumors |
|
|
What are symptoms of primary polycythemia vera?
|
Nonspecific complaints: headache, weakness,dizziness, excessive sweating
Puritis FOLLOWING A SHOWER!!!! Erythromegalia (burning pain in feet/hands) Arterial/DVT |
|
|
Why does someone itch after a shower if they have PCV?
|
Mast cells are overproduced, and the heat stimulates the cells to release their contents, causing an itch.
|
|
|
What are the diagnostic criteria for primary PV?
|
1. High red count
2. JAK2 mutation |
|
|
What labs should you do if you suspect someone has PV?
|
Epo
JAK2 If Epo low and JAK2, then PV. If none of those, do a bone marrow biopsy |
|
|
What is the primary risk to people with PCV?
|
Blood clots
|
|
|
What patients are at a particularly high risk for clots with PV?
|
Any one of them can give you a risk for clots
>70 previous thrombosis platelets > 1,500,000/uL CV risk factors |
|
|
What is the treatment for a high risk patient with PV? Low risk?
|
Low risk: phlebotomy, low dose asprin
High risk: plebotomy + asprin + hydroxyurea |
|
|
What is the definition of thrombocytosis?
|
Platelets > 450,000/uL
|
|
|
What are the two types of thrombocytosis?
|
Primary
Secondary In order to diagnose it as a primary, you've got to rule out all of the possible secondary causes = big work up |
|
|
What are the causes of secondary thrombocytosis?
|
1. Malignancies
2. Infections, inflammatory disorders 3. Meds 4. Post surgery 5. Connective tissue disorders 6. Iron deficiency anemia 7. Splenectomy |
|
|
What are the common symptoms of essential thrombocytopenia?
|
30-50% asymptomatic
Headache, syncope, chest pain, etc. Some have thrombosis Early satiety and bloating due to splenomegaly JAK2 in 50% |
|
|
What are the major risks for people with ET?
|
Blood clots (main risk)
Evolution to myelofibrosis or AML |
|
|
Who is at high risk for thrombosis with ET?
|
Age > 60
Prior thrombosis Long-term exposure to a platelet count > 1,000,000 |
|
|
What's the treatment of ET?
|
Low risk: asprin
High risk: hydroxyurea + asprin |
|
|
How can ET cause problems with vWF?
|
There are so many platelets there that they soak up all of the vWF.
|
|
|
What are they symptoms of primary myelofibrosis?
|
Fatigue
Splenomegaly, hepatomegaly Fever and night sweats Anemic syndromes |
|
|
What are findings in the peripheral smear of primary myelofibrosis?
|
Schistocytes
Odd looking blood cells. |
|
|
What do you have to find to diagnose primary myeloid fibrosis?
|
Collagen scar/fibrosis in the bone
Don't have evidence of another cause (CML, PV, MDS,etc.) Jax2mutation |
|
|
What are the risks for PMF?
|
Transformation into AML
|
|
|
What makes someone at a higher risk for transformation in PMF?
|
Age
Anemia Blasts WBC count Symptoms |
|
|
What's the treatment for PMF?
|
Low risk with symptoms:
-hydroxyurea -androgens, corticosteroids -splenic ablation/removal High risk: (and under 55) Bone marrow transplant |

